Difference Between Osteoarthritis And Rheumatoid Arthritis
There are several different types of arthritis. Osteoarthritis and rheumatoid arthritis are two of the most common forms. Although the symptoms of these two types of arthritis can be similar, it’s very important to distinguish between them in order to determine the proper treatment.
At the University of Michigan Health System, our experienced rheumatologists will do appropriate tests to determine which type of arthritis you have. Then we will develop an effective treatment plan and will explain your options.
Osteoarthritis occurs when the smooth cartilage joint surface wears out. Osteoarthritis usually begins in an isolated joint.
Rheumatoid arthritis is an autoimmune disease, which means that the immune system malfunctions and attacks the body instead of intruders. In this case, it attacks the synovial membrane that encases and protects the joints. Rheumatoid arthritis often targets several joints at one time. The symptoms of rheumatoid arthritis include:
- the symmetrical nature of the disease ,
- fever
Spondylitis With Or Without Sacroiliitis
This occurs in approximately 5% of patients with psoriatic arthritis and has a male predominance.
Clinical evidence of spondylitis and/or sacroiliitis can occur in conjunction with other subgroups of psoriatic arthritis.
Spondylitis may occur without radiologic evidence of sacroiliitis, which frequently tends to be asymmetrical, or sacroiliitis may appear radiologically without the classic symptoms of morning stiffness in the lower back. Thus, the correlation between the symptoms and radiologic signs of sacroiliitis can be poor.
Vertebral involvement differs from that observed in ankylosing spondylitis. Vertebrae are affected asymmetrically, and the atlantoaxial joint may be involved with erosion of the odontoid and subluxation . Therapy may limit subluxation-associated disability.
Unusual radiologic features may be present, such as nonmarginal asymmetrical syndesmophytes , paravertebral ossification, and, less commonly, vertebral fusion with disk calcification.
How Is Psoriatic Arthritis Like Rheumatoid Arthritis
- Usually consists of a pattern of alternating flares and remissions
- Runs in families, showing a probable genetic cause
- Specific causes or triggers are unknown
- Can result in joint destruction and severe disability
- Can also be found in a kids size called Juvenile Psoriatic Arthritis / JPA
- TNF plays a significant role in destruction of tissue
- Treatments for PA include a traditional pyramid of medications consisting of NSAIDs, corticosteroids, DMARDs, and immunosuppressant drugs including the modern class of medications called Biologics
Recommended Reading: How To Help Arthritis In Your Hands
Are Rashes From Rheumatoid Arthritis And Eczema Connected
Any person that is suffering from rheumatoid arthritis is dealing with a health condition where the body attacks its own joints instead of fighting off bacteria and viruses like its supposed to. The result of the autoimmune disease is painful wrists, feet, ankles, and fingers.
However, that isnt necessarily the only problem that surfaces. For some, because of the swelling of the joints, eczema can also be a symptom.
The skin above where the inflammation of the joints is occurring can become inflamed as well. It will get rough, itchy, bleed, and in severe cases, blisters may even form. More often than not, these two conditions appear separately.
Eczema is a skin condition that first appears in early childhood years for most patients and continues on throughout their lives. Sometimes though, an individual can get eczema as a result of their arthritis.
While there is still more research that needs to be done on the connection between arthritis and eczema, experts suggest that the red, itchy, and bumpy skin frequently shows up as an indicator that something related to the restriction in blood flow is happening beneath the surface.
Psoriatic Arthritis Vs Rheumatoid Arthritis

Because psoriatic arthritis impacts the skin as well as the joints, its sometimes referred to as a double whammy, or like rheumatoid arthritis but with a nasty skin rash, according to the arthritis advocacy group Creaky Joints.
Both psoriatic and rheumatoid arthritis are autoimmune disorders that cause joint inflammation, pain, and stiffness, as well as chronic fatigue. But there are differences in how the diseases develop and affect the joints.
