What Are The Complications Of Ra
Rheumatoid arthritis has many physical and social consequences and can lower quality of life. It can cause pain, disability, and premature death.
- Premature heart disease. People with RA are also at a higher risk for developing other chronic diseases such as heart disease and diabetes. To prevent people with RA from developing heart disease, treatment of RA also focuses on reducing heart disease risk factors. For example, doctors will advise patients with RA to stop smoking and lose weight.
- Obesity. People with RA who are obese have an increased risk of developing heart disease risk factors such as high blood pressure and high cholesterol. Being obese also increases risk of developing chronic conditions such as heart disease and diabetes. Finally, people with RA who are obese experience fewer benefits from their medical treatment compared with those with RA who are not obese.
- Employment. RA can make work difficult. Adults with RA are less likely to be employed than those who do not have RA. As the disease gets worse, many people with RA find they cannot do as much as they used to. Work loss among people with RA is highest among people whose jobs are physically demanding. Work loss is lower among those in jobs with few physical demands, or in jobs where they have influence over the job pace and activities.
Shortness Of Breath Or Coughing
The lungs are often affected in people diagnosed with rheumatoid arthritis. Lung conditions may cause coughing, shortness of breath, and chest pain. Rarely, these conditions become life-threatening.
- Interstitial lung disease is an umbrella term used to describe many disorders that cause scarring of the walls of the lungs and certain nearby structures. In people with RA, scarring is typically caused by chronic inflammation. The initial symptoms of interstitial lung disease typically include shortness of breath and a cough.
- Pleural effusion, also called pulmonary effusion or water on the lungs, occurs when fluid collects in the chest cavity outside the lungs. Pleural effusion can cause sharp chest pain, coughing, and shortness of breath. It may be noticeably more difficult to breathe when lying down.
nodules in the lungs typically have no symptoms but may increase the risk for potentially life-threatening conditions, such as a collapsed lung.5,6Rheumatoid nodules in the lungs are rare and account for less than 1% of all rheumatoid nodules.
The chances of developing lung conditions related to RA are increased by smoking.
Antibody To Neutrophil Cytoplasmic Antigens
I will mention one other laboratory test in this context. That is the ANCA test. ANCA stands for antibody to neutrophil cytoplasmic antigens. This test is often positive in forms of blood vessel inflammation such as vasculitis.
One of the strongest disease associations of the ANCA test is a disease called Wegeners granulomatosis. This is a disease that can attack blood vessels in different parts of the body, including the skin. Recognizing the characteristic patterns of skin changes can be a clue to the diagnosis of this disease and getting patients on proper treatment for the internal complications that can be very severe .
However, like the ANA test, one must be careful in interpreting the ANCA test results. The ANCA test can be positive in other conditions besides vasculitic illnesses, such as Wegeners granulomatosis.
The treatment really has to be individualized to the specific disease and to the specific conditions related to a given case. Some drugs might be riskier in women compared to men, for example.
You May Like: Can You Stop Arthritis
What Causes Hives And What Can Be Done About Them
Hives are those awful, itchy red raised welts on your skin.
There are two types of hives, short-term and chronic hives. If you have had hives for less than 6 weeks, you probably have short-term hives or acute urticaria. Common causes include viral infections or an allergic reaction to food or a drug.
Hives that come on all of a sudden and are associated with difficulty breathing, swelling of the lips, tongue or throat, lightheadedness, vomiting, racing heart, chest pain or a feeling of doom could be a sign of anaphylaxis. If you are having any of these associated symptoms with your hives, seek medical attention immediately. Anaphylaxis is a serious, life-threatening allergic reaction, that requires immediate medical attention in the emergency room.
As long as you dont have any of the other symptoms of anaphylaxis, you can probably wait until you can get a doctors appointment.
Most cases of hives are treated with antihistamines like Benadryl, Allegra, Zyrtec, Claritin and Xyzal. If hives do not clear up with antihistamines, stronger medications like corticosteroids, immune suppressants or Xolair shots might be needed to clear up those itchy spots.
