Poor Circulation Skin Rash
Poor Circulation Skin Rash. Stasis dermatitis is the dark discoloration of the skin, usually a brown pigmentation, due to poor venous drainage in the legs. It is also known as venous eczema. This is usually as a result of poor circulation caused by venous insufficiency, the inability or incompetence of the leg veins to assist with returning .
Rheumatoid Arthritis And Itching Attacks
Are you experiencing persistent and painful itching with rheumatoid arthritis ? Youre not alone. While itching is not a classic symptom of RA, myRAteam members are frequently plagued by prickly skin patches, rashes, and hives. Ill scratch and scratch. It makes me crazy! reported one member. It feels like something is crawling on me, said another. I’m literally digging myself raw, added one man.
Rheumatoid Arthritis And Skin Vasculitis
Rheumatoid arthritis can also cause inflammation of the blood vessels, known as vasculitis. Most often, small blood vessels are involved, notably those that supply blood to the skin on the fingertips. This usually looks like a blue or purplish rash near the fingernails, Dr. Tehrani says.
More serious forms of vasculitis can occur in larger blood vessels, such as those in the legs, and cause painful rashes or ulcers. If left untreated, these ulcers can become infected, so see a doctor immediately if you suspect an issue.
Also Check: Tomatoes Bad For Arthritis
Antibody To Neutrophil Cytoplasmic Antigens
I will mention one other laboratory test in this context. That is the ANCA test. ANCA stands for “antibody to neutrophil cytoplasmic antigens.” This test is often positive in forms of blood vessel inflammation such as vasculitis.
One of the strongest disease associations of the ANCA test is a disease called Wegener’s granulomatosis. This is a disease that can attack blood vessels in different parts of the body, including the skin. Recognizing the characteristic patterns of skin changes can be a clue to the diagnosis of this disease and getting patients on proper treatment for the internal complications that can be very severe .
However, like the ANA test, one must be careful in interpreting the ANCA test results. The ANCA test can be positive in other conditions besides vasculitic illnesses, such as Wegener’s granulomatosis.
The treatment really has to be individualized to the specific disease and to the specific conditions related to a given case. Some drugs might be riskier in women compared to men, for example.
Rheumatoid Arthritis Can Cause A Range Of Skin Symptoms But Skin Problems Could Also Indicate You Have A Different Kind Of Arthritis To Begin With
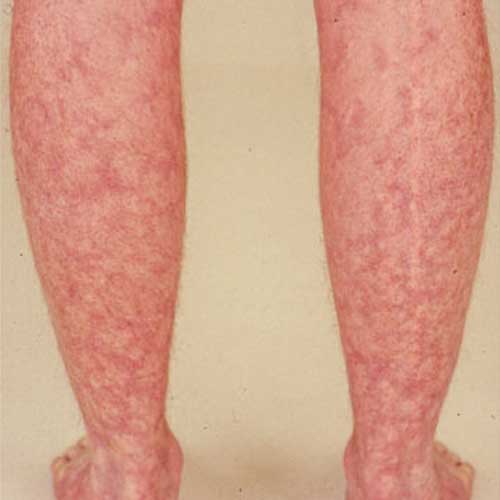
Before the modern era of treating rheumatoid arthritis early with disease-modifying drugs, you could often guess that a person had RA just by looking at their skin. Long-term, severe rheumatoid arthritis damages small blood vessels throughout the body. This condition is called rheumatoid vasculitis, which shows up as bruising, pain, and sores on the skin. Another telltale sign of RA used to be rheumatoid nodules under the skin, often near affected joints.
We used to see nodules a lot, but these lumpy bumps about the consistency of a pencil eraser are getting less common with better therapy, says rheumatologist Kevin Deane, MD, PhD, associate professor of medicine at the University of Colorado School of Medicine.
While, thankfully, these skin conditions are no longer as common as they used to be, many people with RA can develop skin problems that raise questions about whether and how they might be related to their arthritis.
Also Check: Is Eating Tomatoes Bad For Arthritis
What Are The Complications Of Ra
Rheumatoid arthritis has many physical and social consequences and can lower quality of life. It can cause pain, disability, and premature death.
- Premature heart disease. People with RA are also at a higher risk for developing other chronic diseases such as heart disease and diabetes. To prevent people with RA from developing heart disease, treatment of RA also focuses on reducing heart disease risk factors. For example, doctors will advise patients with RA to stop smoking and lose weight.
- Obesity. People with RA who are obese have an increased risk of developing heart disease risk factors such as high blood pressure and high cholesterol. Being obese also increases risk of developing chronic conditions such as heart disease and diabetes. Finally, people with RA who are obese experience fewer benefits from their medical treatment compared with those with RA who are not obese.
