Diagnosing Psoriasis And Psa
Unfortunately, theres no one simple diagnostic test to check for psoriasis or psoriatic arthritis. This means your doctor will need to make a clinical diagnosis, which requires taking into account your symptoms, risk factors, as well as the results of bloodwork and X-rays or other imaging scans to assess any joint involvement.
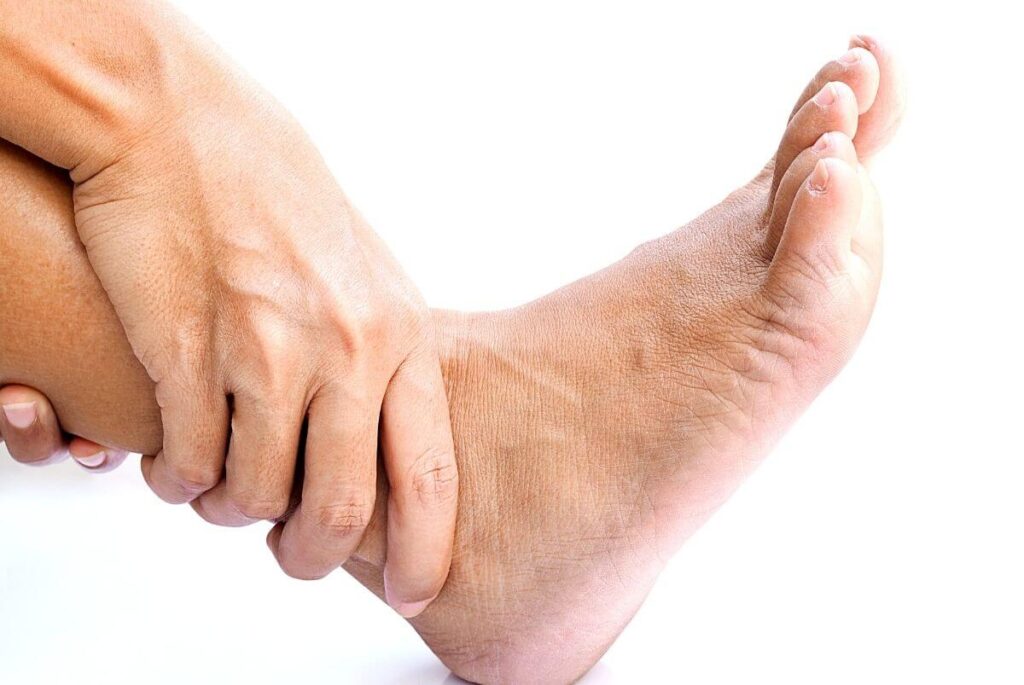
During the physical exam, your doctor might look for signs of psoriasis on the elbows and knees as well as less visible places like the scalp, belly button, intergluteal cleft, palms of hands, and soles of feet. Theyll also check for any fingernail or toenail abnormalities, like pitting or ridging, as well as swollen fingers or toes .
The presence of dactylitis and finger and toenail changes are evidence of psoriasis that can be used to aid in the diagnosis of psoriatic arthritis if there is no evidence of skin disease, says Dr. Haberman.
Here are some common steps used to diagnose psoriasis and PsA:
- A medical exam to discuss family history, risk factors, and symptoms
- Blood tests to check for markers of inflammation and antibodies , which can help rule out other types of arthritis, including rheumatoid arthritis
- Imaging tests to detect any joint damage, dislocation of small or large joints, disfiguration , new bone formation, and inflammation in the enthesis
- Skin biopsy of a skin plaque, if you have previously undiagnosed psoriasis
The Psoriasis Arthritis Symptoms To Watch For
If you are concerned about developing psoriatic arthritis, there are some symptoms to watch out for. First of all, if you have psoriasis already, that is the number one risk factor for getting psoriatic arthritis. Watch for lesions on the nails as a good indicator the ailment will most likely develop.
Family history and age are also determining factors. If you have a parent or sibling with the disease, you are more likely to acquire it as well. The condition usually is diagnosed most frequently in patients between the 30 and 50 years old.
Your Rheumatoid Arthritis And Itching Skin
You may have experienced rashes from rheumatoid arthritis at some point. The question is, where does it come from?
The inflammation that occurs when your body is going through a rheumatoid arthritis flare-up is what leads to rashes. These are called rheumatoid vasculitis. Its prevalent in about only one percent of all people living with arthritis, and it often shows up on the legs.
