Symptoms By Body Part
The most commonly affected areas during the onset of RA are the small joints in your hands and feet. This is where you may first feel stiffness and an ache.
Its also possible for RA inflammation to affect your knees and hips. Because the disease presents differently in different people, it can go on to affect almost any joint.
Your organs are another area that can be disrupted by RA inflammation:
- Your heart muscle can become damaged.
- Your lungs can become scarred.
- Blood vessel damage can lead to subsequent skin and nerve issues.
What Causes Rheumatoid Arthritis Rashes
People with RA are prone to episodes known as flares. A flare indicates that theres increased disease activity in a persons body.
During a flare, they may have more symptoms associated with the condition, including fever, joint swelling, and fatigue. An RA rash is more likely to occur during a flare.
RV is a complication of RA. Its caused by the immune system and high levels of rheumatoid factor in the blood interacting with blood vessels.
This triggers inflammation of small arteries and veins. It can be serious and, while rare, RV
RA can cause complications beyond a rash. Vasculitis can affect blood flow in arteries and veins. The results of severe episodes of vasculitis can be:
- numbness and tingling in the nerves, including loss of sensation in the hands and feet
- affected blood flow to the extremities that can cause gangrene in the fingers or toes
- systemic vasculitis that affects blood flow to the brain or heart that can result in a heart attack or stroke
The occurrence of RV is rare, and the complications above are even rarer. However, its possible that a rash could be a indicate that something more severe may occur. See a doctor if you experience any symptoms of RV.
Anticitrullinated Protein Antibody Test
An anti-CCP test, also known as ACPA, tests for an antibody associated with RA.
A research review from 2015 found that this test may identify people who are more likely to develop severe and irreversible damage due to RA.
If you test positive for anti-CCP antibodies, theres a good chance you have RA. A positive test also indicates that RA is likely to progress more rapidly.
People without RA almost never test positive for anti-CCP. However, people with RA may test negative for anti-CCP.
To confirm RA, your doctor will look at this test result in combination with other tests and clinical findings.
Read Also: What Dosage Of Turmeric Should I Take For Arthritis
Other Tests For Seropositive Rheumatoid Arthritis
Blood tests are not only used to detect RF and anti-CCP antibodies. Theyâre also used to reveal if you have:
- Anemia, or low red blood cell count, which occurs in up to half of people with RA
- A high erythrocyte sedimentation rate, also known as a sed or ESR rate, a crude measure of inflammation in your body
- High C-reactive protein levels, another marker of inflammation
Aside from blood tests, an X-ray can help your doctor determine the degree of destruction in your joints, but may only be useful when RA has progressed to a later phase.
What Are The Four Stages Of Rheumatoid Arthritis
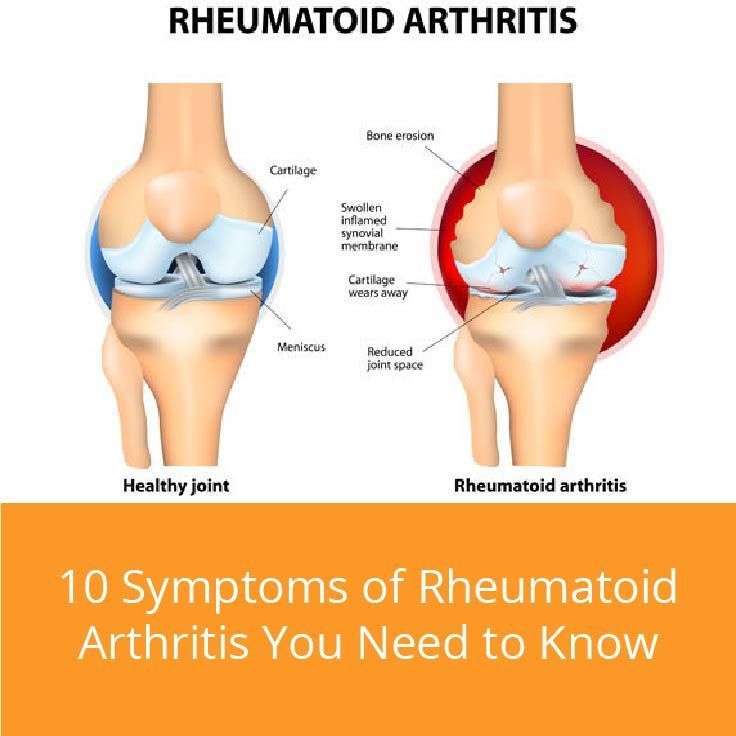
- Stage 1: In early stage rheumatoid arthritis, the tissue around your joint is inflamed. You may have some pain and stiffness. If your provider ordered X-rays, they wouldnt see destructive changes in your bones.
- Stage 2: The inflammation has begun to damage the cartilage in your joints. You might notice stiffness and a decreased range of motion.
- Stage 3: The inflammation is so severe that it damages your bones. Youll have more pain, stiffness and even less range of motion than in stage 2, and you may start to see physical changes.
- Stage 4: In this stage, the inflammation stops but your joints keep getting worse. Youll have severe pain, swelling, stiffness and loss of mobility.
You May Like: Does Advil Work For Arthritis
What Happens In Rheumatoid Arthritis
Doctors do not know why the immune system attacks joint tissues. However, they do know that when a series of events occurs, rheumatoid arthritis can develop. This series of events includes:
- A combination of genes and exposure to environmental factors starts the development of RA.
- The immune system may be activated years before symptoms appear.
- The start of the autoimmune process may happen in other areas of the body, but the impact of the immune malfunction settles in the joints.
- Immune cells cause inflammation in the inner lining of the joint, called the synovium.
- This inflammation becomes chronic, and the synovium thickens due to an increase of cells, production of proteins, and other factors in the joint, which can lead to pain, redness, and warmth.
- As RA progresses, the thickened and inflamed synovium pushes further into the joint and destroys the cartilage and bone within the joint.
- As the joint capsule stretches, the forces cause changes within the joint structure.
- The surrounding muscles, ligaments, and tendons that support and stabilize the joint become weak over time and do not work as well. This can lead to more pain and joint damage, and problems using the affected joint.
Key Points About Rheumatoid Arthritis
- RA is a long-term that causes joint inflammation.
- RA can also affect many nonjoint areas such as the lungs, heart, skin, nerves, muscles, blood vessels, and kidneys.
- RA may cause deformities in the joints of the finger, making movement difficult.
- The joints most often affected by RA are in the hands, wrists, feet, ankles, knees, shoulders, and elbows.
- Symptoms may include joint pain, stiffness, and swelling decreased and painful movement bumps over small joints and fatigue or fever.
Read Also: How Can You Help Arthritis
What Can I Take For Menopausal Arthritis
Treatment
- Perform low-impact exercises such as swimming, yoga, and biking.
- Eat a balanced diet that includes nutrients such as calcium and vitamin D.
- Take anti-inflammatory medications, such as ibuprofen .
- Take pain-relieving medications such as acetaminophen .
Do you get night sweats with RA?
RA is an autoimmune condition that causes inflammation in the joints. It is the result of an overactive immune system mistakenly attacking healthy tissue. Some people with RA report experiencing hot flushes. This includes night sweats and sudden, unexplained changes in temperature during the day.
What does menopausal arthritis feel like?
Menopausal joint pain usually hits the worst in the morning and eases as the joints loosen up with the days activities. Most women complain of back pain, neck pain, as well as pain in the jaw, shoulders, and elbows. Wrists and fingers can also be affected.
What helps with menopause joint pain?
How is menopause pain treated?
What Foods Are Good For Rheumatoid Arthritis
It is important to maintain a healthy diet if you have rheumatoid arthritis to help reduce your risk of developing serious symptoms. This includes:
- eating lots of fruits, vegetables and wholegrain cereal food, such as brown rice or oats
- eating foods that contain fish oil
- avoiding fatty, sugary or very salty foods
- not drinking alcohol often
- maintaining a healthy body weight
You May Like: Is Rheumatoid Arthritis Hard To Diagnose
Question 4 Of : Treatment
Circulatory Problems With Ra In The Feet
Some common circulatory issues in your feet that can result from RA include:
- Atherosclerosis. Also called hardening of the arteries, this happens when your arteries become narrow from plaque buildup. This can cause pain and cramps in your lower leg muscles.
- Raynauds phenomenon.This happens when blood is partially or fully blocked from reaching your toes. This results in blood vessels spasming and causing numbness, and abnormal color changes in your toes from white to blue to red. The toes can feel cold due to decreased blood flow.
- Vasculitis. This happens when your blood vessels get inflamed. This results in skin rashes, ulcers, and other possible symptoms like fever, loss of appetite, and fatigue.
RA cant be fully cured. But there are plenty of treatments to help relieve the symptoms of a flare-up, as well as reduce the number of flare-ups and prevent joint damage.
Here are some of the most common treatments for RA in your foot:
Here are a few tips to help relieve RA symptoms in your foot:
See your doctor as soon as possible if you notice any of the following symptoms of RA in the feet or elsewhere in your body:
- swelling in your feet or ankles
- skin ulcers on your feet or ankles
- foot pain that gets worse over time
- severe foot pain that makes it difficult to walk or do any activities with your feet
- losing range of motion in your foot or legs
- persistent, uncomfortable tingling or numbness in your feet
- abnormal weight loss
- persistent, abnormal exhaustion
Recommended Reading: Does Arthritis Show Up In Blood Work
What Is The Difference
Rheumatoid arthritis vs. osteoarthritis
Rheumatoid arthritis and osteoarthritis are both common causes of pain and stiffness in joints. But they have different causes. In osteoarthritis, inflammation and injury break down your cartilage over time. In rheumatoid arthritis, your immune system attacks the lining of your joints.
Rheumatoid arthritis vs. gout
Rheumatoid arthritis and gout are both painful types of arthritis. Gout symptoms include intense pain, redness, stiffness, swelling and warmth in your big toe or other joints. In gout, uric acid crystals cause inflammation. In rheumatoid arthritis, its your immune system that causes joint damage.
Causes Of Rheumatoid Arthritis

Rheumatoid arthritis is an autoimmune disease. This means your immune system attacks the cells that line your joints by mistake, making the joints swollen, stiff and painful.
Over time, this can damage the joints, cartilage and nearby bone.
It’s not clear what triggers this problem with the immune system, although you’re at an increased risk if:
- you are a woman
- you have a family history of rheumatoid arthritis
Find out more about the causes of rheumatoid arthritis.
Recommended Reading: What Is The Best Glucosamine For Arthritis
How Do Doctors Diagnose Rheumatoid Arthritis
There is no single test that shows whether you have RA. Your doctor will give you a checkup, ask you about your symptoms, and possibly perform X-rays and blood tests.
Rheumatoid arthritis is diagnosed from a combination of things, including:
- The location and symmetry of painful joints, especially the hand joints
- Joint stiffness in the morning
- Bumps and nodules under the skin
- Results of X-rays and blood tests
Can I Prevent Rheumatoid Arthritis
You cannot prevent rheumatoid arthritis because the cause of the disease is not known.
Quitting smoking, or never smoking, will reduce your risk of developing rheumatoid arthritis. You are more likely to develop rheumatoid arthritis if someone in your close family has it, but unfortunately there is no way to reduce this risk.
People who have rheumatoid arthritis often experience flare ups, which are times when their joints are particularly sore. Learning what triggers your flare ups can help reduce or prevent them.
For some people, stress can trigger a flare up, so can being run down or pushing yourself beyond your limits. Having an infection, missing a dose of your medicine or changing your treatment plan can also cause a flare up.
Keeping a food and activity diary may help work out your personal triggers but keep in mind that sometimes flare ups happen without any obvious cause.
You May Like: What Causes Arthritis Pain In Hands
What Are The Goals Of Treating Rheumatoid Arthritis
The most important goal of treating rheumatoid arthritis is to reduce joint pain and swelling. Doing so should help maintain or improve joint function. The long-term goal of treatment is to slow or stop joint damage. Controlling joint inflammation reduces your pain and improves your quality of life.
Symptoms Affecting The Joints
Rheumatoid arthritis is primarily a condition that affects the joints. It can cause problems in any joint in the body, although the small joints in the hands and feet are often the first to be affected.
Rheumatoid arthritis typically affects the joints symmetrically , but this is not always the case.
The main symptoms of rheumatoid arthritis affecting the joints are outlined below.
Don’t Miss: How To Treat Arthritis In Elbow
Joint Pain & Tenderness
Typically, joint pain is felt during times when the disease is active and the inflammation is irritating the joint, ultimately causing the pain .
Conversely, pain can also be felt when the disease isnt active because of past damage that has been done to the joints in the body. This is similar to pain from old sports injuries in the elbows, knees, and other joints.
In addition to outright pain, RA patients may also notice that their joints feel tender to the touch. This occurs when the inflammation in the joint tissue has affected the nerves within the joint capsule. In this case, any pressure placed on the jointseven slight compression during sleepcan elicit immediate pain.
Pain and tenderness may be felt if arthritic disease has settled into the bones in the cervical spine the vertebrae in the neck area of the spinal cord, or more specifically in the atlanto-axial joint .
It is the pain associated with RA that sends many patients in search of effective treatment options. Fortunately, there are quite a fewmany of which include nonsteroidal anti-inflammatory drugs or disease-modifying antirheumatic drugs providing RA patients some much-needed pain relief.
Amplification In The Synovium
Once the generalized abnormal immune response has become established which may take several years before any symptoms occur plasma cells derived from B lymphocytes produce rheumatoid factors and ACPA of the IgG and IgM classes in large quantities. These activate macrophages through Fc receptor and complement binding, which is part of the intense inflammation in RA. Binding of an autoreactive antibody to the Fc receptors is mediated through the antibody’s N-glycans, which are altered to promote inflammation in people with RA.
This contributes to local inflammation in a joint, specifically the synovium with edema, vasodilation and entry of activated T-cells, mainly CD4 in microscopically nodular aggregates and CD8 in microscopically diffuse infiltrates. Synovial macrophages and dendritic cells function as antigen-presenting cells by expressing MHC class II molecules, which establishes the immune reaction in the tissue.
Don’t Miss: Can Dogs Have Ibuprofen For Arthritis
Is It Ra Or Osteoarthritis
When you first notice foot pain, you may wonder if its osteoarthritis . OA is also known as wear-and-tear arthritis, and it is more common than rheumatoid arthritis.
There is no clear-cut way to tell if you have OA or RA without a medical diagnosis. But OA and RA do have some key differences.
-
Usually affects both feet at once
-
Morning stiffness generally lasts longer than half an hour
-
Most often affects only one foot
-
Stiffness tends to be easier to relieve in the morning, often getting better in less than half an hour or with a few minutes of stretching
Rheumatoid Nodules: Are Rheumatoid Nodules Dangerous
A variety of symptoms can occur when suffering from rheumatoid arthritis. The sporadic, yet chronic nature of the disease is such that symptoms may come and go over time and manifest in different ways.
One of the most common skin-based symptoms of rheumatoid arthritis is the development of nodules. These rheumatoid nodules occur in about one-quarter of rheumatoid arthritis patients, both men and women and their severity can vary from patient to patient. Although nodules are generally not dangerous or debilitating, there are treatment options available if it becomes necessary to have them reduced or removed.
Read Also: Can Rheumatoid Arthritis Be Hereditary
What Are The Complications Of Ra
Rheumatoid arthritis has many physical and social consequences and can lower quality of life. It can cause pain, disability, and premature death.
- Premature heart disease. People with RA are also at a higher risk for developing other chronic diseases such as heart disease and diabetes. To prevent people with RA from developing heart disease, treatment of RA also focuses on reducing heart disease risk factors. For example, doctors will advise patients with RA to stop smoking and lose weight.
- Obesity. People with RA who are obese have an increased risk of developing heart disease risk factors such as high blood pressure and high cholesterol. Being obese also increases risk of developing chronic conditions such as heart disease and diabetes. Finally, people with RA who are obese experience fewer benefits from their medical treatment compared with those with RA who are not obese.
- Employment. RA can make work difficult. Adults with RA are less likely to be employed than those who do not have RA. As the disease gets worse, many people with RA find they cannot do as much as they used to. Work loss among people with RA is highest among people whose jobs are physically demanding. Work loss is lower among those in jobs with few physical demands, or in jobs where they have influence over the job pace and activities.