Poor Circulation Skin Rash
Poor Circulation Skin Rash. Stasis dermatitis is the dark discoloration of the skin, usually a brown pigmentation, due to poor venous drainage in the legs. It is also known as venous eczema. This is usually as a result of poor circulation caused by venous insufficiency, the inability or incompetence of the leg veins to assist with returning .
Can Psoriatic Arthritis Affect Other Parts Of The Body
Having psoriatic arthritis can put you at risk of developing other conditions and complications around the body.
The chances of getting one of these are rare. But its worth knowing about them and talking to your doctor if you have any concerns.
Eyes
Seek urgent medical attention if one or both of your eyes are red and painful, particularly if you have a change in your vision. You could go to your GP, an eye hospital, or your local A& E department.
These symptoms could be caused by a condition called uveitis, which is also known as iritis. It involves inflammation at the front of the eye.
This can permanently damage your eyesight if left untreated.
Other symptoms are:
- blurred or cloudy vision
- sensitivity to light
- not being able to see things at the side of your field of vision known as a loss of peripheral vision
- small shapes moving across your field of vision.
These symptoms can come on suddenly, or gradually over a few days. It can affect one or both eyes. It can be treated effectively with steroids.
Heart
Psoriatic arthritis can put you at a slightly higher risk of having a heart condition. You can reduce your risk by:
- not smoking
- staying at a healthy weight
- exercising regularly
- eating a healthy diet, thats low in fat, sugar and salt
- not drinking too much alcohol.
These positive lifestyle choices can help to improve your arthritis and skin symptoms.
Talk to your doctor if you have any concerns about your heart health.
Crohns disease
Non-alcoholic fatty liver disease
Rheumatoid Arthritis Facial Rash
Luckily, facial spider veins can be treated once the cause is identified. Our body is made up of numerous veins. The venous system has a complex network of tiny veins draining into larger veins. Determining the location and type of vein is extremely crucial to find appropriate treatment for spider veins. Anatomical location of Facial Veins. 1.
Also Check: What Helps Lower Back Arthritis
Don’t Miss: Swollen Hot Finger Joint
How Does Scleroderma Affect The Skin
Scleroderma is a term that just means ‘hard skin.’ Like lupus, patients having scleroderma skin changes have a variable risk for having associated damage to internal organs, especially the kidneys and lungs.
Some patients develop a form of scleroderma that never goes on to cause damage to internal organs. This form of the disease is called localized scleroderma or morphea. However, other patients with scleroderma do develop internal complications relatively soon after the onset of skin problems.
Cutaneous Adverse Effects Of Treatment For Rheumatoid Arthritis
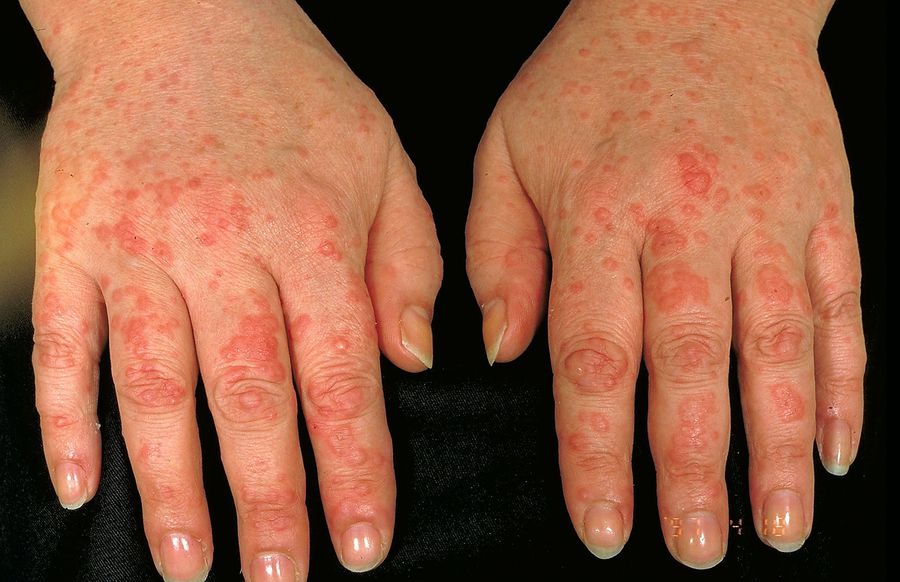
The treatment of rheumatoid arthritis can cause side effects involving the skin.