With rheumatoid vasculitis, other symptoms can emerge including any level of severity from red or irritated skin all the way to an ulcer forming because of the reduced blood flow caused by the inflamed blood vessels. Some of the symptoms of rheumatoid vasculitis include:
- Itchiness
- Pain
- Various sized red patches
Traditional treatment options include topical steroid medications and oral prescription drugs. However, these dont always provide the level of relief most people are looking for, especially when the symptoms of rashes from rheumatoid arthritis are more serious.
Also Check: What Can You Take For Arthritis In Your Hands
How Do You Control Joint Pain In Both Conditions
People who have a thyroid disorder and rheumatoid arthritis are likely to have more aggressive disease progression and poorer responses to treatment. What this means is that it can be hard to manage them. So, suppose you do have both conditions. In that case, you will want to stay on top of your routine testing, follow-up consultations, medications, and lifestyle interventions.
Facing The Challenges Of A Dual Diagnosis With Psoriatic Arthritis

Psoriatic arthritis can co-occur with conditions such as fibromyalgia and gout.
About 1.5 million Americans have psoriatic arthritis , a form of inflammatory arthritis. For many of those people, PsA is only part of the story. Thats because patients may have two or more chronic conditions.
Psoriatic arthritis can be difficult to diagnose because it shares symptoms with conditions like rheumatoid arthritis, osteoarthritis, fibromyalgia, and gout.
According to the Psoriatic Arthritis in America 2016 survey, most people who have PsA experience multiple symptoms over a period of years before the condition is properly diagnosed. The survey found that 41 percent of people saw at least four health professionals before a PsA diagnosis was made.
You May Like: How To Deal With Arthritis
Psoriasis Lupus Rheumatoid Arthritis Share One Gene
DOCTOR’S VIEW ARCHIVE
Nov. 11, 2000 — Changes in one gene have been discovered that are shared bythree common autoimmune diseases — the skin condition psoriasis as well as systemic lupus erythematosus and rheumatoid arthritis . The genetic changes involve a gene called Runx-1.
What is Runx-1?Runx-1 is a protein that acts as a transcription factor. It controls when genes are switched on or off. Runx-1 does so by binding to regulatory sequences– specific sequences of DNA — that are close to the genes they regulate. TheseDNA sequences, called Runx-1 binding sites, are scattered throughout the human genome, wherever there is a gene under the control of Runx-1.
Runx-1 stands for runt-related transcription factor 1. Runx-1 is also called AML1 because it is also altered in a form of acute myeloid leukemia, but that isa very different story, one to be told another time.
The Tie-in with AutoimmunityChanges in Runx-1 appear to contribute to autoimmune diseases. A Runx-1binding site on chromosome 2 is altered in many patients with systemic lupus erythematosus. Many psoriasis patients have a changed Runx-1 binding site on chromosome 17. And a Runx-1 binding site on chromosome 17 is changed in patients with rheumatoid arthritis. Thus, there are genetic connections, some involvingRunx-1, between diverse autoimmune diseases.
Psoriatic Arthritis Versus Rheumatoid Arthritis: Are They The Same
Psoriatic arthritis and rheumatoid arthritis are similar in they both involve your body mistakenly attacking your joints. However, with psoriatic arthritis, your skin is also going to suffer damages. Both have been proven to have genetic factors that are linked to being diagnosed with each disease.
The main difference is that with psoriatic arthritis you will always also be dealing with red, itchy, and painful skin. People living with Rheumatoid arthritis dont always have the accompanied skin condition and may only have to deal with the painful joints.
ILW recommends: Organic Manuka Skin Soothing Cream to naturally heal itchy, irritated skin.
Read Also: Does Psoriatic Arthritis Itch
Living With Psoriatic Arthritis
There is no cure for psoriatic arthritis. However, by understanding the disease and knowing what to expect, you can learn different ways to complete daily tasks or plan activities at times of the day when you are least bothered by its effects. Once you understand and learn to predict the ways in which your body responds to the disease, you can use exercise and therapy to help decrease discomfort, stress and fatigue.
There is a significant list of comorbidities related to PsA. These include these 11 conditions:
Medications For People With Rheumatoid Arthritis
Inflammation in RA is associated with a different interleukin than those in PsA. The IL-6 inhibitor drugs Actemra and Kevzara work against RA, but have not been proven to help with PsA.
In addition, Rituxan and Kineret can be helpful for RA that has not responded to other types of treatment. However, these drugs are not useful in treating PsA.
Recommended Reading: Best Treatment For Lower Back Arthritis
Clinical Characteristics Of Ra And Psa
For RA, the American College of Rheumatology /European League Against Rheumatism classification criteria were designed for patient characterisation and use in clinical trials. The key clinical characteristic is the confirmation of definite, persistent, clinical synovitis in at least one joint. The criteria include the number of joints involved, duration of symptoms, and the demonstration of serological markers and an elevated acute-phase reactant. For PsA, the Classification Criteria for Psoriatic Arthritis help categorise patients with inflammatory articular disease for clinical trials. Key clinical characteristics include a personal or family history of psoriasis, psoriatic nail dystrophy and dactylitis. Neither classification criteria should be confused as diagnostic criteria.
Joint involvement is predominantly symmetric in RA and often, but not always, asymmetric in PsA. In both RA and PsA, most patients have polyarthritis , although joint involvement can be oligoarticular or polyarticular. Monoarticular disease is less common in PsA however, 5%10% of patients may present with isolated distal joint involvement. In PsA, prognosis worsens and symmetry of joint involvement tends to increase as the number of affected joints increases.
A Look At The Most Important Updates That People Living With Psoriatic Arthritis Should Know About From The American College Of Rheumatologys 2021 Medical Conference
You can participate in research studies about arthritis by using our ArthritisPower app to join our patient-centered research registry.
At the American College of Rheumatology/Association of Rheumatology Health Professionals Annual Meeting this year ACR Convergence 2021 more than 16,500 attendees and 600 speakers from more than 100 countries gathered virtually to share the latest research and address the most pressing issues for people living with rheumatic disease.
The CreakyJoints team soaked it all in listening, watching, and learning so we could bring you the most relevant information to ensure you know what you need to better manage your condition and get better care.
We combed through hundreds of studies, attended sessions from top psoriatic arthritis experts, and asked our team of patient and physician advisors to share the psoriatic arthritis updates they deemed most important for patients.
The result: Our curated, patient-friendly guide to psoriatic arthritis research and trends from ACR 2021. For more research breakthroughs from ACR 2021, check out our main guide: 100+ Arthritis & Rheumatic Disease Updates You Need to Know.
You May Like: Rheumatoid Arthritis Symptoms Checker
How Successful Are The Treatments
Anti-inflammatory drugs can help to reduce pain, swelling and stiffness. Unfortunately, however, they can make skin symptoms worse in some people. Steroid injections to joints may give relief. Disease-modifying drugs such as methotrexate can damp down both skin and joint symptoms, as can targeted biologic agents.
In some cases, surgery to remove a thickened synovial membrane , realign a joint or to fuse a joint may stop pain which results from movement.
Sometimes it is possible to remove the painful end of a bone .
Remember: All treatments may have unwanted side effects or require special precautions . Always make sure you have all the information before embarking on any course of therapy this includes reading the patient information leaflets provided with your medicines.
What Are The Symptoms Of Psoriasis
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
Read Also: Rheumatoid Arthritis Edema
Is It Possible To Have Both Psa And Ra
You can have both PsA and RA. However, because its also possible to have just one of the conditions, you should talk to your doctor or rheumatologist if you are confused about your symptoms. Additionally, some people with PsA never experience the obvious skin disease symptoms of psoriasis, making it easy to confuse PsA with RA.
In people who have both PsA and RA, the symptoms may sometimes overlap or come and go. As one MyPsoriasisTeam member shared, My psoriasis has cleared up a lot, but my rheumatoid arthritis and psoriatic arthritis have gotten worse.
Blood Tests For Psa And Ra
Blood tests can also help tell the difference between PsA and RA.
About 80 percent of people with RA are said to have seropositive RA, which means they test positive for rheumatoid factor or for cyclic citrullinated peptide antibodies.
Most people with PsA do not have RF or CCP antibodies and are considered seronegative. However, it is also possible to have seronegative RA.
You May Like: How To Deal With Arthritis
How Is Psoriatic Arthritis Treated
Treatment will depend on your symptoms, age, and general health. It will also depend on the severity of your condition.
Boththe skin condition and the joint inflammation are treated. Early diagnosis andtreatment helps prevent joint damage. Some medicines used to treat psoriatic arthritisinclude:
- Nonsteroidal anti-inflammatory medicines to ease symptoms
- Corticosteroids for inflammation
- Immunosuppressive medicines such as methotrexate to reduce inflammation if NSAIDs don’t work
- Biologic medicines to ease inflammation
- Vitamins and minerals such as calcium and vitamin D to slow bone deformation
Other treatment may include:
- Obesity
Treatment Options For Ra And Psa
Because of the differences in disease pathogenesis, clinical manifestations and response to therapy between RA and PsA, treatment strategies may differ. provides a summary of current Food and Drug Administration -approved treatments for RA and PsA. Agents targeting more upstream factors are effective in both PsA and RA, while agents targeting more downstream cytokines are more disease-specific, demonstrating significant efficacy in either RA or PsA , but not in both diseases.
Don’t Miss: How Do I Know If I Have Knee Arthritis
Psoriasis Arthritis Signs And Symptoms
Psoriatic arthritis, or PsA, is a chronic, autoimmune form of arthritis that causes joint inflammation and occurs with the skin condition psoriasis. It can affect large or small joints, and less commonly, the spine. About a third of people with psoriasis develop PsA.
This condition can also cause painful joints, referred to as psoriatic arthritis.
there is no cure for psoriasis. However, treatment can help manage symptoms, and people with psoriasis can.
What are the signs and symptoms of psoriasis? Dry, thick, and raised patches on the skin are the most common sign of psoriasis. These patches are often covered with a silvery-white coating called scale, and they tend to itch. While patches of thickened, dry skin are common, psoriasis can cause many signs and symptoms.
Diagnosis is typically based on the signs and symptoms. No cure for psoriasis is known, but various treatments can help control the symptoms. These treatments include steroid creams, vitamin D 3 cream, ultraviolet light, and immunosuppressive drugs, such as methotrexate. About 75% of skin involvement improves with creams alone.
The 5 most common symptoms of psoriasis include: Rashes or patches of red, inflamed skin , often covered with loose, silver-colored scales in severe cases, the plaques will grow and merge into.
Psoriasis is a common skin.
If a person also develops psoriatic arthritis, certain joints may stiffen, swell, and become painful, and the symptoms may be worse in the morning.
Could It Be An Allergy
Many patients Ive seen over the years experience various kinds of allergies. The question is, could it be an allergy or could your symptoms be more indicative of psoriasis, rheumatoid arthritis or both? There are many different kinds of signs and symptoms as well as reactions that are common both to allergies as well as psoriasis and RA. Symptoms that are typical of an auto-immune disorder are light sensitivity, dry eyes and mouth, recurrent headaches and swollen glands.
One good tip that will allow you to distinguish between seasonal allergies and auto-immune disease is just that seasonal. Do your symptoms seem to get worse in spring or fall as opposed to being there all the time? If you experience typical seasonal allergic-type of symptoms then it is much more likely to occur at certain times of the year. Do your symptoms appear randomly, unexpectedly or are continuous without a break? Then its time to see your health-care professional for a more formal diagnosis.
Read Also: Is Banana Good For Rheumatoid Arthritis
What Are The Causes Of Psoriatic Arthritis And Rheumatoid Arthritis
We don’t have an understanding of what causes many autoimmune conditions, including RA and PsA, but there are common links among people who develop these diseases.
“We don’t know exactly what causes RA or PSA, but we do know there are genetic components and stress components to both,” Magdalena Perez-Rivera, MD, rheumatology specialist with Conviva Care Centers tells Health.
Here are some of the primary risk factors for RA and PsAyou’ll see there is a good amount of overlap.
There Are Various Forms Of Psoriasis And Psoriatic Arthritis
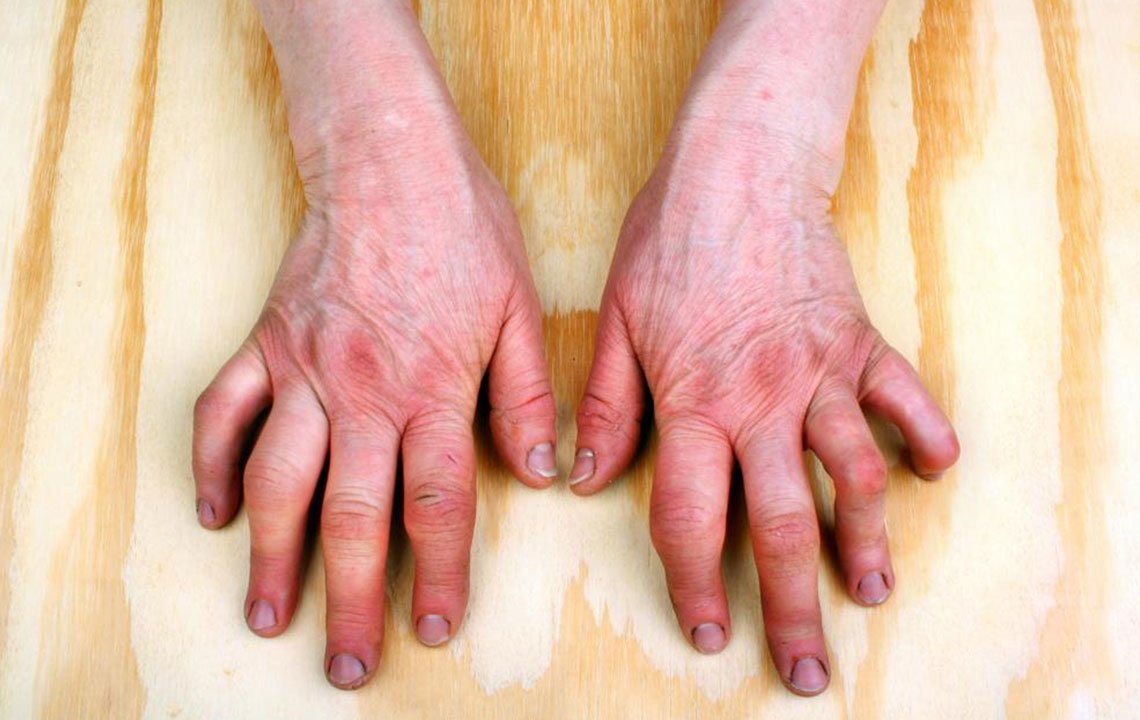
There are five types of psoriatic arthritis, and the disease can trigger symptoms in different areas of your body depending on the type you have, according to NYU Langone Health. They are:
- Asymmetric oligoarthritis can cause pain and stiffness in up to five joints on either side of your body.
- Symmetric arthritis is characterized by painful, swollen joints on just one side of your body.
- Spondylitic arthritis When you experience arthritis symptoms in your spine, or you might have neck pain and difficulty moving your head.
- Distal interphalangeal predominant psoriatic arthritis involves inflammation in your fingernails and toenails.
- Arthritis mutilans is a rare but severe form of psoriatic arthritis that causes damage in the bones of your toes and fingers, according to NYU Langone.
The Mayo Clinic explains there are six types of psoriasis, and your symptoms may vary depending on the type you have.
Psoriasis and psoriatic arthritis do share one common symptom: fatigue, which is likely due to high levels of inflammation, according to NYU Langone Health.
You May Like: How To Ease Arthritis Pain In Fingers
Do You Need To Modify Rheumatoid Arthritis Medications Before Or After Getting The Vaccine
Temporarily stopping certain immunosuppressant medications after receiving the vaccine, or timing when you get the vaccine in the course of your treatment, might help increase the effectiveness of the COVID-19 vaccine if you have RA.
But whether this is right for you depends on a number of factors, including which medications you take and your overall health. For example, if your RA is not well-controlled and skipping medications is likely to cause you to flare, your doctor may suggest that you keep taking them. You and your doctor should decide together about making any medication changes. You should not stop taking any of your rheumatoid arthritis medications on your own.
Most disease-modifying antirheumatic drugs, including biologics, should not be stopped for those with rheumatoid arthritis. Here are the RA drugs for which the ACR guidance suggests changes may be recommended:
- Methotrexate: Skip for 1 week after each vaccine dose
- JAK inhibitors : Skip for 1 week after each vaccine dose
- Abatacept , injectable form: Skip one week before and after the first vaccine dose only
- Abatacept , IV form: Get COVID-19 vaccine 4 weeks after your last infusion, then skip a week and get next infusion
- Rituximab : Get COVID-19 vaccine approximately 4 weeks before next infusion, then delay next infusion by 2-4 weeks after second vaccine dose if possible
- Cyclophosphamide infusion: Time administration so its one week after each COVID-19 vaccine dose