Physical Exam For Diagnosing Psoriatic Arthritis
The next step in diagnosing psoriatic arthritis is a thorough physical exam, which can involve a number of steps, including the following:
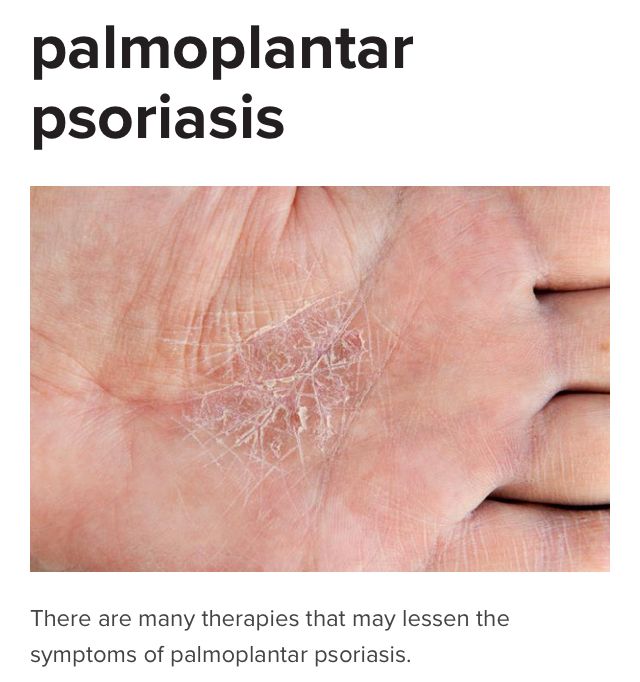
- Looking for signs of psoriasis in usual spots such as elbows and knees, as well as less visible places including the scalp, belly button, intergluteal cleft , palms of hands, and soles of feet
- Checking the nails of fingers and toes for abnormalities
- Applying pressure to joints for tenderness and swelling, as well as looking for redness
- Checking for tendon and ligament issues, including plantar fasciitis and Achilles tendonitis
- Checking for back mobility
- Checking for pain and inflammation along the sacroiliac joints, which is where the spine connects with your pelvis
Four Main Types Of Psoriatic Arthritis
There are 78 major joints in the body and psoriatic arthritis can affect any one of these. Usually, however, certain joints are more likely to be affected . Different patterns are found. Sometimes just one or two joints are a problem but often several joints, both large and small and on both sides of the body, are involved. About a third of people with psoriatic arthritis also have spondylitis which can result in a painful, stiff back or neck. Psoriasis can affect the nails with pitting, discolouration and thickening and this may be associated with inflammation in the joints at the end of the finger or toe. Another way in which psoriatic arthritis can be recognized is the finding of a sausage-like swelling of a finger or toe, called dactylitis. This is caused by inflammation occurring simultaneously in joints and tendons, painful heels and other bony prominence can also occur and this is caused by inflammation where gristle attaches to bone.
Can Psoriatic Arthritis Affect Other Parts Of The Body
Having psoriatic arthritis can put you at risk of developing other conditions and complications around the body.
The chances of getting one of these are rare. But its worth knowing about them and talking to your doctor if you have any concerns.
Eyes
Seek urgent medical attention if one or both of your eyes are red and painful, particularly if you have a change in your vision. You could go to your GP, an eye hospital, or your local A& E department.
These symptoms could be caused by a condition called uveitis, which is also known as iritis. It involves inflammation at the front of the eye.
This can permanently damage your eyesight if left untreated.
Other symptoms are:
- blurred or cloudy vision
- sensitivity to light
- not being able to see things at the side of your field of vision known as a loss of peripheral vision
- small shapes moving across your field of vision.
These symptoms can come on suddenly, or gradually over a few days. It can affect one or both eyes. It can be treated effectively with steroids.
Heart
Psoriatic arthritis can put you at a slightly higher risk of having a heart condition. You can reduce your risk by:
- not smoking
- staying at a healthy weight
- exercising regularly
- eating a healthy diet, thats low in fat, sugar and salt
- not drinking too much alcohol.
These positive lifestyle choices can help to improve your arthritis and skin symptoms.
Talk to your doctor if you have any concerns about your heart health.
Crohns disease
Non-alcoholic fatty liver disease
You May Like: Sudden Arthritis
How Do Doctors Treat Psoriatic Arthritis
Doctors will prescribe medicines to control the rash and lessen the swelling in your joints. Medicines that can help psoriatic arthritis include:
-
Acetaminophen and nonsteroidal anti-inflammatory drugs by mouth or creams that can be rubbed on the skin over painful joints
-
Injections of corticosteroids into the joint
Other Conditions And Joint Pain
Other forms of arthritis, and other conditions, can also cause joint pain. Examples include:
- fibromyalgia syndrome, a condition in which your brain processes pain in your muscles and joints in a way that amplifies your perception of the pain
- scleroderma, an autoimmune condition in which inflammation and hardening in your skin connective tissues can lead to organ damage and joint pain
Read Also: Rheumatoid Factor 7.0
Causes Of Psoriatic Arthritis
Almost 1 in 3 people with psoriasis also have psoriatic arthritis.
It tends to develop 5 to 10 years after psoriasis is diagnosed, although some people may have problems with their joints before they notice any skin-related symptoms.
Like psoriasis, psoriatic arthritis is thought to happen as a result of the immune system mistakenly attacking healthy tissue.
But it’s not clear why some people with psoriasis develop psoriatic arthritis and others do not.
How Psoriatic Arthritis Treatment Prevents Disease Progression
The primary way to slow the progression of PsA is through medications that modify the immune system. It may take trial and error to find the treatment that works best for a given patient, notes Dr. Haberman. While we have a lot of medication options for PsA, we dont know which ones a patient will respond to, so sometimes we need to try more than one medication to find the one thats right for that patient, she says.
In addition, medications that have been effective for you can stop working over time. If this happens, your doctor may recommend a medication that works differently say, targets a different part of the immune system to control disease activity.
There are many drugs used to treat PsA. The ones that you will use will depend on the type and severity of symptoms as well as the most problematic areas .
Medications use to treat PsA include:
Read Also: Rh Arthritis Treatment
You Can Have Psoriasis And A Different Kind Of Arthritis That Is Not Psa
People with psoriasis can develop different types of arthritis including rheumatoid arthritis, gout, osteoarthritis, and reactive arthritis so diagnosing PsA involves ruling out those other conditions.
Its often difficult to say in a first visit whether a patient definitely has psoriatic arthritis or another type of arthritis that just co-exists with psoriasis, says Dr. Kumar. PsA can take a long time to diagnose because a patient can delay seeing the doctor, then confirming PsA can require multiple labs and imaging tests.
The good news is that the diagnosis process for psoriatic arthritis is improving. Whereas PsA wasnt even recognized as a distinct condition decades ago , doctors are now better equipped with improved lab tests and imaging studies that help identify this disease so more patients can find relief.
Just Because Youre Not Strong Enough To Push A Shopping Cart Doesnt Mean You Dont Work Out
Rabe says she exercises four to five times a week at home and in the swimming pool. But on some days the pain can keep her from doing the simplest things, like pushing a shopping cart. While exercising cant completely alleviate your symptoms, it can help strengthen the muscles around your joints. Biking, walking, and swimming are all good fitness options for people with psoriatic arthritis.
Read Also: Psoriatic Arthritis Rash On Face
What Are The Treatment Options For Psoriatic Arthritis
The aim of treatment for psoriatic arthritis is to control the disease and relieve symptoms. Treatment may include any combination of the following:
- Splinting.
- Surgery.
Choice of medications depends on disease severity, number of joints involved, and associated skin symptoms. During the early stages of the disease, mild inflammation may respond to nonsteroidal anti-inflammatory drugs . Cortisone injections may be used to treat ongoing inflammation in a single joint. Oral steroids, if used to treat a psoriatic arthritis flare, can temporarily worsen psoriasis. Long-term use of oral steroids should be avoided when possible due to the negative effects on the body over time.
DMARDs are used when NSAIDs fail to work and for patients with persistent and/or erosive disease. DMARDs that are effective in treating psoriatic arthritis include: methotrexate, sulfasalazine, and cyclosporine.
Biologic agents are an important consideration when disease control is not being achieved with NSAIDS or DMARDs. Biologics have been utilized for the treatment of psoriatic arthritis since 2005 and are highly effective at slowing and preventing progression of joint damage. Your healthcare provider will complete additional laboratory tests and review safety considerations before initiating a medication regimen. Gaining good control of psoriatic arthritis and psoriasis is important to avoid increased systemic risks, particularly heart disease.
Exercise
Heat and cold therapy
Splinting
Surgery
How Is Psa Diagnosed
It can be challenging for doctors to diagnose PsA because the symptoms are similar to other types of arthritic diseases such as rheumatoid arthritis, reactive arthritis, and gout. People who have symptoms of PsA or people who have psoriasis and develop joint pain should consider seeing a type of doctor called a rheumatologist. These doctors are specialists in musculoskeletal disorders , so they have more experience and expertise in making the diagnosis.
To make the diagnosis of psoriatic arthritis, your doctor may:
- Examine you for swollen and painful joints and for skin and nail changes.
- Take X-rays to look for damage to your joints.
- Do scans such as an MRI or ultrasound to get a more detailed look at your joints.
- Do blood tests to make sure you dont have other types of arthritis.
Dont delay
If you have been diagnosed with psoriasis and notice joint pain, tell your doctor right away. It could be a sign of PsA. If you are diagnosed with PsA, work with your healthcare provider to develop a treatment plan best suited for you. Early diagnosis and treatment can help relieve pain and inflammation and help prevent disease progression or reduce further joint damage.
Recommended Reading: Symptoms Of Arthritis In Your Hands
How Can I Find The Appropriate Care I Need
Initially your GP is the first point of contact, who then should refer you on to a dermatologist/rheumatologist, if this is not already the case. If you are not happy with the advice you receive, remember you are always entitled to seek a second opinion. Remember, If you are seeing a dermatologists for your psoriasis and a rheumatologists for your arthritis make sure each is aware of this, so they can liaise and provide you with appropriate care for both conditons.
You Have Pain Or Burning In Your Elbow
A condition called tennis elbow can sometimes show up as a symptom of psoriatic arthritis, even if youve never picked up a racquet. Again, this has to do with the inflammation that happens in spots where your tendons connect to bones, says Dr. Rosenstein. You might notice pain or burning in the external part of your elbow, along with poor grip strength, per the American Academy of Orthopedic Surgeons.
Don’t Miss: Rheumatoid Arthritis Itching Skin
As Can The Words Youre Too Young To Have Arthritis
When you say the word arthritis, every older person you meet has it, too, Dishner says. While well-meaning people may sympathize by comparing their own ailment with yours, psoriatic arthritis is a much different form of arthritis and does not develop because of aging. It can occur at any age but typically begins to cause symptoms among those between 30 and 50 years old, according to the NPF.
Your Lower Back And Hips Are Often Sore
While many of the symptoms of rheumatoid arthritis and psoriatic arthritis overlap, back pain can help differentiate between the two conditions.
When psoriatic arthritis affects the spine, it is most often the lowest portions of the spine and the sacroiliac joints that are affected, whereas rheumatoid arthritis most often affects the very top of the neck, says Dr. Rosenstein.
Inflammation in the sacroiliac joints can also extend into your butt, Lynn M. Ludmer, M.D., medical director of rheumatology at Baltimores Mercy Medical Center, tells SELF. This might make it even more confusing to figure out whats going on.
Also Check: Rheumatoid Arthritis Remission Naturally
Things To Know About Psoriatic Arthritis
Learn more about what it means to have psoriatic arthritis.
1. PsA Is an Autoimmune Disease
2. It Has Ups and Downs, Called Flares
3. It Can Be a Master of Disguise
4. It Has Distinguishing Features
5. It Affects Up to a Third of People with Psoriasis
6. Its Gender Neutral
7. It May be Hereditary
8. Its Not Contagious
9. It Isnt Just About Your Joints
10. You May Not Look Sick
11. Effective Treatment is Available
Quick Links
Swollen And Painful Joints
PsA can lead to pain and swelling in any joint in the body. The joints may also be red and warm to the touch.
PsA often affects the hands, fingers, feet, toes, knees, ankles, and spine. It can also affect the neck and wrists. A person may also experience pain in the lower back.
PsA in the finger usually affects the joint closest to the nail.
Swelling in arthritis happens when either the lining of the joint or the fluid that surrounds the joint increases in volume. When this happens, more blood enters the area around the joint, which increases pressure and causes redness and swelling.
Symptoms can vary in severity between people. In some people, arthritis may affect one or two joints, but others might experience severe changes throughout the body.
Also Check: Mayo Clinic Arthritis Treatment
Delays In Getting Diagnosed With Psoriatic Arthritis Are All Too Common Knowing What To Expect May Help Speed Up The Process
If your shoes are feeling tighter than usual or youre having difficulty or pain opening jars, a type of autoimmune disorder called psoriatic arthritis could be to blame. PsA is an inflammatory arthritis linked to psoriasis . It is characterized by pain, stiffness, and swelling in the joints although these general arthritis symptoms can take on specific characteristics when they are caused by psoriatic arthritis
As with many conditions, early diagnosis and prompt treatment are important. If you put off seeing the doctor, there are two major concerns with a delayed psoriatic arthritis diagnosis, says Bharat Kumar, MD, Associate Rheumatology Fellowship Program Director at University of Iowa Health Care and member of the American College of Rheumatology.
First, he explains, disease activity may worsen and cause lasting joint damage. Second, PsA is linked to a higher rate of heart disease, so the sooner youre diagnosed the quicker you can address cardiovascular factors like high cholesterol and hypertension. Rheumatologists are eager to see anyone with psoriasis who is also experiencing joint pain, Dr. Kumar says.
How Are Ra And Psa Diagnosed
Because these two conditions share similar symptoms, it’s important to get an accurate diagnosis from a rheumatologist. A rheumatoid factor blood test is one way your doctor can tell which condition you have. RF is a protein found in people with rheumatoid arthritis. People with PsA usually don’t have it. Blood tests looking for other antibodies such as anti-CCP can also help differentiate the two.
Another way to tell is to look at your skin and nails. If you have scaly patches on your skin, pitting and flaking on your nails, or both, you have PsA.
Once you’ve had the disease for a while, X-rays might also be able to distinguish the two conditions.
It is possible to have RA and PsA together, but it’s rare. If you do have both, many of the treatments, including some medications, will work for both conditions.
Don’t Miss: Can You Stop Arthritis In Fingers
What Causes Ra And Psa
RA runs in families. If you have a close relative with the disease, your chances of having it are higher. Women are more likely than men to get RA. Usually the symptoms start between ages 40 and 60.
PsA also runs in families. Certain genes may be linked to the condition. Compared to RA, PsA often starts between ages 30 and 50.
Researchers don’t know exactly what triggers either type of arthritis. But they think it probably comes from a mix of genes and other factors, including hormones and bacterial or viral infections that may send the immune system into overdrive.
What To Expect At The Doctors Office
You may be seeing various health care providers during your journey to figure out whats causing your symptoms. Its common for people to see their internist/general practitioner, a dermatologist to treat their psoriasis, or other types of doctors to manage specific areas that are causing pain, such as a podiatrist to treat foot pain. However, if you or any of the health care providers you are currently seeing suspect it could be psoriatic arthritis, ask for a referral to a rheumatologist. These doctors specialize in arthritis and have the training to determine whether your joint symptoms are due to PsA or could be something else.
Psoriatic arthritis can be challenging to diagnose for a number of reasons, including:
Don’t Miss: Arthritis Attack Symptoms
Youre Always On The Search For The Next Best Thing
In recent decades, there have been more advances in medications and studies confirming the benefits of certain therapies for psoriatic arthritis than ever before. Doing your own research and following up on it with your rheumatologist will help you and the doctor find and maintain the best treatment plan. Says Dishner, Its important to understand your options and to never give up hope.
Infectious And Reactive Arthritis
Infectious arthritis is an infection in one of your joints that causes pain or swelling. The infection can be caused by bacteria, viruses, parasites, or fungi. It can start in another part of your body and spread to your joints. This kind of arthritis is often accompanied by a fever and chills.
Reactive arthritis can occur when an infection in one part of your body triggers immune system dysfunction and inflammation in a joint elsewhere in your body. The infection often occurs in your gastrointestinal tract, bladder, or sexual organs.
To diagnose these conditions, your doctor can order tests on samples of your blood, urine, and fluid from inside an affected joint.
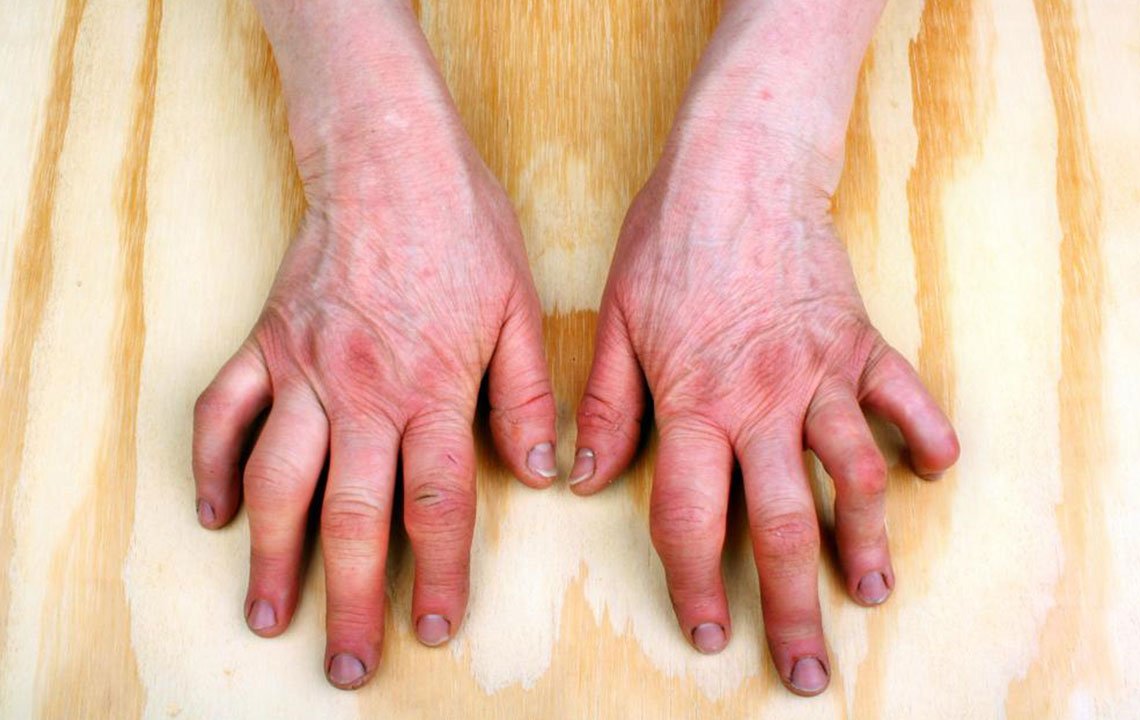
The fingers are most commonly affected with psoriatic arthritis , but this painful condition affects other joints as well. Pink-colored fingers that appear sausage-like, and pitting of the fingernails, may also occur.
The disease may also progress to your spine, causing damage similar to that of ankylosing spondylitis.
If you have psoriasis, theres a chance you could also develop PsA.
Also Check: Rheumatoid Arthritis Better With Movement