Disease modifying antirheumatic drugs used in the treatment of rheumatoid arthritis include methotrexate, azathioprine, leflunamide, ciclosporin, and hydroxychloroquine. Skin side effects are well documented.
There are many new and emerging treatments for rheumatoid arthritis including biological treatments, Janus kinase inhibitors, rituximab , tocilizumab with their associated cutaneous side effects. Tumour necrosis factor inhibitors are biologic agents used widely for treatment-resistant rheumatoid arthritis. Many cutaneous side effects have been reported with their use in rheumatoid arthritis including psoriasis, dermatitis, leukocytoclastic vasculitis, lichenoid drug eruptions, and non-infectious cutaneous granulomatous reactions, such as disseminatedgranuloma annulare, sarcoidosis-like lesions, and interstitial granulomatous dermatitis.
Dermatological side effects of tumour necrosis factor inhibitors
Also Check: Ways To Relieve Arthritis Pain In Hands
Who Should Diagnose And Treat Ra
A doctor or a team of doctors who specialize in care of RA patients should diagnose and treat RA. This is especially important because the signs and symptoms of RA are not specific and can look like signs and symptoms of other inflammatory joint diseases. Doctors who specialize in arthritis are called rheumatologists, and they can make the correct diagnosis. To find a provider near you, visit the database of rheumatologistsexternal icon on the American College of Rheumatology website.
Dont Miss: Is Banana Good For Rheumatoid Arthritis
Rheumatoid Arthritis Skin Problems
Rheumatoid Arthritis is a systemic autoimmune disease that affects the entire body. It does this when the immune system attacks its own healthy tissues because it thinks theyre sick.Most of the time, rheumatoid arthritis is characterized by joint pain and inflammation, and in severe cases, inflammation can also affect the bodys organs.
RA is also associated with a number of skin conditions, and the severity of skin involvement indicates the severity of the disease. In addition, the medications used to treat it may also affect the skin.
Read Also: Arthritis Skin Rash
Lupus Erythematosus Nonspecific Disease
Lupus erythematosus-nonspecific disease can relate to SLE or another autoimmune disease, but nonspecific cutaneous features are most often associated with SLE.
Common cutaneous features seen include:
- this is an abnormal response to UV radiation that is present in 5093% of patients with SLE
- Mouth ulcers these are present in 2545% of patients with SLE
- Nonscarring hair loss in SLE presenting as coarse, dry hair with increased fragility .
Cutaneous vascular disease is also common. Forms of cutaneous vascular disease include:
- Raynaud phenomenon this presents with focalulceration in the fingertips and periungual areas that can cause pitted scarring, haemorrhage and other nail fold complications
- Vasculitisleukocytoclastic vasculitis: urticarial vasculitis presenting with tender papules and plaques over bony prominences and medium or large vessel vasculitis can occur, presenting with purpuric plaques with stellate borders, often with necrosis and ulceration or subcutaneous nodules
- Thromboembolic vasculopathies these may have a similar clinical presentation to vasculitis, but vessel occlusion is due to blood clots
- Livedo reticularis characterised by net-like blanching red-purple rings that commonly arise on the lower limbs
- Erythromelalgia characterised by burning pain in the feet and hands, and with macular erythema it is associated with heat exposure.
Vascular disease in lupus erythematosus
- Rheumatoid nodules.
