Heart Disease Often Missed In Rheumatoid Arthritis
People with rheumatoid arthritis are at high risk of heart attack, atrial fibrillation, heart failure, and stroke. Heres what you need to know.
Everyday Health
People who have rheumatoid arthritis are roughly twice as likely as the general population to experience heart failureand 50 percent more likely to have a heart attack, according to the Cleveland Clinic in Ohio. But despite this increased risk, people living with RA are screened for heart disease far less than other high-risk patients.
In a recent review, Nature Reviews Rheumatology, the authors call for improvements in CVD preventive care in patients with RA. According to the lead author, Anne Grete Semb, MD, PhD, a senior researcher at the Leader Preventive Cardio-Rheumatology Clinic at Diakonhjemmet Hospitaal in Oslo, catching risk factors early is particularly important in people with RA to prevent a fatal cardiac event.
Keep A Check On The Progression Of Your Disease
RA is a progressive, degenerative disease which over the years can cause severe damage to your various vital organs, including lungs. To prevent the acute damage that RA can cause, it is important to keep a close check on the progression of the disease. So, watch out for all the signs of rheumatoid arthritis and immediately get in touch with your primary care physician if you experience persistent cough, shortness of breath, fever or any other health complication.
Eat A Mediterranean Diet
No specific diets have been proven to help fight inflammatory arthritis, but theres one eating style worth latching on to. People read about anti-inflammatory diets, says Dr. Gulati. Theyre really describing the Mediterranean diet.
A study of almost 33,000 women found that the more Mediterranean their eating habits were less red meat and more fruits, vegetables, whole grains, fish, legumes, and healthy fats the lower their risk of heart attack, stroke, and heart failure. Focus on replacing saturated fats with heart-healthy unsaturated fats, and eating plenty of fruits, vegetables, and fiber, suggests Dr. Gulati.
You May Like: How To Cure Arthritis Naturally
Recognizing And Diagnosing Costochondritis
X-rays dont show soft tissue well and theres not a blood test for it, so costochondritis is typically diagnosed by a doctor through a physical exam. Older adults experiencing these symptoms may need to get an EKG to rule out the possibility of cardiac problems.
RELATED: Mystery Symptoms That Could Be Rheumatoid Arthritis
According to Costochondritis, StatPearls medical education book published in January 2021, The most important part of the diagnosis of costochondritis is ensuring other, more deadly causes of chest pain have been ruled out. These can include acute coronary syndrome, pneumothorax, pneumonia, aortic dissection, pulmonary embolism, or an esophageal perforation.
How Do Cardiovascular Diseases Develop In The Case Of Gout
Gout or gouty arthritis is another type of arthritis characterized by the deposition of crystallized uric acid in the joints. The joints swell as a result of this.
Uric acid is found to be associated with various cardiovascular diseases such as hypertension, coronary artery disease, and preeclampsia among others.
High uric acid level along with these health conditions may develop due to factors such as high sugar intake, low birth weight which leads to obesity or genetic traits.
You May Like: Does Hot Tub Help Rheumatoid Arthritis
Arthritis & Heart Disease
Why People With Arthritis Are at Greater Risk for Heart Disease
Youre probably all too aware of how arthritis affects your joints. But the unfair news is that having arthritis osteoarthritis , but especially inflammatory conditions like rheumatoid arthritis , gout, lupus and psoriatic arthritis puts you at increased risk of developing heart disease. That includes heart attack, stroke, atrial fibrillation , high blood pressure, heart failure and atherosclerosis .
People with RA tend to be at highest risk. More than 50 percent of premature deaths in people with rheumatoid arthritis result from cardiovascular disease, according to a 2011 review of 24 mortality studies published in Nature Reviews Rheumatology.
People with gout also have a higher risk of heart attack and death from cardiovascular and coronary heart disease. High uric acid levels a cause gout have been linked to a 44% increased risk of high blood pressure, according to a 2011 review published in Arthritis Care & Research.
As for people with OA, a study of 8,000 people in Finland, published in the Annals of Rheumatic Diseases, found that men with OA in even a single finger joint were 42% more likely to die of cardiovascular disease than those who didnt have OA. Women were at a 26% higher risk than those without the disease. The link may be excess weight.
So, why the double whammy of increased heart disease risk when you have arthritis?
Chronic Inflammation
Lifestyle Factors
Medications
How Can Your Doctor Help
Your doctor may measure your blood pressure or take some blood tests to check your blood glucose or cholesterol levels. Often these are performed in the morning after an overnight fast. You may be prescribed medication to help you reduce your risk of heart disease. Some medications, such as those which can help control cholesterol , have several additional health benefits. Other medications, such as beta-blockers, are helpful for blood pressure but can cause worsening of psoriasis. If a new medication seems to be affecting you in an adverse way, please consult your doctor immediately.Some medications for the treatment of psoriasis can cause high blood pressure or change the levels of triglycerides/cholesterol . If your dermatologist is considering these medications, he or she will check your blood pressure and take blood tests regularly.
Recommended Reading: How To Treat Arthritis In Your Back
Chronic Inflammation Of The Muscle Of The Heart
Chronic inflammation, regardless of its source, is a risk factor for the development of heart disease. Research shows people who suffer from inflammatory conditions are more likely to have cardiac events.
Your risk for heart disease or heart failure is doubled with RA, especially if you have a rheumatoid factor , this according to some 2013 study out of the Mayo Clinic, Rochester, Minnesota, USA. A rheumatoid factor is an antibody measure in the blood doctors use to diagnose RA.
One report in the Journal of Internal Medicine finds people with RA can have heart problems as early as the first year following diagnosis. So, it is clear that getting RA under control as soon as possible and addressing any additional risks is vital to preventing cardiovascular damage.
The Joints Are The Primary Jia Target
JIA kicks off a faulty immune response that causes the release of inflammatory chemicals that attack the synovia, which is the tissue that lines the joints and produces lubricating fluid, says. Dr. Oller. is the equivalent to grease or WD-40 that you put on hinges to make sure everything is moving smoothly and effectively. But with JIA, the inflamed synovia can cause joints to painfully swell and become stiff.
Recommended Reading: What Tests Diagnose Rheumatoid Arthritis
Atrial Fibrillation Link Also Seen
A population-based study in Denmark also found that patients with RA had about a 40 percent increased risk of atrial fibrillation over people who didnt have the disease. In this first study that focuses on AF risk, researchers extend the possible risk factors the inflammatory arthritic disease causes.
Dr. Husni says more studies and increased awareness in the medical community are essential to improve outcomes for patients with inflammatory arthritis.
Traditional risk score calculations can underestimate CV risk in our patients, she says. These patients have not been traditionally included in the large prospective clinical trials for primary cardiac prevention, making it difficult to extrapolate cardiac risk management in the general population to patients with RA, lupus and psoriatic arthritis.
Osteoarthritis And Your Heart
Having OA may increase your risk for cardiovascular disease. Heres what you can do to protect your heart.
Although joint damage, pain, and swelling are the hallmarks of osteoarthritis , joints arent the only part of the body this disease can affect. Research also shows that the heart may be at risk in people with degenerative joint disease.
People with OA are almost three times more likely to develop cardiovascular disease or heart failure than those without OA, studies show. The link is especially strong when arthritis is in certain joints, such as the knee and hip.
But just because you have OA doesnt mean you cant improve your heart health.
Whats Behind the OA-Heart Disease Link?
Inflammation
Although OA is not traditionally considered an inflammatory disease, research is beginning to show that OA does involve inflammation. And long-term inflammation contributes to CVD.
Aging
Growing older makes you more likely to develop both diseases. Aging thickens and stiffens the arteries, which can lead to high blood pressure and heart damage. Joints degenerate from years of use and repeated small injuries. Unfortunately, age isnt reversible, but you can address the preventable risk factors below.
Too little exercise
Obesity
Obesity can lead to both OA and CVD. Carrying excess body weight puts stress on both the joints and heart, which can cause damage over time. Fat cells also produce inflammatory chemicals that are harmful to joints, the heart, and blood vessels.
Stay active
Also Check: What Are The Five Worst Foods For Arthritis
The Ticket To A Healthier Ticker
In general, the more severe your RA, the greater your chance of developing heart problems. To protect your heart, its important to get inflammation under control. And the sooner you can do this the better, because the risk of having a heart attack goes up within the first year after being diagnosed with RA. Work with your doctor to find the treatment thats most effective for you.
To further reduce your risk of heart problems, stay physically active, eat a balanced diet, maintain a healthy weight, and dont smoke. Ask your doctor or a for suggestions on making lifestyle changes successfully.
, unhealthy cholesterol levels, and only add to your risk of developing heart disease. If you need medication to treat any of these conditions, be sure to take it as directed.
The Cardiac Risks Of Rheumatoid Arthritis
As if the chronic pain and mobility challenges of rheumatoid arthritis werent burdensome enough, its becoming clearer that people with the disease face another serious health threata greater risk for heart disease.
Some 1.5 million Americans, a majority of them women, have this form of arthritis, an autoimmune disease that happens when the immune system attacks the bodys own tissues, causing pain, swelling, stiffness and loss of function in the joints.
Doctors have long known that people with rheumatoid arthritis and related conditions had a shorter lifespan than those without these conditions. Data suggest that heart disease may explain this discrepancy. In fact a review of studies in the journal Nature Reviews Rheumatology suggests that more than 50 percent of premature deaths in patients with rheumatoid arthritis result from cardiovascular conditions.
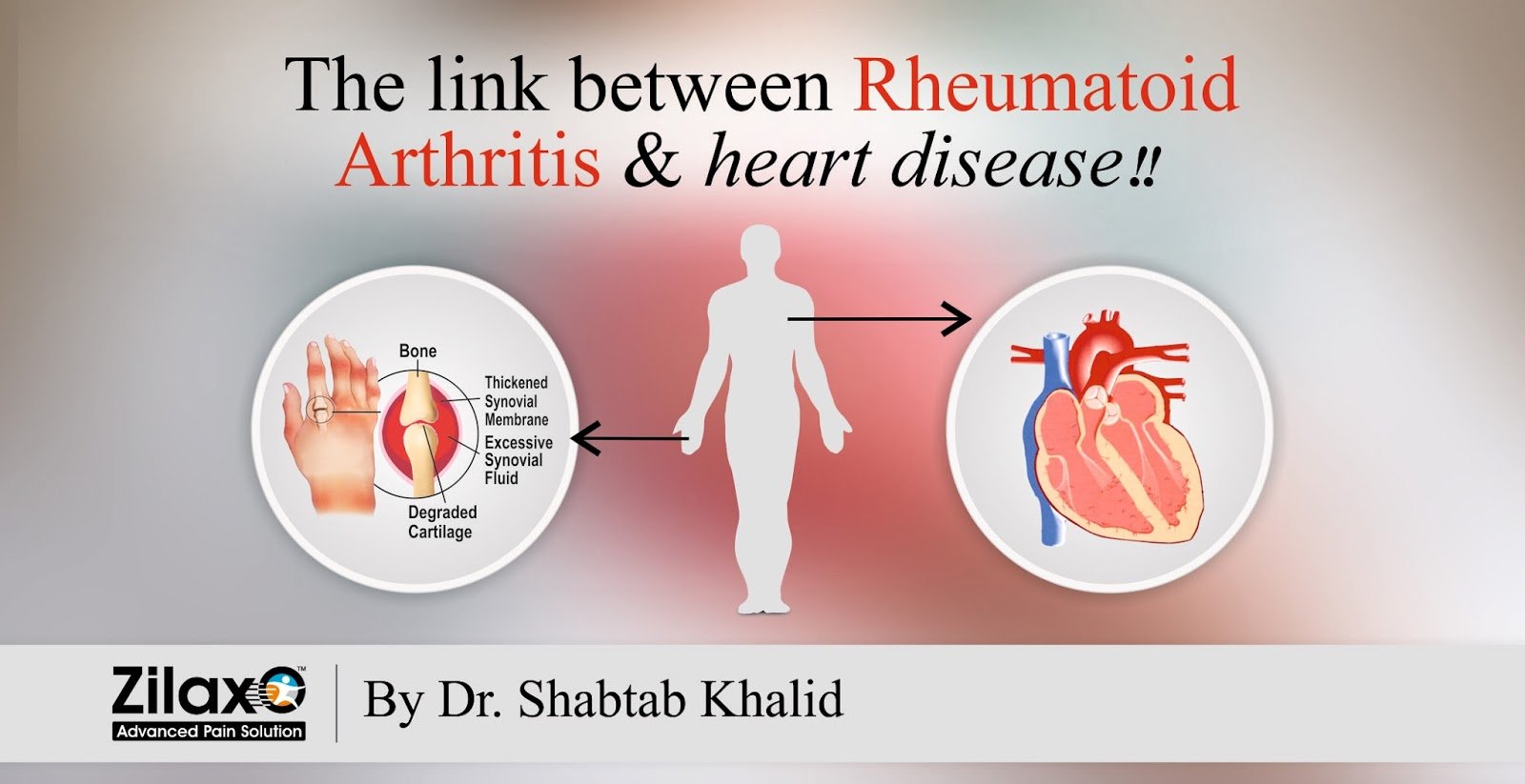
The link between the two diseases: inflammation. In people with rheumatoid arthritis, the immune system attacks the synoviumthe lining of the membranes around the joints. This causes the synovium to thicken, eventually damaging the cartilage and bone.
But the process doesnt stop at the joints. The inflammation can damage systems throughout the body, including the skin, eyes, lungs, and heart. Inflammation narrows the arteries, raising blood pressure and reducing blood flow to the heart, for instance.
You May Like: How To Beat Rheumatoid Arthritis Naturally
From The Lab To The Cardio
Translating research into clinical practice is paramount at Mayo Clinic. To that end, the divisions of cardiovascular diseases and rheumatology have joined forces to change the clinical approach to rheumatic conditions.
The Cardio-Rheumatology Clinic at Mayo Clinic opened in Rochester in the summer of 2013. The clinic provides specialized care focused on early detection, prevention and treatment of cardiovascular disease in patients with rheumatic conditions.
“We saw the need for a team of specialists that understand the unique risks and circumstances of people with rheumatoid arthritis, so we created this special clinic just for those patients,” explains Mayo Clinic cardiologist Rekha Mankad, M.D., who directs the Cardio-Rheumatology Clinic in Rochester.
Dr. Gabriel concurs. “Because they don’t necessarily show cardiovascular symptoms the same way as other people, and because they take medication that other people aren’t on and have poorer outcomes when they develop heart disease, they need more specialized care,” she says.
The Cardio-Rheumatology Clinic enables early referral of patients with rheumatic diseases to cardiology. Patients have both a traditional cardiovascular risk assessment and a vascular health assessment. The results help create an individualized plan to manage risks and symptoms.
“We’ve come full circle,” Dr. Gabriel notes. “Careful clinical observation led to research that now informs and changes clinical practice, making things better for patients.”
How Does Rheumatoid Arthritis Affect The Heart And Lungs
When your RA flares up, the membrane surrounding your heart can also become inflamed. And the worse your RA is, the worse your flares will be, and this means a higher chance your heart is inflamed.
The inflammation around your heart is called pericarditis. With time, all that inflammation causes the heart membrane to get thick and tight, making it harder for your heart to do its job.
Rheumatoid nodules on your heart are also a real possibility. These firm lumps are a complication of RA and affect the way the heart works.
Irregular Heartbeat
People with RA have an increased risk of atrial fibrillation , a condition that causes irregular heartbeats. And AFib is also linked to strokes.
According to one Danish study, adults with RA are 40 percent more likely to have AFib, and they are also 30 percent more likely to have a stroke.
Congestive Heart Failure
A study reported in 2005 from researchers at the Mayo Clinic found RA patients had twice the risk for congestive heart failure. The risk was higher for RA patients who were RF-positive, and in all RA patients, the increased risk was there even in the absence of other cardiovascular risk factors.
A second Mayo Clinic study, this one reported in 2008, found when heart failure presented itself in RA patients, patients had no evidence of signs or symptoms, this compared to people without RA. Death with the first year following heart failure with RA is also higher.
Rheumatoid Arthritis and Cholesterol Levels
Breathing Problems
You May Like: What Are The Five Worst Foods To Eat For Arthritis
General Signs And Symptoms Of Arthritis
Symptoms as related to direct causes vary. The type of arthritis is directly related to the pattern and location of arthritic symptoms.
The general signs and symptoms associated with all variations of arthritis include:
- Joint pain, swelling and stiffness
- Joint tenderness and inflammation
- Redness of the skin surround affected joints
- Loss of hand grip or grip strength
These symptoms may be at the worst first thing in the morning. Symptoms may develop suddenly or over a period of time . Symptoms can also occur in flares and as damage worsens, may begin to persist for longer periods.
Pain in the joints can fluctuate in varying degrees or be constant. It may be isolated to one specific area of the body or in multiple parts, depending on the number of affected joints. Stiffness is more often a problem first thing in the morning once awake, but can also be problematic after sitting for long periods of time, and even after exercise.
As some types of arthritis are closely associated with other types of conditions, a range of related symptoms over and above those which affect the joints can be experienced as well. Types of symptoms in this regard include fatigue, fever, swollen lymph nodes, weight loss, general malaise, as well as a range of others showing problems with the heart, lungs and kidneys.
Severe Ra Doubles The Risk Of Heart Disease
Researchers discovered that the burden RA puts on the joints during the first year of diagnosis is a strong predictor of heart disease. Doctors who diagnose patients with RA should use this time to address potential heart risks in the future, Matteson said.
Another study examined the relationship between RA and cytomegalovirus , a type of herpes virus that typically goes unnoticed in healthy people. Mayo researchers found that a relationship between the two exists, and that CMV, too, affects the heart.
The virus puts patients at a greater risk for myocardial disease, a type of heart disease in which the heart muscle becomes progressively weaker. The relationship should prompt doctors to check for biomarkers of CMV in RA patients to assess their risk of heart problems, Dr. Matteson, a co-author on that study, said.
This is something that is not well-recognized, he added.
A third study from Mayo researchers shows that psoriasis and psoriatic arthritis patients are also at a higher risk of developing heart disease, but not to the same extent as those with RA, Matteson said.
Again, we think its related to inflammation, he said.
You May Like: How Long Can You Take Aleve For Arthritis
How Do I Know If My Ra Is Progressing
Signs Your RA Is Progressing
The Lungs And Heart May Be Affected
Research published in Rheumatology International has found that JIA can interfere with how well the heart pumps blood, particularly through the left ventricle. This can lead to high blood pressure and breathing problems. Along with inflammation of the pericardium patients may also have long-term changes of inflammation and irritation in the lungs and pleura , says Dr. Oller. This over time can lead to lung disease.
You May Like: How Do You Treat Arthritis Pain
Arthritis In The Heel And Ankle
Several types of arthritis, including OA, RA, AS, and PsA, can affect the heels and the ankles.
Symptoms of arthritis in the heel might include:
- Stiffness upon awakening in the morning
- Recurring pain in the heel
- Swelling of the heel
- Limited movement
- Skin changes, including rashes and growths
Inflammation at the heel from RA, AS, or PsA can lead to conditions that cause heel pain. This might include Achilles tendonitis, plantar fasciitis, or retrocalcaneal bursitis, a condition in which the bursa becomes inflamed, causing pain and swelling.
The ankle is not affected by arthritis as often as other joints, but it can be a source of severe pain and instability when it is affected. Additional symptoms of ankle arthritis include swelling and stiffness of the ankle and problems with mobility. Ankle arthritis will eventually affect gaitthe way a person walks.