From Achy Joints To Dry Eyes Heres What You May Expect To Feel When Experiencing Ra Symptoms
by Health Writer
Unless youre living it, its hard to know exactly what having , a chronic inflammatory disease, is really like. For those who think they may have RA, or those already diagnosed who are concerned about a flare-up, learning about what RA symptoms may actually feel like can be a huge benefit. Thats because recognizing RA symptoms quickly can help you get or adjust an existing treatment planfaster, which helps reduce the amount of long-term damage to your body.
Or maybe you came across this article because youre looking to better empathize with a loved one who has RA. Educating yourself about RA can assist you to better support those with this diagnosis.
Keep reading to learn more about what RA symptoms may feel like, from common aches to advanced complications, and to get a look at how these differ during periods of remission.
How Is Rheumatoid Arthritis Treated
Joint damage generally occurs within the first two years of diagnosis, so its important to see your provider if you notice symptoms. Treating rheumatoid arthritis in this window of opportunity can help prevent long-term consequences.
Treatments for rheumatoid arthritis include lifestyle changes, therapies, medicine and surgery. Your provider considers your age, health, medical history and how bad your symptoms are when deciding on a treatment.
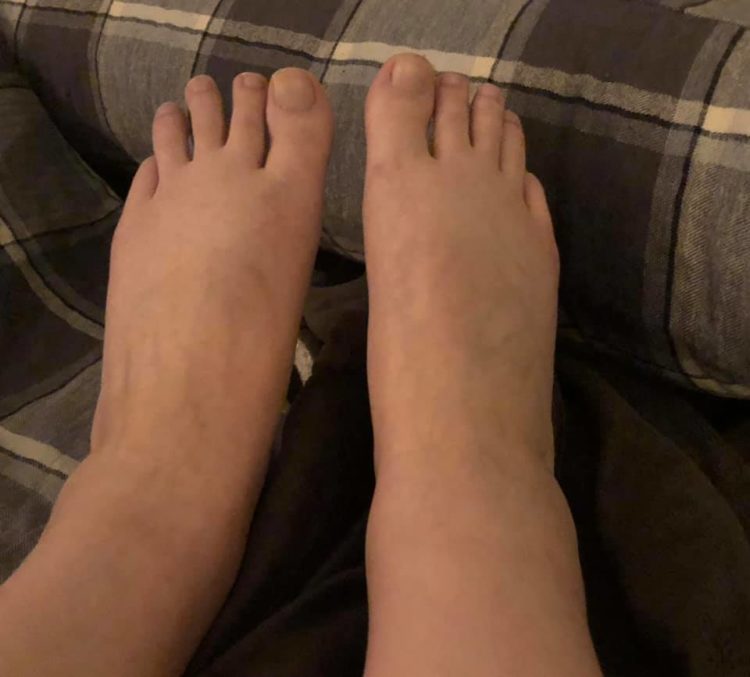
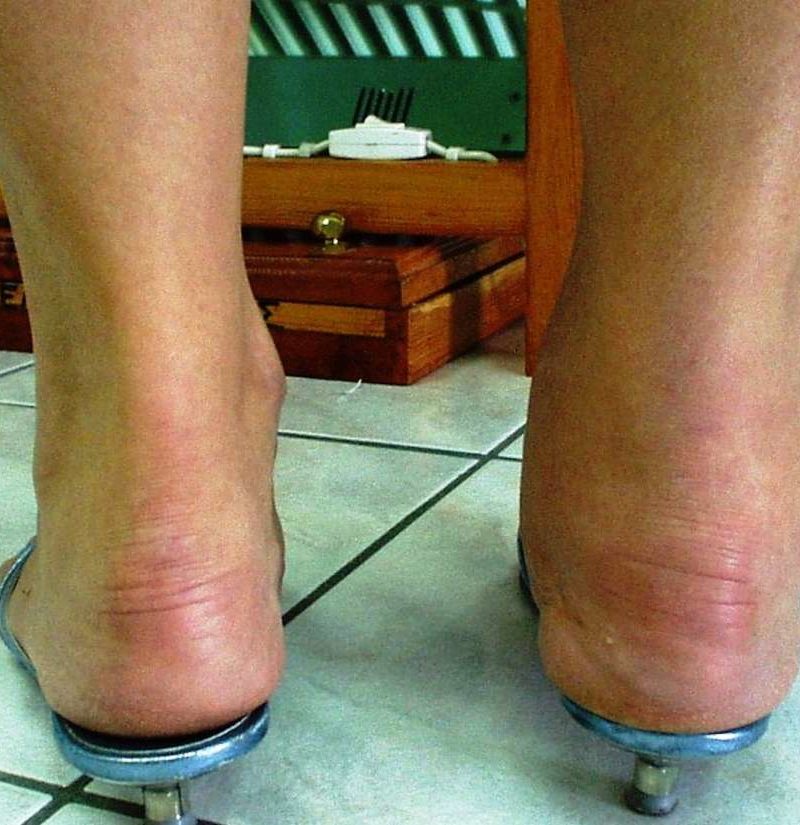
How Does Ra In The Ankles Feel
The main symptom of RA in the ankle joint is inflammation, which leads to swelling, pain, and stiffness in the joint. This can restrict the joints mobility and impair a persons ability to walk and stand.
