Maintain A Healthy Weight
The ankle is a weight-bearing joint, and being overweight places even more pressure on it, making symptoms worse, says Dr. Domingues. Excess body weight also increases inflammation, which fuels the painful symptoms of PsA. It can also make medical treatments less effective.
Unfortunately, joint pain and in particular, foot and ankle pain from psoriatic arthritis can make it difficult to exercise, which is an effective way to manage your weight, as well as PsA symptoms. Despite the common belief that exercise will aggravate joint pain and stiffness, the opposite is actually true, reports the Mayo Clinic: Lack of exercise can actually exacerbate symptoms.
Gentle low-impact exercises like swimming, cycling, and chair yoga are good options for people with ankle-related arthritis. The calorie burn can quickly add up: A 155-pound person can burn almost 250 calories slowly swimming freestyle for half an hour. Just be sure to start slowly and increase activity gradually.
How Does It Affect Cartilage
In arthritis, the cartilage at the end of the bones becomes damaged and breaks down. In PsA, this damage results from persistent inflammation. As the cartilage erodes, the bones rub together, causing further pain and joint damage. Inflammation can also lead to bone erosion and extra bone growth.
Chronic inflammation can also affect the ligaments and tendons around the joint.
Diagnosis Of Eye Problems Related To Rheumatoid Arthritis:
Your doctor would ask questions related to your medical history and symptoms. They would also take a close look at your eyes. In certain cases, your doctor might take a small sample of fluid, pus, or any other material from your eye.
You might require an ophthalmologist to pinpoint the problem of your eye. A rheumatologist may help assess your condition of rheumatoid arthritis. Your doctors can figure out the best treatment for you as per your symptoms and severity.
Also Check: How To Reduce Arthritis And Joint Pain
The Importance Of Regular Eye Care With Arthritis
Its critical for anyone with inflammatory arthritis to get regular preventive eye care and to let your rheumatologist or eye doctor know if youre having new or unusual eye-related symptoms, no matter how minor they may seem. Annual dilated eye exams at the eye doctor are important to check for underlying damage early on. Some eye diseases might not cause a lot of pain or much change in vision, especially in earlier stages, so an eye exam is always necessary, Dr. Akpek says.
Dr. Wu requires annual exams from her inflammatory arthritis patients if there are no issues and wants to see patients more frequently if there are any problems.
All of the physicians we interviewed stressed the importance of fostering communication between rheumatologists and ophthalmologists. As a patient, you can help make sure your health care providers are sharing medical records and are up to date on any new symptoms, diagnoses, or treatment changes. Dont ever assume one doctor knows what the other does.
Seeing My Doctor For Leg Pain And Swelling
I already had experience in the past of letting my pain go too long before I said anything. My reward for that was it caused permanent joint damage in my back. I was not about to wait so long this time. My next visit with my primary care doctor I told her of the pain I was experiencing in my left towards my ankle. She examined my leg. She did not see anything that looked unusual. She then looked at my ankle. She did notice that it was very swollen. I explained to her that it swells a lot along with my other ankle but I was not having the pain in the right ankle. She looks in my chart and notices psoriatic arthritis noted there. She said that the psoriatic arthritis was putting pressure on my joints in my foot causing them to swell. That swelling was causing shooting pain as a reaction.
You May Like: How To Treat Arthritis In Lumbar Spine
If You Have Autoimmune Thyroid Disease
If you have Hashimotos thyroiditis or Graves disease, your risk of developing another autoimmune disease is increased. As a result, its important to become knowledgeable about the common signs and symptoms of other autoimmune conditions. These include fatigue, muscle and joint pain and/or swelling, digestive problems, dry eyes, brain fog and difficulty concentrating, and skin rashes. If you have symptoms that continue after optimal thyroid treatment, you should discuss them with your doctor.
Theres also a caution if you have Graves disease and are being treated with a beta blocker. While most Graves disease patients are not given beta blockers for extended periods, long-term beta blocker use is associated with a significantly increased risk of developing psoriasis.
How Can I Find The Appropriate Care I Need
Initially your GP is the first point of contact, who then should refer you on to a dermatologist/rheumatologist, if this is not already the case. If you are not happy with the advice you receive, remember you are always entitled to seek a second opinion. Remember, If you are seeing a dermatologists for your psoriasis and a rheumatologists for your arthritis make sure each is aware of this, so they can liaise and provide you with appropriate care for both conditons.