- Employment. RA can make work difficult. Adults with RA are less likely to be employed than those who do not have RA. As the disease gets worse, many people with RA find they cannot do as much as they used to. Work loss among people with RA is highest among people whose jobs are physically demanding. Work loss is lower among those in jobs with few physical demands, or in jobs where they have influence over the job pace and activities.
What Causes Rheumatoid Arthritis
Rheumatoid arthritis is multifactorial in origin. Although regarded as autoimmune with anti-citrullinated proteinantibodies and rheumatoid factor , genetic and environmental factors are also important in the pathogenesis. In ACPA-positive disease the most significant association is mapped to the HLA-DRB4 gene. ACPA are found in 60% of patients with rheumatoid arthritis .
Recommended Reading: Is Banana Bad For Arthritis
Treatment Of Rheumatoid Vasculitis
Rheumatoid vasculitis is a serious condition and must be treated aggressively because it can lead to serious complications, depending on the location of the vasculitis. For example, for vasculitis directly on joints, ulcers can form that are difficult to heal. In addition, rheumatoid vasculitis can progress and cause nerve damage.
Treatment is dependent on the severity of the rheumatoid vasculitis. Prednisone, a steroid, is often the first-line treatment.
Controlling RA, in general, is also indicated, so medications that treat RA such as methotrexate and tumor necrosis factor inhibitors are prescribed. If rheumatoid vasculitis has progressed to major organs or has caused a skin ulcer, cyclophosphamide, a chemotherapy medication, may be prescribed.
According to Johns Hopkins, the incidence of rheumatoid vasculitis has declined in recent years. It is possible that better treatment options for RA have led to the decline.
Signs And Symptoms Of Psoriatic Arthritis
For most people, psoriatic arthritis develops years after psoriasis. Contact your dermatologist if you have psoriasis and any of these signs or symptoms:
- A very noticeable swollen finger or toe
- Swollen and tender joints
- Stiffness when you wake up or sit for hours that fades as you move
- Nails that are pitted
- Nail separating from nail bed
- Lower back pain
Read Also: Is Banana Good For Rheumatoid Arthritis
Research On Rheumatoid Arthritis
In the last decade, much research has been conducted to increase our understanding of the immune system and what makes it malfunction. There have also been new therapies developed to help treat the disease. Some of the topics of intense research include:
What are the genetic factors that predispose people to develop rheumatoid arthritis?
Some white blood cells, commonly known as T cells, are important in maintaining a healthy and properly functioning immune system. However, scientists have discovered a variationcalled single nucleotide polymorphism in a gene that controls T cells. When the SNP gene variation is present, T cells attempt to correct abnormalities in joints too quickly, causing the inflammation and tissue damage associated with RA. The discovery of SNP may help determine peoples risk for getting RA and might help explain why autoimmune diseases run in families.
At conception, twins have an identical set of genes. So why would only one twin develop RA?
Broken Or Brittle Bones
Rheumatoid arthritis is associated with a loss in bone mineral density,17,18 which is the hallmark sign of osteoporosis. In fact, osteoporosis is considered typical in people who have had rheumatoid arthritis for a long time.19
Certain medications can also increase the risk of developing osteoporosis and its precursor, osteopenia. For example, prednisone and other corticosteroids, which may be prescribed to treat newly diagnosed RA and RA flares, are associated with a loss of bone mineral density.20
Osteoporosis causes bones to become porous and weaker. Osteoporotic bones are:
- More prone to breaking
- Less suitable for joint replacement or other orthopedic surgeries
A bone break can have a negative effect on joint mechanics, even after the bone has healed, increasing the risk for osteoarthritis.
Recommended Reading: Are Eggs Bad For Psoriatic Arthritis
Lupus Skin Rashes In Adults
Chilblains causes the skin on your toes, other parts of your feet, fingers, or other affected areas to burn and itch. Some people see their skin swell and turn red or dark blue. A severe case of chilblains can cause sores or blisters. Chilblains differs from frostbite, which occurs when the skin freezes. Coronavirus rash appears in many ways
Sticking With Your Medication May Be The Most Important Skin
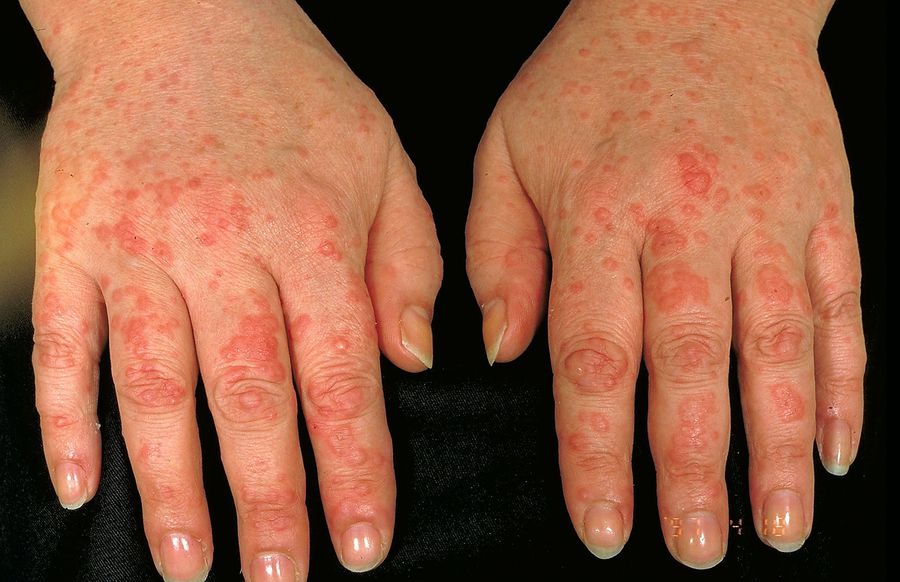
The most important way to maintain healthy skin while living with RA, Tehrani says, is to follow a doctor-prescribed medication schedule. If a patient is complying with the medication their rheumatologist gives them and theyre taking it on time, they usually wont have to deal with many of these side effects, she says.
Sun protection is also key to avoiding skin complications. Wear long sleeves and hats to protect yourself when you go outside, Tehrani says, and always wear sunscreen. Keenan also recommends seeing a dermatologist yearly for a skin check.
Finally, good lifestyle habits can go a long way to ensure healthy, beautiful skin. Weight management, a healthy diet, and trying to reduce stress have tremendous benefits with any chronic condition, Tehrani says. The better you take care of yourself, the less likely it is that flare-ups will occur.
Don’t Miss: Is Banana Good For Rheumatoid Arthritis
Methotrexate Instead Of Corticosteroid
In the case of rheumatoid arthritis, methotrexate is a drug that has been found to be able to prevent patients from having to take so much corticosteroid. Generally, the things a dermatologist does to treat the surface of the skin, such as applying sunscreens and corticosteroid-containing creams or ointments, does not help the more severe skin problems such as vasculitis that are seen in rheumatoid arthritis.
Rheumatoid Arthritis Facial Rash
Luckily, facial spider veins can be treated once the cause is identified. Our body is made up of numerous veins. The venous system has a complex network of tiny veins draining into larger veins. Determining the location and type of vein is extremely crucial to find appropriate treatment for spider veins. Anatomical location of Facial Veins. 1.
Also Check: What Helps Lower Back Arthritis
Ra Medication Side Effects And Skin
Certain medication used to treat RA can have negative side effects on the skin, as well. Nonsteroidal anti-inflammatory drugs and disease-modifying anti-rheumatic drugs are commonly prescribed to ease painful symptoms of the disease, but can sometimes cause skin rashes. This can be a sign of an allergic reaction to the medication, so speak to your doctor if your skin breaks out after starting a new drug.
Pain at the injection site and skin rashes also occur in less than 30 percent of people who use biologic response modifiers, or biologics genetically engineered proteins derived from human genes to treat RA symptoms. Biologics are injected beneath the skin, so itching, burning, and discoloration can occur at the injection site. Usually these side effects will go away on their own, but Dr. Keenan warns, if the reactions get larger with each injection, definitely contact your doctor.
Can Rheumatoid Arthritis Cause Skin Problems
Rheumatoidcanskin disordersproblemscauseandcanskinRArashesskin
RA rashes can appear on the skin as red, painful, and itchy patches. They may also be seen as deep red pinpricks. The most common site for a rash associated with RA is on the fingertips. In some advanced cases, a rash may form painful ulcers.
Also Know, how does rheumatoid arthritis affect normal movement? Because RA damages joints over time, it causes some disability. It can cause pain and movement problems. You may be less able to do your normal daily activities and tasks. RA can also affect many non-joint parts of the body, such as the lungs, heart, skin, nerves, muscles, blood vessels, and kidneys.
Likewise, does rheumatoid arthritis cause dry skin?
Rheumatoid arthritis is frustrating enough on its own. But about 15 percent of people with RA develop a complication that affects the tear and saliva glands, causing dry mouth, dry eyes, dry skin, and additional symptoms that further aggravate their arthritis.
Is there a link between eczema and arthritis?
And eczema, psoriasis, skin infections and rosacea have also been associated with RA. Why and how RA and these skin diseases are related is a subject of research. One study found that drugs that block tumor necrosis factor one of the inflammatory proteins that are elevated in people with RA may play a role.
Read Also: Is Banana Good For Rheumatoid Arthritis
Arthritis And Your Skin
Learn about the various ways having arthritis can affect the skin.
Arthritis is often referred to as an invisible disease because the inflammation and pain that affect the joints are often difficult to see. But some conditions that accompany different forms of arthritis may not be so invisible, because they affect our largest and most visible organ: our skin.
For example, a red or purplish rash across the cheeks and bridge of the nose often occurs in people with lupus, and the scaly skin of psoriasis is present in almost all people with psoriatic arthritis.
But bruises, bumps and lesions on the skin can occur along with many other forms of arthritis. They often signal an underlying problem caused by either the disease or the medications used to treat it that should not be ignored.
Here are several to watch for:
Increased Sun Sensitivity
Skin reddening or burning that occurs with sun exposure could simply be a sign that you should use more sunscreen or spend more time in the shade. But if you notice you burn more easily than you once did or you develop a rash or hives when you are in the sun, you are likely suffering from photosensitivity, says Jeffrey Weinberg, MD, associate clinical professor of dermatology at Mount Sinai School of Medicine in New York.
Cold, Discolored Fingers or Toes
Multiple Sores or Purple Spots
Unusual Bruising
Red or Purple Lines Under the Skin
A Wound That Doesnt Heal
Quick Links
Diabetes Skin Rashes Pictures
Superficial candidal skin infections appear as a red flat rash with sharp, scalloped edges. Smaller patches of similar-appearing rash, known as “satellite lesions” or “satellite pustules,” are usually nearby. These rashes may be hot, itchy, or painful. Intertrigo appears as softened red skin in body fold areas.
Also Check: What Helps Lower Back Arthritis
Lupus Erythematosus Nonspecific Disease
Lupus erythematosus-nonspecific disease can relate to SLE or another autoimmune disease, but nonspecific cutaneous features are most often associated with SLE.
Common cutaneous features seen include:
- this is an abnormal response to UV radiation that is present in 5093% of patients with SLE
- Mouth ulcers these are present in 2545% of patients with SLE
- Nonscarring hair loss in SLE presenting as coarse, dry hair with increased fragility .
Cutaneous vascular disease is also common. Forms of cutaneous vascular disease include:
- Raynaud phenomenon this presents with focalulceration in the fingertips and periungual areas that can cause pitted scarring, haemorrhage and other nail fold complications
- Vasculitis leukocytoclastic vasculitis: urticarial vasculitis presenting with tender papules and plaques over bony prominences and medium or large vessel vasculitis can occur, presenting with purpuric plaques with stellate borders, often with necrosis and ulceration or subcutaneous nodules
- Thromboembolic vasculopathies these may have a similar clinical presentation to vasculitis, but vessel occlusion is due to blood clots
- Livedo reticularis characterised by net-like blanching red-purple rings that commonly arise on the lower limbs
- Erythromelalgia characterised by burning pain in the feet and hands, and with macular erythema it is associated with heat exposure.
Vascular disease in lupus erythematosus
- Rheumatoid nodules.
Who Should Diagnose And Treat Ra
A doctor or a team of doctors who specialize in care of RA patients should diagnose and treat RA. This is especially important because the signs and symptoms of RA are not specific and can look like signs and symptoms of other inflammatory joint diseases. Doctors who specialize in arthritis are called rheumatologists, and they can make the correct diagnosis. To find a provider near you, visit the database of rheumatologistsexternal icon on the American College of Rheumatology website.
Don’t Miss: Is Banana Good For Rheumatoid Arthritis
Is It Ra And Eczema Or Is It Psoriatic Arthritis
The skin condition psoriasis can lead to psoriatic arthritis . RA and PsA symptoms are similar, which can make it difficult for doctors to tell the difference between the two conditions.
Also, they sometimes incorrectly diagnose psoriasis as eczema. As a consequence, some people receive a diagnosis of RA and eczema when they really have PsA, and vice versa.
A dermatologist can help determine whether a rash is due to eczema or psoriasis. Diagnosis often involves a blood test, and it sometimes involves a skin biopsy.
General guidelines from the American Academy of Dermatology to prevent itchy skin include:
- bathing in lukewarm, not hot, water
- limiting showers and baths to up to 10 minutes
- using fragrance-free soap, lotions, and laundry detergents
- wearing loose-fitting clothes made of cotton
- avoiding wool clothing, which can irritate the skin and cause itching
- avoiding extreme changes in temperature, when possible
- keeping the home relatively cool
- using a humidifier in winter, especially for people who are prone to eczema or have dry skin
- reducing stress whenever possible, as stress can make itchy skin worse
If a doctor determines that a medication is causing itching, they may recommend a different treatment.
For some people with RA, tofacitinib may help treat chronic itch. Tofacitinib is a Janus kinase inhibitor that doctors sometimes prescribe to treat RA or PsA.
Simple home remedies can help many cases of itchy skin. The AAD recommend the following tips: