Practice Better Sleep Hygiene
Tossing and turning at night when unable to sleep may cause a person to notice and fixate on their pain. Good sleep hygiene may help a person fall asleep faster and remain asleep longer. People can try the following:
- going to bed at the same time each night and establishing a bedtime ritual, such as taking a bath, meditating, or doing another calming activity
- avoiding daytime naps
- exercising during the day to ease arthritis symptoms and support better health, but avoiding exercise for 4 hours before bed
- avoiding stimulants such as caffeine and nicotine, especially in the afternoon and evening
- refraining from drinking alcohol or only drinking it in moderation
- developing strategies for managing daytime stress to prevent negative thoughts from keeping a person awake or triggering joint pain
- eating a balanced meal a few hours before bed and trying a light snack just before bed if nighttime hunger is a problem
- using the bed only for sleeping and sex and not for watching television or doing work
- keeping the bedroom cool and dark, potentially by using blackout curtains
- investing in a comfortable, supportive mattress and quality pillows
- trying different pillow positioning, such as putting a pillow between the knees or under the hips, to ease joint pain
While they are working on improving their sleep hygiene, a person may find it helpful to get back up if they cannot fall asleep. Doing this helps the association between bed and sleep remain strong.
Tips For Dealing With Arthritis Pain In Winter
How many times have you sworn that a storm was coming because your arthritis pain was flaring up? How many times has a bone-chilling cold caused your joints to swell and get inflamed with pain and stiffness?
Winter weather can be especially tough for those who suffer from arthritis, and there could be some truth to the old wives tale that aching joints can be an indicator of a change in weather. In fact, the Arthritis Foundation even cites studies that show lower barometric pressure caused more aches and pains for people in barometric pressure chambers.
Arthritis can be classified as either inflammatory or non-inflammatory. Inflammatory arthritis features inflammatory white blood cells in the joint fluid. Forms of inflammatory arthritis include rheumatoid arthritis, lupus arthritis, gout, and many others. Forms of non-inflammatory arthritis include osteoarthritis, arthritis of thyroid disease, arthritis after injury and many others. Studies have shown that cold weather can affect both inflammatory and non-inflammatory arthritis.
With winter in full swing, cold weather pain and arthritis can be uncomfortable and affect your quality of life. The cold doesnt cause arthritis, but it can increase joint pain, according to the Arthritis Foundation. Here are some great tips to deal with arthritis pain during the winter months.
1. Stay warm and layer up
2. Eat a healthy diet
3. Get your stress under control
4. Stay active and exercise
6. Get your vitamin D
Talking About Arthritis Pain
Help guide your arthritis pain treatment by learning how and what to communicate to your doctor.
Talking About Arthritis Pain
When you live with chronic pain, the only one who can know how much it hurts is you. Pain can be hard to describe because its both invisible and personal. If you cant put into words how much pain youre in or how it affects your life, your doctor cant prescribe the right treatment for you.
Use this guide to help you talk to your doctor about your arthritis pain so you can get the relief you need.
What Does the Pain Feel Like?
Be as specific as possible about how your pain feels to help your doctor figure out whats wrong.
Here are a few words you can use to describe the way your pain feels, and how your doctor might interpret them:
-
Aching, dull: muscle strains, arthritis pain
-
Shooting, electric, tingling, burning, pins-and-needles: nerve pain
-
Sharp, stabbing: injuries such as a broken bone, muscle or ligament tear, or penetrating wound
-
Throbbing: headache, abscess, gout
-
Tightness: muscle spasm
Where Do You Have Pain?
Describe exactly where you hurt and how that that may or may not change to your doctor.
Here are a few examples:
-
Deep in your shoulder joint or in the muscles near the surface.
-
Under the kneecap or in the back of the knee.
-
The outside of your hip or in your groin.
-
Is the pain in only one spot, or does it travel?
-
Does the pain remain steady, come and go, or only flare up when you move in a certain way?
How Much Does it Hurt?
Recommended Reading: Is Ra Painful
Other Types Of Joint Disease
Sometimes osteoarthritis is a result of damage from a different kind of joint disease, such as rheumatoid arthritis or gout.
Two factors that may affect the symptoms of osteoarthritis, but arent a direct cause of it are the weather and diet:
Weather
Many people with osteoarthritis find that changes in the weather make the pain worse, especially when the atmospheric pressure is falling for example, just before it rains. Although the weather may affect the symptoms of your arthritis, it doesnt cause it.
Diet
Some people find that certain foods seem to increase or lessen their pain and other symptoms. However, your weight is more likely than any other specific dietary factors to affect your risk of developing osteoarthritis.
Read more about osteoarthritis of the spine.
Advanced Glycation End Products
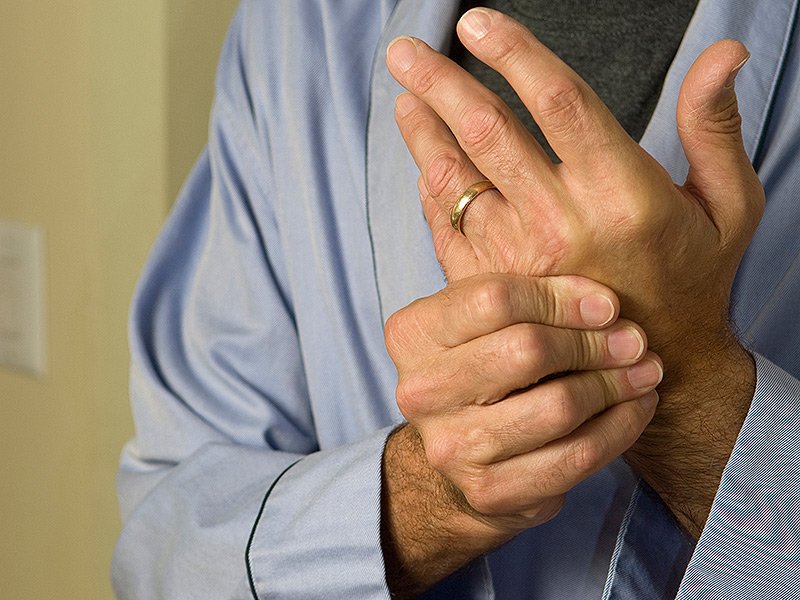
AGEs are inflammatory compounds that can accumulate in tissues, particularly as someone ages. An article in Patient Education explains that people with diseases such as diabetes and RA often have increased AGE levels. So, reducing AGE levels may help reduce inflammation.
Fat and sugar both increase AGE levels in the body. Some food processing methods and high temperature cooking also increase the AGE levels in food.
Read Also: Polyarthritis Causes
What This Means For Stem Cell Treatments For Arthritis In The Hips
Based on our registry data, we know that hips are the one joint in which the severity of arthritis is a factor, and on average, patients with severe arthritis dont respond as well to same-day stem cell treatments as those with severe knee arthritis. While this may be the norm, it doesnt mean that all severe hip arthritis patients do not respond, as of the patients weve treated with severe hip arthritis, some have done much better than expected, especially younger patients. However, those with mild or moderate hip arthritis do tend to respond with more success than those with severe arthritis to same-day stem cell treatments.
The fact that arthritis of the hip occurs and progresses rapidly and is so closely associated with BMLs and bone cysts suggests to us that hip arthritis is as much a bone disease as it is a joint disease, so, importantly, stem cell treatments should be focused not only on the joint but also the bone. And because as weve discussed, hips have fewer local stem cells than the knees and lack the same ability to self-repair, this, again, emphasizes the importance of early intervention with a diagnosis of arthritis in the hip, as once it gets to the point of severe hip arthritis in patients over 55, treating it nonsurgically can be much more challenging, and may not be possible. Our candidacy ratings for hip arthritis reflect these findings.
What Causes Chronic Knee Pain
Temporary knee pain is different from chronic knee pain. Many people experience temporary knee pain as a result of an injury or accident. Chronic knee pain rarely goes away without treatment, and it isnt always attributable to one incident. Its most often the result of several causes or conditions.
Physical conditions or diseases can cause knee pain. These include:
- osteoarthritis: pain, inflammation, and joint destruction caused by degeneration and deterioration of the joint
- tendinitis: pain in the front of the knee that is made worse when climbing, taking stairs, or walking up an incline
- bursitis: inflammation caused by repeated overuse or injury of the knee
- Bakers cyst: a buildup of synovial fluid behind the knee
- rheumatoid arthritis : a chronic autoimmune inflammatory disorder that causes painful swelling and can eventually cause joint deformity and bone erosion
- dislocation: dislocation of the kneecap most often the result of trauma
- meniscus tear: a rupture in one or more of the cartilage in the knee
- torn ligament: tear in one of the four ligaments in the knee the most commonly injured ligament is the anterior cruciate ligament
- bone tumors: osteosarcoma , most commonly occurs in the knee
Factors that may make chronic knee pain worse:
- injuries to the structure of the knee can cause bleeding and swelling and can create a chronic problem over time if not treated properly
- injections
Donât Miss: Can Arthritis Cause A Rash
Read Also: Is Ra Curable
Stop Avoiding Mobility Aids
A cane, walker, or wheelchair may be necessary for some people with arthritis to stay independent and get around on their own. Understandably it can be tough to think about needing some sort of mobility aid, but if you do need one and don’t use it you risk missing out on things you would enjoy.
A cane or wheelchair doesn’t define who you are, and no one will judge you or think less of you for using one. In fact, you’ll probably be admired for getting out there and having fun in spite of needing a little help.
Problems With Old Assessments
After diagnosis, the level and progression of RA need to be monitored and tracked. Prior to RASS, doctors combined results from a physical examination with factors reported by the patient, such as pain level, and inflammatory blood markers, to estimate RA severity.
Doctors also used the Health Assessment Questionnaire , in which patients rated their own level of pain. Of course, everyone has a different threshold for pain, which can make these assessment models inaccurate. These assessment methods were also complicated by a close relationship between pain and depression.
Depression can be a significant component of RA. But there are challenges with using it to measure disease severity, including:
- some patients may be more depressed than others
- some patients may feel particularly depressed at the time of examination
- some patients may not acknowledge they are depressed
While depression can be an element of RA, measuring it is not helpful for disease activity assessment. The RASS is completed by your doctor and based on the visible signs of the disease. Its not based on your individual emotional assessment.
Its important to know what type of RA you have to get an accurate assessment of disease activity. There are three types of RA:
- rheumatoid factor positive
- rheumatoid factor negative
- juvenile RA
The RASS measures three areas:
- disease activity
- functional impairment
- physical damage
Also Check: Arthritis Symptoms Arms And Hands
Arthritis With Involvement Of The Connective Tissues
Connective tissues include tendons, ligaments and cartilages. When someone suffers from arthritis, it is possible that the inflammatory process extends and affects the connective tissues as well.
In such situations, the leg pain becomes more severe and the overall functionality is severely reduced.
As opposed to other types of arthritis, this type is progressive the inflammation becomes worse with the passing of time and it can affect not only the connective tissues and joints but also the muscles, skin and vital organs, such as the lungs and the kidneys.
Examples of such medical conditions include systemic sclerosis, SLE and dermatomyositis.
Leading A Sedentary Lifestyle
Regular physical activity is necessary for everyone, including people with RA, and there are numerous health benefits associated with it. Improved muscle strength, as well as better bone and joint health, is essential for people with RA. Rest is also needed, to restore the body from the episodes of intense pain and fatigue that are characteristic of RA. But rest cant become a way of life striking a balance between rest and activity is optimal. A sedentary lifestyle actually does the opposite of what you want, leading to increased pain, fatigue, and weakness.
RELATED: Best and Worst Exercise Trends for Rheumatoid Arthritis
Also Check: Finger Joint Swelling Treatment
Should I See A Specialist
Its unlikely that youll need to see a specialist to get a diagnosis of osteoarthritis, although your doctor may refer you if theres some doubt about the diagnosis or if they think there might be additional problems.
Your doctor may refer you if specialist help is needed to manage your osteoarthritis this might be for physiotherapy, podiatry for foot problems, or occupational therapy, which can help if youre having difficulty with everyday activities.
If your arthritis becomes severe and is causing long-term problems, your GP may refer you to an orthopaedic surgeon to consider joint surgery or to a pain management programme.
- supplements and complementary treatments.
How Is Arthritis Treated
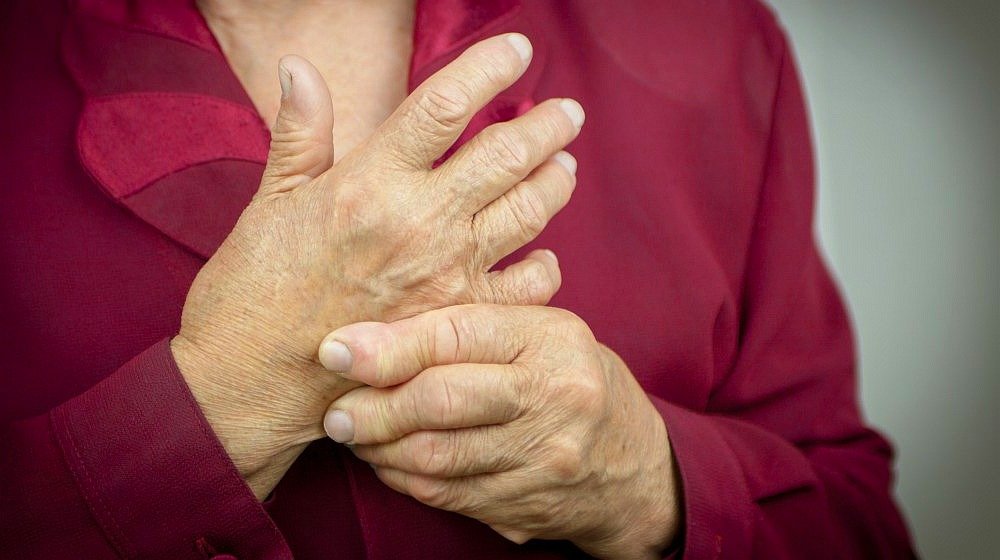
Theres no cure for arthritis, but there are treatments that can help you manage the condition. Your treatment plan will depend on the severity of the arthritis, its symptoms and your overall health.
Conservative treatments include:
- Medication: Anti-inflammatory and pain medications may help relieve your arthritis symptoms. Some medications, called biologics, target your immune systems inflammatory response. A healthcare provider may recommend biologics for your rheumatoid or psoriatic arthritis.
- Physical therapy: Rehabilitation can help improve strength, range of motion and overall mobility. Therapists can teach you how to adjust your daily activities to lessen arthritic pain.
- Therapeutic injections: Cortisone shots may help temporarily relieve pain and inflammation in your joints. Arthritis in certain joints, such as your knee, may improve with a treatment called viscosupplementation. It injects lubricant to help joints move smoothly.
You May Like: What Can I Do For Arthritis In My Hands
What Is A Joint And How Does It Work
A joint is where two or more bones meet, such as in the fingers, knees, and shoulders. Joints hold bones in place and allow them to move freely within limits.
Most of the joints in our body are surrounded by a strong capsule. The capsule is filled with a thick fluid that helps to lubricate the joint. These capsules hold our bones in place. They do this with the help of ligaments. These are a bit like very strong elastic bands.
The ends of the bones within a joint are lined with cartilage. This is a smooth but tough layer of tissue that allows bones to glide over one another as you move.
If we want to move a bone, our brain gives a signal to the muscle, which then pulls a tendon, and this is attached to the bone. Muscles therefore have an important role in supporting a joint.
Treatment Goals: Manage Pain And Improve Function
Osteoarthritis treatment plans often include exercise, rest and joint care, pain relief, weight control, medicines, surgery, and complementary treatment approaches. Current treatments for osteoarthritis can relieve symptoms such as pain and disability, but there are no treatments that can cure the condition.
Although health care professionals can prescribe or recommend treatments to help you manage your arthritis, the real key to living well with the disease is you. Research shows that people with osteoarthritis who take part in their own care report less pain and make fewer doctor visits. They also enjoy a better quality of life.
Also Check: How To Get Rid Of Arthritis In Wrist
What Is The Worst Case Scenario With Rheumatoid Arthritis
You may be wondering if RA gets worse with age. Progressive rheumatoid arthritis may result in the destruction of joint structures, limiting function and mobility.
In the worst cases, fingers may become bent, shortened and misaligned. Patients with end-stage rheumatoid arthritis may require assistance with the activities of daily living and may need a walker or wheelchair for ambulation.
According to WebMD, RA can result in inflammation of the knees requiring surgical knee replacement, damage to the structures in the cervical spine, or damage to organs such as the eyes or lungs.
Rheumatoid arthritis may also contribute to coronary artery disease by speeding the development of arterial plaque. This may increase the risk of stroke if these plaques build up in the arteries of the head and neck.
Some medicines often prescribed to treat rheumatoid arthritis may contribute to the risk of osteoporosis, which can cause further debilitation and lack of mobility.
According to the Arthritis Foundation, arthritis medications may contribute to hair loss, although this may also be attributed to the disease itself.
The RA medication Methotrexate is believed to be responsible for the hair loss in up to 3 percent of patients who take the drug.
When To Call Your Doctor
Dr. Cotter urges anyone who experiences sudden symptoms of arthritis to seek medical attention immediately. If left untreated, these symptoms could lead to long-term problems in the joint.
“It is not normal for a joint to suddenly swell, and getting the correct diagnosis is of the utmost importance,” she says. “Early diagnosis and intervention will mean a better outcome.”
Any persistent issues warrant a call to your doctor as well, she says. For example, if you have joint pain without swelling or joint swelling without pain that persists, you should see your doctor for an evaluation.
Read Also: How To Reduce Arthritis Swelling In Hands
Arthritis With Involvement Of The Soft Tissues
It can happen that the inflammatory process present in the joints of the leg extends to the soft tissues, aggravating the present symptomatology .
When this happens, the whole dynamics of the leg is affected and the patient is prevented from engaging in daily living activities.
*All individuals are unique. Your results can and will vary.
This type of arthritis is common in those who have overused their joints for example, professional athletes, runners, joggers. Physical injuries can trigger the appearance of this form of arthritis as well.
The inflammatory process can stem from the soft tissues as well, affecting the joints as consequence. In making the diagnosis of arthritis, it is important to diagnose the root of the problem and treat it accordingly.
If the leg pain is severe, involving a large surface and being resistant to medication, the condition one is suffering from might be fibromyalgia.