Ways Ra Can Lead To Skin Eruptions
1. Out-of-whack immune system. In RA, your immune system has already attacked your own joints. This revved-up immune system can also be related to eczema or allergies that affect the skin, says Dr. Deane.
2. Tamped down immune defenses. Dampening your immune system with medication can help control your RA symptoms, but they may leave your skin more vulnerable to infection, Dr. Deane cautions.
If you have a rash thats rapidly spreading, is bright red, or is accompanied by fever or malaise, we think about infections such as cellulitis a potentially dangerous bacterial infection of the skin, says Dr. Deane.
3. Other medication reactions. Rashes can occur at the site where you inject a biologic medication. These are usually mild and clear up in a few days. More worrisome are overall rashes or hives that appear during or within 24 hours after you receive infusion of a drug directly into your bloodstream.
Unfortunately, theres a rare but real chance for an allergic-type reaction from infusions of RA medications. These usually appear within 12-24 hours of the infusion and need immediate medical attention, Dr. Deane says.
Several drugs that are used to treat RA, including TNF inhibitors, may sometimes induce or worsen psoriasis, a skin disease that creates an itchy scaly rash .
Long-term use of corticosteroids, such as prednisone, can also leave the skin more prone to bruising or tears.
Also Check: Vicks Vapor Rub For Arthritis
What Are The Complications Of Ra
Rheumatoid arthritis has many physical and social consequences and can lower quality of life. It can cause pain, disability, and premature death.
- Premature heart disease. People with RA are also at a higher risk for developing other chronic diseases such as heart disease and diabetes. To prevent people with RA from developing heart disease, treatment of RA also focuses on reducing heart disease risk factors. For example, doctors will advise patients with RA to stop smoking and lose weight.
- Obesity. People with RA who are obese have an increased risk of developing heart disease risk factors such as high blood pressure and high cholesterol. Being obese also increases risk of developing chronic conditions such as heart disease and diabetes. Finally, people with RA who are obese experience fewer benefits from their medical treatment compared with those with RA who are not obese.
- Employment. RA can make work difficult. Adults with RA are less likely to be employed than those who do not have RA. As the disease gets worse, many people with RA find they cannot do as much as they used to. Work loss among people with RA is highest among people whose jobs are physically demanding. Work loss is lower among those in jobs with few physical demands, or in jobs where they have influence over the job pace and activities.
What Are The Signs And Symptoms Of Ra
With RA, there are times when symptoms get worse, known as flares, and times when symptoms get better, known as remission.
Signs and symptoms of RA include:
- Pain or aching in more than one joint
- Stiffness in more than one joint
- Tenderness and swelling in more than one joint
- The same symptoms on both sides of the body
- Weight loss
You May Like: Side Effects Of Arthritis
Signs And Symptoms Of Psoriatic Arthritis
For most people, psoriatic arthritis develops years after psoriasis. Contact your dermatologist if you have psoriasis and any of these signs or symptoms:
- A very noticeable swollen finger or toe
- Swollen and tender joints
- Stiffness when you wake up or sit for hours that fades as you move
- Nails that are pitted
- Nail separating from nail bed
- Lower back pain
Cognitive Mood And Emotional Disturbances

Chronic illnesses and pain have long been linked with depression. Changes in lifestyle, a loss of ability or function, and pain can all contribute to depression.
A 2019 research review pointed to RA causing disruptions to the chemicals and neurotransmitters in the brain. All of these together can lead to emotional and mood disturbances, as well as trouble concentrating and other cognitive issues.
People with RA are about 70 percent more likely to develop gastrointestinal problems than people without the condition, according to the Arthritis Foundation. These problems are likely due to a number of things, including:
- medications youre taking to treat RA
- other conditions you have alongside RA
- infections
Recommended Reading: Rheumatoid Arthritis Article
What Are The Blood Tests For Autoimmune Diseases
There are some blood tests one can do that can reflect how active the immunological disease is inside our bodies in diseases like rheumatoid arthritis, lupus, and scleroderma. These tests are routinely ordered by doctors who are treating such patients. This information can be very helpful at times both in the diagnosis of the specific problem and in guiding treatment of the problems over time.
