What Is Psoriatic Arthritis In Children
Psoriatic arthritis is a rare form of arthritis or joint inflammation that affects both skin and joints. Psoriasis is an ongoing condition that causes a red, scaly, itchy rash. It also causes nails to become thick and pitted with tiny holes.
Psoriatic arthritis causes painful joint pain and swelling, along with skin rashes. It most often affects finger and toe joints. But it can also affect wrists, knees, ankles, and the lower back.
This condition is most common in adults ages 30 to 50. But it can start in childhood. In many cases, the skin disease starts before the arthritis.
Early diagnosis and treatment helps to ease pain and prevent joint damage from getting worse.
Early Stages Of Psoriatic Arthritis
Recognizing the signs of psoriatic arthritis can be tricky since symptoms differ from patient to patient. For example, one person can experience psoriasis skin involvement and peripheral arthritis, another may experience axial disease , and someone else could have a combination of all three.
Whats more, especially during early disease, you may confuse your symptoms with other conditions. People can mistake enthesitis, inflammation of the entheses for tennis elbow or dactylitis for an infection, explains Dr. Mikulik.
If you have psoriasis and are having pain in your tendon and musculature and you think maybe Ive been too active lately, that may be the first sign of PsA, says Dr. Haberman. Doctors commonly hear people chalk up their symptoms to overuse, such as getting more exercise than usual or doing work around the house.
If you experience any of the following signs of early psoriatic arthritis its important to see your doctor as soon as possible:
- Changes in your fingernails or toenails, including holes, pitting, discoloration, or softness
- Eye inflammation
- Sausage-like swelling of an entire finger or toe
- Scalp psoriasis
- Tendon or ligament pain at the Achilles tendon, bottom of the foot , or elbow
Key Points About Psoriatic Arthritis
- Psoriatic arthritis is a form of arthritis with a skin rash.
- Psoriasis is a chronic skin and nail disease. It causes red, scaly rashes and thick, pitted fingernails. The rash may come before or after the arthritis symptoms.
- Psoriatic arthritis causes inflamed, swollen, and painful joints. It happens most often in the fingers and toes. It can lead to deformed joints.
- Treatment may include medicines, heat and cold, splints, exercise, physical therapy, and surgery.
Also Check: What Essential Oil Is Good For Arthritis In The Hands
Limited Mobility Or Range Of Motion
For men and women who develop arthritis in their knees, activities that were once simple, easy, or routine may become difficult or even impossible to do without limitations and discomfort. Walking, running, or getting in and out of a car can, oftentimes, prove disproportionately challenging for patients with arthritis of the knee. The damage and loss of cartilage associated with arthritis are usually to blame for this phenomenon.
Dont Miss: Eggs Bad For Arthritis
Psoriatic Arthritis Vs Rheumatoid Arthritis
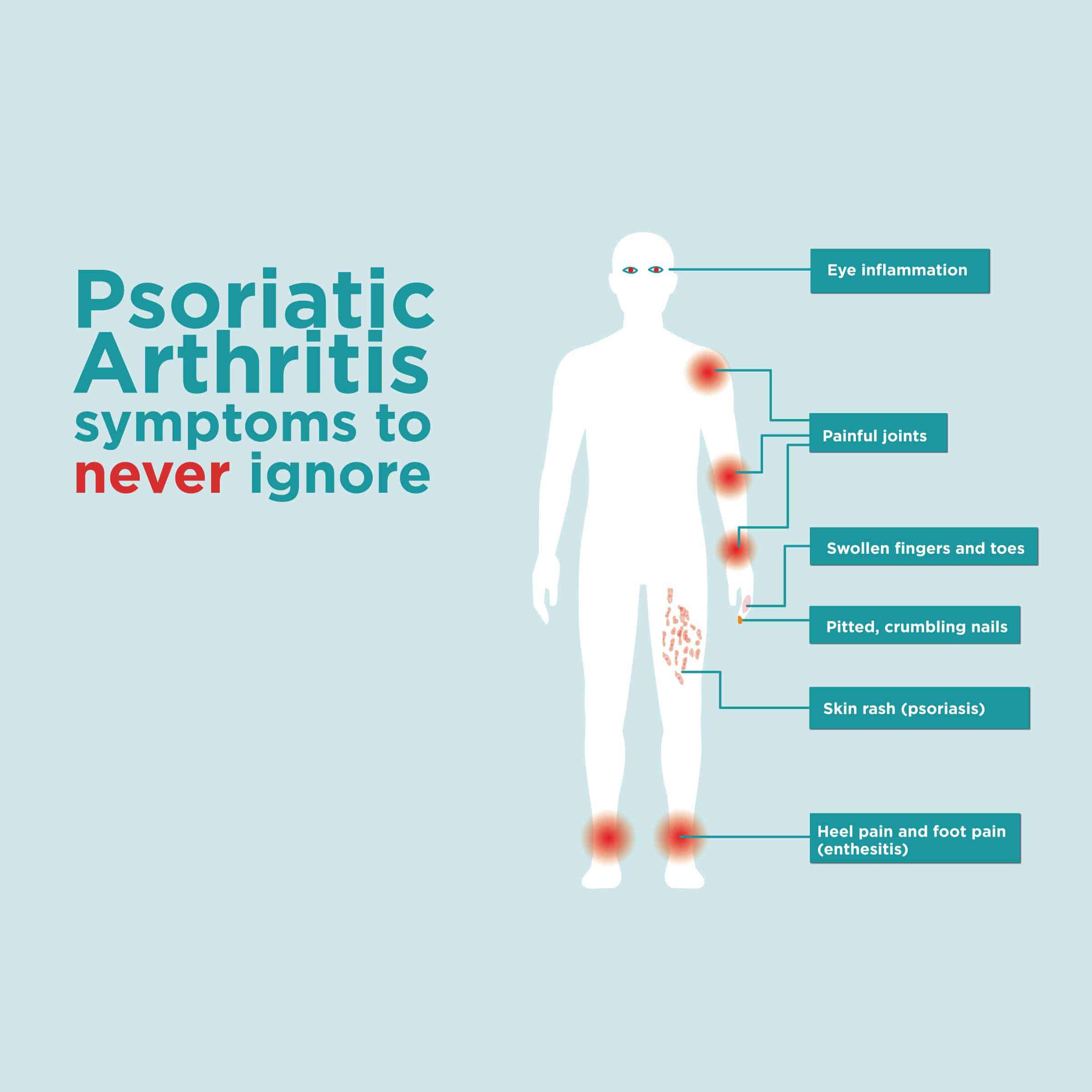
Because psoriatic arthritis impacts the skin as well as the joints, its sometimes referred to as a double whammy, or like rheumatoid arthritis but with a nasty skin rash, according to the arthritis advocacy group Creaky Joints.
Both psoriatic and rheumatoid arthritis are autoimmune disorders that cause joint inflammation, pain, and stiffness, as well as chronic fatigue. But there are differences in how the diseases develop and affect the joints.
According to Kathleen Maksimowicz-Mckinnon, DO, a rheumatologist at Henry Ford Hospital in Detroit, there are some telltale signs that your arthritis pain is due to psoriatic arthritis, and not rheumatoid arthritis. These include:
RELATED: Signs and Symptoms of Psoriatic Arthritis
Recommended Reading: Does Rheumatoid Arthritis Affect The Back
Swollen Joints Fingers And Toes
Often you’ll notice swelling in your knees, ankles, feet, and hands. Usually, a few joints are inflamed at a time. They get painful and puffy, and sometimes hot and red. When your fingers or toes are affected, they might take on a sausage shape. Psoriatic arthritis might affect pairs of joints on both sides of your body, like both of your knees, ankles, hips, and elbows.
Symptoms And Family History
40 percent of people with psoriasis or PsA had a family member with either psoriasis or PsA.
In the study, those with a family history of PsA had a higher risk for developing deformities from PsA, but a lower risk for developing plaque psoriasis, the red, scaly skin patches that are a common symptom of psoriasis.
Researchers are only now beginning to decipher the specific genes associated with PsA. The main challenge is distinguishing genes responsible for psoriasis from those responsible for PsA.
Identifying the genes that lead to PsA may pave the way toward developing gene therapy for treating PsA.
Also Check: What Does Arthritis Do To Your Bones
Treatment For Psoriatic Arthritis
Treatment for psoriatic arthritis aims to:
- relieve symptoms
- slow the condition’s progression
- improve quality of life
This usually involves trying a number of different medicines, some of which can also treat the psoriasis. If possible, you should take 1 medicine to treat both your psoriasis and psoriatic arthritis.
The main medicines used to treat psoriatic arthritis are:
- non-steroidal anti-inflammatory drugs
- biological therapies
How Are Ra And Psa Diagnosed
Because these two conditions share similar symptoms, itâs important to get an accurate diagnosis from a rheumatologist. A rheumatoid factor blood test is one way your doctor can tell which condition you have. RF is a protein found in people with rheumatoid arthritis. People with PsA usually donât have it. Blood tests looking for other antibodies such as anti-CCP can also help differentiate the two.
Another way to tell is to look at your skin and nails. If you have scaly patches on your skin, pitting and flaking on your nails, or both, you have PsA.
Once youâve had the disease for a while, X-rays might also be able to distinguish the two conditions.
It is possible to have RA and PsA together, but itâs rare. If you do have both, many of the treatments, including some medications, will work for both conditions.
Donât Miss: Can You Stop Arthritis In Fingers
You May Like: What Foods Not To Eat If You Have Rheumatoid Arthritis
What Are The Types Of Psoriatic Arthritis
There are different types of psoriatic arthritis, which tend to affect different parts of the body. These include:
- asymmetric arthritis usually affects one side of the body, or different joints on each side
- symmetrical polyarthritis often affects several joints on both sides of the body
- distal interphalangeal arthritis affects the joints closest to the fingernails and toenails
- spondylitis affects the spine, particularly the lower back
- arthritis mutilans a rare condition that severely affects the bones in the hands
There is also a type of psoriatic arthritis that affects children, although the symptoms are usually mild.
Early Symptoms Of Psoriatic Arthritis
Here are some common first signs of PsA. If you experience any of these, talk to your primary care provider. Early detection and treatment of the disease can help prevent future joint damage.
Recommended Reading: How Does Methotrexate Work For Rheumatoid Arthritis
Your Energy Level Is Like A Bank Account
Psoriatic arthritis can cause extreme fatigue. For every task you complete, or plan to complete, you drain your daily energy bank. Putting on mascara or talking to a neighbor on the street costs you energy. And sometimes, even if its the first thing you do after waking up, a shower may be all it takes to put you right back in bed.
Its important to rest when you need to and not push yourself too hard, especially on days when your symptoms are particularly severe, says Joseph Markenson, MD, a rheumatologist at Hospital for Special Surgery in New York City. Its also important for the loved ones of those who have psoriatic arthritis to understand how draining the condition can be for example, people who have psoriatic arthritis may have to cancel plans frequently or head home early and be sympathetic and patient.
Other New Treatment Options For Psa

Some other potential treatments for PsA include the following:
- Light therapy: This may be a safe and inexpensive treatment option to improve skin symptoms. UVB is a type of UV light that reduces psoriasis-inducing cytokines and promotes the production of vitamin D, which is an important vitamin in treating autoimmune conditions.
- Weight management: This may play a key role in managing and treating PsA. A 2018 systematic review suggests that people with obesity had a
There is no one-size-fits-all approach for treating PsA.
Current guidelines from the American College of Rheumatology and the National Psoriasis Foundation advise the use of TNF inhibitors, such as infliximab or adalimumab, as the first-line treatment for PsA.
They suggest that people whose conditions do not respond to their first TNF inhibitor should try another TNF inhibitor rather than using IL-17 or IL-23 inhibitors, such as guselkumab or ixekizumab.
Factors such as a persons preference for oral medication and the location and severity of their symptoms may influence which treatment is best for them. Oral small-molecule medications, such as methotrexate, may be the best treatment option for those who experience frequent infections during treatment with TNF inhibitors or those who have a strong preference for oral treatment.
Although these are the current guidelines, the best treatment option will depend on a persons specific situation.
Don’t Miss: What Is The Best Surgery For Thumb Arthritis
A Good Day Doesnt Mean Youre Better
Many people who live with psoriatic arthritis have good days and bad days. Although good days dont mean youre healed, its important to work with your doctor to find ways to have more good days than bad. Tracking your symptoms and their impact on your life, as well as your ability to participate in everyday activities, may help your healthcare provider identify new ways to help you, says Markenson, including potential lifestyle changes and additional treatments.
Rheumatoid Arthritis And Psoriatic Arthritis: The Similarities And Differences
All forms of arthritis involve tenderness and swelling of the joints. And, at first glance, psoriatic arthritis can be very hard to differentiate from other common types of arthritis, including rheumatoid arthritis and osteoarthritis.
Because psoriatic arthritis symptoms can overlap with those of rheumatoid arthritis and osteoarthritis not just swollen, achy joints but also stiffness and chronic fatigue diagnosing this autoimmune disease can be tricky.
Unlike rheumatoid arthritis, there is no blood test that can determine if a person has psoriatic arthritis, says M. Elaine Husni, MD, MPH, a rheumatologist at the Cleveland Clinic in Ohio.
Psoriatic arthritis can also affect the body in different ways depending on the person and how advanced the disease is, says Dr. Husni. As a result, a rheumatologist may need to examine a patient several times and run a number of tests before having enough information to make a definitive diagnosis.
Recommended Reading: What Can You Take To Relieve Arthritis Pain
Who Will Be Responsible For My Healthcare
Youre likely to see a team of healthcare professionals.
Your doctor, usually a rheumatologist, will be responsible for your overall care. And a specialist nurse may help monitor your condition and treatments. A skin specialist called a dermatologist may be responsible for the treatment of your psoriasis.
You may also see:
- A physiotherapist, who can advise on exercises to help maintain your mobility.
- An occupational therapist, who can help you protect your joints, for example, by using splints for the wrist or knee braces. You may be advised to change the way you do some tasks to reduce the strain on your joints.
- A podiatrist, who can assess your footcare needs and offer advice onspecial insoles and good supportive footwear.
What Are The Symptoms Of Ra
Many of the symptoms of RA mirror those of PsA. Which is why oftentimes, the presence of psoriasis is a distinguishing factor in what type of arthritis you might be diagnosed with. Flare-ups are also common during RA where the symptoms wax and wane. You might experience time periods of minimal symptoms and times when symptoms flare-up. In both RA and PsA, it is important to try to pinpoint what causes flare-ups. If you can determine underlying factors of the flare-ups , you might be able to minimize the presence of these symptoms. As with PsA, the following are RA symptoms that you may or may not have. You might only experience one or two of these symptoms or you might experience more.
Some of the more common symptoms of RA include:
- Joint stiffness
Don’t Miss: Are Eggs Bad For Rheumatoid Arthritis
Psoriatic Arthritis Imaging Test: X
X-rays, which use low-dose radiation to produce images of the inside of the body, can help your doctor make a psoriatic arthritis diagnosis and monitor progression of the autoimmune condition.
X-rays allow the doctor to see changes to the bone, says Elyse Rubenstein, MD, a rheumatologist in Santa Monica, California. In people with psoriatic arthritis, X-rays may show bone erosion, new bone formation, bone fusion, or a phenomenon called pencil in a cup, in which the ends of the bone have been eroded to a pencillike point. Any of these changes indicate that the disease is getting worse, Dr. Rubenstein says.
Frequency of Testing A doctor may take an initial X-ray to help diagnose psoriatic arthritis and rule out other forms of arthritis, such as rheumatoid arthritis, which have different patterns of joint involvement, says Rubenstein.
After that, how often you have X-rays depends on your physician and the state of your disease. Some doctors take X-rays just once a year for routine monitoring, while others may take them only when a patients condition changes.
Also Check: Can Rheumatoid Arthritis Affect Your Jaw And Teeth
You Wish More People Understood What Youre Going Through
Because psoriatic arthritis is not a particularly common condition , it can be hard to find someone else whos going through the same thing you are.
It took 12 years after my diagnosis to meet someone else with psoriatic arthritis, Dishner says. That means its important to create your own support system. Keeping your friends and family involved in your experiences with psoriatic arthritis and your treatment plan, says Markenson, may help them to better understand what youre going through and how to help you.
Recommended Reading: Can Rheumatoid Arthritis Be Treated Without Medication
Will I Pass On Psa To My Child
The exact cause of PsA is unclear, though genetics likely play a role. According to Anthony Scialli, MD, an obstetrician-gynecologist in Washington, DC, it is not possible to predict what proportion of children of people with PsA will get the disease.
“The highest risk seems to be associated with a gene called PSORS1, which increases the risk about sixfold,” says Dr. Scialli, who is an expert member of the Organization of Teratology Information Specialists , a professional nonprofit that provides the service MotherToBaby. “If the general population risk is about 2 percent, inheriting an abnormal PSORS1 gene would increase the risk to 12 percent.
Imaging Tests For Psoriatic Arthritis
Imaging tests can help your doctor closely examine your bones and joints. Some of the imaging tests your doctor may use include:
- X rays. X-rays arent always useful in diagnosing early stage psoriatic arthritis. As the disease progresses, your doctor may use imaging tests to see changes in the joints that are characteristic of this type of arthritis.
- MRI scans. An MRI alone cant diagnose psoriatic arthritis, but it may help detect problems with your tendons and ligaments, or sacroiliac joints.
- CT scans. These are used primarily to examine joints that are deep in the body and not easily seen on x-rays, such as in the spine and pelvis.
- Ultrasounds. These tests can help determine the progression of joint involvement and pinpoint the location.
Also Check: What Is The Best Cream For Arthritis
Neither Will Taking Deep Breaths Or Meditating
While your well-meaning yogi friend may think the cure for your symptoms is to practice a few asanas, try as you might, yoga is not a cure for psoriatic arthritis. However, it may alleviate the stress in your body that can worsen symptoms or trigger a flare. Yoga can also help ease pain and increase mobility. So if you find the practice relaxing and beneficial, go for it!
How Psoriatic Arthritis Treatment Prevents Disease Progression
The primary way to slow the progression of PsA is through medications that modify the immune system. It may take trial and error to find the treatment that works best for a given patient, notes Dr. Haberman. While we have a lot of medication options for PsA, we dont know which ones a patient will respond to, so sometimes we need to try more than one medication to find the one thats right for that patient, she says.
In addition, medications that have been effective for you can stop working over time. If this happens, your doctor may recommend a medication that works differently say, targets a different part of the immune system to control disease activity.
There are many drugs used to treat PsA. The ones that you will use will depend on the type and severity of symptoms as well as the most problematic areas .
Medications use to treat PsA include:
You May Like: Can Psoriatic Arthritis Cause Anemia