Early Warning Signs You Have Psoriatic Arthritis
Autoimmune disorders can be difficult to diagnose, especially in the earlier stages, and psoriatic arthritis is no different. Because there is no definitive blood test that can identify this form of arthritis and the similarities in symptoms it shares with rheumatoid arthritis, diagnosing can be tricky.
Research suggests that more than half of people with psoriatic arthritis must wait at least two years for a diagnosis, so it can be helpful to recognize the symptoms early on. Keep reading to learn about the early signs of psoriatic arthritis and how to find someone who can help provide you some relief.
Six Symptoms You Shouldnt Ignore
The symptoms of psoriatic arthritis can vary in severity, from person to person and can even come and go . Here are six symptoms you should watch out for.
1. Its hard to move in the morning
Psoriatic arthritis can make getting up in the morning a challenge, especially after you havent moved around for a while. It can cause stiffness and pain in one or more joints, from your toes to your fingers. It can even cause pain and swelling in the tendons and surrounding structures that connect to your bone, a condition called enthesitis.
2. Your fingers look like warm sausages
About 30 to 50 percent of patients with psoriatic arthritis will experience the symptoms of dactylitis, or extreme swelling in their fingers and toes, Dr. Aquino said. This is when the entire fingers and toes swell to resemble sausages.
You may notice your swollen joints feel warm to the touch because inflammation and swelling cause heat.
3. You have lower back pain
When you think of psoriatic arthritis, you typically think about skin symptoms, but many people experience lower back pain as well. About 20 percent of those with psoriatic arthritis will develop a subtype called spinal involvement or psoriatic spondylitis, which may result in pain and stiffness in the back and hips, Dr. Aquino said.
4. Your nails have grooves and ridges
5. You experience eye problems
6. Youre always tired
Utility Of Imaging Techniques In Diagnosing Clinical Forms Of Psa
Enthesitis
The entheses consist of unique fibrocartilaginous structures that connect ligaments, tendons, and capsules to the bone. The entheseal organ allows the subtle transfer of mechanical forces from the muscle through the tendon and ligaments to the bone while also having a stabilizing role for the joint.36,37 Enthesitis is defined by pain and tenderness at the site of attachment of the tendon, ligament, or capsule to the bone and is recognized as a feature of all spondylarthritis .24,37,38 The most commonly affected sites in PsA are the Achilles tendon, the plantar fascia, and the common extensor tendon insertion in the lateral epicondyle of the elbow. Clinical assessment of the enthesitis is based on applying a pressure of 4 kg/cm2 which can be difficult to reproduce between examiners,37 meaning that the burden of enthesitis could be higher if imaging techniques were employed to detect it. Enthesitis has been identified as an outcome domain by the ASAS and GRAPPA experts for determining disease activity and response to treatment for both spondyloarthritis and psoriatic arthritis.10, On CR, enthesitis appears late in the course of the disease, as bone cortex irregularities , new bone formation at the insertion of the tendon, ligament, or capsule , and intra- or peri-tendinous calcifications.37
Dactylitis
Onicopathy
Arthritis
Axial PsA
|
Table 1 Imaging Techniques in Psoriatic Arthritis |
You May Like: Best Treatment For Arthritis Pain In Hands
Understanding Remission And Minimal Disease Activity
Psoriatic arthritis disease progression is not inevitable. When your PsA is treated with medications that reduce immune system overactivity, you can reduce your disease activity to a point that its no longer causing significant symptoms or increasing the risk of long-term health issues.
In general, going into remission means that you are no longer showing signs of active disease. Decades ago, remission wasnt conceivable for most people with psoriatic arthritis, but thanks to a proliferation in medication treatment options, getting to remission is a possibility for PsA patients today.
However, going into remission does not mean that you will stay there indefinitely. It is common for PsA symptoms to wax and wane. Even if youve been in remission for a long time and your pain starts coming back and you start flaring more, you may need to change your medication for better control, says Dr. Haberman.
You may also hear the phrase minimal disease activity in conjunction with psoriatic arthritis and remission.
