Oral Microbiome Changes And Ra Risk
In the new study, researchers analyzed the oral microbiome and periodontal status of three groups of 50 people.
People in the first group had ERA, and the second group included people at risk of RA . People in the third group did not have RA and were not at risk, did not have autoimmune conditions, and were generally healthy.
Each participant was examined by a dentist to assess their periodontal condition. Dentists checked whether their gums bled with probing, the inflamed gum surface area, and how deep into the gum line dental tools could probe.
They also examined how many teeth each participant had, how many of their teeth were missing, decayed, or filled, and whether a person wore a removable denture. They also asked each participant about the last time they brushed their teeth and what their regular oral hygiene measures were.
In addition, the scientists collected from each participant samples of the tongue coating or film, saliva, and subgingival dental plaque, which is found below the gum.
After using devices to amplify the DNA present in the samples, they collected, analyzed, and quantified the microbial populations within the samples. They then compared microbial differences between the three groups.
The team identified no difference in periodontal conditions between the groups. There was also no difference in dental plaque samples.
According to the authors, these findings suggest that a possible link between the oral microbe and RA may truly exist.
Heart And Blood Vessels
People with RA are more prone to atherosclerosis, and risk of myocardial infarction and stroke is markedly increased.Other possible complications that may arise include: pericarditis, endocarditis, left ventricular failure, valvulitis and fibrosis. Many people with RA do not experience the same chest pain that others feel when they have angina or myocardial infarction. To reduce cardiovascular risk, it is crucial to maintain optimal control of the inflammation caused by RA , and to use exercise and medications appropriately to reduce other cardiovascular risk factors such as blood lipids and blood pressure. Doctors who treat people with RA should be sensitive to cardiovascular risk when prescribing anti-inflammatory medications, and may want to consider prescribing routine use of low doses of aspirin if the gastrointestinal effects are tolerable.
Gut Microbes Linked To Rheumatoid Arthritis
The presence of a specific type of gut bacteria correlates with rheumatoid arthritis in newly diagnosed, untreated people. The finding suggests a potential role for the bacteria in this autoimmune disease.
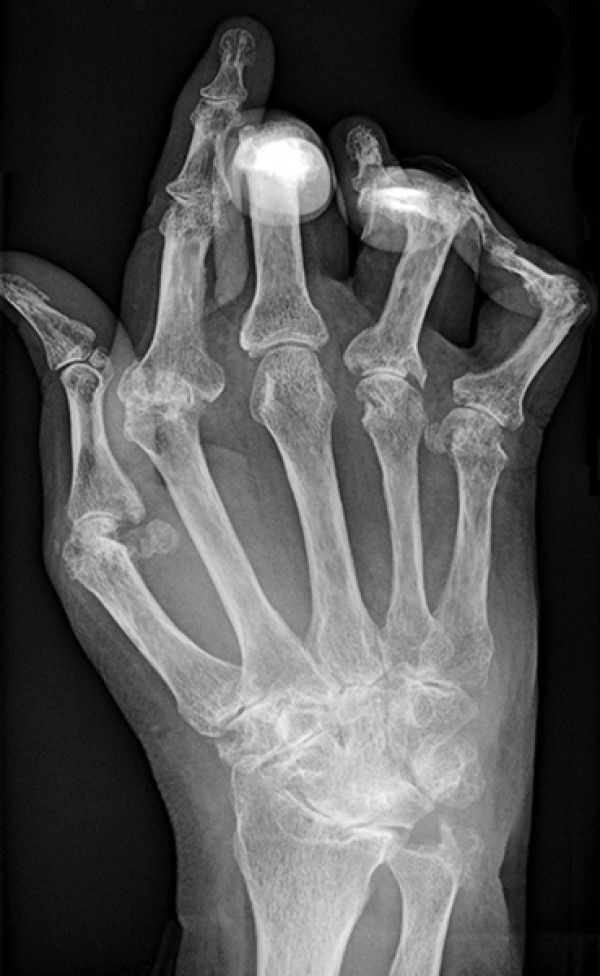
Rheumatoid arthritis is a chronic inflammatory disorder that can cause pain, swelling, stiffness, and loss of function in the finger, wrist, and other joints throughout the body. It occurs when the immune system mistakenly attacks the bodys own tissue, such as the membranes that line the joints.
The causes of rheumatoid arthritis arent completely known. Genes tied to the immune system may contribute. Environmental factors, such as cigarette smoking, diet and stress, may also play a role in triggering the disease. Treatments include medications to relieve pain and reduce inflammation.
The immune system is influenced by the microbiome, a network of microorganisms that live in and on the human body. These microbes outnumber the bodys cells by 10 to 1. Trillions of microbes both helpful and harmful reside in the digestive tract. The gut microbiome has been linked to arthritis in animal studies.
by Carol Torgan, Ph.D.
You May Like: How To Test For Arthritis In Knees
Can Intestinal Bacteria Cause Rheumatoid Arthritis
06 Apr 2016
Researchers worldwide are exploring the flawed immune response that kindles inflammatory disease. Intestinal bacteria may hold the key to understanding what triggers rheumatoid arthritis inflammation. Inflammation defends the body against infection, but must turn on at just the right moment to repel an assaultand then quickly switch off when the invading pathogen is removed. Why does smoldering low-grade inflammation suddenly erupt into a raging autoimmune disease that attacks the joints and sparks the warmth, swelling and pain of rheumatoid arthritis ?
One answer may lie in the microbiomeabout 100 trillion intestinal bacteria microbes weighing up to three poundsthat normally live in the gut. The microbiome shapes our immune system and can play an important role in autoimmune diseases, says Assistant Professor of Medicine Shahla Abdollahi-Roodsaz, PhD, of New York University School of Medicine. The microbiome in the gut activates immune cells that may travel throughout the entire body, including to the joints.
For 2015-16, Dr. Abdollahi-Roodsaz was awarded funding as The Sontag Foundation Fellow of the Arthritis National Research Foundation . An honor awarded by ANRFs partner organization, The Sontag Foundation, thats given towards the research project that they feel demonstrates the the most promise towards finding a cure for RA.
The Differences Between Infectious And Reactive Arthritis
Reactive arthritis occurs when the immune system overreacts to an infection, causing it to attack the joints. The organism that caused the original infectionusually a type of bacteriais not causing the joint symptoms. In fact, the person may be completely recovered from his or her illness and no longer have symptoms from the original infection.
You May Like: What To Do For Rheumatoid Arthritis In Hands
What Are The Symptoms Of Rheumatoid Arthritis
Symptoms include fever, joint pain, swollen joints, lack of flexibility in the joints, and morning stiffness or stiffness in joints.
For more information on arthritis, types of arthritis, symptoms and their causes, visit BYJUS.
Put your understanding of this concept to test by answering a few MCQs. Click Start Quiz to begin!
Select the correct answer and click on the Finish buttonCheck your score and answers at the end of the quiz
Investigating The Relationship Between High
The researchers analysed genetic and microbiome data of 1,650 TwinsUK participants with no history of RA, so that they could see if they could spot any early warning signs before the onset of symptoms.
The team calculated the twins genetic risk for RA and then looked at the gut bacteria identified from stool samples.
The team found that bacteria from a group named Prevotella were associated with high genetic risk of RA.
In addition, the researchers found bacteria from the same group were linked with early stages of RA when they analysed data from participants in another cohort study.
Don’t Miss: What Does Rheumatic Pain Feel Like
Eating For A Healthy Microbiome
It has been very challenging to modify the gut microbiome based on diet, says Davis. Ideally, through understanding the relationships between an individuals genetics and their own microbiome, healthcare providers might eventually be able to recommend individualized dietary guidelines that can improve RA. Additionally, adds Davis, we hope that prebiotics may foster a healthier microbiome constituency, or perhaps probiotics may be helpful in modulating the factors to improve the disease state.” Davis notes that a lot of work still needs to be done to support that hypothesis and to develop individualized RA treatment strategies based on factors related to the gut microbiome.
While definitive connections between the gut microbiome and RA have yet to be discovered, you can adopt a diet that promotes a balanced and diverse level of gut bacteria. Foods to eat include:
Several Explanations Can Be Proposed For These Conflicting Results
First, in the absence of a defined pathogen, the spectrum of microorganisms involved in triggering RA may include polymicrobial communities or the cumulative effect of several bacterial/viral factors. The simultaneous effects of various pathogens on the immune system in an RA patient may have different direct effects. It has been demonstrated that specific infections , hypothetically associated with the changes in the gut microbiome, could diminish or increase the risk of RA .
Second, the spectrum of bacteria and viruses, as well as the reaction of the immune system to such pathogens, with or without clinical manifestations of infection, may vary from preclinical to late-stage RA: such that any of numerous pathogens may trigger RA at a preclinical stage, but subsequently lose their influence in the advanced stage . Moreover, the delicate balance between pathogens and the anti-infection immune response of an RA patient may be disturbed by several factors including the limited mobility of the patients as well as the drug therapy selected.
Accordingly, two aspects of the problem of pathogens and RAversusRA and infections are still debated. Is there an acquired immune deficiency in RA patients caused by too frequent and prolonged infections, which break tolerance of self-antigens? Or, is there a congenital deficiency of the tolerance and inflammation control, which may occur even with ordinary infection frequency and duration?
You May Like: Arthritic Pain Symptoms
What Are The Causes Of Rheumatoid Arthritis
Our immune system releases antibodies when a foreign material like bacteria and fungus enters the body. Those antibodies fight the foreign material and kill them. However, in some cases, the immune system can mistakenly send antibodies to attack their own cells. This is the root cause of Rheumatoid Arthritis.
Mouth Bacteria May Trigger Ra
Studies highlight the role of microbes in rheumatoid arthritis and other inflammatory diseases.
A century ago, people believed that gum infections were the source of many inflammatory diseases, including appendicitis and rheumatoid arthritis . The treatment for so-called oral sepsis was total tooth extraction which rarely improved symptoms and was unpopular with patients and by the 1930s, the oral sepsis theory had largely been discredited.
Today, thinking has come full circle. In the last few years, a great deal of research, aided by DNA sequencing techniques, has shown germs that cause gum disease may contribute to many health problems, including RA and other inflammatory disorders. Gum disease also has been associated with other inflammatory forms of arthritis and rheumatic conditions, including psoriatic arthritis and lupus.
The Research
Collectively called the microbiota or microbiome, the trillions of bacteria that live on and in the human body are mostly beneficial and protective aiding digestion and guarding against pathogens and inflammation. But altering the makeup of complex microbial communities as happens in periodontal disease can trigger an immune response that targets the bodys own tissues.
How Mouth Bacteria Harm Joints
Future RA Prevention and Treatment
You May Like: Rheumatoid Arthritis Longterm Effects
Joint Pain From The Gut
Scientists don’t know what causes rheumatoid arthritis, but many suspect that the microbiomethe bacteria that live in our gastrointestinal tractsmay be to blame.
Doctors arent entirely sure what triggers rheumatoid arthritis, a disease in which the body turns on itself to attack the joints, but an emerging body of research is focusing on a potential culprit: the bacteria that live in our intestines.
Several recent studies have found intriguing links between gut microbes, rheumatoid arthritis, and other diseases in which the bodys immune system goes awry and attacks its own tissue.
A study published in 2013 by Jose Scher, a rheumatologist at New York University, found that people with rheumatoid arthritis were much more likely to have a bug called Prevotella copri in their intestines than people that did not have the disease. In another study published in October, Scher found that patients with psoriatic arthritis, another kind of autoimmune joint disease, had significantly lower levels of other types of intestinal bacteria.
This is frontier stuff, says Scher, the director of the NYUs Microbiome Center for Rheumatology and Autoimmunity. This is a shift in paradigm. By including the microbiome, weve added a new player to the game.
Gut Bacteria Can Cause Predict And Prevent Rheumatoid Arthritis

- Date:
- Mayo Clinic
- Summary:
- The bacteria in your gut do more than break down your food. They also can predict susceptibility to rheumatoid arthritis, suggests a new report.
The bacteria in your gut do more than break down your food. They also can predict susceptibility to rheumatoid arthritis, suggests Veena Taneja, Ph.D., an immunologist at Mayo Clinic’s Center for Individualized Medicine. Dr. Taneja recently published two studies — one in Genome Medicine and one in Arthritis and Rheumatology — connecting the dots between gut microbiota and rheumatoid arthritis.
More than 1.5 million Americans have rheumatoid arthritis, a disorder that causes painful swelling in the joints. Scientists have a limited understanding of the processes that trigger the disease. Dr. Taneja and her team identified intestinal bacteria as a possible cause their studies indicate that testing for specific microbiota in the gut can help physicians predict and prevent the onset of rheumatoid arthritis.
“These are exciting discoveries that we may be able to use to personalize treatment for patients,” Dr. Taneja says.
“Using genomic sequencing technology, we were able to pin down some gut microbes that were normally rare and of low abundance in healthy individuals, but expanded in patients with rheumatoid arthritis,” Dr. Taneja says.
Implications for predicting and preventing rheumatoid arthritis
Possibility for more effective treatment with fewer side effects
Story Source:
You May Like: How To Relieve Arthritis Pain In Fingers
Risk Factors For Rheumatoid Arthritis
It is important to note that while science is good at finding correlations, or apparent relationships, between factors and disease, correlation does not prove that the risk factor causes the disease. Many risk factors for RA have been identified and are being studied, but none have been pinpointed as the cause of RA.
Specific Strains Of Bacteria That May Affect Ra
Research has previously shown a link between RA and the bug Prevotella copri. A study published in the journal eLife found that the intestines of 75 percent of people with early, untreated rheumatoid arthritis had this bacterium in their intestines compared with 12 percent of people with chronic, treated rheumatoid arthritis. The theory is that this bacteria crowds out beneficial microbiota that fight inflammation or itself promotes inflammation.
Another study, published in April 2017 in Arthritis & Rheumatology, examined whether the overexpansion of Prevotella copri in the gut has the potential to affect immune cell functions, contributing to the development of RA. Study authors found that there is evidence for immune relevance of P. copri in RA. At this point, experts cant claim that P. copri causes RA, but the research provides an intriguing path for future study, according to an article published in November 2019 in the Journal of Clinical Medicine.
A different strain of the bacteria, Prevotella histicola, may actually decrease symptoms and disease progression, according to research done by Mayo Clinics Center for Individualized Medicine, published in April 2016 in Genome Medicine. Mice who were given the bacteria saw a delay in the disease and a reduction in the amount of cytokines in their system.
Don’t Miss: Getting Rid Of Arthritis
Bacteria In Milk And Beef Linked To Rheumatoid Arthritis
- Date:
- University of Central Florida
- Summary:
- A strain of bacteria commonly found in milk and beef may be a trigger for developing rheumatoid arthritis in people who are genetically at risk, according to a new study.
A strain of bacteria commonly found in milk and beef may be a trigger for developing rheumatoid arthritis in people who are genetically at risk, according to a new study from the University of Central Florida.
A team of UCF College of Medicine researchers has discovered a link between rheumatoid arthritis and Mycobacterium avium subspecies paratuberculosis, known as MAP, a bacteria found in about half the cows in the United States. The bacteria can be spread to humans through the consumption of infected milk, beef and produce fertilized by cow manure.
The UCF researchers are the first to report this connection between MAP and rheumatoid arthritis in a study published in the Frontiers in Cellular and Infection Microbiology journal this week. The study, funded in part by a $500,000 grant from the Florida Legislative, was a collaboration between Saleh Naser, UCF infectious disease specialist, Dr. Shazia Bég, rheumatologist at UCF’s physician practice, and Robert Sharp, a biomedical sciences doctoral candidate at the medical school.
“We believe that individuals born with this genetic mutation and who are later exposed to MAP through consuming contaminated milk or meat from infected cattle are at a higher risk of developing rheumatoid arthritis,” Naser said.
Map Mycobacterium Subspecies Linked To Rheumatoid Arthritis
People with rheumatoid arthritis were more likely to have mutations in a particular gene than healthy people, and they were more likely to have traces of Mycobacterium avium subspecies paratuberculosis bacteria, known as MAP, researchers have found.
MAP has previously been linked to other conditions related to immune function, including Crohns disease. The bacteria is common in cattle in the US and can be found in contaminated dairy or meat products from infected cows.
The researchers theorise that MAP bacteria may trigger rheumatoid arthritis in people who have genetic mutations. However, that doesnt mean MAP causes the disease. At this stage its just an association worthy of further study.
Read Also: Acute Arthritis Symptoms
Induction Of Arthritis By Infections In Animal Models
Animal studies can directly address the causal relationship between infection and RA in accordant to Kochs postulates, although there is no perfect animal model for human RA yet. Infections by P. gingivalis or mycoplasma induced or aggravated experimental arthritis in mice or rats . Interestingly, a very recent study showed that P. gingivalis facilitated the development and progression of destructive arthritis in CIA mice through its unique bacterial peptidylarginine deiminase . PPAD can lead to the generation of RA related citrullinated autoantigens by converting protein arginine residues to citrulline. This result suggests that P. gingivalis infection may play an important role in the loss of tolerance to citrullinated proteins in RA, implicating the causative link between infection and RA. In another study, experimental arthritis was strongly attenuated in the K/BxN mouse model under germ-free conditions, featured with reduced Th17 cells. Furthermore, introduction of segmented filamentous bacteria into GF mice reinstated the production of autoantibodies and arthritis symptoms . This study shows that a single commensal microbe can drive the autoimmune arthritis possibly via its ability to promote Th17 cells.
Which Natural Remedies Can Eliminate Pain And Discomfort
While treating the cause in order to eliminate the source and therefore curing rheumatoid arthritis, regular symptoms will probably persist or even worse.
The worsening may occur as a symptom of detox. Things get worse before they get better.
The following lists and briefly describes a few, but not all, of the available natural treatments for relief.
Turmeric tops the list as a superb anti-inflammatory. Though its vastly known for its uses in Asian and West Indian cuisine such as curry, it deserves to be even more well-known for its medicinal properties.
Turmeric has been used for ages to combat pain, which is mostly caused by inflammation.
Its most essential component, which attributes to its yellow and orange pigment, is curcumin.
Curcumin can be just as useful as ibuprofen drugs when it comes to alleviating pain.
Furthermore, as documented by V. P Menon and A. R. Sudheer, curcumin is such a powerful anti-inflammatory that it can even prevent cancers related to tumor growths. This is because tumors have a correlation with inflammation.
MSM stands for methylsulfonylmethane and is a sulfur compound also known as an organosulfur.
It is extracted from vegetable sources and has many uses. One of those uses is to help repair and reconnect damaged tissue.
MSM is essential for rheumatoid arthritis since rheumatoid arthritis includes painful joints due to inflammation and depletion.
Tart Cherry Juice contains anthocyanins, which give cherries their deep red and purplish tint.
You May Like: How To Slow Arthritis In Hands