Rheumatoid Arthritis Rash Diagnosis
Not all rashes in people with rheumatoid arthritis are related to their RA. For instance, rashes from shingles, psoriasis and contact dermatitis are common. Since rashes can be difficult to identify on your own, see a board-certified dermatologist for an accurate diagnosis.
Your doctor may be able to identify the rash based on symptoms and appearance. In some cases, the provider may want to perform a skin biopsy. Biopsy is the only definitive laboratory test for rheumatoid vasculitis.
If you suspect your RA medication may be the cause of your rash, keep taking it until you speak with your rheumatologist. Your rheumatologist and dermatologist can work together to manage your RA and keep your skin as healthy as possible.
Don’t Miss: How To Stop Arthritis Pain In Hands
Who Will Be Responsible For My Healthcare
Youre likely to see a team of healthcare professionals.
Your doctor, usually a rheumatologist, will be responsible for your overall care. And a specialist nurse may help monitor your condition and treatments. A skin specialist called a dermatologist may be responsible for the treatment of your psoriasis.
You may also see:
- a physiotherapist, who can advise on exercises to help maintain your mobility
- an occupational therapist, who can help you protect your joints, for example, by using splints for the wrist or knee braces. You may be advised to change the way you do some tasks to reduce the strain on your joints.
- a podiatrist, who can assess your footcare needs and offer advice on special insoles and good supportive footwear.
Risks For Bruises And Sunburns Increase With Some Medication
Certain RA medication may make bruising of the skin more likely to occur, either by thinning the skin or interfering with blood clotting. Another common side effect of RA medication is an increased sensitivity to sunlight. When taking these drugs, its important to practice sun safety rules, including avoiding direct sunlight, especially between the hours of 10 a.m. and 2 p.m.
If you have any concerns over medication side effects, speak to your doctor. He may prescribe a lower dose or switch your medication entirely, depending on the severity. But dont despair if you experience minor irritation when you begin a new drug. Some medications can take from two weeks to up to three or four months to work properly, Tehrani says, so just because something isnt 100 percent working for you immediately, dont give up.
You May Like: Cure For Arthritis In Hands
Shortness Of Breath Or Coughing
The lungs are often affected in people diagnosed with rheumatoid arthritis. Lung conditions may cause coughing, shortness of breath, and chest pain. Rarely, these conditions become life-threatening.
- Interstitial lung disease is an umbrella term used to describe many disorders that cause scarring of the walls of the lungs and certain nearby structures. In people with RA, scarring is typically caused by chronic inflammation. The initial symptoms of interstitial lung disease typically include shortness of breath and a cough.
- Pleural effusion, also called pulmonary effusion or water on the lungs, occurs when fluid collects in the chest cavity outside the lungs. Pleural effusion can cause sharp chest pain, coughing, and shortness of breath. It may be noticeably more difficult to breathe when lying down.
nodules in the lungs typically have no symptoms but may increase the risk for potentially life-threatening conditions, such as a collapsed lung.5,6Rheumatoid nodules in the lungs are rare and account for less than 1% of all rheumatoid nodules.
The chances of developing lung conditions related to RA are increased by smoking.
Dermatologic Signs Of Rheumatoid Arthritis
Senior Care Consultant Pharmacist andPresident of MZ Associates, Inc.Norwich, New Yorkwww.mzassociatesinc.com
US Pharm. 2009 34:22-24.
Rheumatoid arthritis , the most common inflammatory arthritis, is a chronic autoimmune disease and an important cause of disability in seniors.1-3 Medications for RA account for approximately 10% of the total cost of treating a patient with this condition .2 When comparing patients of similar age and gender, the cost of treating a patient with RA is three times as high as the medical care for a patient without this illness.2
While RA usually presents between the ages of 25 and 50, its prevalence increases with advancing age up to 80 years and new cases may occur even in the very old.3-5 Worldwide, RA affects approximately 1% of the population and affects women two to three times more often than men.4,6 In patients age 15 to 45, women predominate by a 6:1 ratio in seniors older than 60 years, the sex ratio is approximately equal.2 The course of this condition is unpredictable, and its progression is most rapid during the first through sixth year after diagnosis.1 Permanent abnormalities of the joint develop within 10 years in 80% of patients.1
Don’t Miss: Back Arthritis Remedies
What Causes Rheumatoid Arthritis
Rheumatoid arthritis is multifactorial in origin. Although regarded as autoimmune with anti-citrullinated proteinantibodies and rheumatoid factor , genetic and environmental factors are also important in the pathogenesis. In ACPA-positive disease the most significant association is mapped to the HLA-DRB4 gene. ACPA are found in 60% of patients with rheumatoid arthritis .
Recommended Reading: Is Banana Bad For Arthritis
What Causes Dermatomyositis
The exact cause is not known, but possible causes include:
-
Abnormal genes you are born with
-
Cancer, especially in older people
-
Autoimmune disease, a type of illness that causes the bodys immune system to attack its own tissues
-
An infection, medication, or another exposure in your environment that triggers the disease
Recommended Reading: What Causes Arthritis Flare Ups In Hands
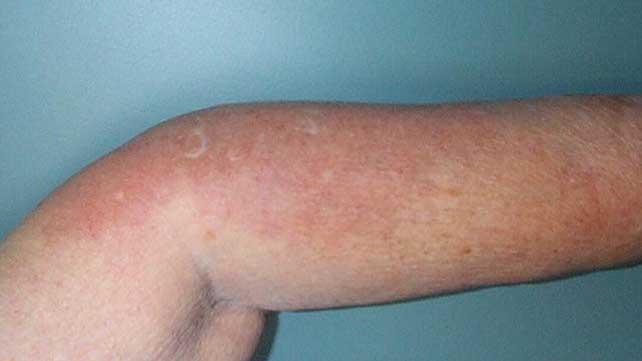
What Is Dermatomyositis
Dermatomyositis is a rare disease that causes muscle inflammation and skin rash. Its one of a group of muscle diseases that cause muscle inflammation and swelling. It’s different from other muscle diseases because it also causes skin problems. Dermatoyositis is the term used to describe both muscle and skin symptoms.
It can occur at any age, but it most often affects adults ages 50 to 70. Women are twice as likely as men to be diagnosed with the disease. Some people with the disease also have a connective tissue disorder, such as lupus or rheumatoid arthritis.
Arthritis And Your Skin
Learn about the various ways having arthritis can affect the skin.
Arthritis is often referred to as an invisible disease because the inflammation and pain that affect the joints are often difficult to see. But some conditions that accompany different forms of arthritis may not be so invisible, because they affect our largest and most visible organ: our skin.
For example, a red or purplish rash across the cheeks and bridge of the nose often occurs in people with lupus, and the scaly skin of psoriasis is present in almost all people with psoriatic arthritis.
But bruises, bumps and lesions on the skin can occur along with many other forms of arthritis. They often signal an underlying problem caused by either the disease or the medications used to treat it that should not be ignored.
Here are several to watch for:
Increased Sun Sensitivity
Skin reddening or burning that occurs with sun exposure could simply be a sign that you should use more sunscreen or spend more time in the shade. But if you notice you burn more easily than you once did or you develop a rash or hives when you are in the sun, you are likely suffering from photosensitivity, says Jeffrey Weinberg, MD, associate clinical professor of dermatology at Mount Sinai School of Medicine in New York.
Cold, Discolored Fingers or Toes
Multiple Sores or Purple Spots
Unusual Bruising
Red or Purple Lines Under the Skin
A Wound That Doesnt Heal
Quick Links
You May Like: Does Rheumatoid Arthritis Cause Itching