Also Check: Is Protein Good For Arthritis
What Are Dry Eyes
Typically, the surfaces of your eyes are spread with a thin layer of tears every time you blink. This tear film is made of watery, oily, and mucous layers.
If your eyes dont make enough tears or the right kind of tears, it causes dry eyes. This can make blinking irritating to your eye.
Typical symptoms of dry eyes include:
- redness
- burning or stinging in the eyes
- scratchy or irritated feeling in the eyes
- feeling of sand in the eyes
- stringy mucus in the eyes
- blurry vision
- difficulty reading
In some cases, dry eye may develop without noticeable symptoms. This can occur in a condition known as Sjögrens syndrome, which affects some people with PsA.
If you develop dry eyes, your doctors recommended treatment plan will depend on the severity and cause.
Treatment may include:
- over-the-counter lubricating eye drops
- prescription eye drops to decrease inflammation
- prescription oral medications to increase your tear production
- silicone or gel plugs to block your tear ducts and keep tears in your eyes for longer
Uveitis is a condition in which inflammation occurs in the uvea of the eye.
The uvea is the middle layer of your eye. It includes three parts:
- The iris. This is the colored part of your eye. It controls the amount of light that comes into your eye.
- The ciliary body. This part helps your eye to focus.
- The choroid. This part contains many blood vessels that deliver nutrients to your eye.
People with PsA are more likely than average to develop uveitis.
The Structure Of The Eye And Where Arthritis Strikes
The eye is a complicated structure. Different types of arthritis can cause different types of eye problems. Its important to understand some general eye anatomy:
The entire eye is covered by a white outer coat called the sclera. The sclera is covered by a thin semi-transparent mucous membrane that has blood vessels, which is called conjunctiva.
At the very front of the eye is the cornea, which is the transparent layer that transmits and focuses light.
Behind the cornea is the iris, which is the colored part of the eye that helps regulate the amount of light that enters the eye like the diaphragm of a camera. The pupil is the dark hole in the middle of the iris, which adjusts in size to let in more or less light.
Just behind iris and pupil is the lens, which is like the lens of the camera. The lens is suspended in the eye cavity through some fine fibrils that attach to the ciliary body.
The back of the eye contains these important structures:
- Choroid: A layer that contains blood vessels, located between the sclera and retina
- Retina: A nerve layer that lines the back of the eye it creates electrical impulses from light that are sent to the brain via the optic nerve
- Macula: An area in the retina with special light-sensitive cells
- Optic nerve: A bundle of nerves that transmits visual messages from the eye to the brain
Don’t Miss: How To Keep Arthritis From Spreading
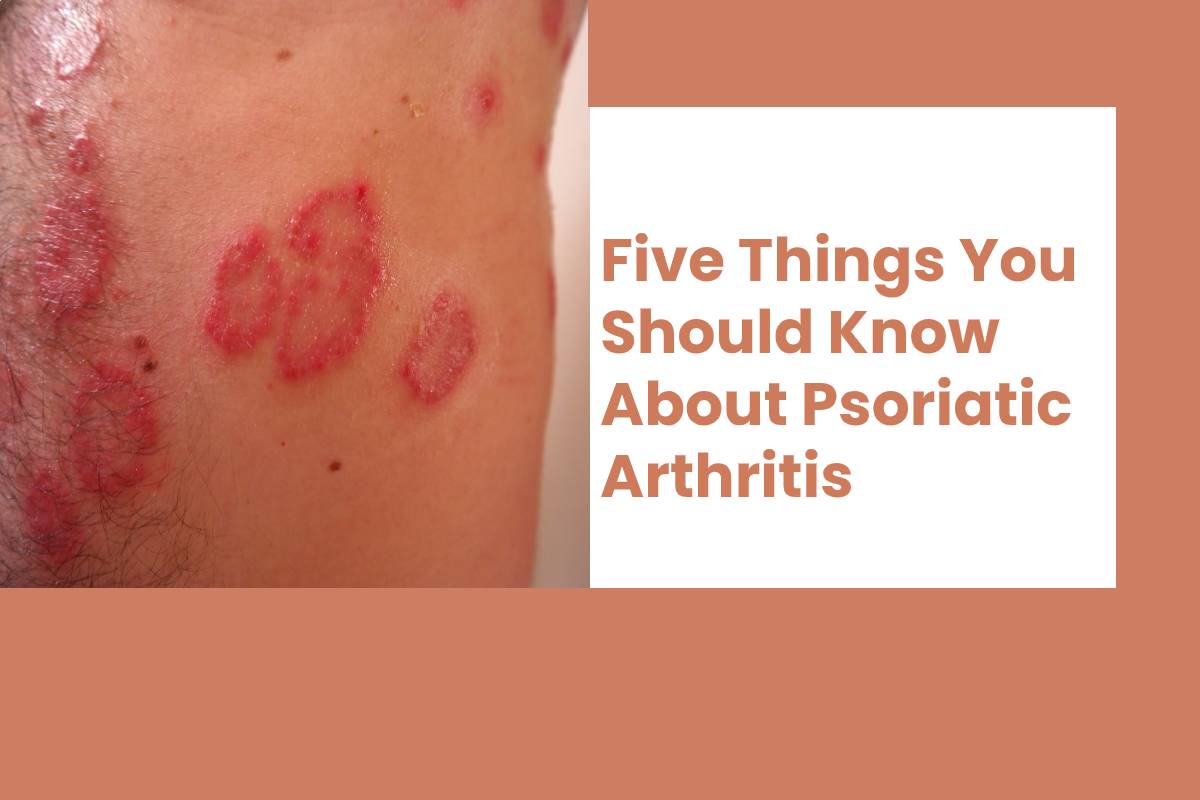
Symptoms On The Inside And Outside
