Psoriatic Arthritis Vs Rheumatoid Arthritis
PsA and RA are two of several types of arthritis. While they may share a common name and many similar symptoms, different underlying factors cause them.
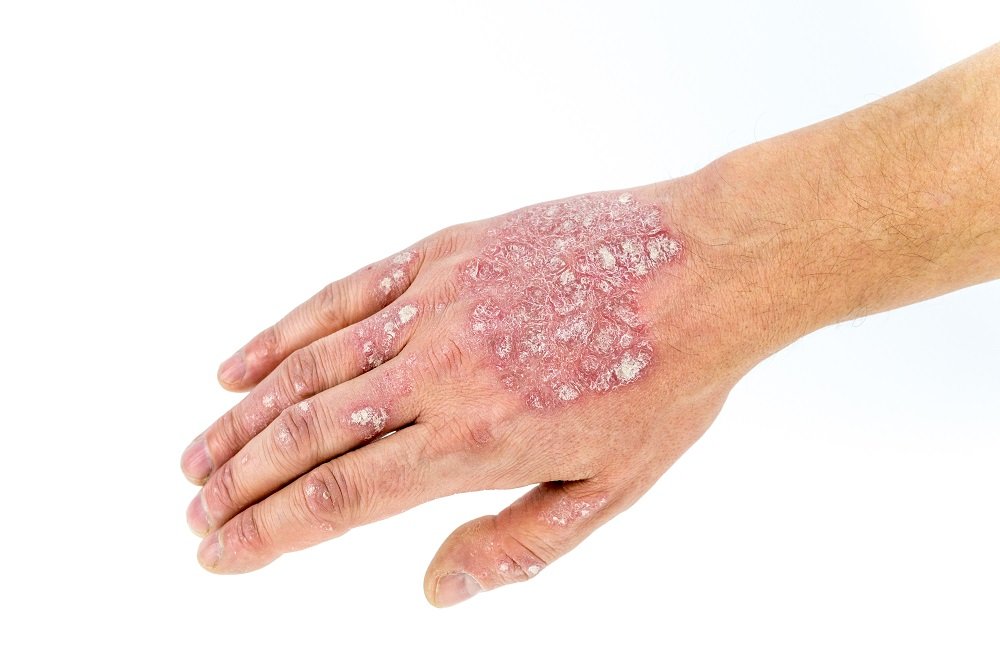
PsA occurs in people with psoriasis. This is a skin condition that causes lesions and scaly spots on the skins surface.
RA is an autoimmune disorder. It occurs when the body mistakenly attacks the tissues lining the joints. This causes swelling and eventually pain and joint destruction.
PsA occurs almost equally in men and women, but women are more likely to develop RA. PsA often first shows up between the ages of 30 and 50 for most individuals. RA usually first develops a bit later in middle age.
In their early stages, both PsA and RA share many similar symptoms. These include pain, swelling, and joint stiffness. As the conditions progress, it may become clearer which condition you have.
Fortunately, a doctor wont have to wait for the arthritis to progress in order to make a diagnosis. Blood and imaging tests can help your doctor decide which condition is affecting your joints.
Deterrence And Patient Education
Patients should be extensively educated and counseled with regards to the chronic nature of psoriatic arthritis and the importance of non-pharmacological measures, including exercise, smoking cessation, weight loss, physical therapy, and occupational therapy. They should be made aware of the fluctuating nature of this disease, requiring very close monitoring by the multi-disciplinary treatment team. The side effects related to immunosuppressive medications require a detailed explanation, and an attempt should be made to educate the patient family as well.
Classification Of Psoriatic Arthritis
The simple and highly specific Classification Criteria for Psoriatic Arthritis , developed by a large international study group, has a sensitivity and specificity of 98.7% and 91.4%, respectively. The criteria consist of established inflammatory articular disease with at least 3 points from the following features:
- Current psoriasis
- A history of psoriasis
- A family history of psoriasis
- Dactylitis
- Juxta-articular new-bone formation
- RF negativity
- Nail dystrophy
Recommended Reading: What Helps Lower Back Arthritis
Psa Symptoms: What Are The First Signs Of Psoriatic Arthritis
Jump to:What is Psoriatic Arthritis?SymptomsNext Steps
Arthritis, by definition, is characterized by the breakdown of the cartilage within the joints. If you are suffering from any type of arthritis, this is the general cause of the pain and stiffness in your joints. With over 100 types of arthritis, the top three most common are osteoarthritis, rheumatoid arthritis, and psoriatic arthritis. In this article, we will discuss the third most common type of arthritis: psoriatic arthritis .
