Is Mental Health Linked To Fatigue
Patients often report fatigue when their vasculitis is in remission. A Cleveland Clinic study, which Dr. Hajj-Ali led, found that depression and lack of sleep contribute to fatigue.
So we always ask vasculitis patients about anxiety and depression, she says. We also ask, How many hours are you sleeping? and What is your sleep pattern?
Recommended Reading: What Does The Rash From Psoriatic Arthritis Look Like
How Is Arthritis Treated
Theres no cure for arthritis, but there are treatments that can help you manage the condition. Your treatment plan will depend on the severity of the arthritis, its symptoms and your overall health.
Conservative treatments include:
- Medication: Anti-inflammatory and pain medications may help relieve your arthritis symptoms. Some medications, called biologics, target your immune systems inflammatory response. A healthcare provider may recommend biologics for your rheumatoid or psoriatic arthritis.
- Physical therapy: Rehabilitation can help improve strength, range of motion and overall mobility. Therapists can teach you how to adjust your daily activities to lessen arthritic pain.
- Therapeutic injections: Cortisone shots may help temporarily relieve pain and inflammation in your joints. Arthritis in certain joints, such as your knee, may improve with a treatment called viscosupplementation. It injects lubricant to help joints move smoothly.
How Long A Flare Lasts
The length of a flare varies, and can be different for different people. Some may experience it for a year, months, or days. A flare can last as long as there isnt a change in treatment. In one study, flares lasted longer than two weeks in 30% of participants, one to two weeks in 13%, and less than one week in 57%. Longer duration of a flare was associated with changes in disease-modifying therapy.
Its essential to work with your healthcare provider to monitor your symptoms and tweak your treatment plan accordingly when you experience RA flares.
Patients with RA experience flares more often when noted to be in higher disease activity states than when in remission.
You May Like: How To Relieve Stomach Stress
Recommended Reading: Is Quinoa Good For Arthritis
Having A Cold Or Other Infection
Getting sick can start a chain reaction that leads to painful arthritis symptoms. According to Dr. Jain, infections can make your immune system even more active, making it likelier it will attack your own joints. We also often tell patients to stop taking their rheumatoid arthritis medication if they are on antibiotics , says Dr. Jain. That combination can lead to flares. It can be harder for rheumatoid arthritis patients to avoid getting sick since the medication prescribed often suppresses the immune system. Thats why its so important to reduce your risk, like by getting the flu vaccine every year, washing your hands frequently, and avoiding others who are ill.
No matter what triggered your flare, its important to talk to your doctor and get it under control as soon as you can to avoid serious damage to your joints.
Inflammatory Arthritis Versus Osteoarthritis
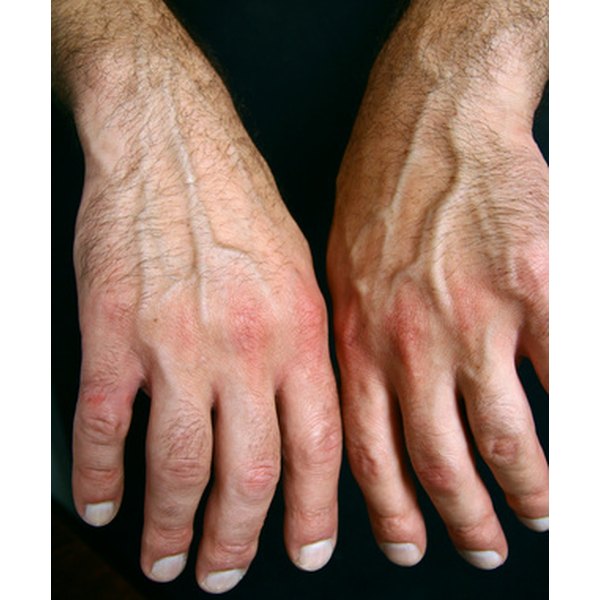
Knowing the type of arthritis, you have is the key to recognizing and managing a flare up. Osteoarthritis is the most common type of arthritis. It is caused by wear and tear of the cartilage linings of your joints. Since wear and tear takes time, this type occurs mostly in older people. It may be more common in a joint that you injured at some time. It causes pain, stiffness, and swelling, but not inflammation.
Inflammatory arthritis may be caused by a disorder of your immune system. Your immune system is your bodys defense system against foreign invaders like germs. If you have an immune system disease called an autoimmune disease, your immune system attacks normal body tissues, including your joints. The symptom of the attack is inflammation of tissue in around your joints.
Autoimmune inflammatory arthritis affects many joints all over your body at the same time. This is also called inflammatory polyarthritis. This type of arthritis is a long-term disease that is often diagnosed in young adults. Both rheumatoid arthritis and psoriatic arthritis are common types. Inflammation adds symptoms of redness and a feeling of warmth to affected joints along with pain and swelling.
Read Also: Can You Have Arthritis In Your Legs
Does Stress Cause Young People With Arthritis To Suffer Flare
Research has begun into looking at whether psychological stress can lead to young people with arthritis suffering flare-ups.
The study, led by BRC-supported Dr John Ioannou, will hopefully lead to a better understanding of a theory held by some doctors that when young people with juvenile idiopathic arthritis suffer stress it can cause their condition to suddenly worsen.
Patients between 13-18 will complete a questionnaire which assesses their mood, well-being, anxiety and depression levels when they attend appointments at the Arthritis Research UK Centre for Adolescent Rheumatology, a collaboration between UCL, University College Hospital and Great Ormond Street Hospital which seeks to understand why rheumatic diseases can be more severe in teenagers.
The patients will also be asked if they have noticed that stress is a trigger for flare-ups and how they manage with this.
There will be a matching questionnaire pack for parents to find out about their childs mood recently and if they are experiencing any stress as a parent.
During the first phase of the trial, 122 people have been recruited and 77 blood samples have been taken. The samples are studied in a laboratory to look at how the immune system changes in response to stress. The team plan to speak to the young people on a six-monthly basis to monitor their overall well-being and inflammatory markers.
You May Like: How To Avoid Arthritis In Hands
Schedule A Girls Night In
Going out is a huge source of stress for Amanda S., of Denver, Colorado, who has inflammatory arthritis, chronic migraines, and type I diabetes. Not only does it take a lot of time and energy to plan and go out but once shes there, her restrictive-but-necessary diet means she has to worry about the food as well. Her stress-free solution? Plan a girls night in. She invites a few girlfriends over to play games or watch a movie and then she doesnt have to worry about getting dressed up or doing something physical when shes in pain. She can make the snacks so she doesnt have to stress over food restrictions. Bonus: Spending time with loved ones is a proven way to reduce stress.
Read Also: Are Psoriasis And Psoriatic Arthritis Related
Get Comfortable With Boundaries
Setting boundaries can be tricky for many people as it can require some confrontation or at least telling others something you think they wont like. But learning to set appropriate boundaries and being firm on maintaining them is the key to managing and preventing stress, Meghan says. This may mean having a set bedtime and asking guests to leave early. Or perhaps it means saying no to a party or other fun invite when youre feeling overwhelmed. Figure out what your limits are and dont apologize for sticking to them, she says.
Can Stress Cause An Arthritis Flare
Yes. A study from Penn State University found that arguing with a spouse can cause you to experience worse arthritis pain on the same day. Whats more, the severity of the pain you experience can trigger emotional tension, which then may create additional conflict with your spouse the next day. Talking through issues calmly can help the metabolic effect of the stress hormone cortisol, which increases inflammation in your system. Try one of these ways to reduce stress in your life, including essential oils.
Read Also: Is Aspirin Good For Arthritis
Eat Small Frequent Meals
Large meals stress my body out and make me feel exhausted afterward, Meghan says. Conversely, being super hungry also feels very stressful to her. Her solution? I eat five or six mini meals spread out throughout my day, she explains. A healthy snack of protein and a fresh fruit or vegetable provides consistent energy and helps defuse stress.
Consider Getting Tested For Sleep Apnea
In addition to making changes to your sleep routine, you may also want to talk to your doctor about getting tested for sleep apnea, a sleeping disorder that can affect your breathing. Sleep apnea can leave you feeling exhausted even after a full nights sleep. People with RA are more likely to have sleep apnea.1,2 This difference seems to exist even when a flare is over and inflammation levels are low.3
You May Like: Can You Have Arthritis In Your Chest
Common Medications To Treat Arthritis Flares
OA patients might just need some OTC pain-relieving medication such as acetaminophen, ibuprofen, or naproxen. Dr. Bose also recommends topical gels and lotions like diclofenac gel or 2 Old Goats. If that doesnt work, Dr. Ashany says joint injections of steroids may be given. RA flares are more complicated. In inflammatory arthritis, steroids are often used to try to quickly bring a flare under control, Dr. Ashany says. If only one joint is involved a steroid can be given by injection, but otherwise it can be taken orally .
In inflammatory arthritis, if flares continue to occur, this indicates that the patients regimen of maintenance medication is not adequate, Dr. Ashany says. This may lead to addition of a medication, switching one drug for another or increasing the dose of medication that the patient is currently taking.
The Mystery Of Autoimmune Illness Continues
Whether stress or stress-related disorders play an important role remains speculative. Even more important is the question of whether any particular treatment of these stress-induced psychological illnesses can prevent autoimmune disease. I look forward to a clinical trial that examines this fascinating possibility.
Follow me on Twitter @RobShmerling
Dont Miss: How To Deal With Stress While Pregnant
You May Like: Does Arthritis Cause Lower Back Pain
How Is Arthritis Diagnosed
If you think you may have arthritis, see your healthcare provider. The provider will ask about your symptoms and learn how joint pain affects your life. Your provider will perform a physical exam, which may include:
- Assessing mobility and range of motion in your joints.
- Checking for areas of tenderness or swelling around your joints.
- Evaluating your overall health to determine if a different condition could be causing your symptoms.
The Effect Of Stress On Arthritis
Stress. There is no avoiding it completely. It is a part of everyday life. Just when you think it is gone, it is back again. It is the way the mind and body react to tension and pressure. Too much stress can increase pain, can make a person prone to illnesses, and can make it more difficult for people with arthritis to cope with the added burdens imposed by their disease.
Don’t Miss: What Natural Medicine Is Good For Arthritis
Try Alternative Relaxation Techniques
Many people use alternative therapies, such as hypnosis, progressive muscle relaxation, and guided imagery training to help manage stress. They are techniques you can learn from a practitioner, books, apps, or CDs, and then practice yourself. “These methods help teach you to carry a lower level of stress around,” says Edward Charlesworth, PhD, author of Stress Management: A Comprehensive Guide to Wellness. “We all run into stressors throughout the day, but these therapies can help you learn how to manage your stress more effectively and make life more enjoyable.”
In addition, acupuncture and massage therapy can also be helpful for reducing stress — and can also help ease the pain of arthritis.
How Long Does It Last
Arthritis flare-ups can be variable, but they generally last three to five days with conservative care. Home care can include anti-inflammatory medicines, changing activities, and using ice, compression, or bracing. If doing those things isnt helping after a week, come in to see the Summit team, and we can help it along. Office-based treatments like joint aspiration and cortisone injections can provide relief from an arthritis flare-up.
Over the long term, its smart to keep track of how many flare-ups youre having. If they are increasing, it might be time to look into injections or surgery. In other words, if youre having more bad days than good, its worth having a discussion about what Summit can do to fix that. Its a quality-of-life issue.
Don’t Miss: How Does Hydroxychloroquine Help Rheumatoid Arthritis
What Can I Do To Make Living With Arthritis Easier
Changing your routine can make living with arthritis easier. Adjust your activities to lessen joint pain. It may help to work with an occupational therapist . An OT is a healthcare provider who specializes in managing physical challenges like arthritis.
An OT may recommend:
- Adaptive equipment, such as grips for opening jars.
- Techniques for doing hobbies, sports or other activities safely.
- Tips for reducing joint pain during arthritic flare-ups.
How Long Does An Arthritis Flare Last
The length and severity of an arthritis flare is unpredictable and differs from person to person. Different people may also have different triggers for their flares. The best advice is to listen to your body and become aware of your flare triggers. It may help to keep a flare diary and work with your doctor to developing a flare management plan. Avoid treating a flare a supplement, unless you talk to your doctor first. If you are having frequent flares or a severe flare that is not responding to your usual home care, call your doctor. Sometime a flare needs medical treatment to prevent permanent joint damage.
Also Check: How To Stop Arthritis Inflammation
Take Physical Signs Of Stress Seriously
Sometimes I feel stress before I even realize Im stressed out, Meghan says. And she cant deal with her stress unless she recognizes how its affecting her. Her telltale symptom? Hello, racoon eyes! she says. Deep, dark undereye bags are a tip-off that she needs to do some self-care immediately.
Why Does Stress And Anxiety Cause Joint Pain
Life is full of stressful situations. You may feel stress over meeting a deadline, managing finances, or even something as simple as getting the kids out the door in the mornings .
According to the Anxiety and Depression Association of America, Seven out of ten adults in the United States say they experience stress or anxiety daily, and most say it interferes at least moderately with their lives.
Stress has become such a part of daily life that many people dont realize its a problem until symptoms become unbearable, and sometimes, irreversible.
Read Also: Are Raisins Good For Arthritis
Can A Positive Attitude Help Reduce My Pain
Absolutely. Re-read this article to remind yourself that you have many good tools and options available to improve your quality of life. You can reduce the severity of arthritis you do have through the changes you make, Blum says. You have control!
Learn how a mindfulness practice can help you live in the here and now.
Tips For Dealing With Arthritis Pain In Winter
How many times have you sworn that a storm was coming because your arthritis pain was flaring up? How many times has a bone-chilling cold caused your joints to swell and get inflamed with pain and stiffness?
Winter weather can be especially tough for those who suffer from arthritis, and there could be some truth to the old wives tale that aching joints can be an indicator of a change in weather. In fact, the Arthritis Foundation even cites studies that show lower barometric pressure caused more aches and pains for people in barometric pressure chambers.
Arthritis can be classified as either inflammatory or non-inflammatory. Inflammatory arthritis features inflammatory white blood cells in the joint fluid. Forms of inflammatory arthritis include rheumatoid arthritis, lupus arthritis, gout, and many others. Forms of non-inflammatory arthritis include osteoarthritis, arthritis of thyroid disease, arthritis after injury and many others. Studies have shown that cold weather can affect both inflammatory and non-inflammatory arthritis.
With winter in full swing, cold weather pain and arthritis can be uncomfortable and affect your quality of life. The cold doesnt cause arthritis, but it can increase joint pain, according to the Arthritis Foundation. Here are some great tips to deal with arthritis pain during the winter months.
1. Stay warm and layer up
2. Eat a healthy diet
3. Get your stress under control
4. Stay active and exercise
6. Get your vitamin D
Also Check: Is Salt Good For Arthritis
Arthritis And Mental Health
Learn more about the connection between arthritis, depression and anxiety, and how these conditions can make your arthritis worse.
Having any form of arthritis including osteoarthritis , rheumatoid arthritis , psoriatic arthritis , lupus, ankylosing spondylitis, gout or fibromyalgia can have a negative effect on your mental health. This most commonly manifests as depression or anxiety. It works the other way around, too. Mental health problems can worsen arthritis symptoms.
Defining Anxiety and Depression According to the American Psychological Association:
- Anxiety is characterized by feelings of tension, worry and irritability along with physical changes like increased blood pressure.
- Depression is characterized by sadness, a lack of interest in daily activities, weight loss or gain, sleeplessnessor excessive sleeping, lack of energy, inability to concentrate, feelings of worthlessness or excessive guilt, and recurrent thoughts of death or suicide.
How Mental Health Affects Arthritis Rates of depression and anxiety in people with arthritis-related diseases vary depending on the population, the size of the study, and the measurement tools used. But data shows that the rates can be between two- and ten-times greater than the rates of the general population, depending on the type of arthritis.
Emotional Wellness
Arthritis And Stress: 4 Things You Need To Know
Arthritis in its many forms represents a major public health challenge, affecting some 54 million Americans according to the CDC. At the same time,77 percentof Americans claim that stress has had a negative impact on their physical health. These two issues can create a feedback loop of pain and disability.
If you have struggled with both arthritis and some form of chronic stress, you need to understand how these conditions feed each other and amplify each other’s worst effects, as well as smart strategies for restoring your mind and body to a more even keel. Check out the answers to these frequently asked questions.
1. Stress Can Worsen Some Forms of Arthritis
Everyday life presents more than its share of stress triggers even in the absence of major life-changing events. Emotional, physical, and psychological stress prompts the body to release large amounts of adrenaline and cortisol, stress hormones that can alter your immune system responses.
Abnormal immune function could play a role in causing or aggravating autoimmune conditions, including psoriatic arthritis, ankylosing spondylitis, and rheumatoid arthritis. Chronic stress may also allow inflammatory substances called cytokines to run wild, which, in turn, can worsen your arthritis symptoms.
2. Arthritis Can Raise Stress Levels
3. Arthritis Management Techniques May Reduce Stress Levels
4. Stress Reduction May Ease Your Arthritis Symptoms
Also Check: What Meds Are Best For Arthritis