What Are The Signs And Symptoms Of Ra
With RA, there are times when symptoms get worse, known as flares, and times when symptoms get better, known as remission.
Signs and symptoms of RA include:
- Pain or aching in more than one joint
- Stiffness in more than one joint
- Tenderness and swelling in more than one joint
- The same symptoms on both sides of the body
- Weight loss
What Are The Complications Of Ra
Rheumatoid arthritis has many physical and social consequences and can lower quality of life. It can cause pain, disability, and premature death.
- Premature heart disease. People with RA are also at a higher risk for developing other chronic diseases such as heart disease and diabetes. To prevent people with RA from developing heart disease, treatment of RA also focuses on reducing heart disease risk factors. For example, doctors will advise patients with RA to stop smoking and lose weight.
- Obesity. People with RA who are obese have an increased risk of developing heart disease risk factors such as high blood pressure and high cholesterol. Being obese also increases risk of developing chronic conditions such as heart disease and diabetes. Finally, people with RA who are obese experience fewer benefits from their medical treatment compared with those with RA who are not obese.
- Employment. RA can make work difficult. Adults with RA are less likely to be employed than those who do not have RA. As the disease gets worse, many people with RA find they cannot do as much as they used to. Work loss among people with RA is highest among people whose jobs are physically demanding. Work loss is lower among those in jobs with few physical demands, or in jobs where they have influence over the job pace and activities.
Early Signs Of Arthritis In The Legs
The term arthritis refers to redness and swelling of the joints characterized by joint pain and stiffness. A joint is the area where two bones meet. The two bones at the site of the joint are separated by a cushioning tissue called the cartilage that protects the joint and facilitates proper movement. The joint space is lined by the synovial membrane that secretes a fluid called synovial fluid. Synovial fluid lubricates and protects the joints to allow for adequate movement. Arthritis may result when any of the joint structures are damaged. Leg arthritis affects the joints of the hips, knees, ankles, or feet. There are over 100 types of arthritis. The most common types of arthritis affecting the legs are
- Osteoarthritis: This is the most common type of arthritis. It occurs due to wear and tear of the joint cartilage that happens with increasing age.
- Rheumatoid arthritis: In this type of arthritis, the bodys immune system attacks and damages the joints.
- Gout: This occurs due to excessive deposition of uric acid crystals in the joints, which causes joint inflammation.
- : This refers to arthritis that occurs as a result of joint infection.
- Post-traumatic arthritis: This type of arthritis results because of injury or after a surgery or other invasive procedure on the joint.
- Psoriatic arthritis: People who suffer from a long-term skin condition, psoriasis, may develop psoriatic arthritis along with the skin manifestations such as plaques.
You May Like: What Does Arthritic Changes Mean
Chronic Joint Pain In The Knees Elbows Hips And Shoulders
Some RA patients may also experience inflammation in the joints of the knees, elbows, and hips. One or both shoulders might also become swollen, lessening range of motion so lifting or reaching becomes painful.
Rheumatoid arthritis typically does not affect the lower back, though a person may experience back pain if they are having difficulty moving other joints or walking, says Manno.
In a small percentage of people, the joint swelling can come and go, sometimes moving around to different joints and even disappearing for a time, a condition known as palindromic rheumatism. But in the vast majority of people, the joint swelling persists and worsens until its treated with medication. With treatment, the majority of people can achieve a significant lessening of symptoms or possibly even remission.
