The Psoriasis Arthritis Symptoms To Watch For
If you are concerned about developing psoriatic arthritis, there are some symptoms to watch out for. First of all, if you have psoriasis already, that is the number one risk factor for getting psoriatic arthritis. Watch for lesions on the nails as a good indicator the ailment will most likely develop.
Family history and age are also determining factors. If you have a parent or sibling with the disease, you are more likely to acquire it as well. The condition usually is diagnosed most frequently in patients between the 30 and 50 years old.
Rheumatoid Arthritis Rashes: Causes And Treatment
While rheumatoid arthritis primarily affects the joints and the connective tissues, other areas of the body can also be involved. More than 1,000 myRAteam members report skin rashes as one of their RA symptoms. I have a horrible rash that flares up at times on both arms, one member said. Another said, I have had a rash on and off on my right forearm for six months now.
When parts of the body besides the joints are affected by RA, the symptoms are called extra-articular manifestations. These can be divided further into two categories: general manifestations, like thinner and paler skin overall, and specific manifestations, like a nodule under the skin.
Rheumatoid Arthritis Can Cause A Range Of Skin Symptoms But Skin Problems Could Also Indicate You Have A Different Kind Of Arthritis To Begin With
Before the modern era of treating rheumatoid arthritis early with disease-modifying drugs, you could often guess that a person had RA just by looking at their skin. Long-term, severe rheumatoid arthritis damages small blood vessels throughout the body. This condition is called rheumatoid vasculitis, which shows up as bruising, pain, and sores on the skin. Another telltale sign of RA used to be rheumatoid nodules under the skin, often near affected joints.
We used to see nodules a lot, but these lumpy bumps about the consistency of a pencil eraser are getting less common with better therapy, says rheumatologist Kevin Deane, MD, PhD, associate professor of medicine at the University of Colorado School of Medicine.
While, thankfully, these skin conditions are no longer as common as they used to be, many people with RA can develop skin problems that raise questions about whether and how they might be related to their arthritis.
Recommended Reading: Does Walking Help Knee Arthritis
When Your Ra Skin Rash Could Actually Mean A Different Diagnosis
Theres lots of overlap in symptoms between various types of arthritis. Even if youve already been diagnosed with RA, your rheumatologist may reconsider your diagnosis if you develop certain telltale skin signs.
- A butterfly-shaped rash on your cheeks and across the bridge of your nose will raise the possibility of lupus.
- A scaly rash may point towards psoriatic arthritis.
If someone with a diagnosis of RA come in with a scaly rash, especially on the elbows, knuckles, behind the ears, scalp, or along with changes in their fingernails, well think about psoriasis and psoriatic arthritis, says Dr. Deane.
Joint Pain Joint Pain Skin Rash And Swelling
- Medical Author: Melissa Conrad Stöppler, MD
Reviewed on 2/19/2021
Joint pain and swelling are characteristic of the many different arthritis conditions including rheumatoid arthritis, osteoarthritis, and gout. Skin rash can accompany some conditions that cause arthritis. Skin rash also has numerous other causes. Keep track of your symptoms, and talk with your healthcare provider if you are concerned about any symptoms.
While the list below can be considered as a guide to educate yourself about these conditions, this is not a substitute for a diagnosis from a health care provider. There are many other medical conditions that also can be associated with your symptoms and signs. Here are a number of those from MedicineNet:
Don’t Miss: Does Sugar Intake Affect Arthritis
Treatment Of Skin Issues
Some skin issues may require treatments, while others might not. Treatment will depend on the cause and severity. The goal of treatment is to reduce pain, discomfort, and inflammation, and also to prevent infection.
It is very important to treat the underlying cause of skin problems, as these conditions are a sign that rheumatoid arthritis symptoms are not well-managed.
Common over-the-counter medications, including acetaminophen , can help with pain, while NSAIDs, including ibuprofen, can help control and reduce inflammation. Severe pain may need prescription NSAIDs. Corticosteroids can also help reduce skin inflammation, but these medications cannot be used in the long-term. If there is a possibility of infection, a topical or oral antibiotic may be prescribed. Hives are usually treated with antihistamines.
If medications are the cause of RA skin symptoms, medication replacement or reduction may help prevent or reduce skin symptoms.
What Causes Rheumatoid Arthritis
Rheumatoid arthritis is multifactorial in origin. Although regarded as autoimmune with anti-citrullinated proteinantibodies and rheumatoid factor , genetic and environmental factors are also important in the pathogenesis. In ACPA-positive disease the most significant association is mapped to the HLA-DRB4 gene. ACPA are found in 60% of patients with rheumatoid arthritis .
Read Also: How To Treat Arthritis In Lower Back
Are Rashes From Rheumatoid Arthritis And Eczema Connected
Any person that is suffering from rheumatoid arthritis is dealing with a health condition where the body attacks its own joints instead of fighting off bacteria and viruses like its supposed to. The result of the autoimmune disease is painful wrists, feet, ankles, and fingers.
However, that isnt necessarily the only problem that surfaces. For some, because of the swelling of the joints, eczema can also be a symptom.
The skin above where the inflammation of the joints is occurring can become inflamed as well. It will get rough, itchy, bleed, and in severe cases, blisters may even form. More often than not, these two conditions appear separately.
Eczema is a skin condition that first appears in early childhood years for most patients and continues on throughout their lives. Sometimes though, an individual can get eczema as a result of their arthritis.
While there is still more research that needs to be done on the connection between arthritis and eczema, experts suggest that the red, itchy, and bumpy skin frequently shows up as an indicator that something related to the restriction in blood flow is happening beneath the surface.
Shortness Of Breath Or Coughing
The lungs are often affected in people diagnosed with rheumatoid arthritis. Lung conditions may cause coughing, shortness of breath, and chest pain. Rarely, these conditions become life-threatening.
- Interstitial lung disease is an umbrella term used to describe many disorders that cause scarring of the walls of the lungs and certain nearby structures. In people with RA, scarring is typically caused by chronic inflammation. The initial symptoms of interstitial lung disease typically include shortness of breath and a cough.
- Pleural effusion, also called pulmonary effusion or water on the lungs, occurs when fluid collects in the chest cavity outside the lungs. Pleural effusion can cause sharp chest pain, coughing, and shortness of breath. It may be noticeably more difficult to breathe when lying down.
nodules in the lungs typically have no symptoms but may increase the risk for potentially life-threatening conditions, such as a collapsed lung.5,6Rheumatoid nodules in the lungs are rare and account for less than 1% of all rheumatoid nodules.
The chances of developing lung conditions related to RA are increased by smoking.
Also Check: What Kind Of Doctor Do You See For Arthritis
What Are The Symptoms Of Rheumatoid Vasculitis
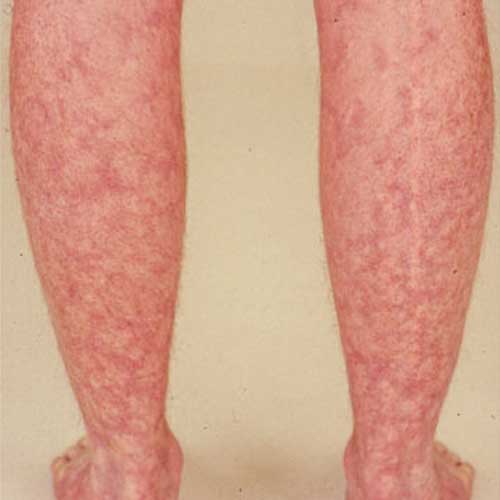
When vasculitis involves the small arteries and veins that nourish the skin of the fingertips and skin around the nails, small pits in the fingertips or small sores causing pain and redness around the nails can occur. Involvement of somewhat larger arteries and veins of the skin can cause a painful red rash that often involves the legs. If the skin is very inflamed, ulcers can occur and infection becomes a complicating risk.
Vasculitis that injures the nerves can cause loss of sensation, numbness and tingling, or potentially weakness or loss of function of the hands and/or feet. The rare vasculitis of larger arteries can cause complete absence of blood flow to tissue sites supplied by the affected vessel , which can cause gangrene of fingers or toes, stomach pain, cough, chest pain, heart attack, and/or a stroke if the brain is involved. This form of systemic vasculitis can also be accompanied by general symptoms such as fever, loss of appetite, weight loss, and loss of energy.
Vision Loss Of Red/green Color Distinction
A rare complication of the commonly used rheumatoid arthritis drug hydroxychloroquine is an injury to the retina . The earliest sign of retinal changes from hydroxychloroquine is a decreased ability to distinguish between red and green colors. This occurs because the retina’s vision area that is first affected by the drug normally detects these colors. People who are taking hydroxychloroquine who lose red/green color distinction should stop the drug and contact their doctor.
