Rheumatoid Arthritis And Your Lungs
The most common RA-related lung complication is interstitial lung disease , a condition that causes inflammation and scarring of the lung tissue. This illness can be hard to detect but occurs when lung tissue becomes inflamed and eventually scarred.
Its unclear exactly how many people with RA develop it, but French researchers presenting an abstract at the American College of Rheumatology annual conference in November 2020 found that the prevalence of subclinical ILD was 18 percent in people who had RA for a dozen years. Other studies put the figure at over 50 percent.
This scarring makes it harder for oxygen in the lungs to enter the bloodstream and travel to other organs. The condition can cause breathlessness and coughing, but it can also be asymptomatic. If untreated, it can progress to pulmonary fibrosis, in which tissues are permanently scarred.
Research also shows that RA sufferers are at double the risk of chronic obstructive pulmonary disease, or COPD , in which the air sacs cant expand as easily and become clogged with mucus. There is no cure for COPD, although inhalers and steroids can help open airways.
Pleurisy is another condition with increased risk. Here, the pleura the tissue surrounding the lungs becomes inflamed, which can lead to fluid buildup at the base of the lungs.
People with RA may also develop nodules in the lungs, though they may not be bothered by them.
Living With Rheumatoid Arthritis
There is no cure for RA. But it is important to help keep your joints working well by reducing pain and inflammation. Work on a treatment plan with your healthcare provider that includes medicine and physical therapy. Work on lifestyle changes that can improve your quality of life. Lifestyle changes include:
- Activity and rest. To reduce stress on your joints, switch between activity and rest. This can help protect your joints and lessen your symptoms.
- Using assistive devices. Canes, crutches, and walkers can help to keep stress off certain joints and to improve balance.
- Using adaptive equipment. Reachers and grabbers let you extend your reach and reduce straining. Dressing aids help you get dressed more easily.
- Managing the use of medicines. Medicines for this condition have some risks. Work with your healthcare provider to create a plan to reduce this risk.
- Seeking support. Find a support group that can help you deal with the effects of RA.
Nutritional Supplements And Dietary Changes
There is no strong evidence to suggest that specific dietary changes can help improve rheumatoid arthritis, although some people with rheumatoid arthritis feel that their symptoms get worse after they have eaten certain foods.
If you think this may be the case for you, it may be useful to try avoiding problematic foods for a few weeks to see if your symptoms improve. However, it is important to ensure your overall diet is still healthy and balanced.
There is also little evidence supporting the use of supplements in rheumatoid arthritis, although some can be useful in preventing side effects of medications you may be taking. For example, calcium and vitamin D supplements may help prevent osteoporosis if you are taking steroids and folic acid supplements may help prevent some of the side effects of methotrexate.
However, there is some evidence to suggest that taking fish oil supplements may help reduce joint pain and stiffness caused by rheumatoid arthritis.
Want to know more?
Recommended Reading: Rheumatoid Arthritis Longterm Effects
Causes Of Rheumatoid Arthritis
Doctors donât know the exact cause. Something seems to trigger the immune system to attack your joints and, sometimes, other organs. Some experts think a virus or bacteria may change your immune system, causing it to attack your joints. Other theories suggest that in some people, smoking may lead to rheumatoid arthritis.
Certain genetic patterns may make some people more likely to get RA than others.
Rheumatoid Arthritis Signs And Symptoms
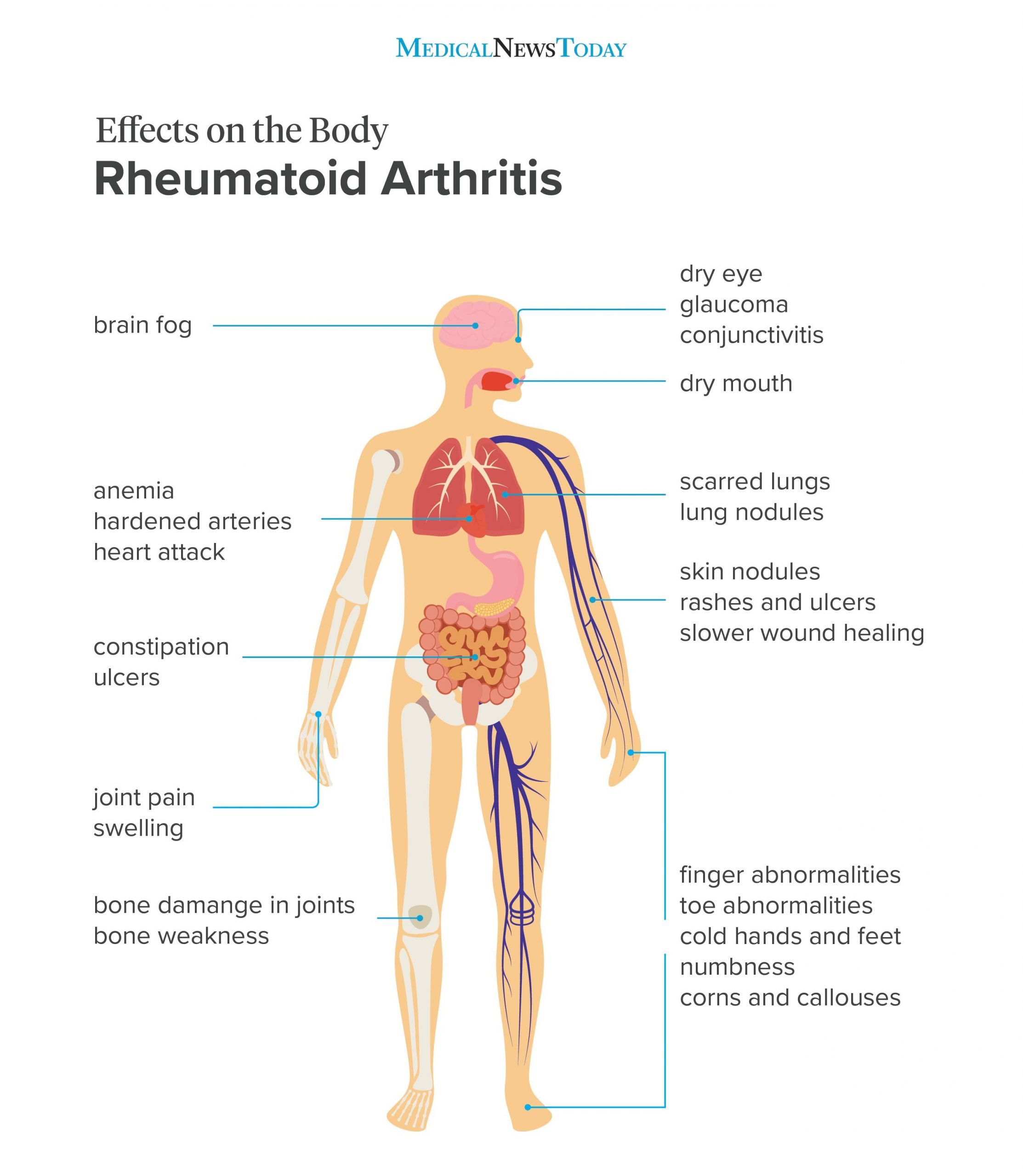
The most commonly affected joints are the fingers, wrists, knees, ankles and feet . Common symptoms include:
- Morning stiffness
- Joint pain
- Joint deformation
- Pleurisy
- Dry eyes and mouth
- Anaemia
Symptoms either begin suddenly or come on gradually, and are typically more severe than osteoarthritis. Main areas of discomfort are the hands, wrists, knees, ankles, feet, shoulders, elbows, neck and jaw. Joint swelling is also typically constant which affects the ability to comfortably perform an array of daily tasks, such as walking or driving. If ill managed symptoms can affect organs such as the heart, lungs and eyes, causing further complications.
You May Like: Does Psoriatic Arthritis Itch
Stick To Your Prescribed Rheumatoid Arthritis Treatment Plan
Medication that helps reduce out-of-control inflammation in the body is a cornerstone of rheumatoid arthritis treatment. Depending on the severity of your symptoms and how long youve had rheumatoid arthritis, your rheumatologist may prescribe a combination of medications. One of the major goals of treatment of RA is to prevent this structural damage that can result in loss of dexterity and strength in the hands, says Dr. Lally.
Commonly prescribed medications include:
Nonsteroidal anti-inflammatory drugs
These medications, such as ibuprofen or naproxen or prescription versions, are used for mild joint pain and reduce inflammation but dont prevent disease progression.
Glucocorticoids
These medications, such as prednisone, help reduce inflammation quickly and tend to be prescribed during flares. They used sparingly and carefully in people with RA because they can have a wide range of side effects.
Disease-modifying anti-rheumatic drugs
These medications address the underlying systemic inflammation in rheumatoid arthritis. They are critical for slowing and stopping the course of inflammatory disease. They fall into three general categories.
The treatments that we have for RA both the conventional DMARDs such as methotrexate and the biologics and JAK inhibitors can help improve joint pain, swelling, and stiffness while preventing the development of long-term damage, adds Dr. Lally.
What Are Tips For Managing And Living With Rheumatoid Arthritis
The following tips are helpful in managing and living with RA:
- Live a healthy lifestyle: Eat healthy foods. Avoid sugar and junk food. Quit smoking, or don’t start. Don’t drink alcohol in excess. These common-sense measures have an enormous impact on general health and help the body function at its best.
- Exercise: Discuss the right kind of exercise for you with your doctor, if necessary.
- Rest when needed, and get a good night’s sleep. The immune system functions better with adequate sleep. Pain and mood improve with adequate rest.
- Follow your doctor’s instructions about medications to maximize effectiveness and minimize side effects.
- Communicate with your doctor about your questions and concerns. They have experience with many issues that are related to rheumatoid arthritis.
Don’t Miss: How To Deal With Arthritis
Who Treats Rheumatoid Arthritis
Diagnosing and treating rheumatoid arthritis requires a team effort involving you and several types of health care professionals. These may include:
- Rheumatologists, who specialize in arthritis and other diseases of the bones, joints, and muscles.
- Primary care providers, such as internists, who specialize in the diagnosis and medical treatment of adults.
- Orthopaedists, who specialize in the treatment of and surgery for bone and joint diseases or injuries.
- Physical therapists, who help to improve joint function.
- Occupational therapists, who teach ways to protect joints, minimize pain, perform activities of daily living, and conserve energy.
- Dietitians, who teach ways to eat a good diet to improve health and maintain a healthy weight.
- Nurse educators, who specialize in helping people understand their overall condition and set up their treatment plans.
- Mental health professionals, who help people cope with difficulties in the home and workplace that may result from their medical conditions.
When Should I Make An Appointment At The Rheumatoid Arthritis Clinic
If you believe yourself to have any of these signs of RA, its best to consult your GP and make an appointment at the rheumatoid arthritis clinic. If you have not previously been diagnosed with RA, your doctor will likely check for:
If you are positive for RA, your doctor will provide you with an immediate treatment plan. Although there are no known cures for RA, its best for you not to worry as the doc will assist you in every way she or he can. Remember to stay healthy in the meantime.
You May Like: Mayo Clinic On Arthritis
What Are Complications Of Rheumatoid Arthritis
Common complications of rheumatoid arthritis include the following:
Overall, the rate of premature death is higher in people with rheumatoid arthritis than in the general population. The most common causes of premature death in people with rheumatoid arthritis are infection, vasculitis, and poor nutrition. Fortunately, the manifestations of severe, long-standing disease, such as nodules, vasculitis, and deforming are becoming less common with optimal treatments.
Rheumatoid Factor And Anti
Specific blood tests can help to diagnosis rheumatoid arthritis, but are not accurate in every person. About half of all people with rheumatoid arthritis have a positive rheumatoid factor present in their blood when the disease starts, but about one in every 20 people without rheumatoid arthritis also tests positive for this.
Another antibody test known as anti-CCP is also available. People who test positive for anti-CCP are very likely to develop rheumatoid arthritis, but not everybody found to have rheumatoid arthritis has this antibody.
Those who test positive for both rheumatoid factor and anti-CCP may be more likely to have severe rheumatoid arthritis requiring higher levels of treatment.
Read Also: Red Swollen Finger Joints
What Is The Patient’s Role In Treating Or Managing Arthritis
The patient is the most important member of the health care team.
The patient plays an important role in his or her medical care. The patient can contribute to the success of a treatment plan by:
- learning about arthritis
- reporting progress and setbacks to health team
- keeping a positive attitude
- developing relationships with the rest of the health care team
Keeping a positive attitude, though sometimes difficult, is an important ingredient in overcoming arthritis. Asking questions and finding out as much as you can about of arthritis and its treatment is important. So talk over your concerns with your doctor. If you still need more information , ask the nurse, physical therapist, social worker, occupational therapist to help you find answers to your questions.
How Rheumatoid Arthritis May Affect Your Mouth
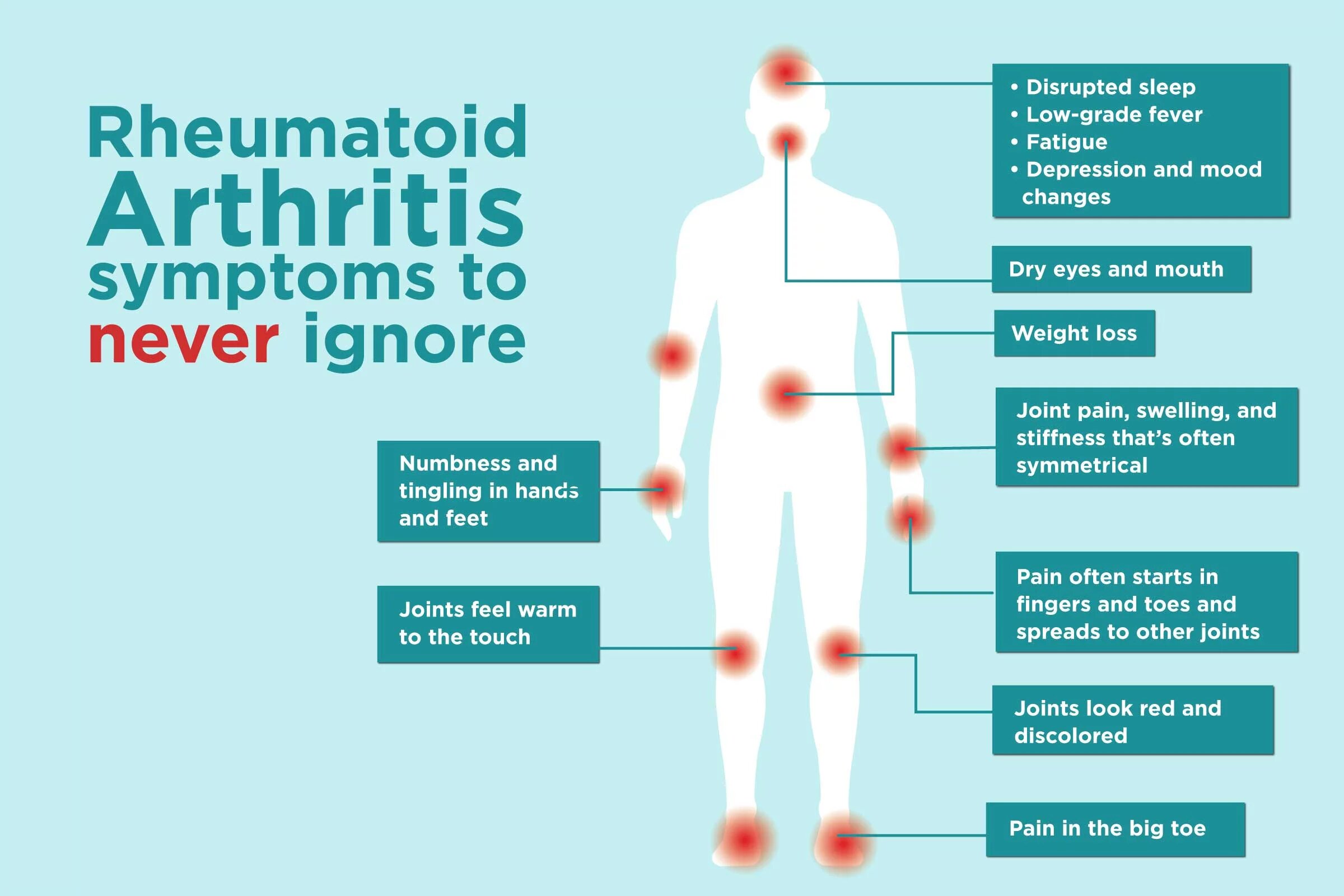
Research shows that people who have rheumatoid arthritis may be more likely to develop periodontal disease, which usually starts with a gum infection.
They are also more likely to have dry mouth, which can predispose them to tooth decay.
The flip side of this may be true too: Poor oral health may lead to the onset or worsening of RA. Experts believe that inflammation in the mouth may stimulate the immune system, and in a people predisposed to RA the inflammation may trigger the body to start making antibodies associated with the disease.
Researchers have been working to better understand the mechanism behind this, but the takeaway is that treating gum disease and preventing unnecessary gum infections is good for your RA, as well. Schedule frequent dental checkups to catch minor issues before they become major problems.
Don’t Miss: Is Banana Good For Arthritis
What Are The Warning Signs Of Arthritis
Pain from arthritis can be ongoing or can come and go. It may occur when you’re moving or after you have been still for some time. You may feel pain in one spot or in many parts of your body.
Your joints may feel stiff and be hard to move. You may find that it’s hard to do daily tasks you used to do easily, such as climbing stairs or opening a jar. Pain and stiffness may be more severe during certain times of the day or after you’ve done certain tasks.
Some types of arthritis cause swelling or inflammation. The skin over the joint may appear swollen and red and feel hot to the touch. Some types of arthritis can also cause fatigue.
What Are The Different Types Of Rheumatoid Arthritis
Symptoms of rheumatoid arthritis usually begin gradually in several joints. Sometimes the symptoms begin only in one joint, and sometimes the symptoms begin initially in the whole body, with generalized stiffness and aching, and then localize to the joints.
- Typical “classic” rheumatoid arthritis is the most common type of rheumatoid arthritis. Classic rheumatoid arthritis involves three or more joints. Usually, people have a gradual onset of joint pain, stiffness, and joint swelling, usually in the fingers, wrists, and forefeet. Elbows, shoulders, hips, ankles and knees are also commonly affected.
- About 80% of people with rheumatoid arthritis are classified as “seropositive,” which simply means the rheumatoid factor blood test is abnormal. Some people with an abnormal rheumatoid factor also have an abnormal anti-CCP blood test. This is another blood test for rheumatoid arthritis.
- Approximately 20% of people with rheumatoid arthritis are classified as “seronegative,” which means the rheumatoid factor blood test is negative, or normal. In this case, the anti-CCP blood test may be abnormal or normal. Other blood tests, such as the ESR measure of inflammation, may be abnormal.
Palindromic rheumatism
Atypical presentations of RA
- Persistent arthritis of just one joint may be the first symptoms of rheumatoid arthritis in some people.
- Some people experience generalized aching, stiffness, weight loss, and fatigue as their initial symptoms of rheumatoid arthritis.
YOU MAY ALSO LIKE
Recommended Reading: Arthritic Pain Symptoms
Talk To Your Doctor About Surgery Options
If pain is unrelenting or there is loss if function in the hands, your rheumatologist may refer you for a surgical evaluation, particularly when theres an anatomic defect that can be corrected, says Dr. Albayda.
Surgery may involve removal of inflamed joint linings, tendon repair, joint fusions, or joint replacements. Depending on the joint involved, the degree of damage, and other factors, you hand surgeon will determine the most appropriate treatment to help correct deformities, relieve pain, or improve function.
How Rheumatoid Arthritis Can Hurt Your Heart
Higher levels of inflammation in people with rheumatoid arthritis increase the risk of heart disease, especially heart attacks and strokes, Greer says.
These heart conditions can also be more fatal. In people with systemic inflammatory diseases like RA, heart attacks in those under 50 are twice as likely to be fatal as for people without an inflammatory condition, according to a study published in the European Journal of Preventive Cardiology in March 2021.
To lower your risk, youll want to get your RA under control and also reduce heart risk factors, such as high blood pressure and high cholesterol. A healthy diet like the Mediterranean diet will lower your risk of heart disease.
Another way to both assist your heart and improve your RA: Dont smoke and if you do smoke, quit as soon as possible in addition, avoid exposure to secondhand smoke.
Finally, know that certain RA medications themselves have been linked to heart problems these side effects are rare, and are not a reason to skip drug treatment. The negative effects of not treating RA with medication are much, much worse than the side effects of RA drugs, cautions Greer.
Also Check: How To Deal With Arthritis
Why Your Mental Health Matters With Ra
When pain reduces your ability to get around or do the things you love, its normal for emotions to get the best of you. Depression is not uncommon in people with rheumatoid arthritis. Studies show a significantly increased risk of depression in people with RA, particularly in women and people older than 30 years of age.16,17
Research also shows that people with RA and depression may experience a lower quality of life and higher disease activity than those without depression. Moreover, some people with chronic conditions, including RA, may be an increased risk for having suicidal thoughts.18
The pain management community is just beginning to focus on the impact of chronic life on mental health. So its important to be proactive and tell your doctor if and when youre feeling depressed or anxious. Treatments from medication to talk therapy can help.
How Does Rheumatoid Arthritis Affect The Entire Body
Like many autoimmune diseases, rheumatoid arthritis typically waxes and wanes. Most people with rheumatoid arthritis experience periods when their symptoms worsen separated by periods in which the symptoms improve. With successful treatment, symptoms may even go away completely .
Although rheumatoid arthritis can have many different symptoms, joints are always affected. Rheumatoid arthritis almost always affects the joints of the hands , wrists, elbows, knees, ankles, and/or feet. The larger joints, such as the shoulders, hips, and jaw, may be affected. The vertebrae of the neck are sometimes involved in people who have had the disease for many years. Usually at least two or three different joints are involved on both sides of the body, often in a symmetrical pattern. The usual joint symptoms include the following:
These symptoms may keep someone from being able to carry out normal activities. General symptoms include the following:
- Malaise
Recommended Reading: How To Help Arthritis In Your Hands
How Ra Hand Pain Is Diagnosed
Theres no one test to diagnose RA and in its early stages, signs and symptoms can mimic those of many other diseases.
But early diagnosis of rheumatoid arthritis is important for the best outcome. We are learning that we need to control inflammation much more aggressively upfront as joint damage can ensue early on, says Dr. Albayda. Hence, there has been a shift in treatment paradigms to catching patients early and instituting treat-to-target control.
To help determine whether you have RA in your hand or wrist, a health care provider will examine your hands and fingers for such symptoms as:
- Swelling
- Pain
- Joint instability
They will also ask questions about other symptoms that tend to go along with RA, such as fatigue, flu-like symptoms, fever, and disrupted sleep.
A health care provider may order imaging tests to check for certain characteristics of RA, such as narrowing of the joint space or erosions of the bone. They will run blood tests to look for antibodies that may be found in people with RA as well as elevated levels of markers of inflammation in the blood.
Here is more information about tests used for diagnosing rheumatoid arthritis and criteria used for diagnosing rheumatoid arthritis.