What Is The Treatment For Rheumatoid Arthritis Rashes
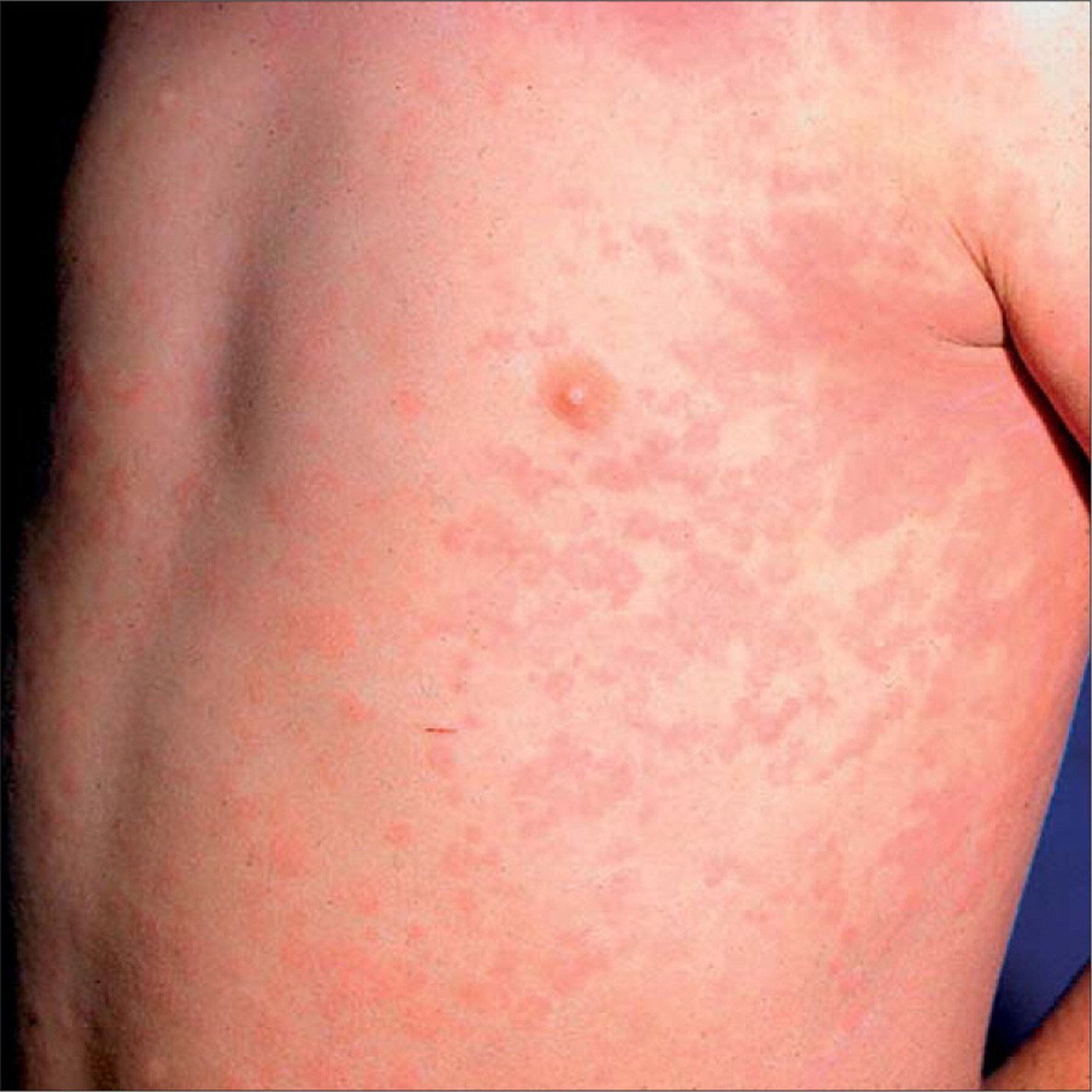
The treatment for a rheumatoid arthritis-related rash depends on its cause and severity. A treatment that works well for one type of rash may be useless for another. Treatment usually focuses on managing pain and discomfort, and preventing an infection. Its also important that treatments target the underlying condition, since rashes may be a sign that your rheumatoid arthritis isnt well-controlled.
Common over-the-counter medications that may reduce the pain of a rash include acetaminophen and nonsteroidal anti-inflammatory drugs . There are several types of NSAIDs, such as ibuprofen , naproxen sodium , and aspirin .
If your pain is severe, your doctor may also consider prescription NSAIDs. Opioid pain drugs are usually only prescribed for very severe pain since they have a high risk of addiction.
Your physician may also prescribe corticosteroids to reduce the inflammation of your rash, which may in turn reduce painful symptoms. However, these drugs arent recommended for long-term use. If your doctor is concerned that your rash could get infected, theyre likely to prescribe either a topical or oral antibiotic, or both.