According to Kathleen Maksimowicz-Mckinnon, DO, a rheumatologist at Henry Ford Hospital in Detroit, there are some telltale signs that your arthritis pain is due to psoriatic arthritis, and not rheumatoid arthritis. These include:
RELATED: Signs and Symptoms of Psoriatic Arthritis
Recommended Reading: How To Relieve Arthritis In Hands
Treatment Options For Ra And Psa
Because of the differences in disease pathogenesis, clinical manifestations and response to therapy between RA and PsA, treatment strategies may differ. provides a summary of current Food and Drug Administration -approved treatments for RA and PsA. Agents targeting more upstream factors are effective in both PsA and RA, while agents targeting more downstream cytokines are more disease-specific, demonstrating significant efficacy in either RA or PsA , but not in both diseases.
Psoriatic Arthritis And Rheumatoid Arthritis Are Both Chronic Inflammatory Conditions
With both diseases, an overzealous immune system mistakenly attacks healthy cells in your body. That can result in joint pain, stiffness, and swelling, along with perpetual fatigue and other symptoms more specific to either disease.
The causes of psoriatic arthritis and rheumatoid arthritis are still up in the air, but doctors suspect the diseases have an underlying genetic component that may make a person more susceptible to certain environmental triggers.
In any case, psoriatic arthritis and rheumatoid arthritis are both lifelong diseases that can occur in flares . And while theres no cure for either disease, treatments for both psoriatic arthritis and rheumatoid arthritis have come a long way toward keeping symptoms at bay, sometimes even putting the disease into remission. Plus, the right medication can help protect your body from the permanent damage these conditions can cause if left untreated, so its important to work with your doctor to manage your disease.
Recommended Reading: How To Deal With Arthritis
So What Is Psoriatic Arthritis And How Does It Differ From Rheumatoid Arthritis
Well, just like rheumatoid arthritis, it is an auto-immune disease. Both cause an erosive inflammatory arthritis in addition to chronic fatigue. And both can have symptoms that vary greatly from person to person. However the distribution of joint involvement differs between the two diseases and psoriatic arthritis involves the skin as well as the joints.
Both diseases can cause destruction of the small joints in your hands and feet as well as larger joints such as knees, hips, shoulders and even the vertebrae in your spine. Classic rheumatoid arthritis primarily involves the PIP joints and wrist, and is generally a symmetrical disease effecting both sides of the body equally. Also with rheumatoid arthritis, nodules specific to this disease are often present.
Both diseases can involve inflammation and scarring of major organs such as your heart and lungs and as in my case can involve your eyes. In addition, both can increase your risk of osteoporosis due the condition itself and also from some of the medications that are used to treat these conditions. After years of taking steroids for my arthritis, it resulted in a couple of compression fractures in my thoracic spine. And, both disorders can also result in joint destruction leading to severe crippling disabilities.
- Was This Helpful?
How Will Psoriatic Arthritis Affect Me
Starting the right treatment as soon as possible will give you the best chance of keeping your arthritis under control and minimise damage to your body.
Psoriatic arthritis can vary a great deal between different people. This makes it difficult to offer advice on what you should expect.
It will usually have some effect on your ability to get around and your quality of life, but treatment will reduce the effect it has.
Psoriatic arthritis can cause long-term damage to joints, bones and other tissues in the body, especially if it isnt treated.
Also Check: High Rheumatoid Factor Causes
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Radiographic Features Of Ra And Psa
Use of imaging can provide important information to help practitioners identify and differentiate between types of inflammatory arthritis. Conventional radiography can be used to identify juxta-articular bony proliferations, which can be used to help discern PsA from other types of inflammatory arthritis, and to visualise osteodestructive lesions characteristic of RA. Other characteristic radiographic changes observed in patients with severe PsA are bone resorption, pencil-in-cup deformities and ankylosis. However, conventional radiographs are not as sensitive as ultrasound or MRI for detection of bone erosions and may not help clinicians detect soft-tissue changes well. Additionally, in our experience, radiologists will often report changes consistent with osteoarthritis in patients with PsA, and it is necessary for rheumatologists to interpret these findings in the proper clinical context.
Ultrasound imaging can be used to identify characteristic features of inflammatory arthritis, including enthesitis, cortical bone erosions, cartilage lesions, synovitis and tenosynovitis. Bone erosions are an important diagnostic criterion of RA that can be identified based on intra-articular discontinuity of the bone surface. Ultrasound evaluations of bone erosions are more reliable for joints that are easily accessible than for carpal or tarsal bones, which cannot be viewed circumferentially.
You May Like: Rheumatoid Arthritis Thigh Pain
Psoriatic Arthritis Versus Osteoarthritis
Joint pain and stiffness, especially in the morning or after resting, can be a symptom of either psoriatic arthritis or osteoarthritis the most common type of arthritis.
Unlike autoimmune forms of arthritis, osteoarthritis is the result of wear-and-tear damage to cartilage the slippery covering that allows bones to easily slide over each other when joints bend, says the Arthritis Foundation.
Damage to the cartilage can result in bone grinding directly on bone, which causes pain and restricts movement.
Osteoarthritis primarily affects the hands, knees, hips, and spine, and can create a grating sensation, along with popping or crackling, when you use the joint, says the Mayo Clinic. You may also notice hard lumps of bone near the joint or the joint may look distorted.
While psoriatic arthritis symptoms tend to flare and subside, osteoarthritis-related pain and swelling usually become progressively worse over time.
Your Rheumatoid Arthritis And Itching Skin
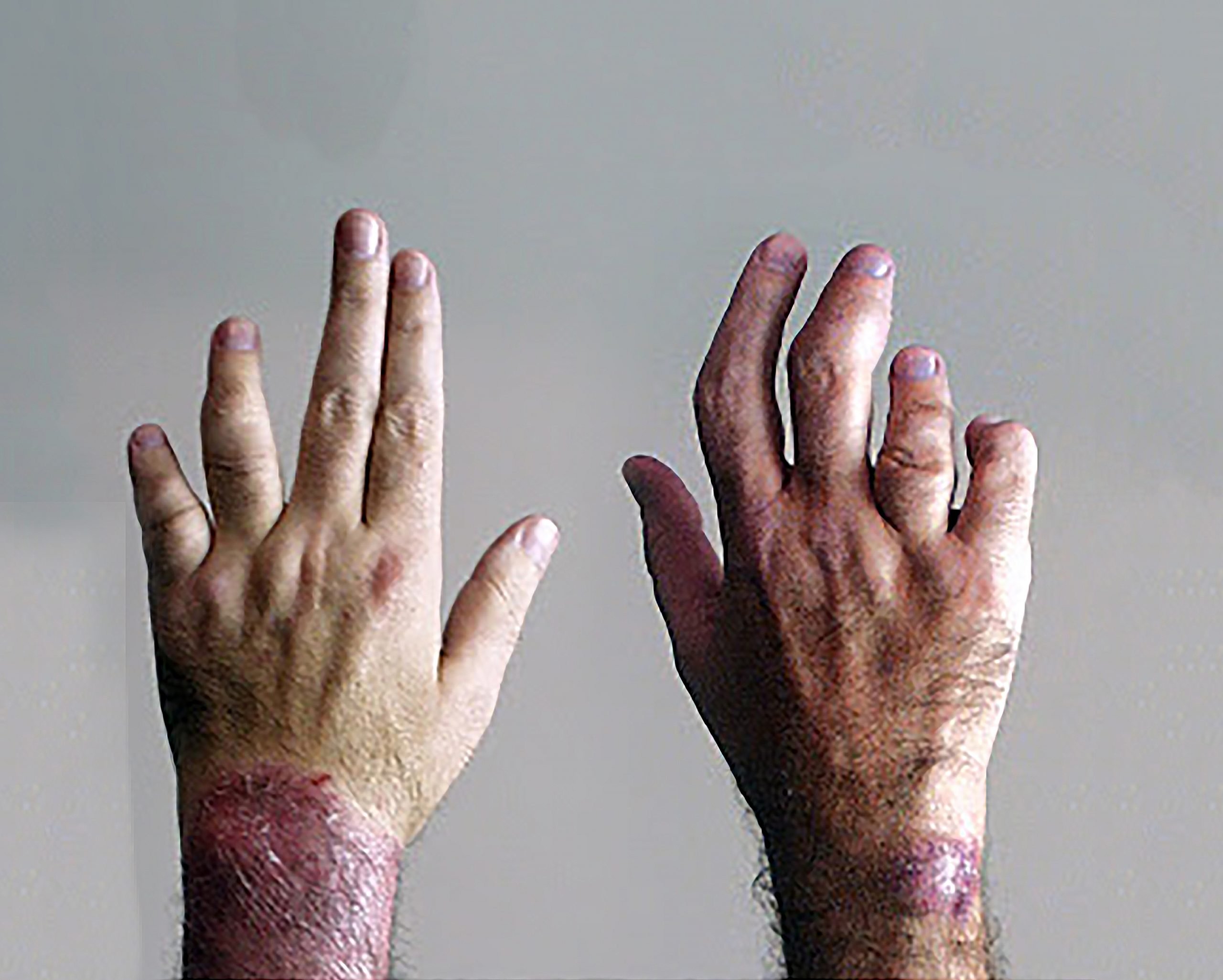
You may have experienced rashes from rheumatoid arthritis at some point. The question is, where does it come from?
The inflammation that occurs when your body is going through a rheumatoid arthritis flare-up is what leads to rashes. These are called rheumatoid vasculitis. Its prevalent in about only one percent of all people living with arthritis, and it often shows up on the legs.
With rheumatoid vasculitis, other symptoms can emerge including any level of severity from red or irritated skin all the way to an ulcer forming because of the reduced blood flow caused by the inflamed blood vessels. Some of the symptoms of rheumatoid vasculitis include:
- Itchiness
- Pain
- Various sized red patches
Traditional treatment options include topical steroid medications and oral prescription drugs. However, these dont always provide the level of relief most people are looking for, especially when the symptoms of rashes from rheumatoid arthritis are more serious.
You May Like: What Does Arthritis In Your Hands Feel Like
When To Get Medical Advice
See a GP if you have persistent pain, swelling or stiffness in your joints even if you have not been diagnosed with psoriasis.
If you’ve been diagnosed with psoriasis, you should have check-ups at least once a year to monitor your condition. Make sure you let the doctor know if you’re experiencing any problems with your joints.
How Psoriatic Arthritis And Rheumatoid Arthritis Differ
Psoriatic arthritis and rheumatoid arthritis are both autoimmune diseases that affect the joints. Both are inflammatory and progressivecausing joint stiffness, pain, and swelling, as well as persistent fatigue. In addition, both occur in flares and can be treated with medications that suppress the immune system.
However, PsA and RA are different diseasesand the differences are important when it comes to their prognosis and the best approach for managing each condition.
With PsA, the joint symptoms are tightly linked to inflammation of the skin from psoriasis . With RA, the immune system primarily targets joint tissue.
The different underlying disease processes mean that the conditions are diagnosed with different methods and they also require different therapeutic approaches.
Don’t Miss: How To Ease Arthritis Pain In Fingers
What Is Psoriatic Arthritis Video
Psoriatic arthritis can cause pain, swelling and stiffness in and around your joints.
It usually affects people who already have the skin condition psoriasis . This causes patches of red, raised skin, with white and silvery flakes.
Sometimes people have arthritis symptoms before the psoriasis. In rare cases, people have psoriatic arthritis and never have any noticeable patches of psoriasis.
Psoriatic arthritis and psoriasis are autoimmune conditions. Our immune system protects us against illness and infection. In autoimmune conditions, the immune system becomes confused and attacks healthy parts of the body.
Both conditions can affect people of any age.
Its estimated that around one in five people with psoriasis will develop psoriatic arthritis.
People with psoriasis are as likely as anyone else to get other types of arthritis, such as osteoarthritis or rheumatoid arthritis. These conditions are not linked to psoriasis.
Psoriatic arthritis is a type of spondyloarthritis. These are a group of conditions with some similar symptoms.
Comorbidities Occurring In Ra And Psa
Differences in patient comorbidities may help clinicians differentiate between RA and PsA . Overall, comorbidity burden may be higher in RA than in PsA, but both diseases are similarly associated with increased risk for comorbidities linked to systemic inflammation . Han and colleagues found that patients with RA and PsA had similarly increased prevalence ratios of ischaemic heart disease, atherosclerosis, peripheral vascular disease, congestive heart failure, cerebrovascular disease, hyperlipidaemia and hypertension compared with healthy controls. However, registry data suggest that the rates of obesity, diabetes mellitus and metabolic syndrome are significantly higher in patients with PsA compared with those with RA. Notably, most patients with PsA are overweight or obese. Cardiometabolic comorbidities of PsA are associated with higher levels of systemic inflammation and increased disease severity. In addition, psoriatic skin lesions are associated with an increased risk for cardiovascular disease and mortality. Of interest, PsA is an independent predictor of non-alcoholic fatty liver disease in patients with psoriasis, while in patients with RA, the rates of NAFLD are similar to those observed in the general population.
Summary of differences in common comorbidities associated with PsA and RA
You May Like: How To Slow Down Arthritis In Hands
Rheumatoid Arthritis And Psoriatic Arthritis: The Similarities And Differences
All forms of arthritis involve tenderness and swelling of the joints. And, at first glance, psoriatic arthritis can be very hard to differentiate from other common types of arthritis, including rheumatoid arthritis and osteoarthritis.
Because psoriatic arthritis symptoms can overlap with those of rheumatoid arthritis and osteoarthritis not just swollen, achy joints but also stiffness and chronic fatigue diagnosing this autoimmune disease can be tricky.
Unlike rheumatoid arthritis, there is no blood test that can determine if a person has psoriatic arthritis, says M. Elaine Husni, MD, MPH, a rheumatologist at the Cleveland Clinic in Ohio.
Psoriatic arthritis can also affect the body in different ways depending on the person and how advanced the disease is, says Dr. Husni. As a result, a rheumatologist may need to examine a patient several times and run a number of tests before having enough information to make a definitive diagnosis.
One unique symptom of psoriatic arthritis that doctors look for is the presence of psoriasis, a condition that causes thick, discolored, scaly skin patches known as plaques, as well as pitted nails or nails that separate from the nail bed, according to the American Academy of Dermatology.
Like psoriatic arthritis, psoriasis stems from a faulty immune response, in which the immune system mistakenly attacks healthy cells and tissues.
Could It Be An Allergy
Many patients Ive seen over the years experience various kinds of allergies. The question is, could it be an allergy or could your symptoms be more indicative of psoriasis, rheumatoid arthritis or both? There are many different kinds of signs and symptoms as well as reactions that are common both to allergies as well as psoriasis and RA. Symptoms that are typical of an auto-immune disorder are light sensitivity, dry eyes and mouth, recurrent headaches and swollen glands.
One good tip that will allow you to distinguish between seasonal allergies and auto-immune disease is just that seasonal. Do your symptoms seem to get worse in spring or fall as opposed to being there all the time? If you experience typical seasonal allergic-type of symptoms then it is much more likely to occur at certain times of the year. Do your symptoms appear randomly, unexpectedly or are continuous without a break? Then its time to see your health-care professional for a more formal diagnosis.
Don’t Miss: What Does The Rash From Psoriatic Arthritis Look Like