Can Rheumatoid Arthritis Be Treated Without Prescription Medications
Medication is the most important part of RA treatment. That said, there are other options that can be helpful when added to medication. These options should not take the place of medications , which are needed to target inflammation and prevent further damage.
The goal of non-medication treatments is to improve your:
-
Mobility
Studies show that these interventions can improve fatigue from RA, stress related to symptoms, and reduce emotional and behavioral expressions of pain.
It might also help to connect with others who have RA. Here you can find a support group or event near you, or sign up to join the RA community online.
What Are The Less Common Forms Of Rheumatoid Arthritis
Rheumatoid arthritis can begin in less common forms. For example, it can begin with the involvement of only a single joint or a few joints. Sometimes, this can later evolve to the more common presentation of many joints on both sides of the body.
- Rarely, the earliest symptom of rheumatoid disease is inflammation of a body area that does not even involve a joint. For example, the lining of the lungs can become inflamed to cause pleurisy many months before arthritis develops.
- Occasionally, only a few joints are involved and the doctor may suspect another type of inflammatory arthritis. Again, this can sometimes only later evolve to become the more typical symmetrical polyarthritis by including many joints on both sides of the body.
- The caveat is that by recognizing the early symptoms of rheumatoid arthritis rheumatologists and their patients can address the disease early, thereby affording optimal outcomes for those affected.
Dont Miss: Mayo Clinic On Arthritis
Is There A Cure For Rheumatoid Arthritis
There is no cure yet, however, we now know a great deal about what causes RA, and how to control it and prevent joint damage. This is achieved by the early implementation of disease-modifying antirheumatic drugs . These are essential to gain rapid control of the disease, in order to avoid joint erosions and long-term limitation of function.
Recommended Reading: What Is The Best Painkiller For Rheumatoid Arthritis
Focusing On Negativity And Pessimism
Simply put, it takes a positive attitude, rather than a negative or pessimistic one, to achieve positive results. It is logical that you need a positive approach to stay on track with your treatment regimen, exercise routine, diet, and more. You must believe in the goal. In a study published in December 2018 in The Clinical Journal of Pain, researchers found that optimism and mental resilience were associated with less pain severity in people with or at risk for knee osteoarthritis.
RELATED: Catastrophizing About Rheumatoid Arthritis Pain Can Make It Worse
What Are The Symptoms Of Rheumatoid Arthritis
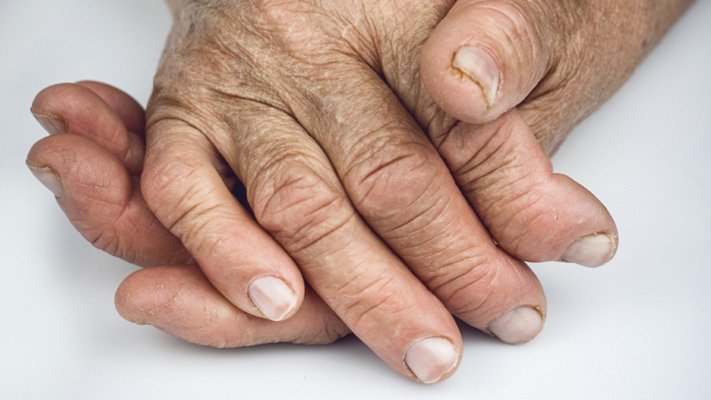
The symptoms of rheumatoid arthritis include the following:
- Stiffness, especially in the morning or after sitting for long periods
- Fatigue
Rheumatoid arthritis affects each person differently. In most people, joint symptoms may develop gradually over several years. In other people, rheumatoid arthritis may proceed rapidly. A few people may have rheumatoid arthritis for a limited period of time and then go into remission .
Cartilage normally acts as a shock absorber between the joints. Uncontrolled inflammation causes the destruction and wearing down of the cartilage, which leads to joint deformities. Eventually, the bone itself erodes, potentially leading to fusion of the joint . This process is aided by specific cells and substances of the immune system, which are produced in the joints but also circulate and cause symptoms throughout the body.
Don’t Miss: Rheumatoid Factor 7.0
Leading A Sedentary Lifestyle
Regular physical activity is necessary for everyone, including people with RA, and there are numerous health benefits associated with it. Improved muscle strength, as well as better bone and joint health, is essential for people with RA. Rest is also needed, to restore the body from the episodes of intense pain and fatigue that are characteristic of RA. But rest cant become a way of life striking a balance between rest and activity is optimal. A sedentary lifestyle actually does the opposite of what you want, leading to increased pain, fatigue, and weakness.
RELATED: Best and Worst Exercise Trends for Rheumatoid Arthritis
Conditions That Can Mimic Ra
Another reason RA may be tough to diagnose in early stages is that some initial signs and symptoms can be difficult to distinguish from other conditions. Viral infections, other kinds of arthritis, and other autoimmune diseases may all be mistaken for RA, depending on which specific constellation of symptoms you have. Its important to learn about these different diseases so you can be sure to be as specific as possible when describing your medical history to your doctor.
Some of the conditions that mimic rheumatoid arthritis include:
Don’t Miss: What Really Causes Arthritis
When To Get Medical Advice
See a GP if you think you have symptoms of rheumatoid arthritis, so they can try to identify the underlying cause.
Diagnosing rheumatoid arthritis quickly is important, because early treatment can prevent it getting worse and reduce the risk of joint damage.
Find out more about diagnosing rheumatoid arthritis.
What Else Could It Be
When a doctor thinks about how likely you are to have one disease over another, or over several others, this is called a differential diagnosis. There are many conditions your doctor may consider besides RA, and besides other forms of autoimmune arthritis:
Viral arthritis: Rubella, parvovirus, and hepatitis B and C can lead to short-term arthritis symptoms that resemble RA.
Palindromic rheumatism: Periodic joint inflammation that may lead to RA, lupus, and similar diseases
Polymyalgia rheumatica: This is more common over age 50, generally less painful than RA, and associated more with shoulders and hips.
Also Check: Stiff Hands Treatment
How Do Doctors Diagnose Rheumatoid Arthritis
There is no single test that shows whether you have RA. Your doctor will give you a checkup, ask you about your symptoms, and possibly perform X-rays and blood tests.
Rheumatoid arthritis is diagnosed from a combination of things, including:
- The location and symmetry of painful joints, especially the hand joints
- Joint stiffness in the morning
- Bumps and nodules under the skin
- Results of X-rays and blood tests
General Joint Pain And Stiffness
In addition to morning joint stiffness, you may also experience general joint stiffness throughout the day, especially after a period of inactivity.
Some of the first areas RA stiffness typically affects are the wrists and certain joints in the hands and feet, but its also possible to experience pain and stiffness in your knees or shoulders. Usually, both sides of your body will be affected.
Don’t Miss: Does Ra Cause Back Pain
Other Conditions Associated With Seronegative Patients
A seronegative result along with what are thought to be rheumatoid arthritis symptoms could potentially indicate other conditions altogether. Often times when inflammation is present or consistent it means that the seronegative patient may have osteoarthritis instead of rheumatoid arthritis. This is a common confusion.
Spondyloarthritis conditions are sometimes associated with seronegative rheumatoid arthritis because they are inflammatory. These are conditions like ankylosing spondylitis, reactive arthritis, as well as psoriatic arthritis.
Treatments For Rheumatoid Arthritis In Hands

There are several ways to treat RA in your hands, from medicine to inexpensive home treatments. Talk with your doctor about oral and topical anti-inflammatory medications that may help and surgical options. You may also want to change your diet or purchase some inexpensive items that could help, such as arthritis gloves.
Also Check: Arthritis In Knuckles Relief
What Is Treat To Target
T2T is a term that experts use to describe treating a disease while keeping very specific goals in mind. In other words, its a methodical way to make decisions regarding treatment. It involves several steps:
Choosing a target, or goal, for treatment
Making a change to treatment if the target is not met
T2T starts with shared decision-making, meaning you and your rheumatologist will work together to come up with a plan. For example, if you were recently diagnosed with RA, and its time to start treatment, you and your healthcare provider would have a discussion based on the points above. This would include your goal for treatment, what medication to start, and how and when to decide if its working.
Take This Test: Do You Have Rheumatoid Arthritis
Related Article
The most common cause for a swollen knee in a young woman?
A swollen knee in a young woman needs a reason. Whats the most common cause? Actually, I dont know the answer to that exactly. But when a 30-something year-old presents to her doctor with a swollen knee thats stiff and …
Like this article? Share the love!
Take this test: Do you have Rheumatoid Arthritis?
Lots of people have joint pain or other joint problems. Most of the time, there are not due to rheumatoid arthritis .
There is no single test to diagnose RA. The diagnosis is made from a combination of clinical symptoms and findings, supported by various blood tests .
However, you can try this arthritis screen to determine the likelihood of having the disease by this series of questions which may act as a rheumatoid arthritis test.
Also Check: Ra Symptoms In Legs
Talk To Your Healthcare Provider
RA is a chronic disease that doesnt currently have a cure. That said, most people with RA dont have constant symptoms. Instead, they have flare-ups followed by relatively symptom-free periods called remissions.
The course of the disease varies from person to person, and symptoms can range from mild to severe.
Though symptoms may stop for extended periods, joint problems caused by RA will usually get worse over time. Thats why early treatment is so important to help delay serious joint damage.
If youre experiencing any symptoms or have concerns about RA, talk to your healthcare provider.
Nutritional Supplements And Dietary Changes
There is no strong evidence to suggest that specific dietary changes can help improve rheumatoid arthritis, although some people with rheumatoid arthritis feel that their symptoms get worse after they have eaten certain foods.
If you think this may be the case for you, it may be useful to try avoiding problematic foods for a few weeks to see if your symptoms improve. However, it is important to ensure your overall diet is still healthy and balanced.
There is also little evidence supporting the use of supplements in rheumatoid arthritis, although some can be useful in preventing side effects of medications you may be taking. For example, calcium and vitamin D supplements may help prevent osteoporosis if you are taking steroids and folic acid supplements may help prevent some of the side effects of methotrexate.
However, there is some evidence to suggest that taking fish oil supplements may help reduce joint pain and stiffness caused by rheumatoid arthritis.
Want to know more?
You May Like: How To Ease Arthritis Pain In Fingers
Rest When You’re Tired
The disease itself causes fatigue. And the strain of dealing with pain and limited activities also can make you tired. The amount of rest you need depends on how bad your symptoms are.
- With severe symptoms, you may need long periods of rest. You might need to rest a joint by lying down for 15 minutes several times a day to relax. Try to find a balance between daily activities that you must do or want to do and the amount of rest you need to do those activities.
- Plan your day carefully, including rest periods. Pace your activities so that you don’t get overtired.
Rheumatoid Arthritis Causes And Risk Factors
The cause of rheumatoid arthritis is not fully understood, however there are certain risk factors that play a role:
- Rheumatoid arthritis can develop at any age and affects women more than men. Roughly 75% of patients with rheumatoid arthritis are women.
- Genetics can play a role in the development of rheumatoid arthritis. Those with a family history of RA have a slightly higher risk, about 5%, of developing RA compared to individuals without a family history.
- Smoking is a significant risk factor for developing RA.
Read Also: Can Osteoarthritis Turn Into Rheumatoid Arthritis
Where The Fda And Cdc Stand
According to the CDC, people ages 50 and up and immunocompromised adults ages 19 and older should get two doses of Shingrix to prevent shingles, PHN, and other possible complications. Shingrix is effective and safe for most people, including people with autoimmune disorders.
The CDC currently recommends that people with chronic medical conditions, such as RA, get the shingles vaccine. Additional CDC guidelines for people with autoimmune conditions are as follows:
- Shingrix is usually delivered in two doses, two to six months apart. If you are immunocompromised, your healthcare provider may suggest that you get your second Shingrix dose after just one to two months instead.
- Its usually best to wait until your symptoms are well-controlled to get Shingrix. If youre currently having a severe RA flare-up, you should typically wait until you feel better to get the shingles vaccine.
- If youre taking immunosuppressants to manage RA symptoms, talk to your healthcare provider about the vaccine schedule that works best for you.
The Food and Drug Administration approved the use of Shingrix in 2017 for people ages 50 and older. In 2019, the FDA approved Shingrix for immunocompromised adults ages 18 and older. The FDA hasnt yet issued any specific guidelines about Shingrix and RA.
Forgetting To Protect Your Joints
Joint protection is an important part of any treatment program for RA. The goal is to reduce pain, prevent deformity, stabilize the joints, and reduce stress on the joints. This is accomplished through the use of splints, braces, or assistive devices exercise proper body mechanics pacing your activities and modifying your environment if necessary. Failure to protect your joints can make RA worse.
RELATED: 8 Ways to Prevent Rheumatoid Arthritis Joint Damage
Read Also: What Can You Do To Help Arthritis In Your Hands
Neglecting Your Oral Health
Research suggests that tooth loss may predict RA and its severity. Researchers who have studied the connection between RA and periodontal disease discovered similarities in the joint and oral tissues, and in the inflammatory processes that affect them. The types of cells that infiltrate both tissues of the joints in RA and of the mouth in periodontitis a progressive form of gum disease are similar. Also, the levels of pro-inflammatory proteins, such as tumor necrosis factor , interleukin-1, and interleukin-6, are also similar in both RA and periodontitis. There are potential consequences when oral health is neglected.
RELATED: Rheumatoid Arthritis and Gum Disease: What You Need to Know
Medicines To Relieve Symptoms
- Non-steroidal anti-inflammatory drugs such as aspirin, ibuprofen, and naproxen. NSAIDs are used to control pain and may help reduce inflammation. They don’t control the disease or stop it from getting worse. NSAIDs may be combined with DMARDs.
- Corticosteroids such as prednisone. These medicines are used to reduce disease activity and joint inflammation. But using only corticosteroids for an extended time is not considered the best treatment. Corticosteroids are often used to control symptoms and flares of joint inflammation until DMARDs reach their full effectiveness.
- Analgesics . These don’t reduce inflammation but may help with pain control. They include:
Recommended Reading: Ra And Pain
Why Diagnosing Ra Is Difficult For Rheumatologists
There are many other stories of RA misdiagnoses, including delays in reaching the correct diagnosis for patient Jeff Krakow and the Canadian snowboarder Spencer OBrien. Why is it so hard for doctors to get it right?
Scott J. Zashin, MD, a rheumatologist based in Dallas, explains how RA can seem difficult to diagnose. When patients present with signs and symptoms of an inflammatory arthritis and have a positive rheumatoid factor or anti-CCP antibody, the diagnosis is very clear. The more difficult diagnosis occurs when the patient may not have clear-cut swelling or RA markers are negative,” he says.
A new diagnostic antibody test, the 14-3-3 ETA, reported on in June 2017 in the Annals of the Rheumatic Diseases, may help in some cases, but it is still being researched and is not commercially available everywhere. “Because it is a more expensive test,” says Zashin, “I reserve it for patients in whom the diagnosis is not confirmed. And, he adds, In some patients, the joint symptoms are felt to be due to a viral cause. But when the symptoms persist after three or four months, a more chronic type of arthritis like RA must be considered.
How Diet Affects Ra
Although there is no demonstrable link between diet and RA, studies have shown that the type of inflammation experienced in RA could be modulated by certain foods. Increased inflammation has been attributed to processed foods or foods cooked at higher temperatures.
It is recommended to increase consumption of foods that are considered to be anti-inflammatory, such as fruits, veggies, and cold water fish . As a result, inflammatory symptoms may improve and possibly lead to fewer flare-ups.
Read Also: Ra Hand Pain
Ra Quiz: Can You Identify Early Rheumatoid Arthritis
Early rheumatoid arthritis is, in part, defined as having symptoms for at least six months. Beyond six months, it’s considered established rheumatoid arthritis. But diagnosing early rheumatoid arthritis is not that straightforward. Serologic tests can confirm a clinical diagnosis, but these tests aren’t always reliable and can be negative in about 50 percent of rheumatoid arthritis cases. In this quiz, we focus on the diagnosis and treatment of early rheumatiod arthritis.
Early rheumatoid arthritis is, in part, defined as having the symptoms of rheumatoid arthritis for at least six months. Beyond six months, it’s considered established rheumatoid arthritis. But diagnosing early rheumatoid arthritis is not that straightforward. Serologic tests can confirm a clinical diagnosis, but these tests aren’t always reliable and can be negative in about 50 percent of rheumatoid arthritis cases. In this quiz, we focus on the diagnosis and treatment of early rheumatiod arthritis.
The diagnosis of early rheumatoid arthritis must be confirmed by signs of joint erosion and rheumatoid nodules. True or False?
Re: “2015 American College of Rheumatology Guideline for the Treatment of Rheumatoid Arthritis”
False. In patients with early rheumatoid arthritis, the classic signs of established RA—such as joint erosion and rheumatoid nodules—are not evident. These are signs usually seen in patients with longstanding, poorly controlled disease.