Rheumatoid Arthritis And Osteoarthritis
Rheumatoid arthritis and osteoarthritis are both types of arthritis. Both require medication that can help the disease, but the medication have side effects such as affecting the heart, kidney, lungs, and the skin. Neither rheumatoid arthritis and osteoarthritis have any known cures. According to the website healthline.com, Both types of arthritis are more common in women than men. Osteoarthritis and Rheumatoid arthritis are more prevalent in older adults, but RA can develop at any age. Rheumatoid
How To Lose Weight If You Have Arthritis Or Any Other Autoimmune Disorder
- Losing weight is extremely beneficial in managing arthritis. It’s however not so easy to shed kilos with the aches, swelling and fatigue that come with the disease.
Living with Rheumatoid arthritis is life changing for many. The constant aches, swelling and stiffness in joints, and restricted movement can affect the quality of life for many patients. While the condition cannot be fully reversed, it can be controlled by keeping an active lifestyle, managing weight, and with a balanced diet. Rheumatoid arthritis like other autoimmune disorders, occurs when your immune system mistakenly attacks your own body’s tissues.
What makes the body attack its own cells in autoimmune disorders
“The immune system normally guards against germs like bacteria and viruses. When it senses these foreign invaders, it sends out an army of fighter cells to attack them. Normally, the immune system can tell the difference between foreign cells and your own cells. In an autoimmune disorder, the immune system mistakes part of your body, like your joints or skin, as foreign. It releases proteins called autoantibodies that attack healthy cells causing achy joints, fatigue, rashes on the skin, brain fog, gut issues and weight fluctuations,” says Jyotika Diwan Nutrition & Diet Advisor.
Why it’s important to lose weight in Arthritis
Tips to lose weight for arthritis patients
Follow more stories on &
How Are Autoimmune Diseases Treated
There are no cures for autoimmune diseases, but symptoms can be managed. Everyones immune system, genetics and environment are different. That means that your treatment must be unique.
Some examples of medications used to treat autoimmune diseases include:
- Painkillers.
- Limiting processed foods from your diet.
Don’t Miss: How To Avoid Getting Arthritis
How Is Osteoarthritis Diagnosed
The physician will begin with a complete medical history and a physical examination. During the exam, the doctor will look for an enlarged or bumpy joint, signs of swelling, or decreased range of motion. Your doctor may then order x-rays, which can show a decrease in the cartilage space, new bone formation, or incorrect alignment. In some cases, your doctor may perform an aspiration the removal of fluid from a swollen joint or bursa to exclude infection, gout, or rheumatoid arthritis as possible causes of your joint pain.
What Are The Risk Factors For Ra
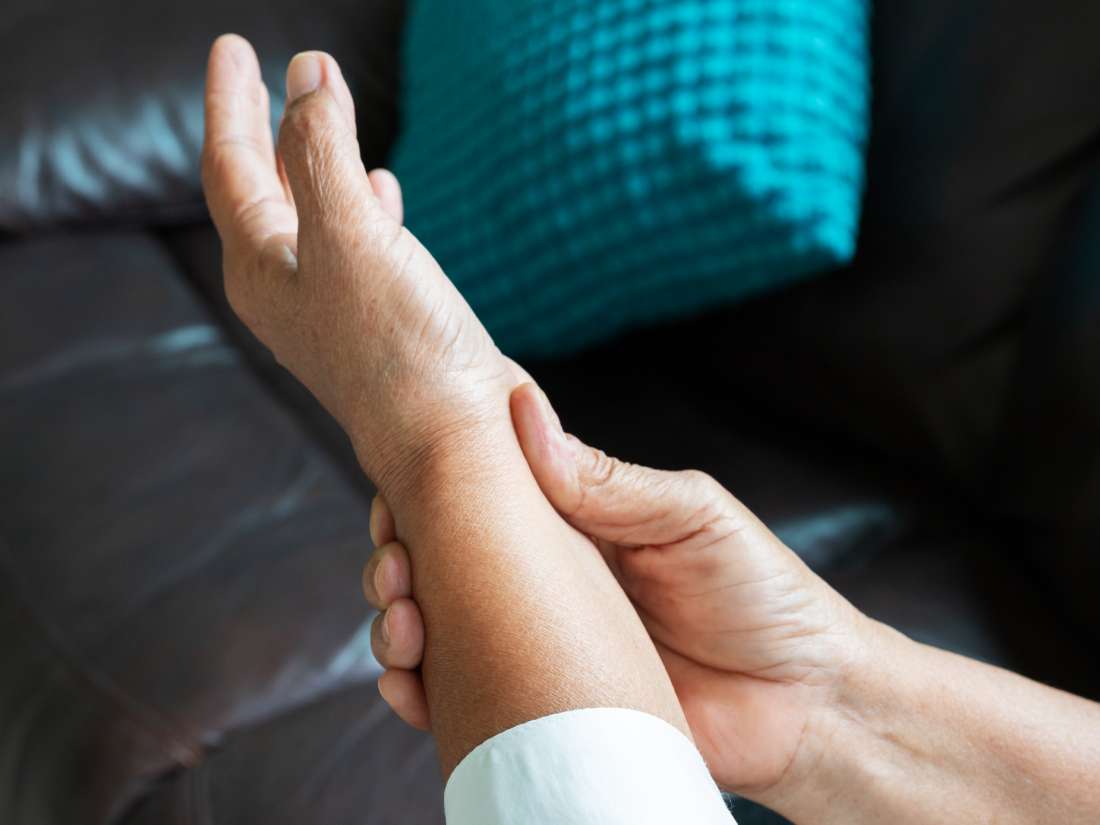
Researchers have studied a number of genetic and environmental factors to determine if they change persons risk of developing RA.
Characteristics that increase risk
- Age. RA can begin at any age, but the likelihood increases with age. The onset of RA is highest among adults in their sixties.
- Sex. New cases of RA are typically two-to-three times higher in women than men.
- Genetics/inherited traits. People born with specific genes are more likely to develop RA. These genes, called HLA class II genotypes, can also make your arthritis worse. The risk of RA may be highest when people with these genes are exposed to environmental factors like smoking or when a person is obese.
- Smoking. Multiple studies show that cigarette smoking increases a persons risk of developing RA and can make the disease worse.
- History of live births. Women who have never given birth may be at greater risk of developing RA.
- Early Life Exposures. Some early life exposures may increase risk of developing RA in adulthood. For example, one study found that children whose mothers smoked had double the risk of developing RA as adults. Children of lower income parents are at increased risk of developing RA as adults.
- Obesity. Being obese can increase the risk of developing RA. Studies examining the role of obesity also found that the more overweight a person was, the higher his or her risk of developing RA became.
Characteristics that can decrease risk
Also Check: What Do You Do For Arthritis In Your Fingers
Risk Factors For Autoimmune Disorders
The exact causes of autoimmune disorders are not known. The risk factors seem to include:
- genetics a predisposition to autoimmune disorders seems to run in families. However, family members can be affected by different disorders for example, one person may have diabetes, while another has rheumatoid arthritis. It seems that genetic susceptibility alone is not enough to trigger an autoimmune reaction, and other factors must contribute.
- environmental factors a family’s susceptibility to autoimmune disorders may be linked to common environmental factors, perhaps working in conjunction with genetic factors.
- gender around three quarters of people with autoimmune disorders are women.
- sex hormones autoimmune disorders tend to strike during the childbearing years. Some disorders seem to be affected, for better or worse, by major hormonal changes such as pregnancy, childbirth and menopause.
- infection some disorders seem to be triggered or worsened by particular infections.
Zagazig University Faculty Of Medicine Rheumatology
Zagazig UniversityFaculty of Medicine Rheumatology and Rehabilitation DepartmentSerum Interleukin-23 Level in Patients With Rheumatoid Arthritis and its Correlation with Disease Activity and Severity Protocol of thesisSubmitted for partial fulfillmentOf M.Sc. DegreeIn Rheumatology and RehabilitationByEnas Tawkal EldesokyMB.B.ChResident of Rheumatology and RehabilitationAt Dekrens General HospitalUnder supervision of Pro. Dr.
Read Also: Can Rheumatoid Arthritis Cause Swollen Lymph Nodes
What Is Autoimmunity How Is It Connected To Vestibular Disorders
Parts of the immune system, working constantly and behind the scenes, patrol the body in search of foreign invaders and relentlessly attack them once found. On rare occasions, in some people the immune system runs amok, identifies the body itself as foreign, and launches a lethal attack. This self-attack is referred to as an autoimmune reaction. In some cases, the reaction takes place in the inner ear, which is called Autoimmune Inner Ear Disease.
The immune system can attack just the ear, attack the ear and some other body part like the eye, or attack the entire body . An autoimmune reaction also creates debris. Even if the ear is not being directly attacked, it can end up with debris transported from distant locations and deposited by the circulation. This debris in the ear can cause problems.
Some autoimmune disorders that can affect the ear include Cogans syndrome, relapsing polychondritis, polyarteritis nodosa, Wegeners granulomatosis, systemic lupus erythematosus, ulcerative colitis, Sjogrens syndrome, and rheumatoid arthritis.
No slam-dunk sort of diagnostic test exists for this type of ear problem. The best tests, such as the 68-kD antigen, are expensive and not widely available. Most tests can easily be positive when there isnt an autoimmune problem and negative when there is the tests arent as accurate as one would like. Sometimes the diagnosis is made only if a favorable response is seen to drug treatment.
Most Common Autoimmune Diseases
1. Rheumatoid Arthritis Rheumatoid arthritis is a chronic inflammation of the lining of the joints, leading to pain and swelling typically in the hands and feet. It can affect anyone, but is most prevalent in women over 40. Rheumatoid arthritis can sometimes affect other organs as well, such as skin, eyes, lungs and blood vessels. As with all autoimmune disorders, treatment focuses on managing pain and minimizing bone erosion and joint damage.
We have more in-depth information on Rheumatoid Arthritis here.
2. Juvenile Rheumatoid Arthritis Juvenile rheumatoid arthritis is the most common form of arthritis in children under 16. Symptoms usually include pain and swelling in the joints, and can vary from moderate to severe. In some cases, symptoms will subside over time while others can persist well into adulthood.
We have more in-depth information on juvenile rheumatoid arthritis here.
3. Systemic Lupus Erythematosus Lupus can be difficult to diagnose because it shares symptoms with many other disorders. The inflammation resulting from lupus can affect many different areas of the body, from the lungs, heart, joints, skin, kidneys, and brain. Like rheumatoid arthritis, lupus is more prevalent in women and can sometimes be identified by a butterfly-shaped rash on the face, along with photosensitivity, fatigue and fever, joint pain, and other skin lesions that worsen under sun exposure.
We have more in-depth information on lupus here.
Don’t Miss: What Supplements Should I Take For Arthritis
What Is Rheumatoid Arthritis
Rheumatoid arthritis, or RA, is an autoimmune and inflammatory disease, which means that your immune system attacks healthy cells in your body by mistake, causing inflammation in the affected parts of the body.
RA mainly attacks the joints, usually many joints at once. RA commonly affects joints in the hands, wrists, and knees. In a joint with RA, the lining of the joint becomes inflamed, causing damage to joint tissue. This tissue damage can cause long-lasting or chronic pain, unsteadiness , and deformity .
RA can also affect other tissues throughout the body and cause problems in organs such as the lungs, heart, and eyes.
Ocular Manifestations Of Autoimmune Disease
SAYJAL J. PATEL, LT, MC, USNR, and DIANE C. LUNDY, CAPT, MC, USN
Naval Medical Center, San Diego, California
Am Fam Physician. 2002 Sep 15 66:991-998.
Patients with autoimmune diseases are frequently encountered by family physicians. It is important to understand not only the systemic effects of these diseases but also their ocular manifestations . Most ocular complications involve the cornea but may also include the conjunctiva, uvea, sclera, retina, and surrounding structures . The majority of these diseases will ultimately need to be referred to an ophthalmologist.
Ocular Manifestations of Autoimmune Disease
Rheumatoid arthritis
Ocular Manifestations of Autoimmune Disease
Rheumatoid arthritis
Cross section of the eye.
FIGURE 1.
Cross section of the eye.
Don’t Miss: What Type Of Doctor Handles Arthritis
What Is The Difference Between Rheumatoid Arthritis And Osteoarthritis
Rheumatoid arthritis and osteoarthritis both cause joint pain, stiffness, and limited range of motion, but the two diseases are distinct in their root cause and treatment.
Rheumatoid arthritis is an autoimmune condition where a persons own immune system attacks their joints, causing inflammation. Rheumatoid arthritis typically affects many joints simultaneously, especially in the hands, wrists, and feet, and is treated with medications to suppress the immune response.
Osteoarthritis is not an autoimmune disease, and although the exact causes are not known, multiple risk factors have been identified. In a healthy joint, cartilage provides cushioning and a smooth joint surface for motion. In an osteoarthritic joint, as cartilage is irreversibly destroyed and bone abnormalities develop, movement becomes painful and more difficult.
What Are Newer Rheumatoid Arthritis Medications And Side Effects
Newer “second-line” drugs for the treatment of rheumatoid arthritis include the following:
Each of these medicines can increase the risk for infections, and the development of any infections should be reported to the doctor when taking these newer second-line drugs.
While biologic drugs are often combined with DMARDs in the treatment of RA, they are generally not used with other biologics due to the risk of serious infections. Similarly, JAK inhibitor medication is not used with traditional biologic medicines.
Also Check: Is Spicy Food Good For Arthritis
What Is A Rheumatologist
Rheumatologists are expert physicians who specialize in diagnosing and treating inflammatory arthritis and autoimmune diseases where joints can be involved. They also care for people with other diseases of the connective tissue and those with osteoporosis. As needed, the rheumatologist coordinates the care his or her patients receive from surgeons and other specialists, as well as from other health care professionals.
In many, but not all cases, people become aware that they have inflammatory arthritis when they develop symptoms of inflammation in one or more joints. On a simple level, joints are where two bones are attached. A joint can be fibrous and a simple connection without movement, such as joints in the pelvis. However, most joints are “ball and socket joints”, which are covered with a smooth layer of specialized tissue called cartilage – allowing for a gliding motion examples are the knees, elbows, shoulders, hips or elbows. Other structures that attach the bones to each other and to muscles include the tendons, tissue that attaches muscles to bones and the ligaments, tissues that attach bone to bone. These can also be targets of inflammation in inflammatory arthritis. Furthermore, the joints are held together by a capsule, a kind of protective container that is lined with a membrane called the synovium. In inflammatory arthritis inflammation of the synovium is what usually causes pain, stiffness and swelling. This is called “synovitis”.
Exploring The Connection Between Stress And Autoimmune Disease
In this new study, researchers analyzed more than 100,000 people diagnosed with stress-related disorders and compared their tendency to develop autoimmune disease at least one year later with 126,000 of their siblings, and another million people who did not have stress-related disorders.
The study found that individuals diagnosed with a stress-related disorder
- were more likely to be diagnosed with an autoimmune disease
- were more likely to develop multiple autoimmune diseases
- had a higher rate of autoimmune disease if younger.
*Patient-years is an expression that combines how many and for how long people are assessed in a study. If the frequency of a condition is 9 per 1,000 patient-years, that means 9 people would develop the disease among ,1000 patients monitored for 1 year, or among 500 patients monitored for 2 years, and so on).
A particularly important observation was that, for those with PTSD who were being treated with an SSRI , the increased rate of autoimmune disease was less dramatic. While these observations are intriguing, they dont tell us why or how a stress-related disorder might provoke or cause autoimmune disease.
Don’t Miss: Is Marijuana Good For Arthritis Pain
Prevalence And Types Of Autoimmune Diseases
There are more than 80 types of autoimmune diseases. Symptoms depend on which part of the body is affected. There are autoimmune disorders that target specific types of tissue . Other autoimmune diseases may target a specific organ. Any organ can be involved. Characteristics that are typically associated with the autoimmune disease include inflammation, pain, muscle aches, fatigue, and a low-grade fever. Inflammation is usually the first sign of an autoimmune disease.
Autoimmune diseases affect more than 23.5 million Americans, according to the U.S. Department of Health and Human Services. While some autoimmune diseases are rare, a number of the conditions are common. Autoimmune diseases can affect anyone but it is believed that some people have a genetic predisposition for developing an autoimmune disease under certain circumstances . People at greater risk for developing an autoimmune disease include:
- Women of childbearing age
- People who have a family history of autoimmune disease
- People who have certain environmental exposures that could act as the trigger
- People of a particular race or ethnicity
Many types of arthritis are considered autoimmune diseases, including:
- Ankylosing spondylitis
- Vasculitis
Chronic fatigue syndrome and fibromyalgia are not considered autoimmune diseases. This has been a source of confusion since some symptoms of chronic fatigue and fibromyalgia overlap with several autoimmune diseases.
Rebecca Macdonald Centre For Arthritis And Autoimmune Disease
The Rebecca MacDonald Centre for Arthritis and Autoimmune Disease at Mount Sinai Hospital is a one-of-a-kind outpatient facility specializing in the research and treatment of rheumatoid arthritis and associated autoimmune diseases. Patients will receive “personalized” care developed on-site by world leaders involved in multi-disciplinary research.
Services include initial diagnosis, tailored therapeutics, current genetic information and testing, and opportunities for research participation. We are affiliated with the University of Toronto and resident education is incorporated in our service delivery.
New patient referrals can be faxed from your specialist or family physician to 416-586-8766 or by email at .
The Rebecca MacDonald Centre for Arthritis and Autoimmune DiseaseMount Sinai Hospital
Also Check: Is Papaya Good For Arthritis
What Can I Do To Prevent Osteoarthritis
Maintaining a healthy lifestyle may help prevent osteoarthritis. Eating nutritious foods, maintaining a healthy weight throughout your life, and exercising regularly to strengthen muscles that protect the joints are three very important methods that may reduce your risk of developing osteoarthritis.
How Autoimmune Diseases Like Arthritis Can Affect Your Sex Life
Certain rheumatoid diseases – and their treatments- can lead to symptoms of sexual dysfunction. But there are options available.
with Elaine Furst, BSN
If you are seeing a rheumatologist for your autoimmune disease, its unlikely that he or she is asking you about your sex lifebut perhaps they should be. Only 37% of specialists talk to their patients about sexual activity compared to 63% of OB/GYNs, according to Elaine Furst, BSN, a nurse educator who serves as the outreach director of the Scleroderma Foundation in Los Angeles. She recently spoke to a group of clinicians in Chicago as part of the 2018 meeting of the American College of Rheumatology/Association of Reproductive Health Professionals, and has lectured at colleges across the country.
Doctors tend to give many reasons given for not discussing the subject with their patients, she shared, ranging from discomfort or lack of awareness to feeling that such conversations belong under the purview of other physicians. However, not addressing the subject does a disservice to those individuals who dont quite understand the connection between their rheumatic condition and possible sexual dysfunction. Difficulties may include, for example, a lack of desire, inability to orgasm, or pain during penetration or intercourse.
Some rheumatic conditions can lead to symptoms of sexual dysfunction.
You May Like: What Tests Are Done For Rheumatoid Arthritis
What Are The Symptoms Of Inflammatory Arthritis
The most common symptoms of inflammatory arthritis are:
- Joint pain and stiffness after periods of rest or inactivity, particularly in the morning
- Swelling, redness and/or a feeling of warmth in the affected joints
- Inflammation of other areas in the body, such as the skin or internal organs like the lungs and heart
People with inflammatory arthritis generally experience alternating periods of “flares” of highly intense symptoms with periods of inactivity.