What Are The 5 Worst Foods To Eat If You Have Arthritis
Here are 8 foods and beverages to avoid if you have arthritis. Added sugars. You should limit your sugar intake no matter what, but especially if you have arthritis. Processed and red meats. Gluten-containing foods. Highly processed foods. Alcohol. Certain vegetable oils. Foods high in salt. Foods high in AGEs.
Clinical Diagnosis Of Inflammatory Arthritis Is Not Always Straightforward
The history of swelling in joints, early morning stiffness lasting > 30 minutes, systemic symptoms such as tiredness combined with objective evidence of synovitis would favour a diagnosis of inflammatory arthritis . However, reality can be more complex:
-
Objective signs may be lacking or have been suppressed by anti-inflammatory medication
-
Joint swelling can be difficult to identify in obese patients
-
The sensation that joints are swollen may be reported even by some patients with fibromyalgia
-
Osteoarthritis as well as RA can cause morning stiffness, though in osteoarthritis it usually lasts less than 30 minutes
-
Inflammatory markers such as the ESR or C-reactive protein are normal in about 60% of patients with early RA
-
In a patient with preceding osteoarthritis, radiographic changes can be misleading, especially if those suggestive of inflammatory arthritis have not yet developed.
How Is Rheumatoid Arthritis Diagnosed
Your doctor will diagnose rheumatoid arthritis after asking questions about your symptoms and looking at your painful or swollen joints. It is likely your doctor will recommend blood tests, including checking your blood levels of antibodies called rheumatoid factor and anti-cyclic citrullinated peptide , as well as some markers of inflammation called erythrocyte sedimentation rate and C-reactive protein . A high result in any of these blood tests may suggest that you have rheumatoid arthritis.
Your doctor may also recommend x-rays or other scans to help make a diagnosis.
If your doctor thinks that you may have rheumatoid arthritis, they will refer you to a rheumatologist, who is a doctor that specialises in joints.
Starting treatment for rheumatoid arthritis as soon as possible is important as it reduces the chance that you will have serious symptoms later.
Also Check: What Does Ra Feel Like
When Should I See My Doctor
If you notice symptoms of rheumatoid arthritis, or you are concerned that you may have rheumatoid arthritis, you should see your doctor as soon as possible. Your doctor may refer you to a rheumatologist who is a doctor that specialises in joints. It is important to act quickly. The sooner you start treatment, the less likely you are to experience permanent joint damage and deformity.
Research And New Developments
We have recently funded research into palindromic rheumatism, which has given new insights into what goes on in the body during an attack or flare and the experiences of people with the condition.
This research used the latest ultrasound and MRI techniques to show that the structures around the outside of the joints are major targets in flares of palindromic rheumatism, and can be affected more than the joint itself. This pattern of inflammation isnt usually seen in rheumatoid arthritis and might allow doctors to better identify people with palindromic rheumatism.
Its hoped that a better understanding of the condition will improve ways of managing it and help in developing new treatments.
You May Like: What Does Arthritis In The Back Feel Like
Early Detection And Diagnosis
As with most diseases, early detection and diagnosis are crucial for being able to treat symptoms, manage pain, and slow progression. An early diagnosis of RA can help you and your team of physicians and specialists put together an individualized treatment plan so that you can continue living a high quality of life.
Early on, you will want to discuss your case with a rheumatologist or RA specialist who can provide you with the treatment you need to delay the diseases progression. Generally, early diagnosis treatment is aggressive and targeted to properly manage the disease and prevent it from progressing.
If your RA was diagnosed in the early stage when symptoms first appeared, your chances of achieving longer periods of remission typically increase drastically. Thats not to say you wont experience flare-ups. Early diagnosis simply helps manage the disease and cannot guarantee the complete elimination of symptoms.
What Treatment Options Are Available For Ra
There are medications that help manage RA symptoms and control inflammation, such as NSAIDs, corticosteroids, disease-modifying anti-rheumatic drugs, and biologics. However, there are non-medication treatment options as well. Non-pharmacologic treatment options include rest, exercise, physical and occupational therapies, dietary management, and, in some cases, surgery.
Don’t Miss: Symptom Of Arthritis
How Is Sustained Remission Defined
RA is characterized by chronic, progressively destructive inflammation. Disease activity and flares over time are associated with disease progression, functional deterioration and development of radiographic damage. Hence, the primary target of treatment of RA is to achieve clinical remission., It has been proved that the target-steered approach in the management of RA conveys better outcomes than routine care. It is likely that stable remission could be a stronger predictor of a better RA prognosis than remission at a single timepoint. Conceptually, remission and absence of disease, chronic by its nature, should include a time perspective and should be defined at an individual patient level in clinical practice.