Also Check: Is Humira Good For Arthritis
Skin Problems In People With Rheumatoid Arthritis
RA is one of common types of arthritis, though it is less common than osteoarthritis. It occurs when the body immune system attacks the lining of the protective membranes surrounding the joints called synovium.
So in RA, there is something that goes awry with the body immune system. Therefore its also known as autoimmune disease.
Still, it mainly affects and attacks your joints. But again the effect of the disease is systemic. In other words, it can affect other parts /organs of your body that have nothing to do with your joints, including skin.
For more information about the link between RA and skin problems, you might also like to read:
What Are The Side Effects Of Rheumatoid Arthritis
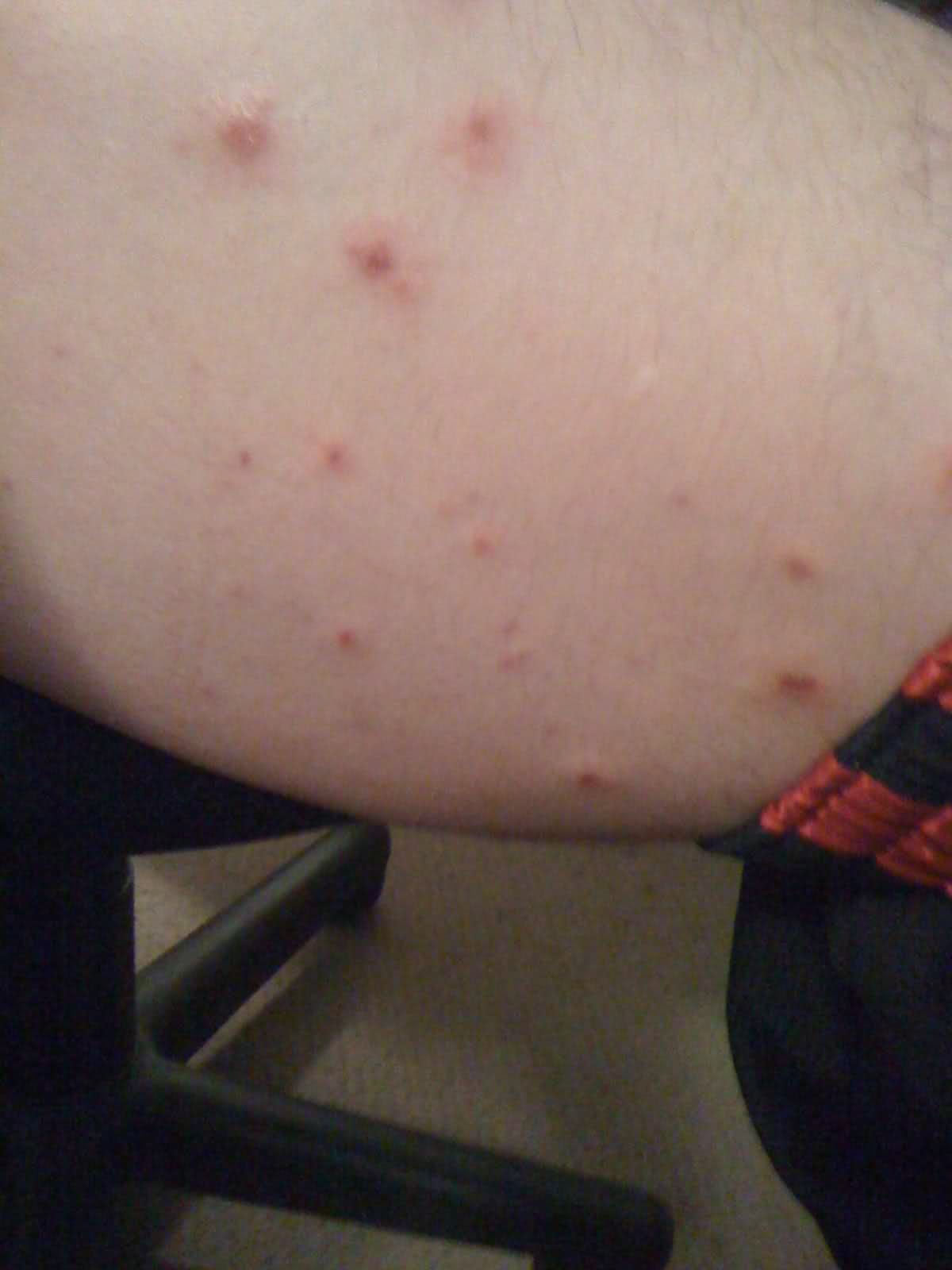
Medication Side Effects. The skin problems people with RA have are often related to the medications they take to ease symptoms or control their disease. Drug-related skin problems include: Skin rashes . This can happen if you take drugs such as:
Rheumatoid arthritis affects all races. The peak age of onset is 3550 years. Extra-articular involvement develops in approximately 40%, and skin changes in 30%. What causes rheumatoid arthritis?