Osteoarthritis Vs Rheumatoid Arthritis
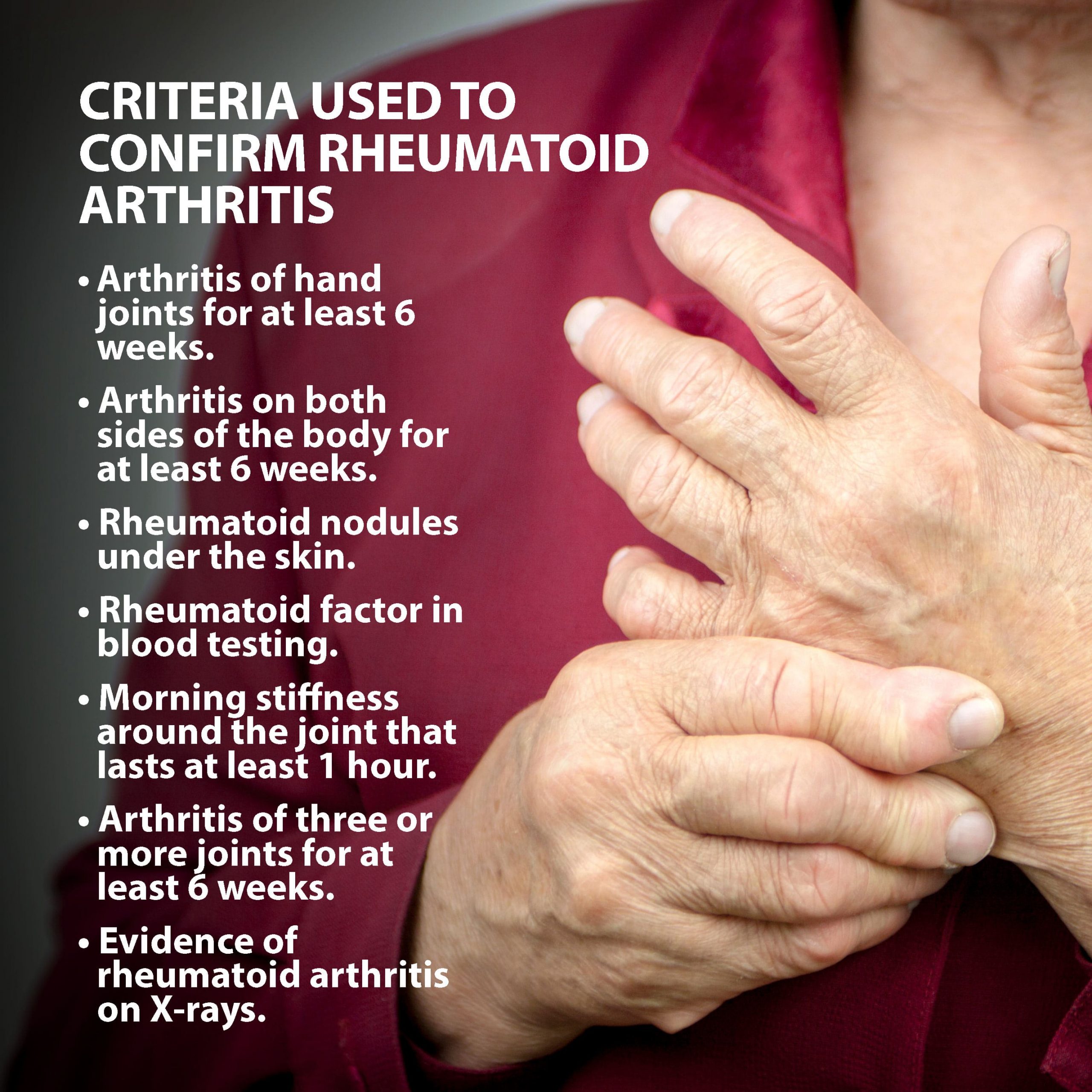
Osteoarthritis is the most common type of arthritis, affecting about 27 million people in the United States. Osteoarthritis is caused by degeneration of cartilage, and is also known as degenerative arthritis. In contrast, rheumatoid arthritis is caused by the immune system attacking the joints. This autoimmune process causes systemic inflammation, while in osteoarthritis, mechanical degeneration causes localized inflammation.
Osteoarthritis commonly affects a single joint, such as one knee. Trauma, such as multiple injuries playing sports, is a risk factor for osteoarthritis. On the other hand, rheumatoid arthritis usually affects three or more joints, in a symmetric distribution . Rheumatoid arthritis frequently, but not always, causes elevation in blood levels of substances that are markers of systemic inflammation such as the ESR and CRP . In contrast, osteoarthritis does not cause abnormal blood test results. Both osteoarthritis and rheumatoid arthritis are hereditary. For example, if a woman has osteoarthritis or rheumatoid arthritis, her/his children are at increased risk of developing the same type of arthritis.
You May Like: Can Arthritis Cause A Rash
Other Causes Of Hand And Finger Symptoms
RA hand symptoms can mimic those of other conditions, such as osteoarthritis. Some members of myRAteam discovered their hand pain was actually related to secondary Raynauds disease, a vascular condition that affects 10 percent to 20 percent of people with RA. Psoriatic arthritis, another autoimmune disease, can also cause hand and finger dysfunction as can pinched nerves in the neck.
A rheumatologist can diagnose the specific cause of symptoms in the hand with a physical exam and X-rays. X-rays can detect narrowing of joint space or erosions of the bone that could signal RA. Ultrasound and MRI technology has improved the ability to spot joint damage earlier in the course of the disease.
One Types Of Arthritis In Hands
Rheumatoid arthritis is included in one of inflammatory arthritis types. The disease is mainly identified by joint inflammation in relatively chronic condition occurs in some part of the human body including knees, fingers, joints, and hands.
Rheumatoid arthritis is feared by most people since it can result in systemic illness that affects many organs of the human body.
However, there is no exact factor of symptoms of arthritis in hands found by scientists that becomes the cause of the disease till now.
Also Check: How To Ease Arthritis Pain In Hands
Don’t Miss: Rheumatoid Arthritis Pain Relief
Causes Of Rheumatoid Arthritis In The Hands
Joints are susceptible to inflammation for people with rheumatoid arthritis. The nature of an autoimmune disease is to attack cells that the body thinks are dangerous.
White blood cells, called leukocytes, are sent out to the hand joints. These white blood cells trigger inflammation in the synovial joints, which are the joints that allow for movement.
Symptoms start when the immune system malfunctions and attacks the joints in the hands
Loss Of Joint Function
Because rheumatoid arthritis leads to pain, swelling, and tenderness of the involved joints, there is the loss of joint function. The swelling and sensitivity impede the full motion and stability of the joint and it becomes incapable of carrying the movement with confidence, balance, and completeness.
- This loss of joint function leads to limping, lack of coordination, loss of grip and dexterity, and disability.
Don’t Miss: Ra Pain Relief
Signs Of Arthritis In The Hand Causes & Treatment
Arthritis is inflammation of one or more joints in the body. There are over 100 different types of arthritis but the most common types of arthritis are osteoarthritis and rheumatoid arthritis .
Osteoarthritis is the most common type of arthritis that often develops with age. It is a chronic condition in which the cartilage between the bones that cushions the joints wears down, and as it does, the bones rub against each other causing pain, stiffness, swelling, and reduced joint motion. Osteoarthritis most commonly affects the hands, knees, hips, feet, and spine, though it can affect almost any joint in the body.
Rheumatoid arthritis is a chronic autoimmune disorder characterized by persistent joint pain, swelling, and stiffness that affect both sides of the body. It can also affect the skin, heart, lungs, and eyes.
In osteoarthritis, symptoms are usually worse in the patients dominant hand, while in rheumatoid arthritis, both hands are usually affected.
The first signs of arthritis in the hands may include:
- Pain in the hands
How Is Ra Treated
RA can be effectively treated and managed with medication and self-management strategies. Treatment for RA usually includes the use of medications that slow disease and prevent joint deformity, called disease-modifying antirheumatic drugs biological response modifiers are medications that are an effective second-line treatment. In addition to medications, people can manage their RA with self-management strategies proven to reduce pain and disability, allowing them to pursue the activities important to them. People with RA can relieve pain and improve joint function by learning to use five simple and effective arthritis management strategies.
Don’t Miss: How To Relieve Arthritis Pain In Lower Back
Lifestyle Changes That Help Ease Ra Symptoms
In addition to treatment with drugs, the following remedies and lifestyle approaches can help alleviate symptoms at any stage of RA:
Occupational or Physical Therapy Rheumatologists frequently refer patients to occupational or physical therapy practitioners to help patients find ways of moving that are less painful, and that strengthen muscles, says Manno. Decreased movement can cause muscles to atrophy and can reduce a persons cardiovascular fitness.
Generalized Symptoms Of Rheumatoid Arthritis Of Hands
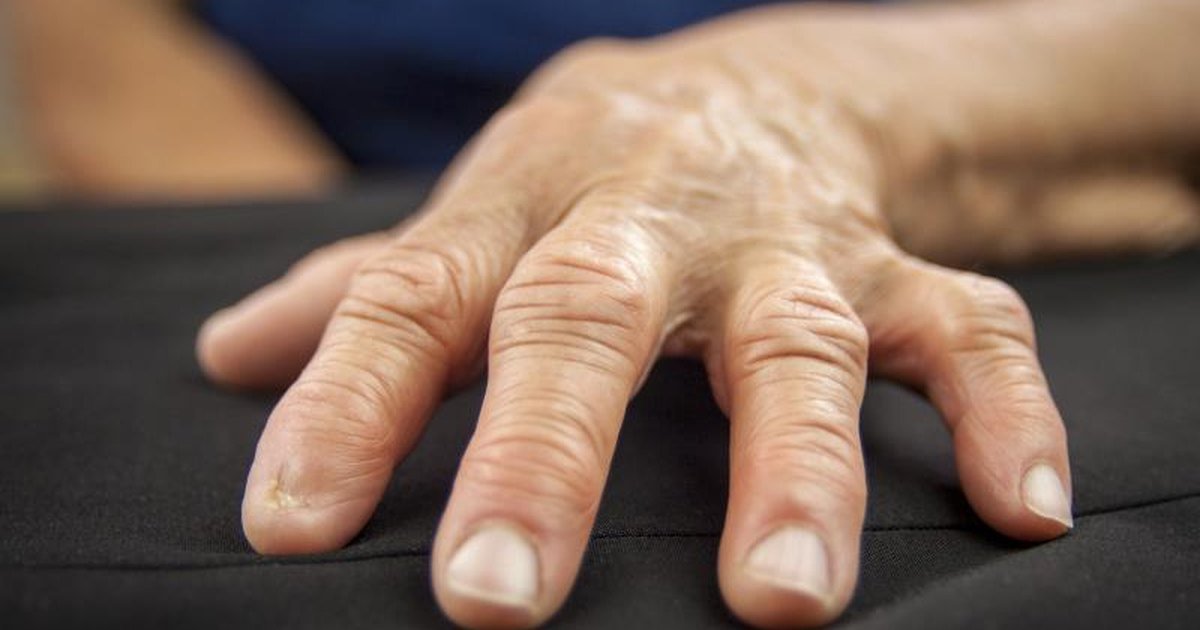
- Fever Fever is observed during early stage of the disease. Fever often accompanies the inflammation of interphalangeal joint, which is tender on touch.
- Weakness Patient complaints of generalized weakness during inflammatory phase, early stage of the disease.
- Fatigue and Tiredness Symptoms of fatigue and tiredness are observed during all the stages of rheumatoid arthritis of hand. During initial phase of joint inflammation the tiredness is caused by severe inflammation involving multiple joints.
- Loss of Appetite.
- Numbness Patients often have problems with numbness and tingling in their hand because the swelling of the tendons causes pressure on the adjacent nerve. They may make a squeaky sound as they move joints and sometimes the joints snap or lock because of the swelling.
Recommended Reading: How To Avoid Arthritis In Hands
Chest Pain/shortness Of Breath
Rheumatoid arthritis can affect blood vessels throughout the entire body, including the heart. People with RA are at a greater risk for heart attacks and other cardiovascular issues. Additionally, shortness of breath could be a sign that something is wrong, such as a lung infection or inflammation. If you frequently find yourself running out of breath or suffering chest pain, please call a rheumatologist as soon as possible.
Also Check: Symptoms Of Arthritis In Legs And Knees
Mri And Cat Scan5 For Rheumatoid Arthritis Of Hands
- Findings of the X-ray Confirmed.
- Joint Erosions Joint erosions are observed with thinning of cartilage and ligament subluxation.
- Subcutaneous Nodules SN are observed within subcutaneous tissue over hand and finger.
- Osteopenia Decreased bone density.
- Synovial Membrane Thickening of synovial membrane is better observed with MRI.
Read Also: How To Get Rid Of Arthritis In Fingers
Chronic Swelling And Inflammation In Synovial Lining In Joints
No one knows exactly why RA targets the small joints of the feet and hands first, but experts do know that the synovial lining is involved.
The synovial lining is the thin layer of cells between all joints. A joint is where two bones meet, and the synovial lining is the thin layer of cells between them. Joints are covered in cartilage to cushions them, and the synovial lining between joints nourishes both the cartilage and bones.
Experts believe that RA develops when the white blood cells that normally protect the body turn on the joints instead, causing inflammation. This may occur because a person is predisposed, due to genes or environmental factors.
This inflammation is why people with RA experience pain, heat, and swelling early in the disease process .
How Arthritis Of The Hand Is Diagnosed
Your doctor will examine you and determine whether you have similar symptoms in other joints and assess the impact of the arthritis on your life and activities. The clinical appearance of the hands and fingers helps to diagnose the type of arthritis. X-rays will also show certain characteristics of rheumatoid arthritis, such as narrowing of the joint space, swelling and diminished bone density near the joints, and erosions of the bone. If your doctor suspects rheumatoid arthritis, he or she may request blood or other lab tests to confirm the diagnosis.
Recommended Reading: Is Ra Curable
Tests Used To Help Diagnose Rheumatoid Arthritis
There are various tests that will be conducted including a blood test to determine if you test positive for Rheumatoid Factor.
Rheumatoid factors are a variety of antibodies that are present in 70% to 90% of people with RA.
However, rheumatoid factors can be found in people without RA or with other autoimmune disorders.
Other tests, including X-rays, MRI, ultrasound, and other scans, may be ordered.
These tests are used to help the doctor make an accurate diagnosis.
- Blood Test: the blood test will not provide a definitive answer if you have RA, but it will allow doctors to review:
- rheumatoid factor check for rheumatoid factor antibodies that collect in the synovium of the joint. These antibodies are present in about 80% of RA patients
- erythrocyte sedimentation rate and C-reactive protein A high erythrocyte sedimentation rate may indicate inflammation in the jointsas do high levels of C-reactive protein
- complete blood count. This includes hemoglobin and hematocrit tests, which may reveal anemia, an indicator of RA.
Read Also: Does Arthritis Cause Redness
Talk To Your Doctor About Surgery Options
If pain is unrelenting or there is loss if function in the hands, your rheumatologist may refer you for a surgical evaluation, particularly when theres an anatomic defect that can be corrected, says Dr. Albayda.
Surgery may involve removal of inflamed joint linings, tendon repair, joint fusions, or joint replacements. Depending on the joint involved, the degree of damage, and other factors, you hand surgeon will determine the most appropriate treatment to help correct deformities, relieve pain, or improve function.
Read Also: Rheumatoid Arthritis Knee Pain Relief
Symptoms By Body Part
The most commonly affected areas during the onset of RA are the small joints in your hands and feet. This is where you may first feel stiffness and an ache.
Its also possible for RA inflammation to affect your knees and hips. Because the disease presents differently in different people, it can go on to affect almost any joint.
Your organs are another area that can be disrupted by RA inflammation:
- Your heart muscle can become damaged.
- Your lungs can become scarred.
- Blood vessel damage can lead to subsequent skin and nerve issues.
See A Physical Or Occupational Therapist

Your doctor may refer you to a physical or occupational therapist to help maintain hand function and dexterity and strengthen joints, say experts. Depending on your needs, a therapist may give you exercises to improve range of motion and function in your hand and wrist, recommend the use of splints or braces to help support joints and ease stress, and suggest new ways to do everyday tasks that may help relieve pain and protect your joints.
Here are some arthritis-friendly hand exercises you can do regularly.
Don’t Miss: Rash With Rheumatoid Arthritis
How Is Ra Diagnosed
RA is diagnosed by reviewing symptoms, conducting a physical examination, and doing X-rays and lab tests. Its best to diagnose RA earlywithin 6 months of the onset of symptomsso that people with the disease can begin treatment to slow or stop disease progression . Diagnosis and effective treatments, particularly treatment to suppress or control inflammation, can help reduce the damaging effects of RA.
Hand Rheumatoid Arthritis Signs And Symptoms
The first signs and symptoms of rheumatoid arthritis may appear in the small joints of the hands. The fingers, thumbs, and wrists may be painful and swollen, with no clear cause. If left untreated, RA symptoms may become more severe over time, and certain joint deformities may develop.
WatchRheumatoid Arthritis Overview Video
Don’t Miss: What To Do For Rheumatoid Arthritis Pain
Numbness In The Hands
Rheumatoid arthritis can cause inflammation of the connective tissues in your hands or feet, leading to painful sensations of tingling or numbness. Though this swelling can occur in any part of the body, its more common around the wrists. When tissues in the hands are being compressed, its referred to as carpal tunnel syndrome.
Malalignment Of One Or More Finger Joints
Over time, the destruction of bone and joint tissue may cause fingers and thumbs to become deformed. While the risk of hand deformities is significant, they are not inevitable.
A diagnosing physician will examine a patients hands, feet, and any other jointslarge or smallthat the patient reports as painful.
Read Are My Painful Joints Caused By Rheumatoid Arthritis or Something Else?
Recommended Reading: Living With Arthritis In Back
Cold Or Discolored Fingers
People with RA are at a higher risk of developing another condition called Raynauds syndrome, which causes color and temperature changes in the fingers.
This issue occurs when the blood vessels in the fingers narrow and decrease even further in size. As a result of this, less blood flow is able to get through to your hands and fingers. Typically the effects of the syndrome are more severe in people whose Raynauds is the result of another condition like RA.
Individuals with Raynauds become extremely sensitive to cold temperatures and may notice their fingers turning a white or blueish color as the blood flow diminishes. Numbness, tingling, or sensitivity in the hands may also accompany these changes. In severe cases, ulceration of the skin or even gangrene can develop if your Raynauds is not properly treated by a healthcare provider.