Who Will Be Responsible For My Healthcare
Youre likely to see a team of healthcare professionals.
Your doctor, usually a rheumatologist, will be responsible for your overall care. And a specialist nurse may help monitor your condition and treatments. A skin specialist called a dermatologist may be responsible for the treatment of your psoriasis.
You may also see:
- a physiotherapist, who can advise on exercises to help maintain your mobility
- an occupational therapist, who can help you protect your joints, for example, by using splints for the wrist or knee braces. You may be advised to change the way you do some tasks to reduce the strain on your joints.
- a podiatrist, who can assess your footcare needs and offer advice on special insoles and good supportive footwear.
Also Check: What Does Arthritis In Your Hands Feel Like
Efficacy And Safety Of Risankizumab For Active Psoriatic Arthritis: 24
Andrew Ostor1, Kim Papp2, Mireia Moreno3, Cathy Spargo4, Lisa Barcomb5, Ahmed M. Soliman5, Wenjing Lu6, Ann Eldred5 and Lars Erik Kristensen7, 1Monash University, Cabrini Hospital, and Emertius Research, Melbourne, Australia, 2K Papp Clinical Research and Probity Medical Research, Waterloo, ON, Canada, 3Rheumatology Department, Parc Taulí Hospital Universitari, Institut d’Investigació i Innovació Parc Taulí, Universitat Autònoma de Barcelona, Barcelona, Spain, 4Vincent Pallotti Hospital, Johannesburg, South Africa, 5Abbvie Inc., North Chicago, IL, 6AbbVie Inc., North Chicago, 7The Parker Institute, Copenhagen University Hospital, Bispebjerg and Frederiksberg, Frederiksberg, Denmark
Session Type: Plenary Session
Session Time: 10:45AM-11:00AM
Background/Purpose: Risankizumab is a humanized immunoglobulin G1 monoclonal antibody that specifically inhibits interleukin 23 by binding to its p19 subunit. RZB is being investigated as a treatment for adults with psoriatic arthritis .
Results: A total of 1407 patients were initially enrolled and 1354 completed the 24-week assessments. Demographics and baseline disease characteristics were similar between the two groups. Patients receiving RZB achieved higher rates of ACR20 than patients receiving PBO at Week 24 . Patients receiving RZB showed greater improvements than patients receiving PBO in all secondary clinical and patient-reported outcome endpoints . RZB was well tolerated, and no new safety signals were observed .
Disclosures:
Cannabidiol Was Not Found To Help With Psa Pain
Whats New Cannabidiol is increasingly sold in stores and websites, and is discussed in many online chat groups as a potentially useful way to deal with pain, including for PsA.
But while patients were asking Jonathan Vela, MD, a rheumatologist at Aalborg University Hospital in Denmark, whether they should take it for their condition, he didnt have an answer. I first heard about CBD in 2017, but at that time no proper study had been done, making it hard to counsel patients, he says.
So Dr. Vela set out to study it. What he and his colleagues eventually found is that people taking CBD had no better response than the placebo.
Research Details The study enrolled 136 people with PsA or osteoarthritis . Half were told to take 20 to 30 mg of synthetic CBD daily for three months the rest swallowed a placebo during that time.
When people were evaluated at the end of the clinical trial, no statistically significant differences were found between the two groups for pain intensity, sleep quality, depression, anxiety, or pain catastrophizing.
Why It Matters Like other therapies, it is important for research to prove the effectiveness of any treatment before people decide to take it.
Although theres a lot of buzz around CBD, at present there is no proper study showing the effect of CBD for pain relief if you have psoriatic arthritis, Vela says.
You May Like: Can You Stop Rheumatoid Arthritis From Progressing
Sex Fertility And Pregnancy
Sex can sometimes be painful for people with psoriatic arthritis, particularly a woman whose hips are affected. Experimenting with different positions and communicating well with your partner will usually provide a solution.
Psoriatic arthritis wont affect your chances of having children. But if youre thinking of starting a family, its important to discuss your drug treatment with a doctor well in advance. If you become pregnant unexpectedly, talk to your rheumatology department as soon as possible.
The following must be avoided when trying to start a family, during pregnancy and when breastfeeding:
Loss Of Significant Joint Mobility
For example, you were able to flex your wrist 60 degrees, and two years later, you lost 50 percent of that range of motion. Its possible to feel okay and still experience loss of range of motion, says Dr. Domingues. But the idea is to prevent joint damage and to make you have less pain. If you have less pain and are still progressing, that means your treatment could be working better.
You May Like: How To Deal With Arthritis
Occurrence In The United States
According to the National Psoriasis Foundation, psoriatic arthritis affects about 1 million people in the United States, or about 30% of all persons with psoriasis. However, prevalence rates vary widely among studies. In one population-based study, less than 10% of patients with psoriasis developed clinically recognized psoriatic arthritis during a 30-year period. A random telephone survey of 27,220 US residents found a 0.25% prevalence rate for psoriatic arthritis in the general population and an 11% prevalence rate in patients with psoriasis. However, the exact frequency of the disorder in patients with psoriasis remains uncertain, with the estimated rate ranging from 5-30%.
Moreover, since the late 20th century, the incidence of psoriatic arthritis appears to have been rising in both men and women. Reasons for the increase are unknown it may be related to a true change in incidence or to a greater overall awareness of the diagnosis by physicians.
Spondylitis With Or Without Sacroiliitis
This occurs in approximately 5% of patients with psoriatic arthritis and has a male predominance.
Clinical evidence of spondylitis and/or sacroiliitis can occur in conjunction with other subgroups of psoriatic arthritis.
Spondylitis may occur without radiologic evidence of sacroiliitis, which frequently tends to be asymmetrical, or sacroiliitis may appear radiologically without the classic symptoms of morning stiffness in the lower back. Thus, the correlation between the symptoms and radiologic signs of sacroiliitis can be poor.
Vertebral involvement differs from that observed in ankylosing spondylitis. Vertebrae are affected asymmetrically, and the atlantoaxial joint may be involved with erosion of the odontoid and subluxation . Therapy may limit subluxation-associated disability.
Unusual radiologic features may be present, such as nonmarginal asymmetrical syndesmophytes , paravertebral ossification, and, less commonly, vertebral fusion with disk calcification.
Read Also: How Can You Stop Arthritis In Your Hands
Important Update To The Medication Guide For Rinvoq Extended
On December 2, 2021, the RINVOQ Prescribing Information and Medication Guide were updated to include new information about the increased risk of death and serious heart-related events, such as heart attack or stroke, and updated information about the risk of cancer and blood clots based on discussions with the FDA.
The following describes the recent changes to the RINVOQ Medication Guide. Please refer to the full Prescribing Information and Medication Guide for additional safety information.
The following serious side effects were added to the section What is the most important information I should know about RINVOQ?
RINVOQ may cause serious side effects, including:
Focusing On People With Psoriasis
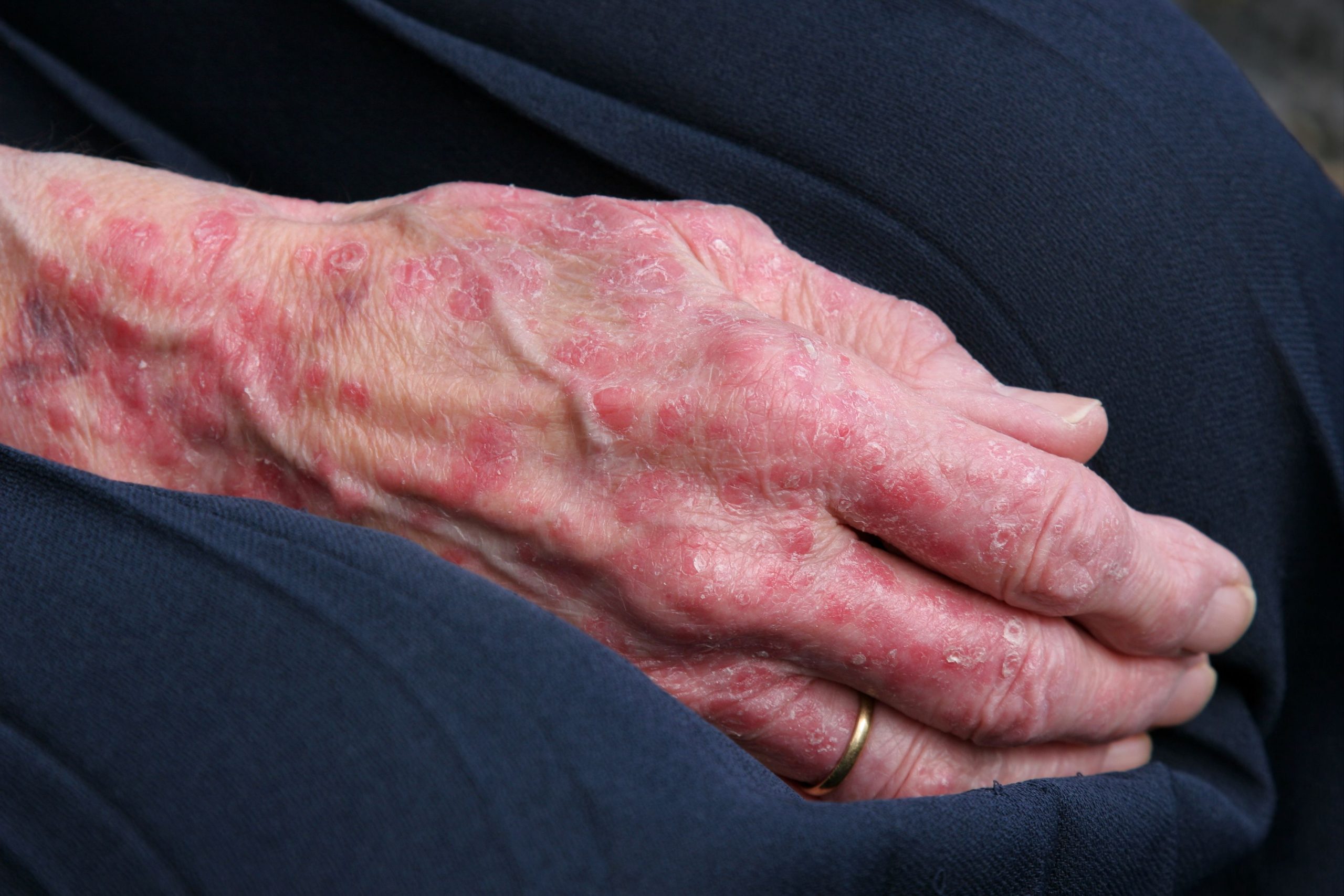
Most people with psoriatic arthritis have psoriasis first. For a small percentage of patients, psoriatic arthritis occurs before psoriasis, although most often they will have a first-degree relative with skin psoriasis, notes Dr. Haberman. Still, others have no skin psoriasis or dont notice the psoriasis hidden in areas like the scalp, umbilicus, and gluteal fold.
Read more about the connection between psoriasis and PsA.
Up to 30 percent of patients with psoriasis will go on to develop psoriatic arthritis, says Dr. Haberman. The majority of cases begin with the skin condition and then progress to joint pain within seven to 10 years. Recent studies have found that patients with psoriasis who develop severe fatigue, heel pain, and joint pain without overt swelling are more likely to develop PsA.
While we dont yet know which individual patients with psoriasis will go onto develop PsA, researchers have identified a few potential risk factors for the progression of PsA, including:
- Family history of psoriatic arthritis
- Psoriasis that affects the scalp and groin
- Nail involvement in psoriasis, such as nail pitting
- Being overweight or obese. PsA is worse in patients who are overweight and often biologics may not work as effectively in people who are overweight, says Dr. Haberman.
- Smoking
- Age
- Exposure to certain infections
- Physical trauma
You May Like: Does Psoriatic Arthritis Itch
Im Training For My First Bodybuilding Contest
Lauren Scholl, 33, views exercise as her me time. Long-distance running and dancing used to be her favorite ways to unwind and zone out. In fact, she was once a competitive dancer, but that career came to a halt when she developed psoriatic arthritis around five years ago.
Ive been through about six or seven different drugs that unfortunately did not work for me, Scholl tells SELF. She says joining CreakyJoints, an organization for people with arthritis and rheumatic disease, gave her a lot of support during the process. Knowing that youre not alone and youre not the only one going through this made a huge impact on my life, she says.
Her sons, now five and eight years old, were also very young at the time of her diagnosis. Scholl says changing their diapers, preparing their bottles, and generally just trying to keep up with their energy was physically overwhelming with her joint pain. She remembers waking up dreading the physical toll it took on her body.
Eventually, though, Scholl found a medication that worked. She receives a biologic infusion once a month. It makes her mood a bit low for about 48 hours, but she says that side effect is worth it: I get almost a full month of feeling like myself.
Being able to run around and go to the park with her sons without having to grit her teeth through the pain has been life-changing. My symptoms have curbed enough that Im able to enjoy things like playing with my kids now that theyre older, she says.
Related:
What Is Psoriatic Arthritis
Psoriatic arthritis is a form of inflammatory arthritis. It affects about 1 million people in the United States, or 30% of people who have psoriasis. Psoriasis is a skin disease that causes a red, scaly rash, most often on your elbows, knees, ankles, feet, and hands.
Psoriatic arthritis is an autoimmune condition. It happens when your bodys immune system attacks healthy tissue by mistake. PsA most often affects your skin and your joints, which can become swollen, stiff, and painful. Over time, if you dont treat it, the inflammation can damage joints and tissues.
Also Check: Is Peanut Butter Bad For Arthritis
Expert Interview: The Big Psoriasis And Psoriatic Arthritis Questions
Psoriatic arthritis is a condition that causes inflammation of the joints. This causes the joints to become painful, stiff and often swollen. Only one or two out of every 10 people with psoriasis will develop this type of arthritis. Psoriatic arthritis can affect any joint in the body and symptoms can vary from person to person. It can develop slowly with mild symptoms, or come on quickly and be severe.
I did do a lot of dating in my twenties, and as someone who has always had psoriasis, I have a lot of flaky first date encounter stories too.
Arthritis is a term often used to mean any disorder that affects joints. There are over types of arthritis. Treatment may include resting the joint and alternating between applying ice and heat. Osteoarthritis affects more than 3. There are several diseases where joint pain is primary, and is considered the main feature. Generally when a person has arthritis it means that they have one of these diseases, which include:.
Joint pain can also be a symptom of other diseases. In this case, the arthritis is considered to be secondary to the main disease these include:. An undifferentiated arthritis is an arthritis that does not fit into well-known clinical disease categories, possibly being an early stage of a definite rheumatic disease. Pain, which can vary in severity, is a common symptom in virtually all types of arthritis.
Treatment Of Psoriatic Arthritis
-
Arthritis treated with disease-modifying antirheumatic drugs and biologic agents
Ustekinumab is an interleukin -12 and IL-23 antagonist. The dosage is 45 mg subcutaneously at weeks 0 and 4 followed by 45 mg every 12 weeks thereafter. The dosage is 90 mg subcutaneously if the patient weighs > 100 kg. Adverse effects are similar to those of the other biologic agents Biologic agents Rheumatoid arthritis is a chronic systemic autoimmune disease that primarily involves the joints. RA causes damage mediated by cytokines, chemokines, and metalloproteases. Characteristically… read more .
Secukinumab is an IL-17 inhibitor. Secukinumab can be given at a dosage of 150 mg subcutaneously at weeks 0, 1, 2, 3, and 4 and every 4 weeks thereafter. Without the loading dosage, secukinumab is given at 150 mg subcutaneously every 4 weeks. If patients continue to have active psoriatic arthritis, a dose of 300 mg should be considered. Secukinumab may be given with or without methotrexate. Adverse effects include urticaria, upper respiratory infections, fungal infections due to Candida, diarrhea, herpes zoster, and inflammatory bowel disease.
Also Check: Ra Hand Pain
What Are The Symptoms Of Psoriasis
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
Symptoms And Signs Of Psoriatic Arthritis
Psoriasis of the skin or nails may precede or follow joint involvement. Severity of the joint and skin disease is often discordant. Also, skin lesions may be hidden in the scalp, gluteal folds, or umbilicus and go unrecognized by the patient.
The distal interphalangeal joints of fingers and toes are especially affected. Asymmetric involvement of large and small joints, including the sacroiliacs and spine, is common. Joint and skin symptoms may lessen or worsen simultaneously. Inflammation of the fingers, toes, or both may lead to sausage-shaped deformities, which are not present in patients with rheumatoid arthritis Rheumatoid Arthritis Rheumatoid arthritis is a chronic systemic autoimmune disease that primarily involves the joints. RA causes damage mediated by cytokines, chemokines, and metalloproteases. Characteristically… read more . Rheumatoid nodules are absent. Arthritic remissions tend to be more frequent, rapid, and complete than in rheumatoid arthritis, but progression to chronic arthritis and crippling may occur. There may be arthritis mutilans .
Enthesopathy can develop and cause pain.
Back pain may be present. It is often accompanied by asymmetric syndesmophytes of the spine.
Don’t Miss: How To Deal With Arthritis