Doctors dont have a clear definition of what it means to be in remission in PsA, but they have defined something called minimal disease activity as a treatment target. This is what your doctor may use to determine whether your PsA disease activity is low enough that you have few symptoms and a low risk of long-term damage.
People are considered to be in minimal disease activity when their scores on five out of these seven criteria are low enough.
Access To Care Challenges
Serious racial disparities exist when it comes to access to care, both when it comes to psoriatic arthritis and in general.
Studies show differences in psoriatic arthritis based on skin color and race. For example, Black people tend to have more severe:
- Skin involvement
Despite that, they’re less likely than White people to be put on immunosuppressive drugs.
Furthermore, according to 2021 research, psoriatic arthritis is diagnosed less often in:
- Black people
- People of Asian descent
- Latinx people
People in these groups who have psoriatic arthritis often have a higher disease burden and lower quality of life because of disparities in care.
Some studies show implicit, often unconscious biases against people of color throughout the healthcare community. This is believed to have negative effects when it comes to treatment decisions and outcomes.
Some facilities have looked at disparities in their own patients. They found that poverty plays a role. But when comparing Black and White people of the same socioeconomic status, it became clear that outcomes remained worse for Black people.
Researchers call for more investigation into the impacts and disparities caused by bias in the medical profession and better education aimed at eliminating these issues.
Recommended Reading: Is Peanut Bad For Arthritis
Psoriatic Arthritis Blood Test: Erythrocyte Sedimentation Rate
Erythrocyte sedimentation rate, or ESR or sed rate, is a blood test that measures inflammation in the body, which helps determine a psoriatic arthritis diagnosis, explains Elaine Husni, MD, MPH, vice chair of rheumatology and director of the Arthritis and Musculoskeletal Center at the Cleveland Clinic.
The test measures how many milliliters of red blood cells settle per hour in a vial of blood. When swelling and inflammation are present, the bloods proteins clump together and become heavier as a result, they will fall and settle faster at the bottom of the test tube, according to Johns Hopkins Medicine.
As with many blood tests, labs each have their own, slightly different reading of what ESR numbers mean, which they interpret based on past results, explains Cadet. Age is also a factor. ESR can be elevated slightly in elderly patients and still be normal for that person, she says.
Frequency of Testing In addition to diagnosis, Testing may be done several times a year to determine if theres ongoing inflammation, says Cadet.
Editor’s Picks
Early Stages Of Psoriatic Arthritis
Recognizing the signs of psoriatic arthritis can be tricky since symptoms differ from patient to patient. For example, one person can experience psoriasis skin involvement and peripheral arthritis, another may experience axial disease , and someone else could have a combination of all three.
Whats more, especially during early disease, you may confuse your symptoms with other conditions. People can mistake enthesitis, inflammation of the entheses for tennis elbow or dactylitis for an infection, explains Dr. Mikulik.
If you have psoriasis and are having pain in your tendon and musculature and you think maybe Ive been too active lately, that may be the first sign of PsA, says Dr. Haberman. Doctors commonly hear people chalk up their symptoms to overuse, such as getting more exercise than usual or doing work around the house.
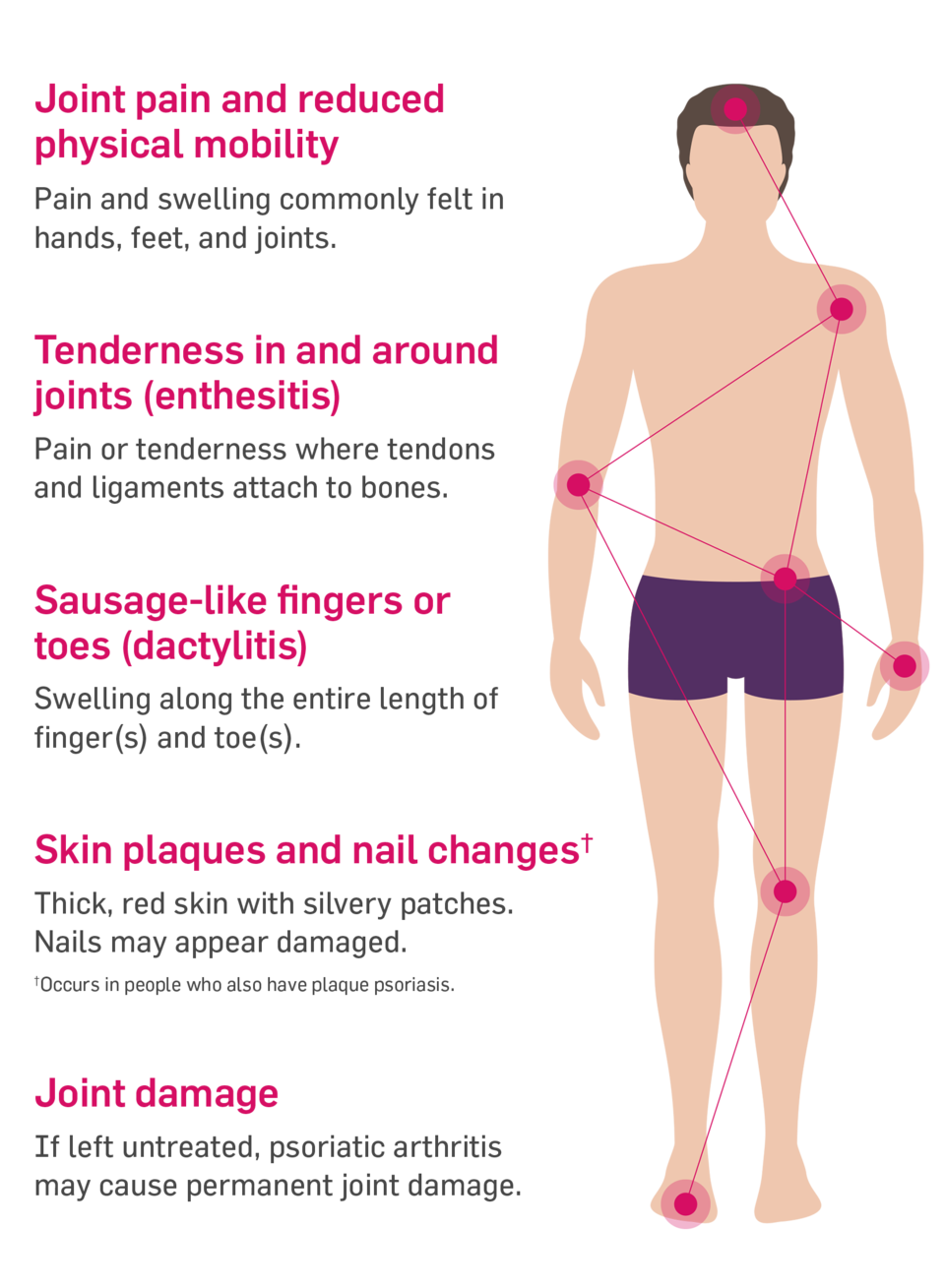
If you experience any of the following signs of early psoriatic arthritis its important to see your doctor as soon as possible:
- Back pain
- Changes in your fingernails or toenails, including holes, pitting, discoloration, or softness
- Eye inflammation
- Sausage-like swelling of an entire finger or toe
- Scalp psoriasis
- Skin rash
- Tendon or ligament pain at the Achilles tendon, bottom of the foot , or elbow
Also Check: How To Relieve Arthritis Pain In Fingers
What Are The Treatment Options For Psoriatic Arthritis
The aim of treatment for psoriatic arthritis is to control the disease and relieve symptoms. Treatment may include any combination of the following:
- Splinting.
- Surgery.
Choice of medications depends on disease severity, number of joints involved, and associated skin symptoms. During the early stages of the disease, mild inflammation may respond to nonsteroidal anti-inflammatory drugs . Cortisone injections may be used to treat ongoing inflammation in a single joint. Oral steroids, if used to treat a psoriatic arthritis flare, can temporarily worsen psoriasis. Long-term use of oral steroids should be avoided when possible due to the negative effects on the body over time.
DMARDs are used when NSAIDs fail to work and for patients with persistent and/or erosive disease. DMARDs that are effective in treating psoriatic arthritis include: methotrexate, sulfasalazine, and cyclosporine.