When it comes to treating the underlying condition, there are several different medication options available:
Treatments for interstitial granulomatous dermatitis include topical steroids and antibiotics. Doctors may also prescribe etanercept , a medication thats also used to treat psoriasis and psoriatic arthritis.
Read Also: What Does Arthritis Feel Like In Your Back
What Causes Rheumatoid Arthritis Rashes
People with RA are prone to episodes known as flares. A flare indicates that there is increased disease activity in a persons body. A person may have more symptoms associated with the condition, including fever, joint swelling, and fatigue. During a flare-up, a rheumatoid arthritis rash is more likely to occur.
When vasculitis causes a rash, this is most likely due to inflammation of small arteries and veins. This is due to high levels of rheumatoid factor in the blood.
RA can cause complications beyond a rash. Vasculitis can affect blood flow in arteries and veins. The results of severe episodes of vasculitis can be:
- numbness and tingling in the nerves, including loss of sensation in the hands and feet
- affected blood flow to the extremities that can cause gangrene in the fingers or toes
- systemic vasculitis that affects blood flow to the brain or heart that can result in heart attack or stroke
The occurrence of RV is rare, and the complications above are even rarer. However, its possible that a rash could be a precursor to something more severe. See your doctor if you experience any signs or symptoms of RV.
Can Rheumatoid Arthritis Cause Itchy Skin
RA can causeskinRARAcanskinitchyRA
. Hereof, can Rheumatoid arthritis cause itching?
Causes of Rheumatoid Arthritis Itching. Although many RA patients report severe itching, the cause might actually be another related issue, such as eczema, hives, or medication side effects. But you can have RA and chronic hives, or RA and eczema, at the same time.
what autoimmune disease causes itchy skin? However, dermatomyositis skin disease generally is harder to treat than is lupus skin disease. In addition, dermatomyositis skin disease is often more troublesome for the patient by producing symptoms such as itching .
Additionally, can rheumatoid arthritis affect your skin?
Rheumatoid patients can develop skin disorders. UIHC notes that the same kind of immune system problems that cause joint inflammation, swelling, and pain can also affect your skin. When this happens, RA patients may develop lesions or rashes on the skin, reflecting immunological dysfunctions.
What does it mean when your joints itch?
Psoriasis. Psoriasis is a skin condition that causes skin cells to quickly build up, resulting in patches of flaky, itchy, scaly skin. Psoriasis can affect different areas of a person’s body, primarily the joints, but also areas such as fingers and nails.
You May Like: Does Arthritis Cause Swelling
Exercise And Therapy Treatments
Once your doctor confirms a diagnosis, they can set your child up with a treatment plan to reduce any pain, swelling or skin rashes. Exercising is the best way to keep juvenile arthritis under control. Walking and biking are low-impact activities your child can enjoy. Swimming is one of the preferred exercise methods since waters buoyancy puts less pressure on joints.
Physical activity may seem counterproductive if your childs joints are swollen or painful, but staying mobile will help keep joints loose and flexible to maintain a range of motion. Have your child take breaks or rest days if certain body parts become inflamed.
A physical therapist can work with your child on ways to strengthen joints and muscles and maintain flexibility. In more moderate cases, your child may find relief from massage therapy or acupuncture.
Treatment Of Skin Issues
Some skin issues may require treatments, while others might not. Treatment will depend on the cause and severity. The goal of treatment is to reduce pain, discomfort, and inflammation, and also to prevent infection.
It is very important to treat the underlying cause of skin problems, as these conditions are a sign that rheumatoid arthritis symptoms are not well-managed.
Common over-the-counter medications, including acetaminophen , can help with pain, while NSAIDs, including ibuprofen, can help control and reduce inflammation. Severe pain may need prescription NSAIDs. Corticosteroids can also help reduce skin inflammation, but these medications cannot be used in the long-term. If there is a possibility of infection, a topical or oral antibiotic may be prescribed. Hives are usually treated with antihistamines.
If medications are the cause of RA skin symptoms, medication replacement or reduction may help prevent or reduce skin symptoms.
Also Check: What Relieves Arthritis Pain In The Hands
Rheumatoid Arthritis Itching Attacks: Causes And Relief Tips
People with rheumatoid arthritis sometimes experience itchy skin. This may be due to the condition itself, the medications they are taking, or another condition, such as eczema. Switching medications with a doctors approval may be an option. Home remedies can also provide relief.
RA is an autoimmune condition that primarily causes inflammation and pain in the joints.
RA can also sometimes cause skin problems, including itchiness. This may be related to RA itself or to other factors, including medications.
Learn about the causes of itching in people with RA, along with some tips for prevention and relief.
People with RA often experience symptoms including:
- joint pain, swelling, and stiffness that:
- lasts for at least 6 weeks
- usually affects both sides of the body
- frequently starts in the hands and feet
RA can also affect other areas of the body, including the skin.
For example, some people with RA report itchy skin. Rashes are uncommon in RA, but a person does not need to have a rash to have itchy skin.
Surprising Triggers Of Chronic Hives
You already knew that heat can trigger hives, but did you know that tooth decay and stress can, too?
Thinkstock
For most healthy people, an outbreak of hives is as worrisome and temporary as catching a cold. But for those who have chronic hives, or urticaria, the condition can seem relentless.
Chronic idiopathic hives are itchy red welts that persist for at least six weeks and have no known cause, says Miriam Anand, MD, an allergist with Allergy Associates and Asthma in Tempe, Arizona. The condition is marked by periods of exacerbation and remission, and for many who have it, the hives may persist for more than five years.
If you have chronic hives, its important to try to identify your triggers, if possible, and take steps to avoid them so you can lower the risk of an exacerbation. While you may already be aware of common triggers, such as allergies to pollen, pet dander, and shellfish, here are some lesser-known triggers of chronic hives:
1. Tooth decay and other infections
Heres an additional reason to brush, floss, and see your dentist regularly: In a study published in April 2013 in the journal Advances in Dermatology and Allergology, researchers found that tooth decay and several other infections can play a significant role in the development of chronic hives. Bacterial infections and viral infections were also found to be triggers of chronic hives.
2. Working out
3. Stress
4. Artificial colors and preservatives
You May Like: What Does Ra Feel Like
Skin Conditions Linked To Lupus
Lupus is known to cause a number of skin problems, including hives, cutaneous vasculitis , photosensitivity, alopecia, and purpura . About 10 percent of all people with lupus will experience hives. Most individual hives will fade and disappear within hours, while new welts flare. Individual hives lasting more than 24 hours may be due to inflammation in the blood vessels that could be due to lupus.
Bacterial Infections In The Body
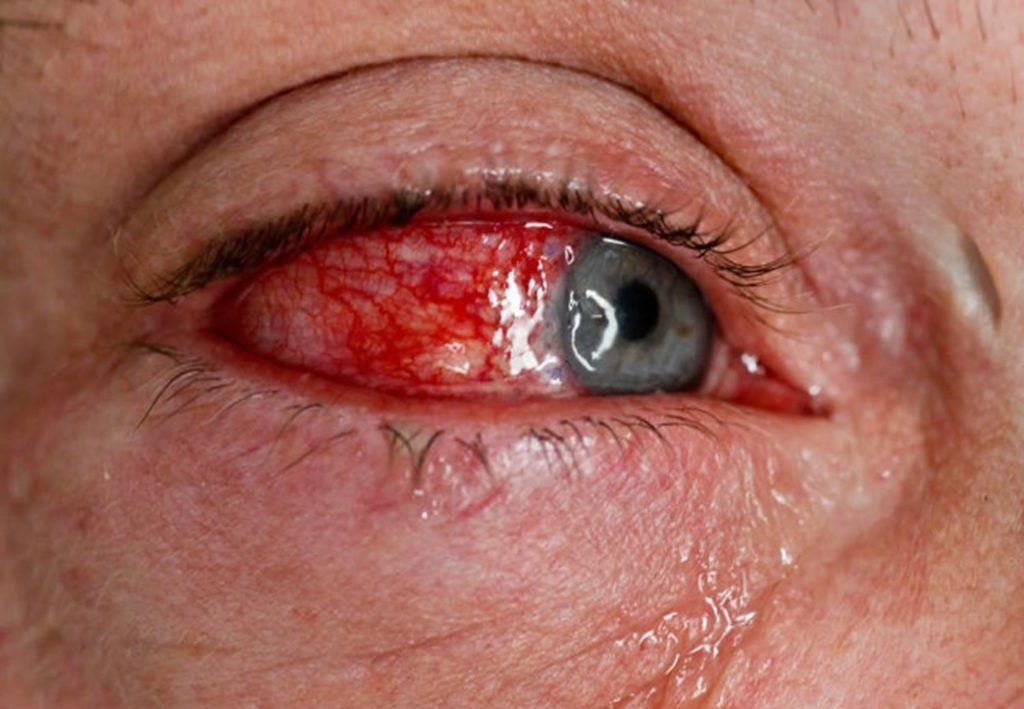
Bacterial infections in the body can also produce hives and hive-like symptoms in many individuals. Two of the most common bacterial infections that can present hives are strep throat as urinary tract infections . Influenza and the common cold are both well-known culprits of producing hives, or the appearance of hives, and these ailments are usually cured with bed-rest and hydration. Also, glandular fever can also cause the skin to break out, causing blisters or bumps in one, or several, areas. Hepatitis B – an infectious disease – will also cause these symptoms on the skin. Even tooth decay and dental health can play a role in these signs developing on the body. Many infectious diseases can cause the body to exhibit these types of symptoms of distress.
Don’t Miss: Rheumatoid Factor 7.0
What Causes Dermatomyositis
The exact cause is not known, but possible causes include:
-
Abnormal genes you are born with
-
Cancer, especially in older people
-
Autoimmune disease, a type of illness that causes the bodys immune system to attack its own tissues
-
An infection, medication, or another exposure in your environment that triggers the disease
Skin Conditions And Rashes
RA can even affect your skin. Up to 25 percent of people with RA develop rheumatoid nodules lumps of tissue under the skin and many also experience itchy hands and feet and skin rashes. Painful rashes, skin ulcers, or mouth sores may be symptoms of a more serious condition related to RA vasculitis, or inflammation of blood vessels. In rare cases, these inflamed blood vessels can actually stop blood flow, notes the Cleveland Clinic. See your doctor if you have RA and show signs of possible vasculitis, which can be detected through a biopsy.
Also Check: Is Vicks Vaporub Good For Knee Pain
Chronic Autoimmune Illnesses Linked To Chronic Hives
by Health Writer
Chronic hives can be a formidable foe, especially when its not clear whats causing the itchy, red welts or wheals that can appear anywhere on the body and recur for six weeks or more. Sometimes a hidden illness may be an underlying cause. Studies have found a strong association between chronic hives and autoimmune diseases such as thyroid disease, rheumatoid arthritis, celiac disease, type 1 diabetes, Sjögren syndrome, and lupus.
How Long Do Ra Flares Last
The length of time an RA flare lasts can vary widely, from a few hours to several days or weeks. If a flare does not improve after 7 days, it may be a good idea to contact a physician. The doctor may suggest adjusting the persons medication.
Before a RA flare begins, a person may experience fatigue or feel that something is not quite right.
During a flare, symptoms tend to increase until they reach their peak. As the peak passes, the symptoms will lessen and may completely disappear.
The frequency and severity of flares can vary widely between individuals. With treatment, a person may spend months or years in remission, while others may experience flares more frequently.
RA flares can be predictable or unpredictable. A flare will occur when something triggers an increase in disease activity, which means that levels of inflammation go up.
Predictable flares usually occur in response to one or more triggers.
Some flares have no apparent trigger, and a person may be unable to identify why it started. This can make them harder to avoid.
In 2017, a involving 274 people with RA who attended a clinic in Turkey found the following appeared to worsen their symptoms:
- emotional or physical stress
Read Also: Autoimmune Leg Pain
Other Body Parts Ra Can Affect
- Bones. The chemicals that cause inflammation can also take a bite out of your bones. It often affects your hips and spine. Sometimes, itâs a byproduct of years of treating RA with steroids.
- Liver and kidneys. Itâs rare for RA to affect these organs. But the drugs that treat it can. Nonsteroidal anti-inflammatory drugs can be bad for both. Cyclosporine may cause kidney disease. Methotrexate can damage your liver.
- Immune system. The medications you take can slow it down. This makes you more likely to get infections.
- Mucous membranes. You might be more likely to get a condition called Sjogrenâs syndrome that dries out moist places in your body like your eyes, your mouth, and inside your nose.
- Muscles. When inflammation stops you from moving your joints, the attached muscles can get weak. Or you could get a condition called myositis that weakens them. The medications you take for RA can also be to blame.
- Nerves. RA causes symptoms that range from numbness and tingling to paralysis. It can result from joint damage that RA causes, the disease process itself, or medications that treat it.
- Blood vessels. RA can cause inflammation of your blood vessels. It can show up as spots on the skin or can cause ulcers in more severe cases.