What Causes Autoimmune Disease
This is a question that is often ignored by much of the medical community. The diagnosis of autoimmunity is given on a regular basis, but doctors often fail to discuss the root cause of these conditions. The traditional treatment for most autoimmune problems is to treat the symptoms with medications. For example, in painful inflammatory diseases like rheumatoid arthritis and lupus, doctors give medicines that suppress inflammation and the immune system. And although these medicines can be helpful in reducing symptoms, they do not resolve what causes autoimmune disease in the first place.
In the following special presentation, Dr. Osborne breaks down the known mechanisms and causes of AID.
According to the American Autoimmune Related Disorders Association
Common Autoimmune Disease Symptoms
Despite the varying types of autoimmune disease, many of them share similar symptoms. Common symptoms of autoimmune disease include:
- Fatigue
- Abdominal pain or digestive issues
- Recurring fever
- Swollen glands
Many women say its hard to get diagnosed, something that Orbai agrees with. Its not black or white, she says. Theres usually no single test to diagnose autoimmune disease. You have to have certain symptoms combined with specific blood markers and in some cases, even a tissue biopsy. Its not just one factor.
Diagnosis can also be difficult because these symptoms can come from other common conditions. Orbai says women should seek treatment when they notice new symptoms.
If youve been healthy and suddenly you feel fatigue or joint stiffness, dont downplay that, she says. Telling your doctor helps him or her to look closer at your symptoms and run tests to either identify or rule out autoimmune disease.
Autoimmune Disease: Why Is My Immune System Attacking Itself?
Autoimmune disease affects 23.5 million Americans, and nearly 80 percent of those are women. If you’re one of the millions of women affected by this group of diseases, which includes lupus, rheumatoid arthritis and thyroid disease, you may be wondering why your immune system is attacking itself.
Autoimmune Disease Risk Factors
Researchers dont know what causes autoimmune disease, but several theories point to an overactive immune system attacking the body after an infection or injury. We do know that certain risk factors increase the chances of developing autoimmune disorders, including:
- Genetics: Certain disorders such as lupus and multiple sclerosis tend to run in families. Having a relative with autoimmune disease increases your risk, but it doesnt mean you will develop a disease for certain, says Orbai.
- Weight: Being overweight or obese raises your risk of developing rheumatoid arthritis or psoriatic arthritis. This could be because more weight puts greater stress on the joints or because fat tissue makes substances that encourage inflammation.
- Smoking: Research has linked smoking to a number of autoimmune diseases, including lupus, rheumatoid arthritis, hyperthyroidism and MS.
- Certain medications: Certain blood pressure medications or antibiotics can trigger drug-induced lupus, which is often a more benign form of lupus, Orbai says. Our myositis center also discovered that specific medications used to lower cholesterol, called statins, can trigger statin-induced myopathy. Myopathy is a rare autoimmune disease that causes muscle weakness. Before starting or stopping any medications, however, make sure to talk to your doctor.
Recommended Reading: Ra Symptoms Hands
Who Gets Autoimmune Diseases
Doctors do not know exactly what causes autoimmune diseases, but some run in families, suggesting a genetic predisposition. Diet and environment may also impact whether or not an autoimmune condition expresses itself in ones lifetime. 23 Additionally, women are more likely to have autoimmune issues than men and comprise approximately 75% of cases in the US. 4
Most Common Autoimmune Diseases
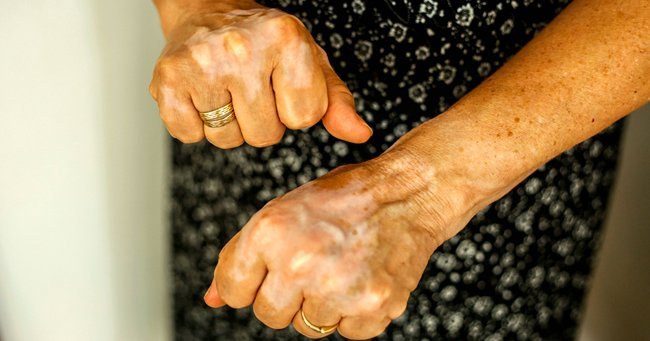
1. Rheumatoid Arthritis Rheumatoid arthritis is a chronic inflammation of the lining of the joints, leading to pain and swelling typically in the hands and feet. It can affect anyone, but is most prevalent in women over 40. Rheumatoid arthritis can sometimes affect other organs as well, such as skin, eyes, lungs and blood vessels. As with all autoimmune disorders, treatment focuses on managing pain and minimizing bone erosion and joint damage.
We have more in-depth information on Rheumatoid Arthritis here.
2. Juvenile Rheumatoid Arthritis Juvenile rheumatoid arthritis is the most common form of arthritis in children under 16. Symptoms usually include pain and swelling in the joints, and can vary from moderate to severe. In some cases, symptoms will subside over time while others can persist well into adulthood.
We have more in-depth information on juvenile rheumatoid arthritis here.
3. Systemic Lupus Erythematosus Lupus can be difficult to diagnose because it shares symptoms with many other disorders. The inflammation resulting from lupus can affect many different areas of the body, from the lungs, heart, joints, skin, kidneys, and brain. Like rheumatoid arthritis, lupus is more prevalent in women and can sometimes be identified by a butterfly-shaped rash on the face, along with photosensitivity, fatigue and fever, joint pain, and other skin lesions that worsen under sun exposure.
We have more in-depth information on lupus here.
Also Check: Vicks Vaporub For Joint Pain
What Does The Science Say About An Autoimmune Disease Diet Healthy Plant
Every autoimmune disease is different. Yet science is pointing to the power of plants to help alleviate symptoms and heal the body.
A 2014 research review in the journal Current Allergy and Asthma Reports found that the symptoms of many autoimmune diseases including fatigue in MS, pain and diarrhea in IBD, or the need of insulin in type one diabetes may be considerably affected by food choices.
A whole food, plant-based diet, in particular, can make a world of difference.
A 2001 study in the journal Rheumatology found that a vegan diet could significantly improve the signs and symptoms of rheumatoid arthritis .
One potential driver of RA is low levels of potassium. Multiple studies including this one in the Annals of the Rheumatic Disease have noted that patients with RA tend to have lower levels of potassium in their blood.
Another study in 2008 in the Journal of Pain found that increasing potassium intake could decrease pain levels in RA patients. Further research has suggested that may apply to other autoimmune conditions as well.
Where does potassium come from? The leading sources are plant foods, such as avocado, acorn squash, spinach, sweet potato, pomegranate, and bananas.
Whats An Autoimmune Disease
When you have an autoimmune disease, your immune system misidentifies healthy tissues and organs as being foreign. This causes the body to produce antibodies that attack your bodys own tissues.
Your symptoms might come on quickly or gradually. You may feel overwhelming fatigue, crippling pain, and debilitating weakness. Or you may feel dizzy and have brain fog.
You may feel miserable like youre on a roller coaster of good days and bad days with no end in sight. These diseases can be frustrating and isolating, but each experience is unique.
All autoimmune diseases share one common theme: an out-of-sync immune system that has turned inward, attacking parts of the body as if they were foreign invaders.
In fact, autoimmune diseases can show up in at least 80 different ways in all areas of the body.
But all autoimmune diseases share one common theme: an out-of-sync immune system that has turned inward, attacking parts of the body as if they were foreign invaders.
Your immune system is crucially important, serving the purpose of protecting your body from infections and bacteria. But when its functions are out of balance, your immune system can become dangerous.
Read Also: Rheumatoid Arthritis Burning Pain
Chronic Recurrent Multifocal Osteomyelitis
Chronic recurrent multifocal osteomyelitis is a disease affecting the bones. Inflammation is normally one of the bodys protective responses to infection or injury, but in diseases such as CRMO, uncontrolled inflammation can cause damage. In CRMO, inflammation targets the bone and can occur throughout the body.
What Is The Difference Between Osteoarthritis And Inflammatory Arthritis
The major distinction between OA and IA is that:
- Osteoarthritis is caused by physical use wear and tear of a joint over time .
- Inflammatory arthritis is a chronic autoimmune disease in which your immune system misidentifies your own body tissues as harmful germs or pathogens and attacks them. The result is inflammation of the affected tissues in and around joints.
Because OA involves physical wear on joints in the body, it usually appears in people after the age of 50. The older you get, the more likely you are to get osteoarthritis.
Since inflammatory arthritis is a chronic disease, it affects people of all ages, often striking people in their peak working and child-rearing age. IA diseases can often be diagnosed in patients as young as age 20 or 30. Less commonly, kids and teens may be diagnosed with a form of childhood arthritis, such as . IA is more common in females than in males, and it is not understood why.
You May Like: Can You Get Arthritis In Your Back
Add Some Spice To Your Life
Certain spices are particularly beneficial when it comes to minimizing inflammation and boosting your bodys healthy immune response.
Super-flavorful options include ginger, cayenne pepper, cloves, garlic, cinnamon, and turmeric.
Turmeric, in particular, is a powerful anti-inflammatory.
A 2007 study in Advances in Experimental Medicine and Biology noted that curcumin has been shown to help with multiple sclerosis, rheumatoid arthritis, psoriasis, and inflammatory bowel disease.
According to the Journal of Alternative Medicine Review: Curcumin supplementation can result in up to a 60% reduction in pain and a 73% reduction in joint stiffness.
How Are Autoimmune Diseases Diagnosed
Diagnosing an autoimmune disease usually takes healthcare providers longer than it does to diagnose other diseases. This is because many autoimmune diseases have similar symptoms with each other and with other diseases. You can help your healthcare provider with the diagnosing process by bringing the following to your appointment:
- A detailed list of any symptoms and how long youve had them.
- A record of your familys health history. Note if anyone in your family has an autoimmune disease.
In addition to interviewing you about your symptoms, your healthcare provider may do some blood tests to check for autoimmune diseases, including:
- Antinuclear antibody test .
Specific symptoms combined with specific blood markers may prove that you have an autoimmune disease.
Read Also: I Think I Have Rheumatoid Arthritis
Autoimmune Disease Types And Treatment
Simply put, autoimmune disease is associated with a malfunction of the immune system which causes the body to attack its own tissues. The body’s immune system is a complex network of specialized cells and organs that defends against foreign substances and invaders. The foreign substances and invaders can include bacteria, parasites, some cancer cells, and transplant tissue. Normally, the body’s immune system only reacts to foreign substances and invaders in order to protect the body. Normal antibodies are proteins produced by the immune system to target foreign invaders.
When the immune system malfunctions, the body mistakes its own tissues as foreign and it produces immune cells and autoantibodies that target and attack those tissues. The inappropriate response, which is referred to as an autoimmune reaction, can cause inflammation and tissue damage.
Ethical Issues Concerning Personalized Prevention
Obvious ethical concerns exist for any type of effort toward personalized prevention. One concern, valid for all studies, observational or interventional, relates to effects, psychological, and/or legal that may occur from notifying an individual that he/she is a high risk for acquiring a serious disease with as yet limited capacity for prevention. Another concern is the risk associated with testing of a drug with potential side-effects in individuals where development of future disease is substantially lower than 100%. The opportunity to prevent disease by modifying environment or lifestyle, addresses to some extent the first concern. The opportunity to treat symptoms, such as arthralgia and bone loss, that may exist in the âpre-RAâ phase with the same therapy as is aimed to prevent arthritis may address the second concern. The main argument, however, remains the wins that may follow from any successful prevention strategy that can be based on the science that requires the contribution from individuals at risk for disease.
Read Also: Joint Pain Medical Term
How Is Osteoarthritis Diagnosed
The physician will begin with a complete medical history and a physical examination. During the exam, the doctor will look for an enlarged or bumpy joint, signs of swelling, or decreased range of motion. Your doctor may then order x-rays, which can show a decrease in the cartilage space, new bone formation, or incorrect alignment. In some cases, your doctor may perform an aspiration the removal of fluid from a swollen joint or bursa to exclude infection, gout, or rheumatoid arthritis as possible causes of your joint pain.
What Is The Difference Between Rheumatoid Arthritis And Osteoarthritis
Rheumatoid arthritis and osteoarthritis both cause joint pain, stiffness, and limited range of motion, but the two diseases are distinct in their root cause and treatment.
Rheumatoid arthritis is an autoimmune condition where a persons own immune system attacks their joints, causing inflammation. Rheumatoid arthritis typically affects many joints simultaneously, especially in the hands, wrists, and feet, and is treated with medications to suppress the immune response.
Osteoarthritis is not an autoimmune disease, and although the exact causes are not known, multiple risk factors have been identified. In a healthy joint, cartilage provides cushioning and a smooth joint surface for motion. In an osteoarthritic joint, as cartilage is irreversibly destroyed and bone abnormalities develop, movement becomes painful and more difficult.
Read Also: Autoimmune Leg Pain
Three Common Autoimmune Diseases
There are many recognised autoimmune diseases and a growing list of illnesses not traditionally thought to be linked to the immune system, such as schizophrenia and narcolepsy, are now being recognised as having autoimmune components.
Heres how three common autoimmune diseases work.
Approximately 10% to 15% diabetics have the autoimmune form of the disease, known as type 1 diabetes.
Formerly known as insulin-dependent or juvenile diabetes, this illness is caused when the immune system attacks the beta cells in the pancreas. The pancreas is a gland located behind the stomach and beta cells normally produce insulin .
Insulin regulates levels of sugar in the body, ensuring you store and break it down properly. In the absence of insulin, the body starts to use fat as a substitute energy source, leading to a build-up of dangerous chemicals in the body which can cause a potentially fatal condition known as ketoacidosis.
Type 1 diabetes is generally treated using insulin injections and by monitoring blood sugar levels.
Multiple sclerosis affects the nervous system. Nerve cells in the brain and spinal cord communicate signals throughout the body and are wrapped in a protective cover called myelin that allows these signals to travel quickly.
The number of autoimmune diseases is growing as we discover more and more illnesses have an underlying autoimmune component. Current therapies mainly aim to replace a lost function in patients, or to broadly block inflammation.
Diagnosis Of Oa And Ra
The causes, symptoms, and treatment methods differ for OA and RA, so its important that we determine the type of arthritis a patient has in order for us to develop an effective treatment plan.
How Osteoarthritis is Diagnosed
Osteoarthritis is generally diagnosed through a series of tests, along with a physical examination and an assessment of past medical history.
Common tests used to diagnose OA include:
- Ultrasound to evaluate the ligaments and tendons around the affected joint
- Analysis of synovial fluid to determine whether degeneration is present
- Closed synovial biopsy to remove a piece of synovial tissue and assess its condition
- Arthroscopy examination of the joints through a small camera
- Arthrocentesis examination to remove joint fluid and assess its condition
How Rheumatoid Arthritis is Diagnosed
Rheumatoid arthritis is generally diagnosed through a series of tests, including physical examinations, blood tests, and x-rays.
If our rheumatology doctor, Dr. Maria Farooq, suspects rheumatoid arthritis, she will assess the affected joints to determine whether they are swollen, red, or warm, as these signs are indicative of RA. This physical exam may be followed by any of the following tests:
Also Check: Side Effects Of Arthritis Medicine
What Are The Treatments
Medicine and lifestyle changes can often control symptoms and slow these diseases.
Medication. Many drugs can now treat RA and other autoimmune disorders. Some are used for pain relief. Others target inflammation. Early treatment with drugs like these may be the best way to prevent joint damage. See your doctor to talk about your options.
Lifestyle choices. While you canât change your genes, you can sometimes change how you live. That can help your treatment work better.
Even if you donât have an autoimmune disease, but you think you might be at risk, these steps may help lower your chances.
Researchers Find One Autoimmune Disease Could Lead To Another
Researchers at the University of Colorado Anschutz Medical Campus have discovered that having one kind of autoimmune disease can lead to another.
The scientists serendipitously found that mice with antibody-induced rheumatoid arthritis in their joints went on to develop spinal lesions similar to those in axial spondyloarthritis which causes fusion of the vertebrate and curvature, or bending, of the backbone.
The study was published today in the journal Immune Network.
“Our results suggest that one autoimmune disease, such as inflammatory arthritis, may also lead to a secondary autoimmune disease such as AxSpA,” said the study’s lead author Nirmal Banda, Ph.D., professor in the division of rheumatology at the University of Colorado School of Medicine. “This interesting disease association may be due to the binding of anti-collagen autoantibodies to the spine, or to some alteration of the immune system that requires further investigation.”
These same anti-collagen antibodies are also present in humans with arthritis. They directly attack joint cartilage resulting in inflammation and pain.
Banda noted that every mouse injected with collagen antibody-induced arthritis developed arthritis and then curvature of the spine consistent with axial spondyloarthritis.
The connection, he said, has not been made in any other study he’s seen.
“I believe we are the first to make this link,” he said.
“I want to know what the mechanism is,” he said.
Read Also: Arthritis Triggers