Biologic agents are an important consideration when disease control is not being achieved with NSAIDS or DMARDs. Biologics have been utilized for the treatment of psoriatic arthritis since 2005 and are highly effective at slowing and preventing progression of joint damage. Your healthcare provider will complete additional laboratory tests and review safety considerations before initiating a medication regimen. Gaining good control of psoriatic arthritis and psoriasis is important to avoid increased systemic risks, particularly heart disease.
Exercise
Heat and cold therapy
Splinting
Surgery
Caspar Criteria For Diagnosis
Diagnosing psoriatic arthritis relies on markers in an established system called the Classification Criteria for Psoriatic Arthritis .
The criteria are each assigned a point value. Each one has a value of 1 point except for current psoriasis, which has a value of 2 points.
The criteria are as follows:
- current psoriasis outbreak
- personal or family history of psoriasis
- swollen fingers or toes, known as dactylitis
- nail problems, like separation from the nail bed
- bone growths near a joint that are visible on an X-ray
- absence of rheumatoid factor
A person must have at least 3 points based on the CASPAR criteria to be diagnosed with psoriatic arthritis.
Recommended Reading: Can Arthritis Cause Itching
You Can Have Psoriasis And A Different Kind Of Arthritis That Is Not Psa
People with psoriasis can develop different types of arthritis including rheumatoid arthritis, gout, osteoarthritis, and reactive arthritis so diagnosing PsA involves ruling out those other conditions.
Its often difficult to say in a first visit whether a patient definitely has psoriatic arthritis or another type of arthritis that just co-exists with psoriasis, says Dr. Kumar. PsA can take a long time to diagnose because a patient can delay seeing the doctor, then confirming PsA can require multiple labs and imaging tests.
The good news is that the diagnosis process for psoriatic arthritis is improving. Whereas PsA wasnt even recognized as a distinct condition decades ago , doctors are now better equipped with improved lab tests and imaging studies that help identify this disease so more patients can find relief.
What Is A Rheumatologist
A rheumatologist is a specialist in the nonsurgical treatment of autoimmune, inflammatory, or other musculoskeletal conditions commonly referred to as rheumatic diseases.
Your rheumatologist is the best person to:
- Confirm your diagnosis after reviewing all test results and your medical history
- Direct you toward the best treatment depending on the severity of your psoriatic arthritis and whether the symptoms are mostly external , internal , or a combination of both.
Read Also: Vicks Vaporub For Arthritis
Psoriatic Arthritis Imaging Test: X
X-rays, which use low-dose radiation to produce images of the inside of the body, can help your doctor make a psoriatic arthritis diagnosis and monitor progression of the autoimmune condition.
X-rays allow the doctor to see changes to the bone, says Elyse Rubenstein, MD, a rheumatologist in Santa Monica, California. In people with psoriatic arthritis, X-rays may show bone erosion, new bone formation, bone fusion, or a phenomenon called pencil in a cup, in which the ends of the bone have been eroded to a pencillike point. Any of these changes indicate that the disease is getting worse, Dr. Rubenstein says.
Frequency of Testing A doctor may take an initial X-ray to help diagnose psoriatic arthritis and rule out other forms of arthritis, such as rheumatoid arthritis, which have different patterns of joint involvement, says Rubenstein.
After that, how often you have X-rays depends on your physician and the state of your disease. Some doctors take X-rays just once a year for routine monitoring, while others may take them only when a patients condition changes.
Symptoms Of Psoriatic Arthritis
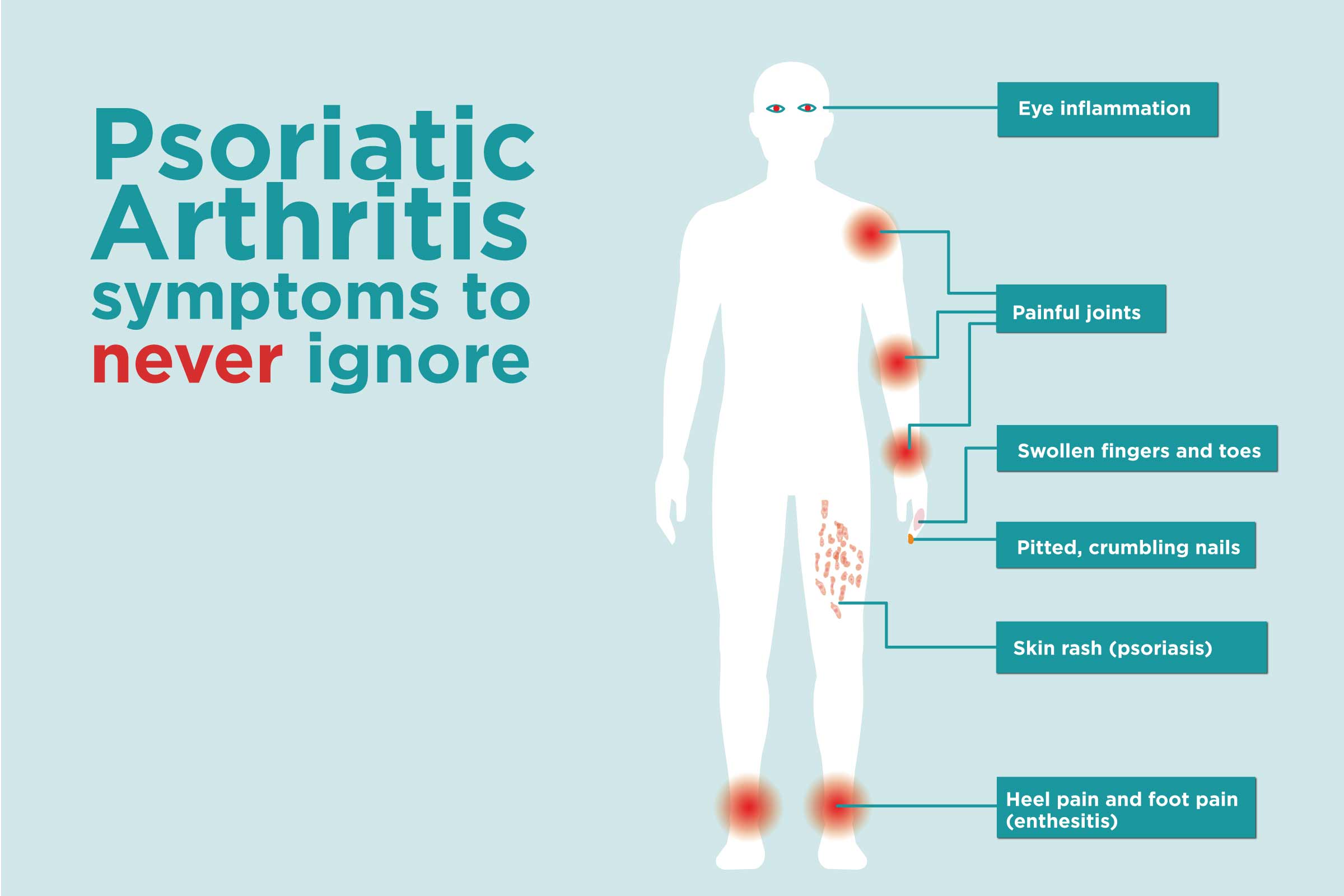
The severity of the condition can vary considerably from person to person. Some people may have severe problems affecting many joints, whereas others may only notice mild symptoms in 1 or 2 joints.
There may be times when your symptoms improve and periods when they get worse .
Relapses can be very difficult to predict, but can often be managed with medicine when they do occur.
Recommended Reading: Rheumatoid Arthritis And Itching
Psoriatic Arthritis Blood Test: Hla
HLA-B27 is a blood test that looks for a genetic marker for psoriatic arthritis a protein called human leukocyte antigen B27 , which is located on the surface of white blood cells. About 20 percent of people with psoriatic arthritis are positive for HBL-B27, according to CreakyJoints.
HLA-B27 is associated with a larger group of autoimmune diseases, called spondyloarthropathies, which includes psoriatic arthritis, Cadet says. These conditions can cause inflammation in the enthesis anywhere in the body but mainly in the spine.
If untreated over a long period, this inflammation may cause the destruction of cartilage, muscle spasms, and a decrease in bone mineral density that may lead to osteopenia or osteoporosis.
Frequency of Testing The HLA-B27 test is usually performed only at an initial visit to help establish a diagnosis, says Cadet.
Psoriatic Arthritis Blood Test: C
C-reactive protein is a protein in the blood that indicates inflammation. If a blood test shows high CRP levels, you might have psoriatic arthritis, explains Dr. Husni.
Your doctor may use the test if your ESR is normal, since CRP is more accurate at detecting inflammation in some people, adds Cadet.
Again, different labs may have slightly different interpretations of readings.
Frequency of Testing CRP analysis may be done for diagnosis and then several times a year to assess whether inflammation has responded to treatment, notes Cadet.
Also Check: Arthritis In Lower Right Side Of Back
How Do You Diagnose Psoriatic Arthritis
Psoriatic arthritis can be a difficult condition to diagnose as there is no test which will conclusively give a diagnosis. Some patients can have symptoms for many years before they are diagnosed. Diagnosis often relies on a constellation of features:
- Presence of skin psoriasis
- Presence of swollen joints
- History of inflammatory back pain
- Presence of pain and tenderness at areas where tendons, ligaments and joint capsules attach to bone
- Some patients may have raised inflammatory blood tests but many do not.
- Blood tests are also ordered to exclude other conditions that can cause inflammatory arthritis. Psoriatic arthritis is a seronegative condition meaning that autoimmune tests are negative. The presence of a gene called HLA B27 is more common in patients with psoriatic arthritis, however many people with the gene never develop arthritis.
If your symptoms sound suggestive then your doctor may order further tests to determine if inflammation is present. This may include MRI scans or ultrasound. X-rays may be ordered to determine if there has been any permanent bone and joint deformities.
Get the help you deserve – talk to our friendly team today! 1300 252 698
Imaging Tests For Psoriatic Arthritis
Imaging tests can help your doctor closely examine your bones and joints. Some of the imaging tests your doctor may use include:
- X rays. X-rays arent always useful in diagnosing early stage psoriatic arthritis. As the disease progresses, your doctor may use imaging tests to see changes in the joints that are characteristic of this type of arthritis.
- MRI scans. An MRI alone cant diagnose psoriatic arthritis, but it may help detect problems with your tendons and ligaments, or sacroiliac joints.
- CT scans. These are used primarily to examine joints that are deep in the body and not easily seen on x-rays, such as in the spine and pelvis.
- Ultrasounds. These tests can help determine the progression of joint involvement and pinpoint the location.
You May Like: Stop Arthritis In Fingers
Psoriatic Arthritis Tests And Diagnosis
The diagnosis of psoriatic arthritis is largely based on your medical history and a physical exam, and laboratory tests may be used to rule out other conditions. During an appointment, your doctor will likely ask you questions about specific skin and joint symptoms and your overall well-being.
Psoriatic arthritis can damage joints over time if not controlled, so the earlier you receive a diagnosis and appropriate treatment, the better. If youre currently seeing a dermatologist for psoriasis, and you are experiencing joint pain, tell your doctor. They may refer you to a rheumatologist. If any of these symptoms seem familiar, talk to your doctor.
About 1 in 3 people with psoriasis may develop PsA.
What to expect when getting diagnosed with PsA
Medical history:
At your doctor appointment, be prepared to answer questions regarding your medical history as accurately as possible. Some of the questions your doctor may ask you will likely include the following:
- Which joints hurt?
- Joints at the ends of fingers and toes
Physical exam:
During a physical exam, your doctor will look for several symptoms that are commonly associated with psoriatic arthritis:
- Tender, painful, or swollen joints
- Pain in your feet, ankles, and lower back
- An indication of psoriasis
- Dactylitis
- Enthesitis
Laboratory tests and imaging procedures:
Your doctor may order tests and procedures to help rule out other diseases or confirm your diagnosis. Some of these tests may include: