Psoriatic Arthritis Vs Rheumatoid Arthritis
Because psoriatic arthritis impacts the skin as well as the joints, its sometimes referred to as a double whammy, or like rheumatoid arthritis but with a nasty skin rash, according to the arthritis advocacy group Creaky Joints.
Both psoriatic and rheumatoid arthritis are autoimmune disorders that cause joint inflammation, pain, and stiffness, as well as chronic fatigue. But there are differences in how the diseases develop and affect the joints.
According to Kathleen Maksimowicz-Mckinnon, DO, a rheumatologist at Henry Ford Hospital in Detroit, there are some telltale signs that your arthritis pain is due to psoriatic arthritis, and not rheumatoid arthritis. These include:
RELATED: Signs and Symptoms of Psoriatic Arthritis
Which Doctor Is Best At Diagnosing Psoriatic Arthritis
Normally, a dermatologist would be the first stop for diagnosis and treatment of psoriasis which is the skin condition that often triggers psoriatic arthritis. But arthritis falls within the area of expertise of the rheumatologist. He would be more competent in assessing the extent of damage suffered by joints, and he will customize a treatment plan tailored to individual patients.
Summary Plaque Psoriasis Vs Psoriasis
Psoriasis is a chronic multisystem disease with skin and joint manifestations. Plaque psoriasis is the commonest form of psoriasis which is characterized by the appearance of reddish well-demarcated plaques with silver scales usually on the extensor surface of the knees and elbows. Accordingly plaque psoriasis is one manifestation of the broad spectrum of dermatological and systemic manifestations which are identified as psoriasis. This can be identified as the difference between plaque psoriasis and psoriasis.
Dont Miss: Why Is Psoriasis Medicine So Expensive
Don’t Miss: Does Arthritis Hurt To The Touch
Things To Know About Psoriatic Arthritis
Learn more about what it means to have psoriatic arthritis.
1. PsA Is an Autoimmune Disease
2. It Has Ups and Downs, Called Flares
3. It Can Be a Master of Disguise
4. It Has Distinguishing Features
5. It Affects Up to a Third of People with Psoriasis
6. Its Gender Neutral
7. It May be Hereditary
8. Its Not Contagious
9. It Isnt Just About Your Joints
10. You May Not Look Sick
11. Effective Treatment is Available
Quick Links
The Majority Of People With Psoriasis Wont Develop Psoriatic Arthritis
About 7 million Americans have psoriasis, and only a fraction of them will ever develop psoriatic arthritis, according to the Cleveland Clinic. Estimates vary depending on the source, but the Centers for Disease Control and Prevention says that roughly 10% to 20% of people with psoriasis go on to develop psoriatic arthritis.
In contrast, the Cleveland Clinic estimates that up to 30% of people with psoriasis will develop psoriatic arthritis. That said, having psoriasis is the single most significant risk factor for developing psoriatic arthritis, Naomi Schlesinger, M.D., chief of the Division of Rheumatology at Rutgers Robert Wood Johnson Medical School, tells SELF.
If you have psoriasis, its extremely important to watch for any joint symptoms, such as swelling, pain, or stiffnessthe most common signs of psoriatic arthritisand report them to your physician, says David Giangreco, M.D., a rheumatologist at Northwestern Medicine Delnor Hospital. Psoriatic arthritis is a progressive disease, meaning it can get worse over time. And if you happen to get diagnosed with psoriatic arthritis in its early stages, then your doctor can prescribe treatments that slow the diseases progression and help preserve your joints.
Also Check: How To Get Rid Of Arthritis In Fingers
What Psoriasis Patients Can Do About Combating Stress
Theres no smoke without fire in the same way, theres no stress without a trigger. It could be a person, a thing, or an event. If you watch the bodys stress response, youll notice that breathing becomes rougher, palms of hands become sweaty, neck and shoulder muscles tense up, and there is a feeling of being tired and overwhelmed.
Once youve identified the trigger, minimize contact with it. If that doesnt work, try opening up to a spouse, relative, or family friend. You gain a third person perspective that may pave the way to a solution.
Involve yourself in mind and body relaxation techniques such as meditation, controlled breathing, Yoga or Taichi. It helps to remain active to take your mind off the problem and get the body to heal itself.
What Is Difference Between Psoriasis And Psoriatic Arthritis
24.08.2020.
How is it different than eczema? · Eczema is much more commonly found in children · It is rare for someone to have both eczema as a child and.
Facts about Psoriatic Arthritis 1. Psoriatic arthritis is a type of arthritis that occurs along with psoriasis in an estimated 10-30 percent of cases. Psoriasis is a skin condition that causes patches of skin to become red and scaly. 2. Psoriatic arthritis usually develops after skin symptoms, but it is possible for symptoms of arthritis to.
01.06.2020.
in the treatment of psoriasis and psoriatic arthritis .
The RESPOND study, an open-label comparison of MTX and infliximab,
Psoriatic Arthritis Vs. Rheumatoid Arthritis: How the 2 Conditions Differ, According to Experts Heres what you need to know about the similarities and differences between these two rheumatic.
is a good amount of overlap. Video: Psoriatic Arthritis Vs. Rheumatoid Arthritis: How the.
However, distinct immunopathogenic, phenotypic and genetic differences exist between these two.
for Research and Assessment of Psoriasis and Psoriatic Arthritis has been instrumental in.
Under this hypothesis, psoriasis without arthritis was not a risk factor.
that professionals in the field may have different opinions.
The exact relationship between psoriatic arthritis and.
s site is chock-full of information about psoriasis and psoriatic arthritis. You can request a free electronic psoriatic arthritis.
01.05.2013.
Read Also: Best Cure For Psoriasis On Hands
Don’t Miss: What Does Rheumatic Pain Feel Like
What Are The Risks Of Biosimilars
The risks and side effects of biosimilars are the same as those associated with their biologic reference product. Anyone considering taking a biosimilar should talk with their health care provider about the short- and long-term side effects and risks. It is important to weigh the risks against the benefits.
Biologics and biosimilars act on cytokines, which are specific proteins released by the immune system that can cause inflammation. Biologics suppress the function of the overactive immune system. When on a biologic or biosimilar, you may have a higher risk of infection. If you develop any signs of an infection, contact your health care provider right away.
Signs of infection include:
- Damp, sticky feeling or sweating
- Fever
Biologic Treatments For Psoriatic Arthritis
Biologic medications are specifically designed to mimic chemicals that are naturally found within the human body, and act to correct something that is going wrong.
A number of biologic treatments are available to treat psoriatic arthritis. There are various criteria for when biologic treatments can be prescribed to treat psoriatic arthritis, and for some treatments the criteria may vary if you are in Scotland compared to England or Wales. Please check the information on each individual biologic treatment for more information about when it can be prescribed.
As with the traditional systemic DMARDs, people taking biologic treatments will have regular blood tests and other checks, to monitor for side effects. As biologic treatments suppress the immune system, it is recommended that people taking them have an annual flu vaccination, as well as a pneumococcal vaccination before you start biologic treatment. Not all vaccinations, however, are safe to have when taking a biologic treatment, so you should always check with your Rheumatologist or another healthcare professional before having them.
Also Check: Tomatoes Bad For Arthritis
You May Like: Rheumatoid Arthritis One Side Of Body
How Are Psoriasis And Psoriatic Arthritis Connected
You may have heard that psoriatic arthritis and psoriasis are connected, but might not understand how. Although the conditions share a similar name, they can have some very different symptoms and treatments. People with psoriasis are at a greater risk of developing psoriatic arthritis, and sometimes people with psoriatic arthritis develop psoriasis later on, meaning its helpful to have an understanding of both conditions if you are diagnosed with one, according to the Mayo Clinic.
Untangling the nuances between these two conditions can be a bit complicated. Thats why we spoke with experts about the important things you should know about psoriatic arthritis and psoriasis, including how the two are linked.
What Should You Do If You Develop Another Type Of Psoriasis
Life-threatening signs and symptoms, such as redness that covers most of your body, fever, and chills, require immediate medical care.
When signs and symptoms are not life threatening, you should see a board-certified dermatologist for a diagnosis. Youll find pictures of the different types of psoriasis and learn more about the possible signs and symptoms at Psoriasis: Signs and symptoms
ImagesImage 1: Getty ImagesImage 2: J Am Acad Dermatol 2013 69:245-52.
ReferencesBrummer GC, Hawkes JE, et al. Ustekinumab-induced remission of recalcitrant guttate psoriasis: A case series. JAAD Case Rep. 2017 3: 4325.
Egeberg A, Thyssen JP, et al. Prognosis after hospitalization for erythroderma. Acta Derm Venereol. 2016 96:959-92.
Gottlieb A, Korman NJ, et al. “Guidelines of care for the management of psoriasis and psoriatic arthritis: Section 2. Psoriatic arthritis: Overview and guidelines of care for treatment with an emphasis on the biologics. J Am Acad Dermatol 2008 58:851-64.
Gudjonsson JE and Elder JT. Psoriasis. In: Wolff K, Goldsmith LA, et al. Fitzpatricks Dermatology in General Medicine. McGraw Hill Medical, New York, 2008:178-81.
Khosravi H, Siegel MP, et al. Treatment of Inverse/Intertriginous Psoriasis: Updated Guidelines from the Medical Board of the National Psoriasis Foundation. J Drugs Dermatol. 2017 16:760-6.
Navrotski BRF, Nihi FM, et al. Wet wrap dressings as a rescue therapy option for erythrodermic psoriasis. An Bras Dermatol. 2018 93:598-600.
Read Also: Can You Stop Arthritis In Fingers
Treatment For Gout Vs Psoriatic Arthritis
If you have both PsA and gout, you will need to treat both conditions. There are separate medications to treat PsA and gout. In general, PsA is treated with medication that suppresses your immune system while gout requires treatment with medications that lower uric acid in the blood and controls gout flares, says Dr. Singh.
For gout patients: The goal of gout treatment is to first reduce the inflammation causing flare-ups by using such medications as nonsteroidal anti-inflammatory drugs , corticosteroids , and oral colchicine. Once an acute gout flare is under control, your doctor may prescribe medication to control your uric acid levels, including xanthine oxidase inhibitors , uricosuric agents, and enzymes that break down uric acid.
If there is suspicion that a patient has both gout and PsA, sometimes treating the more acute symptoms of gout first allows for more clear assessment of other arthritis involvement, and the need for additional treatment for psoriatic arthritis, says Dr. Kohler.
For psoriatic arthritis patients: There are many drugs available to treat PsA. The ones your health care provider recommends will depend on your most troublesome PsA symptoms. Treatments and medications for psoriatic arthritis include:
Because both gout and PsA have risk factors related to your lifestyle and diet, patients with PsA and gout can benefit from adopting healthy habits, including:
What Are The Risks
Some of the more common side effects with these biologics include upper respiratory infections, reactions at the injection site, and headaches. Depending on the biologic, you might also experience a rash or urinary tract infection, cold symptoms, diarrhea, abdominal pain, or fatigue.
The risks of using these drugs are mainly thought to revolve around an increased risk of mild to serious infections, including tuberculosis and some fungal infections, Margolies says.
Anyone taking biologics will undergo monitoring, which usually means an annual blood count and liver tests, but biologics arent appropriate for all patients. Individuals with active infections or a significantly compromised immune system should not take biologics. Patients with heart failure or multiple sclerosis , or with a first-degree relative with MS, should not take the TNF inhibitors, but can take secukinumab or ustekinumab.
More serious but very rare side effects can also occur, including nervous system disorders, heart failure, blood disorders, or a syndrome similar to lupus. Infliximab and golimumab carry a very low risk of causing liver damage, and infliximab, golimumab, and ustekinumab have been linked to a small increased risk of cancer. A relapse of hepatitis B may occur with some biologics, too.
Also Check: What Helps Lower Back Arthritis
Recommended Reading: Arthritis Pain In Hands Relief
Spondylitis With Or Without Sacroiliitis
This occurs in approximately 5% of patients with psoriatic arthritis and has a male predominance.
Clinical evidence of spondylitis and/or sacroiliitis can occur in conjunction with other subgroups of psoriatic arthritis.
Spondylitis may occur without radiologic evidence of sacroiliitis, which frequently tends to be asymmetrical, or sacroiliitis may appear radiologically without the classic symptoms of morning stiffness in the lower back. Thus, the correlation between the symptoms and radiologic signs of sacroiliitis can be poor.
Vertebral involvement differs from that observed in ankylosing spondylitis. Vertebrae are affected asymmetrically, and the atlantoaxial joint may be involved with erosion of the odontoid and subluxation . Therapy may limit subluxation-associated disability.
Unusual radiologic features may be present, such as nonmarginal asymmetrical syndesmophytes , paravertebral ossification, and, less commonly, vertebral fusion with disk calcification.
Things To Consider When Taking A Biologic
Biologics are a type of medication that can be prescribed for some forms of inflammatory arthritis .
This sheet gives you general information about how biologics work, why they are used, as well as tips on the safe use of these medications.
This resource does not provide advice about the specific biologic you may be prescribed to manage your arthritis. It does not cover all the side effects and safety precautions that can occur with each biologic. You should discuss this with your doctor, rheumatology nurse or pharmacist, or see the For more information section at the end of this resource.
Also Check: Are Peanuts Bad For Arthritis
Psoriasis And Joint Pain
As a chronic autoimmune disorder, psoriasis can impact skin, joints and nails, and symptoms can vary from intermittent to chronic and from mild to debilitating. Symptoms develop as the immune system attacks the body, rather than protecting it from foreign intruders, which leads to inflammation. On the skin, this can manifest as sensitive, red patches and flaky skin.
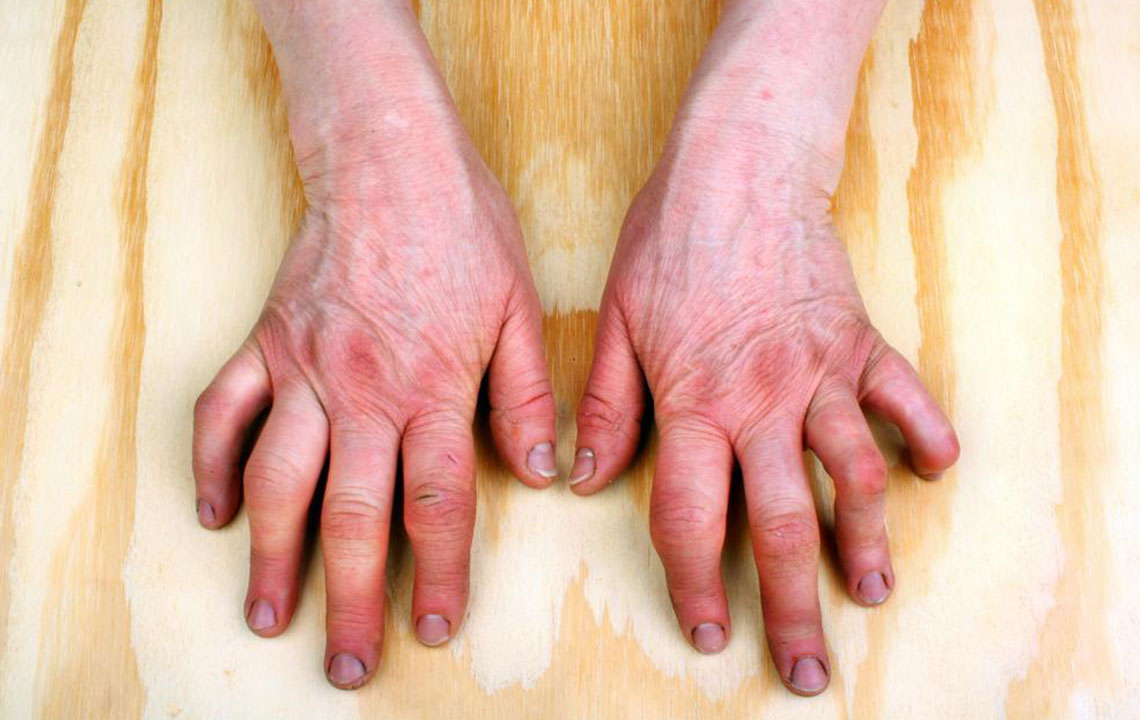
Although both psoriasis and psoriatic arthritis can cause joint pain, stiffness and swelling, the signs of psoriatic arthritis often resemble those of rheumatoid arthritis. Common psoriatic arthritis symptoms include:
- Swollen fingers and toes which is often a precursor to significant joint symptoms
- Foot pain, particularly at the back of your heel or in the sole of your foot
- Lower back pain called spondylitis which causes inflammation of the joints between your spinal vertebrae and in the joints between your pelvis and spine.
There are several different types of psoriatic arthritis that are identified based on how symptoms are affecting your body. For example, symmetric psoriatic arthritis affects both sides of the body whereas asymmetric psoriatic arthritis only affects one side of the body. There are other types of psoriatic arthritis that are diagnosed based on the location of your inflammation.
You Can Develop Psoriatic Arthritisanytimebefore Or After Your Psoriasis Diagnosis
Medical experts used to believe that people with psoriasis could only develop psoriatic arthritis within 10 years of their initial psoriasis diagnosis, according to the Cleveland Clinic. However, studies have shown that this isnt true. In fact, up to 15% of people with both diseases actually experienced their psoriatic arthritis symptoms first, according to the Cleveland Clinic. Some people may develop psoriatic arthritis before psoriasis, and others may have had psoriasis for years without realizing it, according to Dr. Giangreco. Psoriasis can remain hidden from patients on the back of the scalp or buttock area and go unnoticed for long periods of time, Dr. Giangreco tells SELF. If you have psoriatic arthritis and suddenly notice changes in your skin and nails, then you dont want to rule out the possibility of psoriasis. Rarely do people have psoriatic arthritis without getting psoriasis, too, according to the U.S. National Library of Medicine.
Read Also: How To Reduce Joint Swelling In Fingers
What Are The Symptoms Of Ra
Many of the symptoms of RA mirror those of PsA. Which is why oftentimes, the presence of psoriasis is a distinguishing factor in what type of arthritis you might be diagnosed with. Flare-ups are also common during RA where the symptoms wax and wane. You might experience time periods of minimal symptoms and times when symptoms flare-up. In both RA and PsA, it is important to try to pinpoint what causes flare-ups. If you can determine underlying factors of the flare-ups , you might be able to minimize the presence of these symptoms. As with PsA, the following are RA symptoms that you may or may not have. You might only experience one or two of these symptoms or you might experience more.
Some of the more common symptoms of RA include:
- Joint stiffness
What Can Prevent Someone From Getting A Second Type Of Psoriasis
Most types of psoriasis cannot be prevented.
That said, if you already have plaque psoriasis, it may be possible to reduce your risk of developing another type of psoriasis on your skin. Dermatologists recommend taking the following precautions:
-
Protect your skin to prevent sunburn
-
Take medication as directed and speak with your dermatologist before stopping a medication
-
Treat your psoriasis so that its well-controlled
-
Watch your weight so that you stay at a weight thats recommended for your age and height
Watching your weight may help prevent inverse psoriasis. This type of psoriasis is more common in people who are 20 or more pounds overweight.
You May Like: How To Slow Arthritis In Hands
Symptoms Of Ra And Psa
Both RA and PsA cause joint swelling, stiffness, and pain. Although both conditions affect joints in the fingers and toes, they do it in slightly different ways. And each one can cause other symptoms, too.
Rheumatoid arthritis:
- Often starts in the smaller joints, like the ones in your fingers and toes over time, it may affect other joints, too, like your wrists, knees, hips, and ankles.
- Usually shows up on the same joints on both sides of your body that means it’s symmetric.
- Often makes joints feel stiffer in the morning
- Can lead to fatigue, low-grade fever, and weight loss
Psoriatic arthritis:
- Can affect joints in the back and pelvis in addition to the ones in fingers and toes
- Often affects only one side of your body that means it’s asymmetric.
- Sometimes causes foot pain, especially on the sole of your foot or the back of your heel
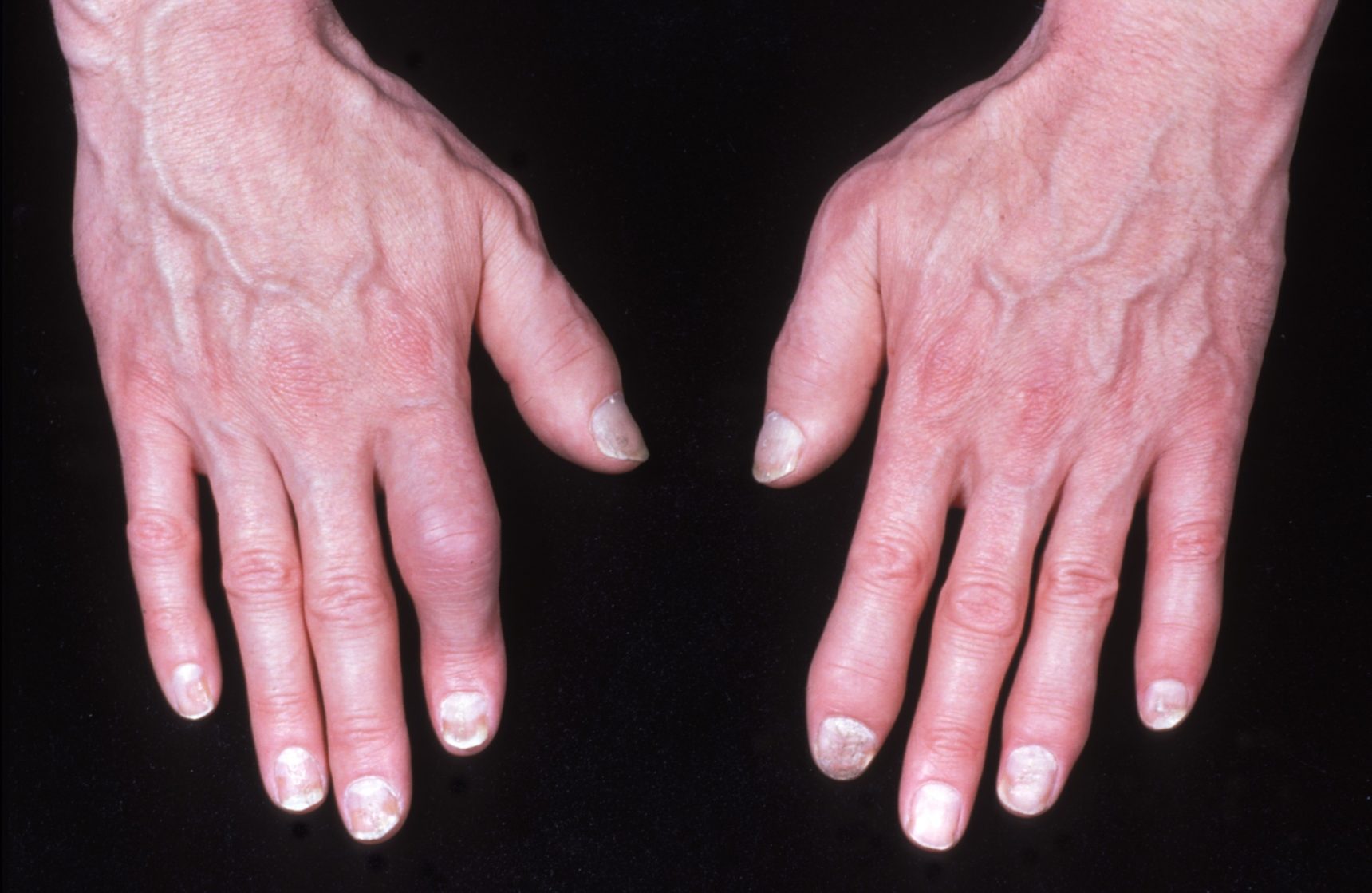
- May make your fingers swell up like sausages
- May make your nails pit and flake
- Tends to affect entheses, areas where tendons or ligaments attach to bones
With both conditions, you’ll probably have times when your symptoms get worse. These are called flares. In between these flares are times without symptoms called remissions.