In the early stages, symptoms may be mild and infrequent. For example, people may begin to feel discomfort when walking up a hill, as this places the ankle joints under extra pressure.
Over time, inflammation can become worse, causing damage to the joints and their surrounding tissues. Symptoms then become more pronounced. The ankles may frequently become painful and stiff, particularly when walking or standing.
In longstanding disease, the ankle joint can become fused and lose range of motion, which impacts gait significantly because the foot cannot flex to allow the necessary push-off. However, as a result of developments in treatments, this is now rare.
When chronic RA causes changes to the structure of the foot, it can lead to calluses, bunions, nodules, and corns.
Aside from inflammation in the joints, other symptoms of RA may include:
Don’t Miss: Which Omega 3 Is Best For Arthritis
Types Of Psoriatic Arthritis
What is psoriatic arthritis? Psoriatic arthritis is a condition that affects the joints, particularly in people with a skin disease called psoriasis. While symptoms can be mild, ongoing treatment is usually needed. Like other types of arthritis, psoriatic arthritis causes pain and stiffness in the joints.
What Are The Four Stages Of Rheumatoid Arthritis
- Stage 1: In early stage rheumatoid arthritis, the tissue around your joint is inflamed. You may have some pain and stiffness. If your provider ordered X-rays, they wouldnt see destructive changes in your bones.
- Stage 2: The inflammation has begun to damage the cartilage in your joints. You might notice stiffness and a decreased range of motion.
- Stage 3: The inflammation is so severe that it damages your bones. Youll have more pain, stiffness and even less range of motion than in stage 2, and you may start to see physical changes.
- Stage 4: In this stage, the inflammation stops but your joints keep getting worse. Youll have severe pain, swelling, stiffness and loss of mobility.
Recommended Reading: How To Slow Arthritis In Knees
Stiffness In The Joints
In addition to pain, this disease causes stiffness in the affected joints. You may have difficulty getting out of bed or walking in the morning because of stiff and painful ankles, knees, or feet. This stiffness is usually worse in the mornings and can last for 45 minutes or more.
RA can also trigger swelling in the affected joints. Long-term inflammation can cause you to feel physically exhausted.
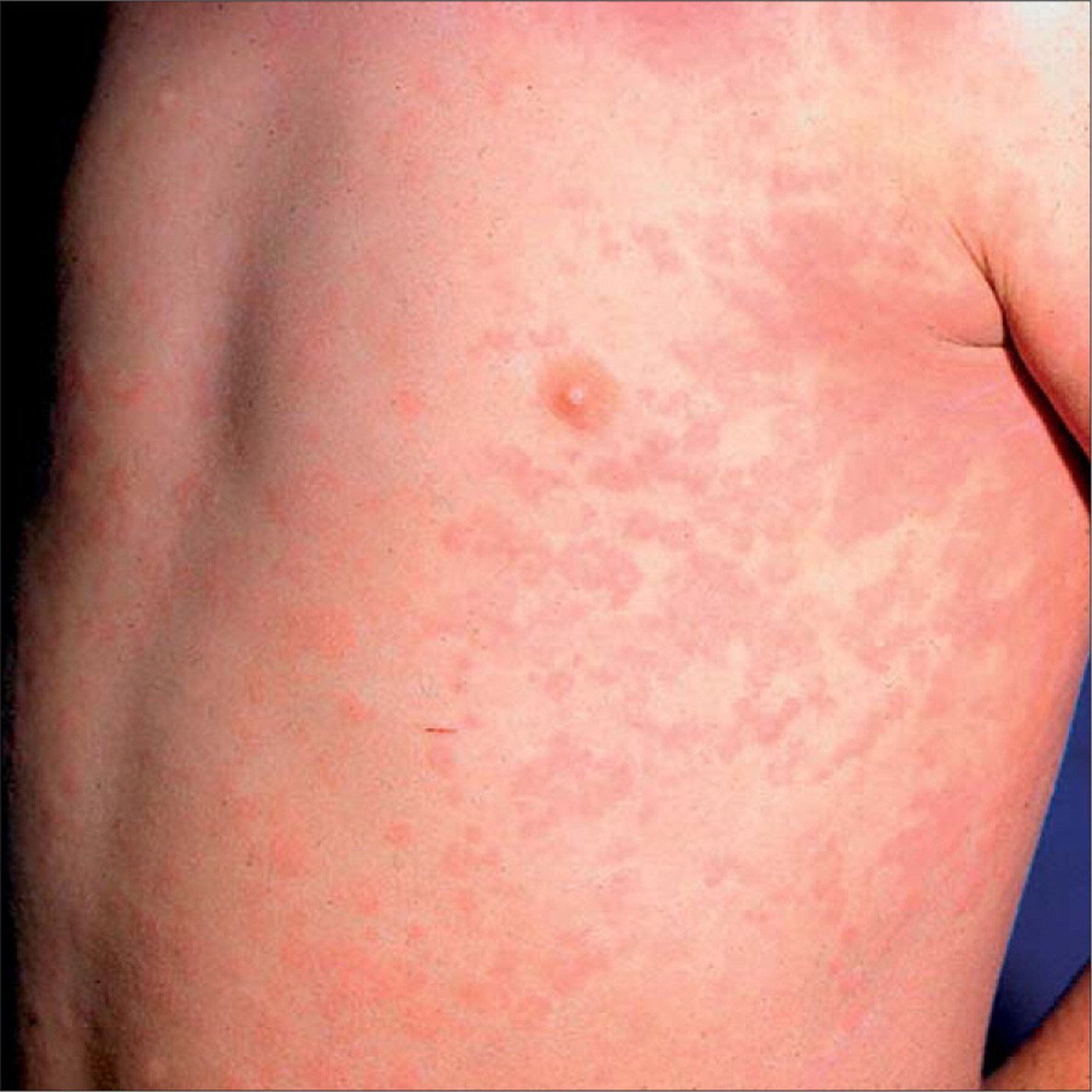
Psoriasis Rash On Back
The fully comprehensive site for all information and support for people affected by psoriasis, psoriatic arthritis and other related or similar conditions. Treatment guides, how to cope and manage this skin and joint condition Access is free to information, stories, tips, blogs, signposting and much more. You can also access, real life stories and short films of what it is like to live, manage .
You May Like: Bee Pollen For Arthritis
You May Like: How To Help Rheumatoid Arthritis Naturally
What Are The Signs And Symptoms Of Ra
With RA, there are times when symptoms get worse, known as flares, and times when symptoms get better, known as remission.
Signs and symptoms of RA include:
- Pain or aching in more than one joint
- Stiffness in more than one joint
- Tenderness and swelling in more than one joint
- The same symptoms on both sides of the body
What Types Of Lifestyle Changes Can Help With Rheumatoid Arthritis
Having a lifelong illness like rheumatoid arthritis may make you feel like you dont have much control over your quality of life. While there are aspects of RA that you cant control, there are things you can do to help you feel the best that you can.
Such lifestyle changes include:
Rest
When your joints are inflamed, the risk of injury to your joints and nearby soft tissue structures is high. This is why you need to rest your inflamed joints. But its still important for you to exercise. Maintaining a good range of motion in your joints and good fitness overall are important in coping with RA.
Exercise
Pain and stiffness can slow you down. Some people with rheumatoid arthritis become inactive. But inactivity can lead to a loss of joint motion and loss of muscle strength. These, in turn, decrease joint stability and increase pain and fatigue.
Regular exercise can help prevent and reverse these effects. You might want to start by seeing a physical or occupational therapist for advice about how to exercise safely. Beneficial workouts include:
- Range-of-motion exercises to preserve and restore joint motion.
- Exercises to increase strength.
- Exercises to increase endurance .
You May Like: How To Treat Arthritis In My Feet
How Do You Test For Rheumatoid Arthritis
The diagnosis of RA is based on a person’s clinical signs and symptoms, but it is supported by laboratory tests, including X-rays and various blood tests. No single blood test makes the diagnosis, but rather it is the pattern of the arthritis, in combination with blood testing and X-ray findings.
If a person has an elevation of one or both of two blood tests sedimentation rate and CRP this suggests the presence of an inflammatory process that could be rheumatoid arthritis. A positive blood test for the rheumatoid factor suggests RA, but this test can also be positive in people who have other disorders. The CCP antibody is more specific to RA than is the rheumatoid factor, but just having the CCP antibody positive does not by itself confirm a diagnosis of RA. Also, it is possible for a person to have RA but still have a normal sedimentation rate and CRP test results, and to test negative for rheumatoid factor or CCP antibody. A diagnosis is made by taking into account the whole picture symptoms, patient history and blood test results.
For example, the tests for RA discussed above are much more meaningful if a patient also has multiple swollen and tender joints, and even more so if the joint swelling is accompanied by fatigue or weight loss. Rheumatologists put all these elements on the scale to make a final diagnosis.
Causes And Risk Factors
RA is the primary cause of rheumatoid nodules, but some people with the disease are more susceptible than others to nodules. Rheumatoid nodules are also a sign of inflammation and heightened immune system activity.
Doctors still do not fully understand why rheumatoid nodules develop, so they cannot predict who will develop them and who will not. However, there are some potential risk factors.
There is a link between rheumatoid nodules and rheumatoid factor , a protein that many people with RA have in their blood. Older research suggests that about
Unless rheumatoid nodules cause pain or other symptoms, they do not usually need treatment. The goal of treatment should be to manage the symptoms of the underlying disease.
Numerous treatments are available to manage RA symptoms, including:
- Disease-modifying antirheumatic drugs : DMARDs slow the progression of RA, with a type called biologics being especially effective. Some research suggests that treatment with the biologic rituximab may reduce the likelihood of nodules developing.
- Physical therapy: Treatment approaches such as joint mobilizations, manual therapy, strength training, and mobility training can help retain mobility and reduce pain.
- Pain relievers: Doctors may recommend taking nonsteroidal anti-inflammatory drugs or using them topically.
- Steroid medications: Steroids, such as prednisone, can reduce the inflammation that causes pain and other symptoms.
A person can discuss the risks and benefits with a doctor.
You May Like: What Is The Meaning Of Arthritis
Pain And Stress Management
Patients can learn strategies to cope with the stress and frustration of living with chronic pain. Relaxation and stress management techniques such as guided imagery, breathing exercises, hypnosis, or biofeedback can be helpful.
Although there is no definitive evidence to support their efficacy, some patients report relief with modalities such as acupuncture, massage, and mineral baths.
Thats Not What Ra Looks Like She Said
Furthermore, the images on the slides were only of the most extreme rheumatoid deformity. As fate would have it, that error didnt go undetected either. Another girl in KBs class exclaimed, Thats not what Rheumatoid Arthritis looks like. My mom has RA. A surprised KB had someone to compare notes with. I wonder whether the professor recognized that with a disease as common as RD, theres bound to be people affected by it sitting in his lecture hall.
You May Like: What Is The Best Medicine For Degenerative Arthritis
The Immune Response And Inflammatory Process
The immune system determines the body’s responses to foreign or dangerous substances such as viruses, toxins, or abnormal proteins. The immune response helps the body to fight infection and heal wounds and injuries. The inflammatory process is a byproduct of the immune response.
Two important components of the immune system that play a role in the inflammation associated with RA are B cells and T cells, both of which belong to a family of immune cells called lymphocytes. Lymphocytes are a type of white blood cell.
A key feature of a healthy immune system is the ability to tell what is normal or “self” and what is foreign and possibly harmful or “non-self.” If the T cell “sees” an antigen as “non-self” or dangerous, it will produce chemicals that cause B cells to multiply and release many immune proteins . These antibodies circulate widely in the bloodstream, recognizing the target particles and triggering inflammation in order to rid the body of the invasion.
For reasons that are still not completely understood, both T cells and B cells become overactive in patients with RA and attack normal tissue as if it were foreign. This is why conditions like RA are referred to as “autoimmune” diseases: the body’s immune system produces antibodies that attack it.
An antigen is a substance that can trigger an immune response. Normally, antigens are substances that are not present in the healthy body.
Psoriatic Rashes In Skin Of Color
Psoriasis rashes can also present differently on different skin tones, which can lead to psoriatic rashes being misdiagnosed more often in people of color.
According to the American Academy of Dermatology:
- In white people, psoriasis tends to be red or pink, and the scale is often silvery white.
- In Hispanic and Latinx people, the psoriasis tends to be salmon-colored and the scale is often silvery white
- In Black people, the psoriasis often looks violet or dark brown, and the scale is often gray.
Read Also: What Does The Rash From Psoriatic Arthritis Look Like
You May Like: What Foods Cause Arthritis To Be Worse
What Are Some Tips For Children Living With Jia
Children with JIA should live life as normal as possible. Attending school, playing sports, participating in extracurricular and family activities regularly is encouraged. Exercise does not make symptoms of arthritis worse. In fact, exercise can help prevent deconditioning, increase muscle strength and muscle endurance to support the joints.
There is no evidence that shows special diets are effective for arthritis, so children can eat a standard, well-balanced diet.
Who Should Diagnose And Treat Ra
A doctor or a team of doctors who specialize in care of RA patients should diagnose and treat RA. This is especially important because the signs and symptoms of RA are not specific and can look like signs and symptoms of other inflammatory joint diseases. Doctors who specialize in arthritis are called rheumatologists, and they can make the correct diagnosis. To find a provider near you, visit the database of rheumatologistsexternal icon on the American College of Rheumatology website.
Don’t Miss: Is Aleve Good To Take For Arthritis
Outlook For People With Rheumatoid Arthritis
RA can affect each person differently, so you may not have all of these symptoms. If you have RA, you may even experience remission, or periods where your symptoms stop.
In addition to medications, there are lifestyle changes that can have a positive impact on your condition. If youve received an RA diagnosis, talk with a doctor about the following strategies:
Rheumatoid Arthritis Is An Autoimmune Disease That Attacks The Joints And Other Body Parts
Rheumatoid arthritis is an autoimmune and inflammatory disease that mainly affects the body’s joints, according to the Centers for Disease Control and Prevention .
The condition, per the CDC, commonly affects the joints in the hands, wrists, knees, ankles and feetand occurs when the lining of those joints becomes inflamed, damaging the joint tissue.
That damage can eventually lead to long-lasting or chronic pain, unsteadiness, and deformity.
The symptoms of RAwhich can include pain, stiffness, tenderness, and swellingcan go through phases where they’re worse and better .
But some symptoms of RA can mimic those of other conditionshere’s what to look out for and how to know if it’s due to RA or something else.
You May Like: How Do Know If You Have Arthritis
How Ra Affects Your Knees
In RA, your immune system attacks and damages the synovial cell lining of your joint. The synovial cell is the connective tissue that lines your joints. RA causes your synovial cells to increase, which causes thickening and inflammation. Its the same with RA in your knees:
Over time, the inflammation can damage the cartilage and ligaments of your knee joints. Along with synovial fluid, these help your knees move and keep your bones from grinding against each other.
As they become damaged, your cartilage wears away and exposes your bone. Bone, unlike cartilage, has pain receptors. As your bone is exposed, your bones start to push and grind against each other. This results in pain and bone damage.
Tissue damage from RA can led to chronic, or lasting, pain, affect your balance and steadiness, and change the appearance of your joints.
A hallmark symptom of RA is tenderness, pain, or joint discomfort that worsens when you stand, walk, or exercise. This is known as a flare. It can range from a mild, throbbing pain to intense, sharp pain.
How Is Rheumatoid Arthritis Diagnosed
Your healthcare provider may refer you to a physician who specializes in arthritis . Rheumatologists diagnose people with rheumatoid arthritis based on a combination of several factors. Theyll do a physical exam and ask you about your medical history and symptoms. Your rheumatologist will order blood tests and imaging tests.
The blood tests look for inflammation and blood proteins that are signs of rheumatoid arthritis. These may include:
- Erythrocyte sedimentation rate or sed rate confirms inflammation in your joints.
- C-reactive protein .
- About 80% of people with RA test positive for rheumatoid factor .
- About 60% to 70% of people living with rheumatoid arthritis have antibodies to cyclic citrullinated peptides .
Your rheumatologist may order imaging tests to look for signs that your joints are wearing away. Rheumatoid arthritis can cause the ends of the bones within your joints to wear down. The imaging tests may include:
In some cases, your provider may watch how you do over time before making a definitive diagnosis of rheumatoid arthritis.
Also Check: What Is Good For Arthritis Inflammation
Talk To Your Doctor About Surgery Options
If pain is unrelenting or there is loss if function in the hands, your rheumatologist may refer you for a surgical evaluation, particularly when theres an anatomic defect that can be corrected, says Dr. Albayda.
Surgery may involve removal of inflamed joint linings, tendon repair, joint fusions, or joint replacements. Depending on the joint involved, the degree of damage, and other factors, you hand surgeon will determine the most appropriate treatment to help correct deformities, relieve pain, or improve function.
What Are The Risk Factors For Developing Rheumatoid Arthritis
There are several risk factors for developing rheumatoid arthritis. These include:
- Family history: Youre more likely to develop RA if you have a close relative who also has it.
- Sex: Women and people designated female at birth are two to three times more likely to develop rheumatoid arthritis.
- Smoking:Smoking increases a persons risk of rheumatoid arthritis and makes the disease worse.
- Obesity: Your chances of developing RA are higher if you have obesity.
You May Like: What To Do When Arthritis Flares Up