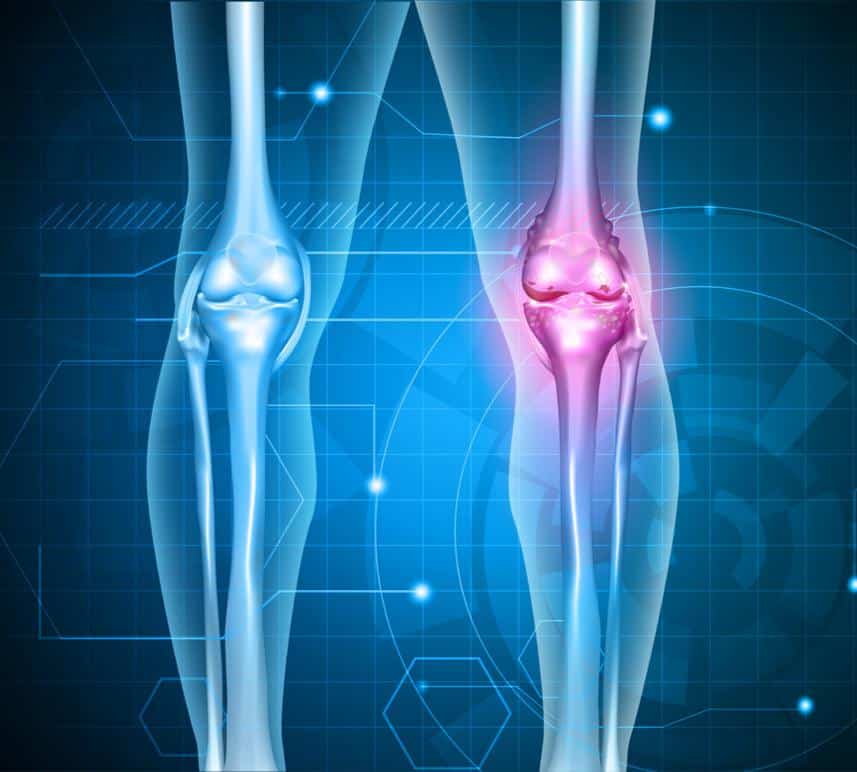
Ra In The Skeletal System
One of the first indications of RA is inflammation in the small joints of the hands and feet. Often, RA is symmetricalaffecting both sides of the body at once. Symmetry is key to diagnosing RA. Sometimes, RA does not cause symptoms on both sides, especially early on in the disease. The condition will become symmetrical as RA progresses.
Additional joints symptoms of RA include pain, swelling, stiffness, and tenderness. These are usually much worse in the morning and can last for 30 or more minutes. RA can also cause tingling or burning in the joints.
RA symptoms can affect any of your joints, especially as RA progresses. This includes symptoms in the hands, feet, shoulders, elbows, hips, knees, and ankles.
As the disease progresses, it will affect tendons, ligaments, and muscles. These symptoms will eventually lead to range-of-motion problems and difficulty with moving your joints. Long-term inflammation in affected joints will cause those joints to become damaged and deformed.
Having RA can put you at a higher risk for osteoporosisa condition that bone loss and weakness. This weakness can eventually lead to bone fractures .
Ongoing inflammation in your wrists may lead to a condition called carpal tunnel syndrome, which can make it harder to use your wrists and hands. This same inflammation can cause weakness and damage the bones of your neck and cervical spine causing severe, ongoing pain.
How To Stay Safe
Getting the COVID-19 vaccine will help protect you against the virus. You’ve probably also heard this a lot. But if you are unvaccinated, wear a face mask.Ã Wash your hands often.They are the best ways to protect you from germs:
- Scrub up for 20 seconds.
- Keep count by singing the “Happy Birthday” song, twice.
- Use regular soap and either cold or warm water.
- If those aren’t around, an alcohol-based hand sanitizer with at least 60% alcohol is the next best thing.
Make sure you clean every part of your hands. That includes under your fingernails, the back of your hands, and in between your fingers and thumbs.
If you have active RA or take an autoimmune drug, you should also:
- Keep away from people, especially big groups .
- Stay home as much as possible.
- Have someone else do your grocery runs.
- Avoid close contact with others .
- Wear a face mask when you have to go out.
- Disinfect surfaces people touch a lot.
- Try not to touch your eyes, nose, and mouth.
- Get a 2- to 4-week supply of medicine, if possible.
You can help your immune system by preventing infections from other diseases. Talk to your doctor about vaccines for things like the flu, pneumonia, whooping cough, and shingles.
Sidebar: Fast Fact: Vaccines And Immunity
The ability of the immune system to fingerprint and remember an antigen is the idea behind vaccination. When you get a vaccine for the flu or another virus, your immune system is given a deactivated portion of the antigen that causes the infection. Your immune system studies that antigen and develops a matching antibody, so that when your body encounters the real virus, it can generate antibodies to fight infection caused by that virus.
Note that while normally antibodies are positive things that help us fight infection by any number of infectious microorganisms, people with RA and other autoimmune diseases develop antibodies that attack their own healthy tissues. These are called auto-antibodies, . Thus RA is an instance where an antibody can be destructive.
In addition to presenting the antigen to the B-cell, the macrophage also presents it to the Th cell . By closely examining the antigen, the Th cell determines whether it should stimulate production of B-cells for antibody production against an extracellular antigen or stimulate production of killer T-cells. Killer T-cells are produced if the antigen has invaded cells. The killer T-cell attaches itself to an infected cell and in most cases destroys that cell.2,3
The role of T-cells in RA is not fully understood, but large numbers of T-cells are routinely found in the synovial fluid of people whose joints are affected by RA.
Don’t Miss: Is Tramadol Good For Arthritis Pain
What Affects Life Expectancy
If youre diagnosed with rheumatoid arthritis, its important to understand how this condition can reduce life expectancy.
As a progressive illness, its not uncommon for RA symptoms to worsen over the years. It isnt the disease itself that shortens life expectancy, though. Rather, its the effects of the disease.
The major effects involve:
- your immune system: As an autoimmune disease, rheumatoid arthritis weakens the immune system, making you susceptible to infections some serious.
- chronic inflammation: Chronic inflammation can damage healthy tissues, cells, and organs, which can be life threatening if left unchecked.
- duration of the disease: If youre diagnosed with rheumatoid arthritis at a young age, youll live with the disease longer than someone diagnosed with the disease later in life.
- comorbidities and complications: You can develop complications or other conditions while having RA, and these can affect your outlook. The longer you have the disease, the greater the likelihood of developing complications that could shorten your lifespan.
- untreated RA: Reduced life expectancy can also occur when RA treatment doesnt work or if you dont seek treatment for symptoms or complications. People living with untreated RA are twice as likely to die than people who are the same age without RA.
Ra In The Muscular System
When inflammation makes it harder to move your joints, the attached joints will get weak. According to a 2017 report in the journal EBioMedicine, a 2575% reduction in muscle strength has been observed in people with RA when compared to others without RA of the same ages.
People with RA can develop a condition called rheumatoid myositis that causes weakness, swelling, and pain. While rheumatoid myositis is poorly understood, researchers speculate a number of causes, including inflammation, the medications used to treat RA, impaired joint flexibility, and reduced activity levels.
Rheumatoid Arthritis Doctor Discussion Guide
Get our printable guide for your next doctor’s appointment to help you ask the right questions.
You May Like: Does Sugar Intake Affect Arthritis
Whats The Normal Sed Rate For Rheumatoid Arthritis
Sed rate is a blood test that helps detect inflammation in your body. Your healthcare provider may also use this test to watch how your RA progresses. Normal sed rates are as follows:
| People designated male at birth | Erythrocyte sedimentation rate |
|---|---|
| > 50 years old | 30 mm/hr |
In rheumatoid arthritis, your sed rate is likely higher than normal. To take part in clinical trials related to rheumatoid arthritis, you usually need an ESR of 28 mm/hr. With treatment, your sed rate may decrease. If you reach the normal ranges listed above, you may be in remission.
Gut Health And Ra Outlook
Your microbiome also might affect how youâll do with treatment, according to at least one study. Researchers looked at the gut microbiome of patients before treatment. They found that the microbiomes of those who got better with treatment looked different to start with than the microbiomes of those who didnât respond to the treatment as well.
The researcher went on to show that a computer could use information about the gut microbiome to predict whether a person with RA would get better with treatment or not. The findings suggest it may one day be possible to use microbiome tests to help make treatment decisions.
You May Like: What Is Psoriatic Rheumatoid Arthritis
What Problems Does The Rheumatoid Arthritis Causes To The Immune System
RA does not cause a problem with the imune system it is the result of a problem with the imune system.
The problem with rheumatiod Arthritis is a malfunctioning imune system. chronic joint disease that damages the joints of the body. The damage is the result of inflammation of the joint lining tissue. Inflammation is usually in response to the body’s immune system to “assaults” such as infections, wounds, and foreign objects. In rheumatoid arthritis however the inflammation is attacks the joints.
What Are The Goals Of Treating Rheumatoid Arthritis
The most important goal of treating rheumatoid arthritis is to reduce joint pain and swelling. Doing so should help maintain or improve joint function. The long-term goal of treatment is to slow or stop joint damage. Controlling joint inflammation reduces your pain and improves your quality of life.
Don’t Miss: What Can Be Done For Degenerative Arthritis
How Is Rheumatoid Arthritis Diagnosed
Your healthcare provider may refer you to a physician who specializes in arthritis . Rheumatologists diagnose people with rheumatoid arthritis based on a combination of several factors. Theyll do a physical exam and ask you about your medical history and symptoms. Your rheumatologist will order blood tests and imaging tests.
The blood tests look for inflammation and blood proteins that are signs of rheumatoid arthritis. These may include:
- Erythrocyte sedimentation rate or sed rate confirms inflammation in your joints.
- C-reactive protein .
- About 80% of people with RA test positive for rheumatoid factor .
- About 60% to 70% of people living with rheumatoid arthritis have antibodies to cyclic citrullinated peptides .
Your rheumatologist may order imaging tests to look for signs that your joints are wearing away. Rheumatoid arthritis can cause the ends of the bones within your joints to wear down. The imaging tests may include:
In some cases, your provider may watch how you do over time before making a definitive diagnosis of rheumatoid arthritis.
How Is Rheumatoid Arthritis Managed
You can manage rheumatoid arthritis by taking medicines as prescribed to treat pain and joint inflammation. You can also help reduce symptoms by exercising and maintaining a healthy weight. Aim to do 30 minutes of moderate exercise most days of the week. This can be at one time or broken up into shorter sessions.
You may also need to make changes at home to help you manage daily tasks like cleaning or gardening. An occupational therapist can help you make adjustments if pain or joint stiffness makes certain tasks hard to complete. They can recommend tools to reduce strain on your joints, such as long-handled dustpans so you dont need to bend over, or book holders to reduce the strain on your hands and wrists.
You might find that rheumatoid arthritis makes you frustrated and upset. Rheumatoid arthritis can cause poor sleep, which can also make you feel down. Discus your feelings with friends and family and explain to them what they can do to support you. This may help you feel better and reassured that help is available, if needed. If you are struggling with a low mood or not managing to sleep, your doctor will be able to support you and work with you to build a plan to help.
Recommended Reading: How Does Someone Get Arthritis
Conditions With Similar Symptoms
Symptoms of RA can resemble things as harmless as having slept on a bad mattress or as serious as cancer. Several rare genetic diseases attack the joints. Physical injuries, infections, and poor circulation are among the many problems that can cause aches and pains. Many conditions start with symptoms of joint aches and pains. A few that in particular may be confused with RA arthritis include:
Osteoarthritis
Osteoarthritis is the most common form of arthritis, but it differs from RA in several important respects:
- Osteoarthritis usually occurs in older people.
- It is located in only one or a few joints.
- The joints are less inflamed.
- Progression of pain is almost always gradual.
- X-rays show changes typical for osteoarthritis.
Gout
Gout also causes swelling and severe pain in a joint. It most commonly starts in one joint. It is sometimes difficult to distinguish chronic gout in older people from rheumatoid arthritis, since gout in this population can occur in a number of joints. A proper diagnosis can be made with a detailed medical history, blood tests, and finding uric acid crystals in the affected joint.
Can Ra Drugs Treat Covid
While there are now vaccine for the virus, there’s noà treatment asà yet. But some researchers are studying whether certain RA drugs might help. They include:
Some studies found early evidence that hydroxychloroquine had an effect against the new coronavirus. But many of those trials were stopped when they found serious side effects or failed to show lasting results.
Based on early findings, the FDA issued an emergency ruling that would allow doctors to use chloroquine and hydroxychloroquine in people who were in the hospital with COVID-19. The agency later revoked the ruling amid concerns about the drugs’ safety and how well they worked against the coronavirus.
You may still notice a shortage if you order this medicine. That’s why experts are urging drugmakers to keep up with demand. And some states have new rules about who can get the drug. That may make it easier for people with RA to get it.
You May Like: What Is Good To Treat Arthritis
How Is Ra Treated
RA can be effectively treated and managed with medication and self-management strategies. Treatment for RA usually includes the use of medications that slow disease and prevent joint deformity, called disease-modifying antirheumatic drugs biological response modifiers are medications that are an effective second-line treatment. In addition to medications, people can manage their RA with self-management strategies proven to reduce pain and disability, allowing them to pursue the activities important to them. People with RA can relieve pain and improve joint function by learning to use five simple and effective arthritis management strategies.
How To Bolster Health With Rheumatoid Arthritis
One of the main issues caused by rheumatoid arthritis is that your chances of getting sick from various infections are twice as high. Rheumatoid arthritis cannot be cured, but there are effective strategies to protect and improve your wellbeing and bolster your health even while showing symptoms of rheumatoid arthritis: pain, swelling and stiffness. Adopting a healthier lifestyle may also help prevent the degenerative condition from getting out of hand and causing irreparable, lasting damage on the joints.
To secure the optimal outcome for your present and future self, you need to safeguard yourself against infections, take a holistic approach and combine all the options available, from switching to a more wholesome lifestyle to undergoing the best procedures for rheumatoid arthritis in San Diego.
Don’t Miss: Is Rheumatoid Arthritis And Autoimmune Disease
Will Changing My Diet Help My Rheumatoid Arthritis
When combined with the treatments and medications your provider recommends, changes in diet may help reduce inflammation and other symptoms of RA. But it wont cure you. You can talk with your doctor about adding good fats and minimizing bad fats, salt and processed carbohydrates. No herbal or nutritional supplements, like collagen, can cure rheumatoid arthritis. These dietary changes are safer and most successful when monitored by your rheumatologist.
But there are lifestyle changes you can make that may help relieve your symptoms. Your rheumatologist may recommend weight loss to reduce stress on inflamed joints.
People with rheumatoid arthritis also have a higher risk of coronary artery disease. High blood cholesterol can respond to changes in diet. A nutritionist can recommend specific foods to eat or avoid to reach a desirable cholesterol level.
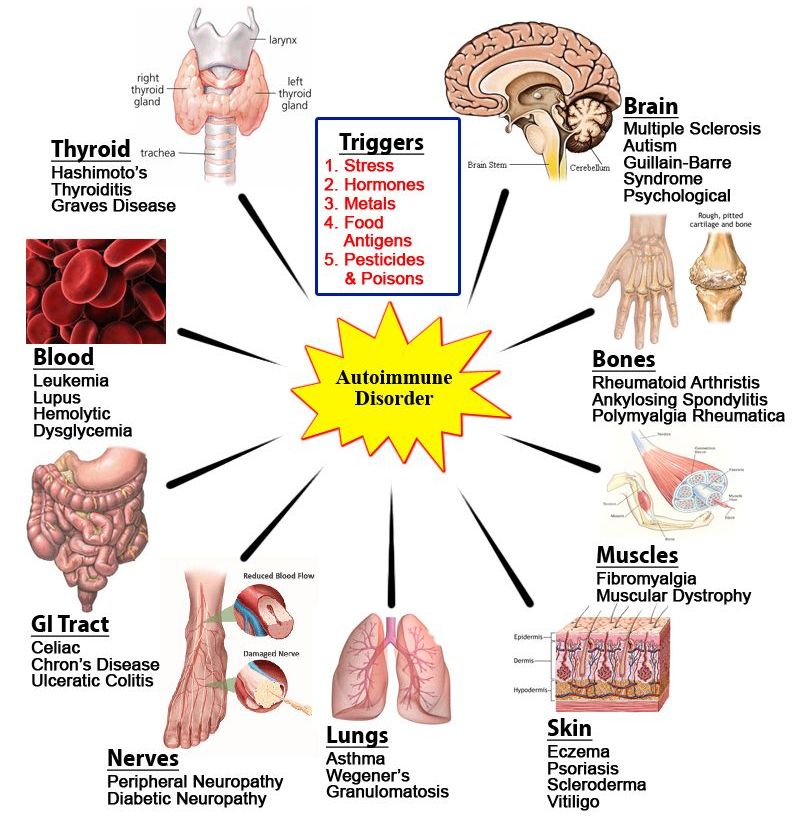
What Triggers Autoimmune Diseases
That’s still not clear. But researchers are making progress.
As with other life-long conditions like heart disease, itâs probably not just one thing that causes these disorders. Many things work together to raise your risk, like your genes, environment, and lifestyle choices, says John A. Peyman, PhD, program officer in the autoimmunity branch of the National Institute of Allergy and Infectious Diseases .
For starters, it seems that you can be more likely to get an autoimmune disease if other members of your family have one. Your parents can pass down genes that make it more likely.
One gene has been linked with most autoimmune diseases, Peyman says. Itâs called human leukocyte antigen .
â200 other genes contribute a tiny bit to the chance of getting RA,â he says.
So what happens if you inherit one of the genes?
You may be more likely than the average person to get an autoimmune disorder. While another person might get an infection and get better, the same infection might trigger the inflammation inside your body that leads to the disease, Peyman says.
For example, researchers are studying super-tiny living things called microbes in your gut, mouth, and on your skin. They may work more closely with the immune system than people thought, Ladd says. If they’re out of balance, it may trigger your immune system and make more inflammation.
Recommended Reading: Are Carrots Good For Arthritis
Rheumatoid Arthritis Is Not Osteoarthritis: 2 Different Types Of Arthritis
Osteoarthritis affects over 32.5 million adults in the United States, according to the Centers for Disease Control and Prevention . It is the most common type of arthritis its the type that your grandparents have, most likely. It is known as degenerative arthritis and also called wear-and-tear arthritis, aptly named because the cartilage that lines your joints wears down. The risk of developing osteoarthritis increases with age.
Rheumatoid arthritis is an autoimmune, inflammatory, systemic disease. In RA, your immune system attacks healthy cells in your body by mistake, resulting in inflammation, pain, and swelling in affected body parts. Typically, with rheumatoid arthritis, the pattern of affected joints occurs symmetrically .
RELATED: 10 Essential Facts About Inflammation and Rheumatoid Arthritis
Symptoms Affecting The Joints
Rheumatoid arthritis is primarily a condition that affects the joints. It can cause problems in any joint in the body, although the small joints in the hands and feet are often the first to be affected.
Rheumatoid arthritis typically affects the joints symmetrically , but this is not always the case.
The main symptoms of rheumatoid arthritis affecting the joints are outlined below.
Don’t Miss: Is There Treatment For Arthritis
How Is Ra Diagnosed
RA is diagnosed by reviewing symptoms, conducting a physical examination, and doing X-rays and lab tests. Its best to diagnose RA earlywithin 6 months of the onset of symptomsso that people with the disease can begin treatment to slow or stop disease progression . Diagnosis and effective treatments, particularly treatment to suppress or control inflammation, can help reduce the damaging effects of RA.