How Is Seronegative Rheumatoid Arthritis Diagnosed
Some patients still have RA but do not test positive for either anti-CCPs or RF they have seronegative RA.
Annals of the Rheumatic Diseases
Your doctor may also conduct a synovial biopsy, which involves removing a small piece of the tissue lining one of your joints.
RELATED: Psoriatic vs Rheumatoid Arthritis: Whats The Difference?
Types Of Rheumatoid Arthritis
Rheumatoid arthritis is often diagnosed at least in part by blood test results that indicate the presence of certain proteins or other blood factors. These test results can indicate the type of RA thats present:
Juvenile RA is when children under age 17 show symptoms of rheumatoid arthritis. Juvenile RA symptoms can be temporary or long-term and can affect normal growth and development.
Seronegative RA is showing signs and symptoms of rheumatoid arthritis despite testing negative for RF and anti-CCP. People with RF-negative RA tend to have milder symptoms than those who have RF-positive RA.
Seropositive RA is when your blood tests show the presence of a protein called rheumatoid factor , or the antibody anti-cyclic citrullinated peptide . These results indicate that your body could be having an abnormal immune system response. Most people with rheumatoid arthritis are RF-positive.
What Are First Signs Of Rheumatoid Arthritis
The 15 early RA symptoms and signs discussed in this article include the following:
- Fatigue.
- Loss of joint range of motion.
Likewise, how do you know if you have arthritis in your hands?
arthritisfingersif yourfingerhavefinger
What are the symptoms of arthritis in the fingers?
Symptoms of arthritis in the hands may include:
- Pain in some or all of the joints, including joints of the fingers, wrists, and thumbs.
- The growth of bony knobs on finger joints.
- Numbness in fingers.
- Swollen, red, or warm joints.
- Stiffness in the fingers, especially in the morning in patients who have rheumatoid arthritis.
Can I have arthritis in one finger?
arthritiscanhandsfingersYoufinger
Read Also: Mayo Clinic On Arthritis
Difference Between Osteoarthritis And Rheumatoid Arthritis
There are several different types of arthritis. Osteoarthritis and rheumatoid arthritis are two of the most common forms. Although the symptoms of these two types of arthritis can be similar, it’s very important to distinguish between them in order to determine the proper treatment.
At the University of Michigan Health System, our experienced rheumatologists will do appropriate tests to determine which type of arthritis you have. Then we will develop an effective treatment plan and will explain your options.
Osteoarthritis occurs when the smooth cartilage joint surface wears out. Osteoarthritis usually begins in an isolated joint.
Rheumatoid arthritis is an autoimmune disease, which means that the immune system malfunctions and attacks the body instead of intruders. In this case, it attacks the synovial membrane that encases and protects the joints. Rheumatoid arthritis often targets several joints at one time. The symptoms of rheumatoid arthritis include:
- the symmetrical nature of the disease ,
- fever
What Foods Are Good For Rheumatoid Arthritis

It is important to maintain a healthy diet if you have rheumatoid arthritis to help reduce your risk of developing serious symptoms. This includes:
- eating lots of fruits, vegetables and wholegrain cereal food, such as brown rice or oats
- eating foods that contain fish oil
- avoiding fatty, sugary or very salty foods
- not drinking alcohol often
- maintaining a healthy body weight
You May Like: Side Effects Of Arthritis
What Is The Prognosis For People Who Have Rheumatoid Arthritis
Although there is no cure for rheumatoid arthritis, there are many effective methods for decreasing the pain and inflammation and slowing down the disease process. Early diagnosis and effective treatment are very important.
Extensive research is being done to learn the cause of rheumatoid arthritis and the best methods of treatment.
Last reviewed by a Cleveland Clinic medical professional on 11/17/2017.
References
Lab And Blood Tests For Ra
Here are some of the things you can expect to happen at your appointment if the doctor thinks you have RA.
Personal and family medical history: Your doctor will ask about your past and your relativesâ. If someone in your family tree has RA, you may be more likely to have the disease.
Physical exam: The doctor will check your joints for swelling, tenderness, and range of motion. RA tends to strike several joints.
Antibody blood tests: Doctors look for certain proteins that show up in your blood when you have RA. These proteins mistakenly target healthy cells and kick off the inflammation process. So a high or positive test result means inflammation is in your body.
- Rheumatoid factor : high levels
- Anti-CCP : high levels
- ANA, or antinuclear antibodies: the results are positive or negative
Not all people with RA have these proteins.
Other blood tests: Besides RF and anti-CCP, other blood tests could include:
Complete blood count: It helps your doctor find anemia , which is common in RA. It looks for four things:
- White blood cells 4.8-10.8
- Hematocrit 42-52
- Platelets 150-450
Erythrocyte sedimentation rate: This measures how fast your red blood cells clump and fall to the bottom of a glass tube within an hour. Your doctor might call it a sed rate.
Normal ranges are:
- Men younger than 50: 0-15 mm/h
- Men older than 50: 0-20 mm/h
- Women younger than 50: 0-20 mm/h
- Women older than 50: 0-30 mm/h
Don’t Miss: Relief For Rheumatoid Arthritis In Hands
They Ask About Other Symptoms
Although symmetrical joint pain and swelling are the hallmarks of rheumatoid arthritis, its a full-body disease that can cause full-body symptoms. Sometimes, people experience loss of appetite, exhaustion, low-grade fever, and even nerve damage, says Dr. Cohen. Neuropathymuscle weakness, numbness, or a pins-and-needles sensationmay be another clue RA is the culprit. Osteoarthritis, on the other hand, is much more of a localized condition.
Recommended Reading: Whats Best To Take For Arthritis
Problems With Old Assessments
After diagnosis, the level and progression of RA need to be monitored and tracked. Prior to RASS, doctors combined results from a physical examination with factors reported by the patient, such as pain level, and inflammatory blood markers, to estimate RA severity.
Doctors also used the Health Assessment Questionnaire , in which patients rated their own level of pain. Of course, everyone has a different threshold for pain, which can make these assessment models inaccurate. These assessment methods were also complicated by a close relationship between pain and depression.
Depression can be a significant component of RA. But there are challenges with using it to measure disease severity, including:
- some patients may be more depressed than others
- some patients may feel particularly depressed at the time of examination
- some patients may not acknowledge they are depressed
While depression can be an element of RA, measuring it is not helpful for disease activity assessment. The RASS is completed by your doctor and based on the visible signs of the disease. Its not based on your individual emotional assessment.
Its important to know what type of RA you have to get an accurate assessment of disease activity. There are three types of RA:
- rheumatoid factor positive
Recommended Reading: What To Take For Arthritis Pain
Also Check: Signs Of Arthritis In Arm
When To See A Doctor
RA can become worse the longer its left untreated. Its important to visit your doctor if youve been living with some of these symptoms for more than a few weeks, especially if youve been noticing joint stiffness that takes a while to loosen up in the mornings.
Even if its not RA, persistent fatigue and a general sense of illness can be the precursor to many inflammation-related issues, so the sooner youre seen by a physician, the better.
Theres no single test that can reveal an RA diagnosis. Instead, youll most likely be diagnosed through blood tests, joint and organ examinations, and X-ray or ultrasound images.
If a positive rheumatoid arthritis diagnosis is found, youll probably be referred to a rheumatologist, a doctor whos had extra training around the treatment of diseases that affect the muscles, bones, joints, ligaments, and tendons.
Care For Hand Arthritis In The Greater Chesapeake Region
If you have ongoing hand pain, see the orthopedic experts at Greater Chesapeake Hand to Shoulder. We specialize in both non-surgical and surgical treatments to address a full range of hand and finger conditions and injuries.
To find out more about the services we offer, schedule an appointment with one of our Maryland hand surgeons today at or fill out our Request an Appointment form now for a visit at any of our Greater Chesapeake locations. We look forward to helping you find relief from your hand pain so you can get back to doing everything you enjoy every day.
Recommended Reading: Arthritis Remission
The Diagnostic Criteria For Rheumatoid Arthritis
The diagnosis of rheumatoid arthritis cant be established with just one test. Instead, rheumatologists rely on a combination of your medical history, a physical exam, laboratory tests, and sometimes imaging tests to pinpoint the disease.
They also try to rule out the possibility of other conditions that may resemble RA, such as lupus, psoriatic arthritis, gout, or osteoarthritis. This is called a differential diagnosis.
To begin the diagnostic process, a rheumatologist will take your medical history, which includes asking questions about your current symptoms particularly pain, swelling, and stiffness and their location, duration, and severity.
Theyll also ask about your familys medical history as it pertains to RA and other autoimmune conditions. Conditions like RA can be more common in families with RA or other immune system-related health problems. For example, research recently published in the journal Arthritis Care & Research found that people who have a first-degree relative with RA are more than twice as likely as the general population to develop RA. A family history of lupus, scleroderma, thyroid disease, or inflammatory bowel disease also substantially increased the risk of RA.
Your rheumatologist will also perform a physical examination, testing each of your joints for things like swelling, tenderness, and limited range of motion. The location of affected joints is important to diagnosis.
Physical Exam And Medical History
The appointment will likely begin with the physician taking a thorough medical history. This will include asking the patient several questions, such as:
- What joints are affected?
- How would you describe the pain?
- Do you have morning stiffness?
- Have you noticed increased fatigue or weight changes?
- Have you experienced other symptoms besides joint pain?
- When did symptoms begin?
- How have symptoms changed over time?
- What movements or activities make the patient feel better or worse?
The history will also include a review of the patients:
- Other medical problems
See Lifestyle Factors and Fatigue Associated with Rheumatoid Arthritis
During the physical exam, a doctor will evaluate the patients general health and then examine the joints, looking for signs of joint inflammation. For example, a doctor may measure a joints range of motion, press the skin over a joint to see if it causes pain, and test joint strength.
Don’t Miss: What Does A High Rheumatoid Factor Mean
Diagnosis And Management Of Rheumatoid Arthritis
AMY M. WASSERMAN, MD, Boston University School of Medicine, Boston, Massachusetts
Am Fam Physician. 2011 Dec 1 84:1245-1252.
Patient information: A handout on this topic is available at .
Rheumatoid arthritis is the most common inflammatory arthritis, with a lifetime prevalence of up to 1 percent worldwide.1 Onset can occur at any age, but peaks between 30 and 50 years.2 Disability is common and significant. In a large U.S. cohort, 35 percent of patients with RA had work disability after 10 years.3
SORT: KEY RECOMMENDATIONS FOR PRACTICE
Patients with inflammatory joint disease should be referred to a rheumatology subspecialist, especially if symptoms last more than six weeks.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
|
In persons with RA, combination therapy with two or more disease-modifying antirheumatic drugs is more effective than monotherapy. However, more than one biologic agent should not be used at one time because of the high risk of adverse effects. |
||
|
A guided exercise program can improve quality of life and muscle strength in patients with RA. |
||
|
Cardiovascular disease is the main cause of mortality in persons with RA therefore, risk factors for coronary artery disease should be addressed in these patients. |
RA = rheumatoid arthritis.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
RA = rheumatoid arthritis.
Rheumatoid Arthritis: Causes Symptoms Treatments And More
Rheumatoid arthritis is an inflammatory type of arthritis that can causes joint pain, swelling and damage. Learn what causes RA and how to treat it.
Rheumatoid arthritis causes joint inflammation and pain. It happens when the immune system doesnt work properly and attacks the lining of the joints . The disease commonly affects the hands, knees or ankles, and usually the same joint on both sides of the body. But sometimes, RA causes problems in other parts of the body as well, such as the eyes, heart and circulatory system and/or lungs. For unknown reasons, more women than men get RA, and it usually develops in middle age. Having a family member with RA increases the odds of developing RA.
Causes
In a healthy person, the immune system fights invaders, such as bacteria and viruses. With an autoimmune disease like RA, the immune system mistakes the bodys cells for foreign invaders and releases inflammatory chemicals that attack, in the case of RA, the synovium. Thats the tissue lining around a joint that produces a fluid to help the joint move smoothly. The inflamed synovium gets thicker and makes the joint area feel painful and tender, look red and swollen and moving the joint may be difficult.
Researchers arent sure why some people develop RA. They think that these individuals have certain genes that are activated by a trigger in the environment, like a virus or bacteria, or physical or emotional stress or some other external factor.
Symptoms
Also Check: Can Arthritis Cause Swelling
Human Leukocyte Antigen Tissue Typing
This test checks for a genetic marker called human leukocyte antigen .
Some studies suggest that around 60% of RA cases may be inherited. If a person has specific antigens, it could mean that they have a higher likelihood of developing RA. However, other factors, such as tobacco use, can also trigger the condition.
HLA markers in the blood can help indicate the likelihood of developing an immune-related condition such as RA. These markers may also be a sign of another condition, such as ankylosing spondylitis or reactive arthritis.
What Are The Symptoms Of Rheumatoid Arthritis
The symptoms of rheumatoid arthritis include the following:
- Stiffness, especially in the morning or after sitting for long periods
- Fatigue
Rheumatoid arthritis affects each person differently. In most people, joint symptoms may develop gradually over several years. In other people, rheumatoid arthritis may proceed rapidly. A few people may have rheumatoid arthritis for a limited period of time and then go into remission .
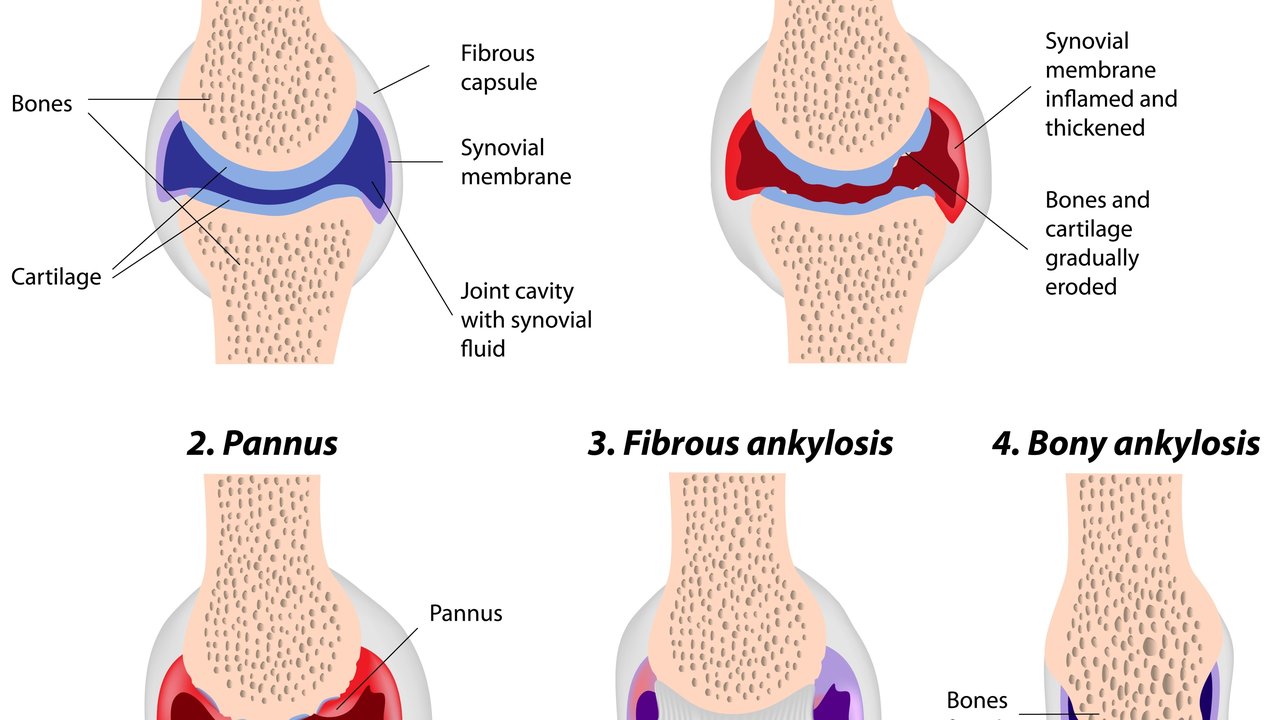
Cartilage normally acts as a shock absorber between the joints. Uncontrolled inflammation causes the destruction and wearing down of the cartilage, which leads to joint deformities. Eventually, the bone itself erodes, potentially leading to fusion of the joint . This process is aided by specific cells and substances of the immune system, which are produced in the joints but also circulate and cause symptoms throughout the body.
Don’t Miss: Arthritis On One Side Of Body
Making A Diagnosis Of Rheumatoid Arthritis
Diagnosis of RA is not straight forward as there is no individual test for RA. A diagnosis tends to be made by a consultant rheumatologist on the basis of tests, examination and ruling out other possible causes for symptoms.
Sometimes it is clear from symptoms and initial blood tests that someone has rheumatoid arthritis, but not always. Specialist criteria have been developed jointly by American and European experts to try to help make a diagnosis of rheumatoid arthritis in people presenting with new-onset swollen, painful joints with no obvious cause . These should be used with care though as people with osteoarthritis or a crystal arthritis could meet the criteria and end up being incorrectly diagnosed with rheumatoid arthritis, which could have significant consequences for treatment. They have also been developed to classify, not diagnose, rheumatoid arthritis and so should not be used to decide who gets referred.
As already mentioned above, there are a number of other conditions that can cause very similar symptoms to rheumatoid arthritis and your GP will have to consider these when assessing each case.
What Should Be Done If Rheumatoid Arthritis Is Suspected
Any person who is suspected of having RA should be referred to a specialist rheumatologist. Early referral is important so that disease modifying anti-rheumatic drugs may be prescribed as soon as possible so as to slow or halt the disease process. Delay in referral or receiving a definitive diagnosis and treatment can result in significant costs to the individual, particularly those who are employed. This is because joint damage occurs most rapidly in the early stages of the disease, and often the treatment drugs can take several months to work.
Many areas now offer Early Arthritis Clinics where a rapid assessment is performed by specialists/specialist nurses in order to limit any delays. An ultrasound of the affected joints may be performed during this assessment.
If your symptoms are particularly severe when you first see your GP, then they may refer you urgently but also ring to speak to one of the local rheumatologists to ask for assistance in how to best help you in the meantime. Sometimes people are started on treatments other than those mentioned above, e.g. steroid tablets or a steroid injection, prior to being seen, in order to improve their condition. This though can affect what the specialists see and find at the first appointment, which can potentially delay their making a diagnosis or there may be increased uncertainty of the diagnosis.
You May Like: What Relieves Arthritis Pain In The Hands