Recent Posts
Read Also: What Foods Aggravate Rheumatoid Arthritis
What Is Rheumatoid Arthritis
Rheumatoid arthritis is a chronicsystemicinflammatoryautoimmune disease characterised by a symmetric destructive polyarthritis and extra-articularmanifestations including skin changes.
Skin changes of rheumatoid arthritis can be classified as:
- General cutaneous manifestations
- Adverse cutaneous effects of treatment.
Foamy Pink Or Brown Urine
Research suggests 30% of people with RA experience kidney problems at some point,15 though only a portion will develop chronic kidney disease. The kidneys filter blood, removing waste and excess water to create urine. When there is a problem with the kidneys, urine may look differentpossibly foamy, pink, or brown.
Kidney problems can also cause:
- Fatigue and/or insomnia
- Poor appetite
- Muscle cramping
Swelling related to kidney problems may also be less tender and painful than swelling related to an RA flare.
Kidney problems may be the result of:
- Body-wide inflammation related to RA
- Medications used to treat RA, including but not limited to methotrexate and nonsteroidal anti-inflammatory drugs , such as Aleve, Advil, and Celebrex
The most common kidney problems associated with RA include mesangial glomerulonephritis , membranous nephropathy, and secondary amyloidosis.15 Making an exact diagnosis typically requires a surgical biopsy and is not always necessary for treatment.
While kidney conditions can be serious and lead to chronic kidney disease, they may also be relatively mild or reversible with treatment. Physicians must evaluate each person individually.
Recommended treatment may include changes to medication, especially if medications are the suspected cause of kidney problems. Other first-line treatments may include taking steps to control blood pressure and making lifestyle changes, such as changing diet, exercising regularly, and quitting tobacco products.16
Also Check: How To Deal With Arthritis
Cutaneous Adverse Effects Of Treatment For Rheumatoid Arthritis
The treatment of rheumatoid arthritis can cause side effects involving the skin.
Disease modifying antirheumatic drugs used in the treatment of rheumatoid arthritis include methotrexate, azathioprine, leflunamide, ciclosporin, and hydroxychloroquine. Skin side effects are well documented.
There are many new and emerging treatments for rheumatoid arthritis including biological treatments, Janus kinase inhibitors, rituximab , tocilizumab with their associated cutaneous side effects. Tumour necrosis factor inhibitors are biologic agents used widely for treatment-resistant rheumatoid arthritis. Many cutaneous side effects have been reported with their use in rheumatoid arthritis including psoriasis, dermatitis, leukocytoclastic vasculitis, lichenoid drug eruptions, and non-infectious cutaneous granulomatous reactions, such as disseminatedgranuloma annulare, sarcoidosis-like lesions, and interstitial granulomatous dermatitis.
Dermatological side effects of tumour necrosis factor inhibitors
How Is Dermatomyositis Treated
Treatment will depend on your symptoms, your age, and your general health. There’s no cure for the condition, but the symptoms can be managed. You may need more than one kind of treatment. And your treatment may need to be changed over time. Treatments include:
-
Physical therapy. Special exercises help to stretch and strengthen the muscles. Orthotics or assistive devices may be used.
-
Skin treatment. You may need to avoid sun exposure and wear sunscreen to help prevent skin rashes. Your health care provider can treat itchy skin rashes with antihistamine drugs or with anti-inflammatory steroid creams that are applied to the skin.
-
Anti-inflammatory medications. These are steroid drugs, or corticosteroids. They ease inflammation in the body. They may be given by mouth or through an IV.
-
Immunosuppressive drugs. These are drugs that block or slow down your body’s immune system. These include the drugs azathioprine, methotrexate, cyclosporine A, cyclophosphamide, and tacrolimus.
-
Immunoglobulin. If you have not responded to other treatments, these drugs may be given. They are donated blood products that may boost your body’s immune system. They are put directly into your bloodstream through an IV.
-
Surgery. Surgery may be done to remove the calcium deposits under the skin if they become painful or infected.
Talk with your health care providers about the risks, benefits, and possible side effects of all medications.
Don’t Miss: How Do You Treat Arthritis In The Fingers
Does Rheumatoid Arthritis Cause Rashes
RA dorashRAcauserashRashesRARA rashes
Rheumatoid patients can develop skin disorders. UIHC notes that the same kind of immune system problems that cause joint inflammation, swelling, and pain can also affect your skin. When this happens, RA patients may develop lesions or rashes on the skin, reflecting immunological dysfunctions.
Secondly, how long does RA rash last? These are usually mild and clear up in a few days. More worrisome are overall rashes or hives that appear during or within 24 hours after you receive infusion of a drug directly into your bloodstream.
Similarly, what type of arthritis causes a rash?
Psoriatic arthritis is a form of arthritis that typically occurs in people with psoriasis. In addition to pain, stiffness, and swelling of the joints, psoriatic arthritis can cause a red, scaly rash. In this article, we discuss whether psoriatic arthritis always causes a rash.
Is there a link between eczema and arthritis?
And eczema, psoriasis, skin infections and rosacea have also been associated with RA. Why and how RA and these skin diseases are related is a subject of research. One study found that drugs that block tumor necrosis factor one of the inflammatory proteins that are elevated in people with RA may play a role.
Treatment Of Rheumatoid Nodules
Rheumatoid nodules are not known to be painful, so they typically are not treated aggressively. However, the nodules can become infected at the surface at that time, aggressive treatment of the infection is suggested.
Occasionally, nodules may become painful if they are in sensitive locations or are putting pressure on nerves. In this case, the nodules may be aggressively treated.
Research shows that DMARDs may reduce the size of the nodules. However, a certain DMARD, methotrexate, may increase the size of the nodules. Steroid injections can also shrink the nodule.
For nodules that cause severe pain, surgery may be indicated to remove the nodule fully.
Unfortunately, nodules that reduce or even go away due to aggressive therapy may come back RA by nature is a disease that comes and goes, so nodules may do the same.
Don’t Miss: What’s Best To Take For Arthritis
What Actually Is Hives
Also called as urticaria, it is a skin reaction that leads to itchy nettle rash. It can range in size from tinny spots to large blotches as large as your hand . It may appear suddenly on a small area of the skin or affect across large areas, depending on the severity of the problem.
The symptoms of itchy nettle rash associated with hives include:
The risk factors, conditions /factors that increase your risk of developing hives, are as follows:
Hives is common, and having some of risk factors mentioned above can put you at higher risk than others.
It can be acute or chronic. Acute or short-term hives can affect about 1 out of 5 people at some point in their lives. Chronic or long-term hives is less common, but it is more difficult to treat.
Causes
Some people have hives when a trigger leads to high levels of histamine and other certain chemicals in the skin.
What Is Rheumatoid Vasculitis
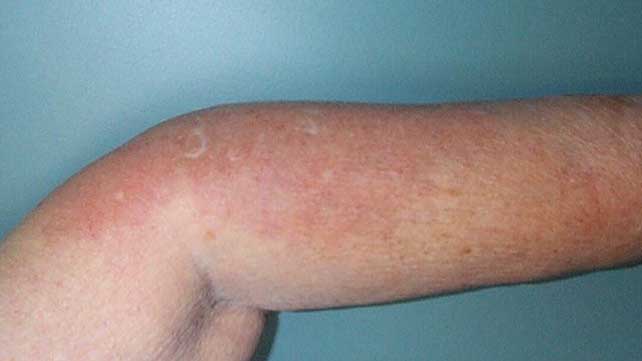
Vasculitis is a serious complication of rheumatoid arthritis. While rheumatoid arthritis affects the body’s joints, vasculitis is a condition in which blood vessels become inflamed. When blood vessels become inflamed, they may become weakened and increase in size, or become narrowed, sometimes to the point of stopping blood flow. The blood vessels most often involved are arteries that bring blood to the skin, nerves, and internal organs. Veins can also be involved.
Also Check: Does Glucosamine Help Arthritis Pain