The Basics Of Psoriatic Arthritis
When people think of psoriatic arthritis, they often immediately associate it with the skin disease psoriasis. Psoriasis is an autoimmune skin condition characterized by scaly red patches that commonly show up on your elbows, knees, and scalp. In about 70 percent of PsA cases, psoriasis appears first, though arthritis symptoms precede psoriasis in about 15 percent of cases and in another 15 percent of cases, the joint and skin symptoms strike at the same time.
Estimates vary, but its thought that roughly one in three people with psoriasis will develop psoriatic arthritis over time, according to the Johns Hopkins Arthritis Center.
As with many inflammatory conditions, doctors dont know what causes psoriatic arthritis, though a combination of environment and genetics are thought to play a role about four in 10 people with PsA have family with either psoriasis or arthritis. PsA often strikes between the ages 30 and 50 and tends to occur in men and women equally. Caucasian people develop it more often than African or Asian Americans.
Like AS, PsA is also associated with many comorbidities, including inflammatory bowel disease, skin cancer, and depression. Many patients have metabolic syndrome, a group of health problems including obesity, high blood pressure, and high blood sugar that raises the risk for heart disease. Heart disease is a common complication among those with PsA.
Common Types Of Arthritis
Commonly associated with older age, arthritis affects more than 50 million Americans, including more than 300,000 children each year. There are over 100 different forms of arthritis. Depending on the type, it can be extremely painful and affect everyday activities or go relatively unnoticed and be easily managed for years.
Simply put, arthritis is the inflammation of one or more joints. Most individuals experience common symptoms like joint pain, swelling, stiffness and/or decreased range of motion.
Here are 5 of the most common types of arthritis:
Joint Pain Swelling And Stiffness
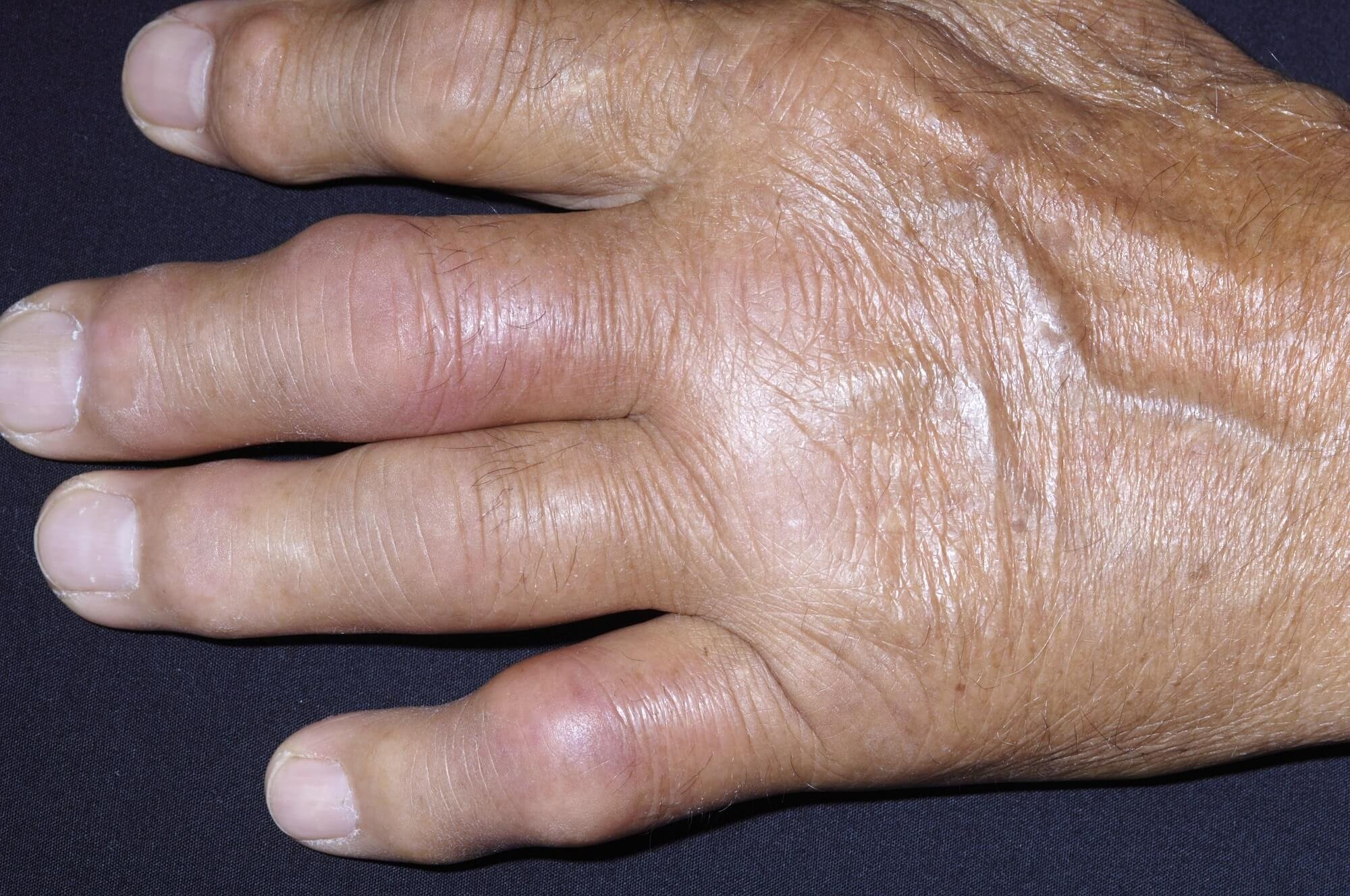
People with PsA experience swelling, pain, and stiffness in joints especially in the fingers and toes. This pain can affect a single joint or many joints and can appear in different parts of the body. Just like with AS, symptoms can especially bad in the morning or after being in the same position for a long time. In PsA, joint pain is less likely to be symmetrical, which is a distinction from rheumatoid arthritis .
Don’t Miss: How To Cure Arthritis Naturally
Does Everyone With Psoriasis Get Psoriatic Arthritis
Not every person with psoriasis gets psoriatic arthritis. The condition affects about one-third of the people with psoriasis. Studies report that having severe psoriasis symptoms or nail psoriasis generally increases the risk of psoriatic arthritis. About 90 percent of people with psoriatic arthritis have nail psoriasis.
Many people with psoriatic arthritis initially have skin lesions of psoriasis. Nonetheless, psoriatic arthritis can occur in people with no skin signs of psoriasis. Furthermore, the joint affected may not coincide with the site where skin lesions are present.
- For example, you may have psoriatic arthritis that affects the knee but no psoriatic skin lesions over the legs or knee.
- Similarly, you may have psoriatic plaques over the elbow but no involvement of the elbow joint.
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else.
Psoriatic arthritis can be classed as a disability if it:
- makes daily tasks difficult
- lasts for more than 12 months.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Read Also: How To Massage Someone With Rheumatoid Arthritis
The Connection With Arthritis
Some kinds of arthritis are autoimmune disorders. This means your body’s immune system makes chemicals that attack and damage your own tissues. This can cause enthesitis.
It’s a common symptom of two kinds of autoimmune arthritis — psoriatic arthritis and ankylosing spondylitis. Psoriatic arthritis, which is common in people with the skin condition psoriasis, can affect your entire body. Ankylosing spondylitis mainly affects your spine.
Enthesitis also happens in about 10% to 20% of children with juvenile idiopathic arthritis, which can affect one or more joints and lasts at least 6 weeks. These children are described as having enthesitis-related arthritis .
Kids with juvenile arthritis often have a family history of inflammatory conditions, like ankylosing spondylitis, psoriatic arthritis, or inflammatory bowel disease. They also have eye redness and pain due to inflammation, along with other arthritis symptoms.
Show Sources
Similarities Between Psoriatic Arthritis And Psoriasis
Even though they are independent diseases, there are striking similarities between the two. Both the conditions are related, but it is not certain that a patient suffering from Psoriasis will develop Psoriatic arthritis. Acute inflammation is a common factor in both diseases. In both cases, the immune system attacks the body to cause this. Just like Psoriasis, the symptoms are not consistent. They can stay for months and then disappear only to come back after some time. Genetic factors, as well as environmental conditions, are responsible for both.
MEDICATION USED FOR TREATING BOTH PSORIATIC ARTHRITIS AND PSORIASIS
Although there is no permanent solution to these conditions, there are certain medicines that can help you to deal with the symptoms. is one such drug that is taken orally with or without food. It is usually started on a low dosage of 10 mg to see if the body is responding to it properly. Another kinase inhibitor named Tofacitinib is preferred by doctors to treat conditions where the body has not responded adequately to previous treatments. For treating moderate to severe Plaque Psoriasis, Etanercept is recommended by doctors. The usual dose is 25mg or 50mg twice a week, to which a number of patients have responded well. Tacrolimus is used to deal with Plaque Psoriasis, Inverse Psoriasis as well as refractory Psoriatic arthritis. It can be prescribed alone or in combination with other drugs.
Recommended Reading: Is Biofreeze Good For Arthritis
Treatments For Psoriasis And Psoriatic Arthritis
Many medications can help treat both the skin and joints, but there are definitely medications that work better for one than the other, explains Dr. Haberman. When treating PsA, we focus on both domains. We may start with one medication if your skin is worse that is better on the skin, but it should still have effects on the joints, she says.
According to the clinical treatment guidelines by the American College of Rheumatology and the National Psoriasis Foundation , your personal treatment plan should depend on how PsA is impacting your body as well as the severity of your symptoms.
Since patients with psoriatic arthritis may have different degrees of involvement of skin, joint pain, finger and toe swelling , and pain where tendons and ligaments attach to bone , its important to identify the most problematic areas and choose treatment options that are best suited for them, says Dr. Husni.
For example, if you have little joint pain and a lot of skin involvement, your rheumatologist might try newer biologics called IL-17 inhibitors, like secukinumab and ixekizumab , notes Dr. Haberman.
While we have a lot of medication options for PsA, sometimes it is more of trial and error to see which medication the patient will respond to, she says. Sometimes we need to try more than one medication to find the one that is right for that patient.
Medications use to treat both psoriasis and PsA include:
What You Need To Know About Psoriasis Is Plaque Psoriasis The Same As Psoriatic Arthritis
Is Your Stomach to Blame?
Who would have thought that a severe psoriasis outbreak could start because of something going wrong inside of your stomach and intestines? Yet, new research developed by psoriasis expert Edgard Cayce shows a distinct link between a leaky gut and a scaly psoriatic episode. According to Cayce, the primary source of psoriasis can be found in the intestinal tract, where toxins are leached into the body. This causes the immune system to react by thickening the skin. At the same time, the skin tries to purge the toxins through its layers, which can cause scabs and sores to form.
Could Arthritis Be the Cuplrit?
The intestines arent the only link to psoriasis found by researchers arthritis seems to also contribute to it. As many as one-third of all psoriasis patients eventually develop some form of psoriatic arthritis. Unlike normal forms of arthritis, those with psoriatic arthritis do not exhibit a rheumatoid factor when their blood is tested. This indicates that the arthritic condition comes solely from either the psoriasis itself or the underlying cause of the skin affliction.
Could a Virus Be the Cause?
Arthritis has been linked to certain virus and so have other auto-immune disorders. This leads some researchers to think that psoriasis too may start with a virus, which is what kicks the immune system into overdrive.
Recommended Reading: How To Stop Psoriatic Arthritis Pain
How Is Psoriatic Arthritis Treated
Treatment will depend on your symptoms, age, and general health. It will also depend on the severity of your condition.
Boththe skin condition and the joint inflammation are treated. Early diagnosis andtreatment helps prevent joint damage. Some medicines used to treat psoriatic arthritisinclude:
- Nonsteroidal anti-inflammatory medicines to ease symptoms
- Corticosteroids for inflammation
- Immunosuppressive medicines such as methotrexate to reduce inflammation if NSAIDs don’t work
- Biologic medicines to ease inflammation
- Vitamins and minerals such as calcium and vitamin D to slow bone deformation
Other treatment may include:
- Obesity
Genetic Markers Of Psoriatic Arthritis
In the last 3 years, significant progress has been made toward identifying genetic markers associated with psoriatic arthritis. However, most of these markers are also associated with psoriasis, and thus a major remaining challenge is to identify genetic risk factors that are specific to psoriatic arthritis.
HLA locus
The HLA locus contains many genes responsible for immunologic function in humans. Psoriasis and psoriatic arthritis demonstrate human leukocyte antigen associations, most frequently with HLA-Cw6.29,6769 However, the HLA region may potentially harbor multiple genes that are associated with psoriasis and psoriatic arthritis. For psoriasis, Feng et al.70 recently identified three independent signals near the HLA locus that contribute to psoriasis risk: HLA-Cw6, c6orf10, and the region between HLA-B and MICA.
Although psoriatic arthritis is most strongly associated with HLA-Cw6, other HLA markers have also been associated with it. The frequency of HLA-B27 is reportedly higher among patients with psoriatic arthritis.28,71,72 Gladmann and Farewell71 performed a univariate analysis of psoriatic arthritis patients and showed that HLA-B27, HLA-B39, and HLA-DQw3 antigens were associated with psoriatic arthritis disease progression, whereas HLA-DR7 was protective. Additionally, the presence of HLA-B39 suggested early progression in psoriatic arthritis.
MICA locus
Other genetic loci
Recommended Reading: What Is The Dosage For Tylenol Arthritis
Symptoms Of Ra And Psa
Both RA and PsA cause joint swelling, stiffness, and pain. Although both conditions affect joints in the fingers and toes, they do it in slightly different ways. And each one can cause other symptoms, too.
Rheumatoid arthritis:
- Often starts in the smaller joints, like the ones in your fingers and toes over time, it may affect other joints, too, like your wrists, knees, hips, and ankles.
- Usually shows up on the same joints on both sides of your body that means itâs symmetric.
- Often makes joints feel stiffer in the morning
- Can lead to fatigue, low-grade fever, and weight loss
Psoriatic arthritis:
- Can affect joints in the back and pelvis in addition to the ones in fingers and toes
- Often affects only one side of your body that means itâs asymmetric.
- Sometimes causes foot pain, especially on the sole of your foot or the back of your heel
- May make your fingers swell up like sausages
- May make your nails pit and flake
- Tends to affect entheses, areas where tendons or ligaments attach to bones
With both conditions, youâll probably have times when your symptoms get worse. These are called flares. In between these flares are times without symptoms called remissions.
Recommended Reading: Signs Of Arthritis In Legs
Types Of Psoriatic Arthritis
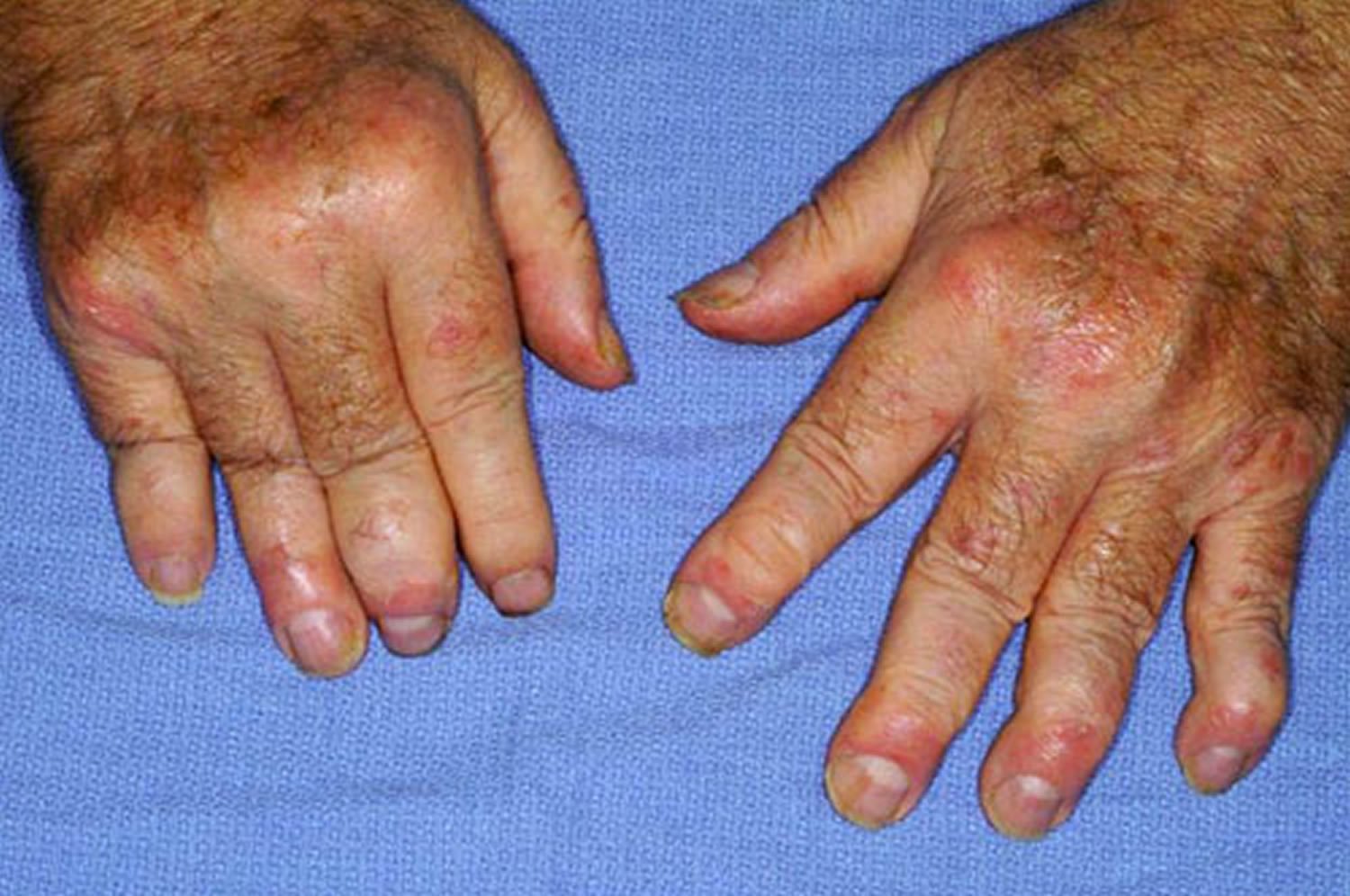
Here are the five different types of psoriatic arthritis:
- Symmetric psoriatic arthritis As its name implies, this type affects joints on both sides of your body at the same time. About half of people with psoriatic arthritis have the symmetric kind.
- Asymmetric psoriatic arthritis With the asymmetric type, problems dont develop in the same joints on both sides of the body. It occurs in about 35 percent of people with the disease and often causes more mild symptoms.
- Spondylitis This form of psoriatic arthritis is characterized by pain and stiffness in the neck and spine.
- Arthritis mutilans People with arthritis mutilans experience deformities in the small joints at the ends of the fingers and toes. This type is considered the most severe form of psoriatic arthritis, but it only affects about 5 percent of people with the condition.
- Distal psoriatic arthritis It causes inflammation and stiffness near the ends of the fingers and toes, while also affecting the nails.
Read Also: What Can Be Done For Arthritis
Don’t Miss: How Long Does Rheumatoid Arthritis Last
How Is Psoriasis Diagnosed And Treated
Psoriasis often has a typical appearance that a primary care doctor can recognize, but it can be confused with other skin diseases , so a dermatologist is often the best doctor to diagnose it. The treatment of psoriasis usually depends on how much skin is affected, how bad the disease is , or the location . Treatments range from creams and ointments applied to the affected areas to ultraviolet light therapy to drugs . Many people who have psoriasis also have serious health conditions such as diabetes, heart disease, and depression. Some people with psoriasis also have an inflammatory condition which affects their joints, called psoriatic arthritis.
Psoriatic arthritis has many of the same symptoms as other types of arthritis, so a rheumatologist is often the best doctor to diagnose it. The treatment of psoriatic arthritis usually involves the use of drugs .
Psoriatic disease may be treated with drugs or a combination of drugs and creams or ointments.
Treatment Options For Psoriasis Only
The most common treatments for mild psoriasis are topical skin creams and ointments. These include vitamin D, salicylic acid, and a class of drugs called corticosteroids.
Vitamin D has been deemed an effective treatment for autoimmune problems in the body, including psoriasis.
Corticosteroids have been found to be at least as effective as vitamin D. The drawback of corticosteroids is that over time, using them on your skin might make your skin weaker. Other side effects of corticosteroids include:
- broken blood vessels
- irritation
- skin that bruises
Corticosteroids range from mild to extremely potent. The more potent the drugs, the higher the potential for side effects. Because psoriasis is a chronic disease, the best treatments are those that can be used long term without risk of injury to your body.
Certain home remedies may also help you relieve psoriasis symptoms. Daily baths using Epsom salts can soothe scaly patches on your skin. Topical aloe vera and Oregon grape have been found to help reduce irritation and inflammation.
Read Also: Can Rheumatoid Arthritis Cause Extreme Fatigue
The Best And Safest Treatment Available
Tens of thousands of men and women in more than 176 countries have naturally got rid of Psoriasis and are now Psoriasis free. The best part is, they did it without drugs, over the counters and without creams or any side effects
How did they do it? They used a scientifically proven and real-world tested program thats been sweeping the Internet called, Psoriasis Revolution.
What Makes This Psoriasis Breakthrough So Exciting is That it Gives You The Power To
Psoriasis Revolution is a 250-page downloadable e-book, jam-packed cover to cover with all the secret Psoriasis cure methods and unique powerful techniques, and the step-by-step holistic Psoriasis system Ive discovered in over 14 years of Psoriasis research. This program contains all the information youll ever need to eliminate your Psoriasis permanently without topical corticosteroids, de-pigmentation or UV therapy and without any side effects.
There are NO gimmicks in this program there are no magic pills, or drugs to buy and no hidden agendas just the FACTS you need to know to get rid of Psoriasis quickly and naturally. Its great news that someone has finally released an effective Psoriasis program based on the truth, but this also means that you have to ask if this is the right program for you:
To learn more about the Psoriasis Revolution system and to find out how YOU can start re-balancing your body today and start the path to becoming Psoriasis free, visit the Psoriasis Revolution