According to the recommendations on RA management, regular monitoring of disease activity should guide decisions on choice and changes in therapy to reach a state of clinical remission. The treatment target is moved forward to the goal of maintenance of remission in the last 2016 update of the EULAR treatment recommendations. As a developing definition, a minimum of 6 months is mentioned as a time frame for the target-state of sustained remission. However, the strict approach of sustained remission could only be recommended after validation of application of this criterion in prospective RA clinical settings if the preselected remission duration could differentiate the long-term outcomes.
Symptoms Of Progressive Rheumatoid Arthritis
Here are some general warning signs and symptoms that you may have developed progressive rheumatoid arthritis:
The active state of the disease is becoming more frequent Flare-ups are occurring regularly and lasting for longer periods of time Your pain and swelling are becoming more intense, spreading throughout other areas of your body Your diagnosis occurred early on, and so the disease has had a long time to develop You are beginning to develop rheumatoid nodules that you didnt have before Your blood tests show high levels of Rheumatoid Factor or anti-CCP
If you suspect that your rheumatoid arthritis has become progressive, consult your rheumatologist to determine the changes in your condition and discuss potential adjustments to your treatment plan.
You May Like: Rheumatoid Arthritis And Muscle Cramps
How Your Ra Treatment Plan Prevents Disease Progression
Perhaps the biggest factor that affects how RA progresses is if youre in treatment with a specialist who can put you on medications to slow the disease. Being on a DMARD or biologic therapy for RA is the best way to prevent progression, Dr. Lally says.
Disease-modifying anti-rheumatic drugs are usually the first line in medication. Methotrexate is the anchor drug for rheumatoid arthritis, Dr. Bhatt says. Some patients are scared because methotrexate is also used for cancer chemotherapy so they dont want to take a chemo pill, but those we use for RA are a very small dose with lesser chance of side effects. Your doctor will reassess in a month or so and see if its necessary to add in other drugs.
If after three to six months they have still not responded then we progress to medications called biologics, Dr. Bhatt says. These genetically engineered drugs target the inflammation process specifically, and are usually self-injected or infused via IV in your doctors office or a medical center. There are sub-classes and different types, Dr. Bhatt says. Your doctor will try various medications to see which you respond best to.
Not All Patients With ‘early Polyarthritis’ Develop Persistent Disease
When a patient with inflammatory arthritis cannot definitely be labelled as having RA, it becomes important to decide whether the arthritis is likely to remit or to persist. Clearly, if spontaneous remission seems likely, the patient should be spared potentially toxic DMARD therapy. On the other hand, a patient with persistent inflammation should be started promptly on DMARDs since the condition may represent RA in evolution. From the Norfolk Arthritis Register there is evidence that an overwhelming majority of patients with persistent polyarthritis in due course come to satisfy diagnostic criteria for RA . Thus, since joint damage and functional loss occur early, most patients develop these irreversible changes before a definite diagnosis of RA can be made.
How can the clinician predict persistence of disease? Several research groups have tried to identify pointers in patients with early arthritis but their results are not easily combined because of heterogeneity in populations, predictive factors used and duration of follow-up. Among the predictive factors suggested, the most useful seems to be disease duration exceeding 12 weeks: a patient who has had inflammatory joint symptoms for this long is very unlikely to experience a spontaneous remission. Other features suggesting the unlikelihood of remission are positive tests for rheumatoid factor or cyclic citrullinated peptide antibodies and the presence of erosions on radiographs.
Recommended Reading: Can Rheumatoid Arthritis Affect Your Back
Can Arthritis Cause Numbness
Numbness is often a symptom of nerve involvement. For instance, numbness in the arm may be related to nerve irritation in the neck. In such a situation, turning or bending the head to the involved side may increase the symptoms. For example, a pinched nerve in the right side of the neck may cause numbness in the arm and hand when a person attempts to look back over the right shoulder. If nerve irritation becomes more severe, the arm and hand may become weak. A physical examination X-rays and an MRI of the neck and electrodiagnostic tests may be useful in establishing the diagnosis.
Stage : Antibodies Develop And Swelling Worsens
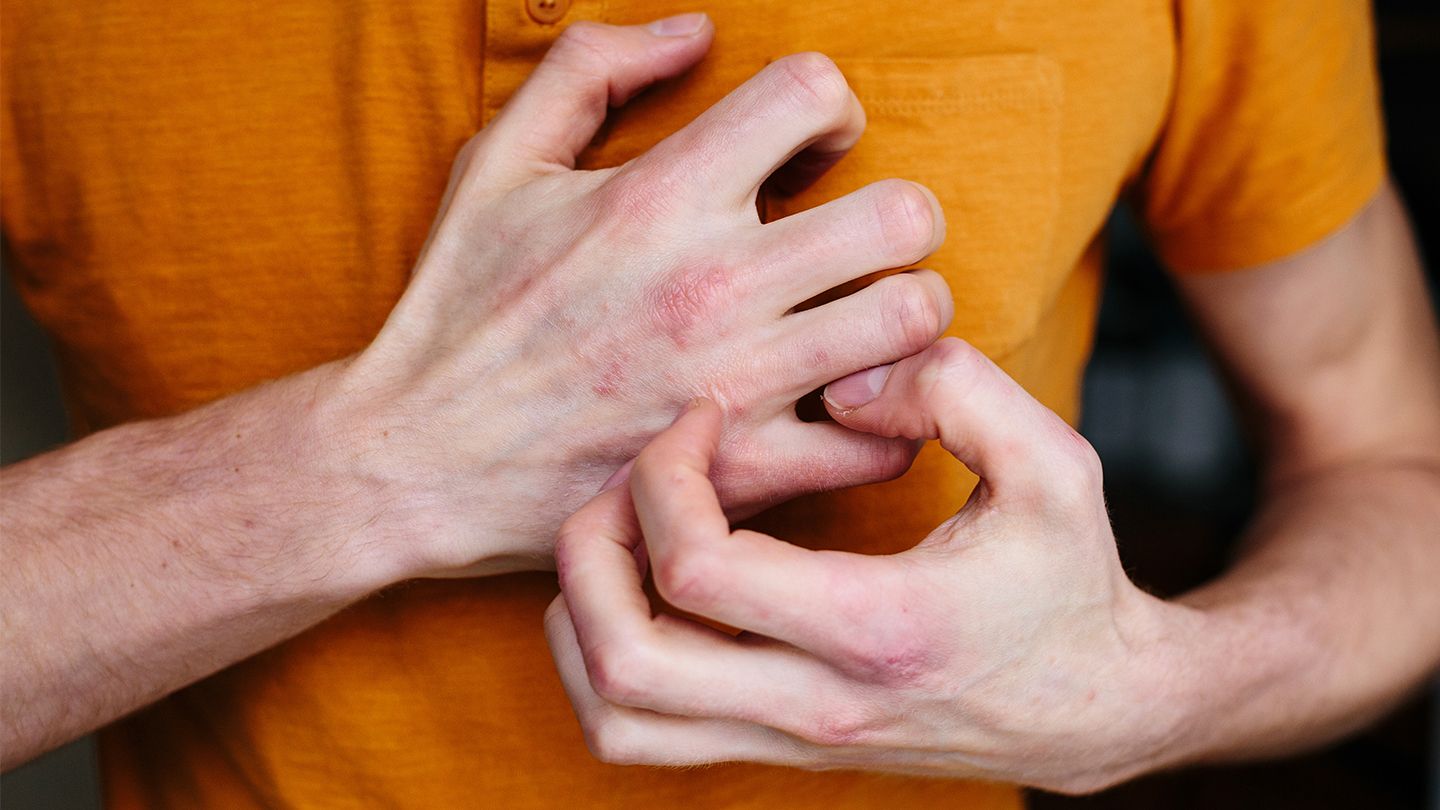
In many cases, RA progresses to the second stage without being diagnosed. In the second stage the body makes the antibodies and the joints start swelling up, Dr. Bhatt says. It can affect other organ systems and cause inflammation there: the lungs, the eyes, a skin rash, and it can even affect the heart. Lumps on the elbows called rheumatoid nodules may also develop.
When it comes to imaging results, the second stage is more confirmative for the diagnosis, Dr. Bhatt says. It has kind of a moth-eaten, chipped off appearance on the X-rays. Ultrasound can also be done, and the most sensitive is an MRI, which would pick up if there are any problems even if the X-ray is normal.
Recommended Reading: Rheumatoid Arthritis Over The Counter Medications
What Are The Complications Of Ra
Rheumatoid arthritis has many physical and social consequences and can lower quality of life. It can cause pain, disability, and premature death.
- Premature heart disease. People with RA are also at a higher risk for developing other chronic diseases such as heart disease and diabetes. To prevent people with RA from developing heart disease, treatment of RA also focuses on reducing heart disease risk factors. For example, doctors will advise patients with RA to stop smoking and lose weight.
- Obesity. People with RA who are obese have an increased risk of developing heart disease risk factors such as high blood pressure and high cholesterol. Being obese also increases risk of developing chronic conditions such as heart disease and diabetes. Finally, people with RA who are obese experience fewer benefits from their medical treatment compared with those with RA who are not obese.
- Employment. RA can make work difficult. Adults with RA are less likely to be employed than those who do not have RA. As the disease gets worse, many people with RA find they cannot do as much as they used to. Work loss among people with RA is highest among people whose jobs are physically demanding. Work loss is lower among those in jobs with few physical demands, or in jobs where they have influence over the job pace and activities.
Is Sustained Remission Uncommon
In general, sustained remission in established RA might be achievable in fewer patients than in early RA, and it is likely not as common in clinical practice as in trials. Higher rates of remission can be achieved in both observational datasets and clinical trials when a treat-to-target strategy is adopted. Currently, there is no definite answer on how often sustained remission could be achieved and how long sustained remission could be maintained because of several different definitions of sustained remission used in the studies.
Firstly, the time frame to assess remission at consecutive visits ranges from two consecutive assessments with at least 1 month apart, to biannual assessments,, annual assessments, or longer periods between assessments. The rate of persistent DAS-based remission in these studies ranges from 545%.
Hence, a definition of accurate timeframes to assess remission is required. This question has been investigated in the recent pooled analysis of patient-level clinical trial data. It has been shown that 3-month changes are critical timepoints for the target of remission , and that type of treatment or early versus established RA did not significantly influence the accuracy of the 3-month changes to predict response. In the observational setting, 3-month monitoring has also been shown as a minimum timeframe to assess remission, taking into account prediction of good functional and good overall outcome.
Don’t Miss: Ra And Tendonitis
When To Get Medical Advice
See a GP if you think you have symptoms of rheumatoid arthritis, so they can try to identify the underlying cause.
Diagnosing rheumatoid arthritis quickly is important, because early treatment can prevent it getting worse and reduce the risk of joint damage.
Find out more about diagnosing rheumatoid arthritis.
Ra Is A Constant Companion
The thing to understand about RA is that it is always there and it is a constant companion for most of us. Some days might better than others, but most of us have pain and symptoms every single day.
I have pain every day. Some days, it is mild, and I can do a lot not as much as someone without RA, but a lot more than usual. Even on the days where it the pain and fatigue are bad, I try to put on my best face and deal with it because I dont have a choice.
There are times where it seems I am flaring all the time and some flares seem to last days or even weeks. And in all these nine years of living with this disease, I have had a handful of flares that have gone on for months.
Recommended Reading: Rollator Knee Scooter
You May Like: Symptoms Of Arthritis In Knees And Legs
Seeking Help When Symptoms Cannot Be Contained
The tipping point for seeking professional help is reached when multiple symptoms cannot be controlled by even increased self-management strategies, and patients cannot run their normal lives . They may be supported or prompted in this decision by family:
When its all over, along with the other symptoms that I know I get with inflammation, thats my personal tipping point
In such a place of despair I think I just cant go on with this anymore and Im trying this medication and Im trying to pace my working, Im trying to have so many hours sleep and Im still waking up in pain. and its still not working
The reason that I end up running back to crying is, Ive got 3 young children and I teach and its where it gets to the point where I cant function any more its got to the point where Im not coping, the household chores just arent being done and I just beat myself up because I cant be like all the other mums and do little things for the kids. If its not me its my husband, hell say You need to go and get some reinforcement and usually I go to the GP .
How Does Treatment Improve Life Expectancy
Early treatment greatly improves the prognosis of RA patients. If treatment begins before symptoms cause too much damage, patients can generally go on to live a better quality of life.
Ongoing treatment and monitoring can help rheumatologists provide the most appropriate and personalized care for their patients. Each patient will experience a different set of symptoms over their lifetime. Doctors look for warning signs of other complications associated with RA and work to either prevent them or treat them as they develop.
The main goal of treatment is to reduce pain and improve quality of life. Many patients experience very effective treatment plans and continue to live their lives making appropriate lifestyle adjustments along the way.
Read Also: Joint Inflammation Cause
Can Rheumatoid Arthritis Spread Quickly
The symptoms of rheumatoid arthritis often develop gradually over several weeks, but some cases can progress quickly over a number of days. The symptoms vary from person to person. They may come and go, or change over time. You may experience flares when your condition deteriorates and your symptoms become worse.
Her Flare Ups Often Come On Over Night Are Very Painful Restrict Mobility And She Has To Rest
The worst type of flare involves pain, stiffness and swelling throughout the body and leaves people incapacitated for several months. These again could start quickly – within a few hours or days but were less frequent. One woman had three of these major flares in 12 years, whilst another said she got them maybe once a year. One young mother said that she has had two major flares’ one before diagnosis and the other after her second baby was born when she has been off medication.
Don’t Miss: How Can I Slow Down Arthritis In My Hands