Can you suffer from joint pain? Do you have pitted nails? What among rashes that are swollen and scaly? This are some of the most prominent psoriatic arthritis symptoms . This form of arthritis resembles rheumatoid arthritis. It affects about 30% of people who have psoriasis, a skin disease. It can affect a variety of body parts as well as the emotions.
Peripheral Ulcerative Keratitis Or Puk:
Peripheral Ulcerative Keratitis or PUK is a rare, yet serious condition that involves inflammation of the blood vessels in the eyes or ulceration in the cornea of your eye.
Symptoms of this eye condition are quite similar to those of Scleritis and Uveitis and include pain, redness, and sensitivity to light. However, PUK can also result in blurred vision. Sometimes people with Peripheral ulcerative keratitis complain that things look fuzzy due to swelling, that can distort the lens of the eyes.
You May Like: Does Walking Help Knee Arthritis
The Arthritis And Eye Connection
Arthritis involves an inflammatory condition of the joints and connective tissues. Depending on the form, various other symptoms may also develop. According to the , there are about 100 different forms of arthritis.Although the condition primarily affects the joints, it is also associated with an increased risk of certain eye problems. Continue reading below to learn more about arthritis and how it can affect your eyes.
Hands And Feet Of Deformities

Arthritis mutilans is the most serious type of psoriatic arthritis . It causes inflammation in the small bones in your hands and feet, causing them to break down. Its possible that the fingertips and toes will become deformed and difficult to lift. They can have become thinner as a result of bone loss. This unusual type of psoriatic arthritis affects less than 5% of individuals with the disease.
You May Like: How To Fight Against Arthritis
Psoriasis Psa And Thyroid Disease
While researchers have studied connections between psoriasis/PsA and other autoimmune diseases, a late 2018 study published in the Journal of the American Academy of Dermatology found that having psoriasis and PsA increases the risk of developing autoimmune Graves disease and Hashimotos thyroiditis. The risk was even greater for patients with PsA.
As with many autoimmune disease issues, researchers havent yet determined the explanation. But they theorize that genetic and immune system irregularities common to both diseases may link psoriasis/PsA and autoimmune thyroid disease.
Based on their findings, the study authors recommended increased physician awareness of the risks. They also advised thyroid screening for patients with psoriasis and PsA, and for those psoriasis/PsA patients who have thyroid symptoms.
Psoriasis And The Eye
Psoriasis and the eye for patients with psoriasis, uveitis had been commonly thought to occur only in conjunction with psoriatic arthritis, however, there have been many case reports of psoriatic uveitis presenting independent of joint disease. Furthermore, the temporal relationship of these two entities has been disputed. Some recent studies suggest that inflammatory joint manifestations precede uveitis. Nevertheless, some cases of uveitis have been reported to occur even before psoriatic skin disease, and uveitis has been reported as the first presenting sign of psoriatic arthritis in 0% to 11.4% of cases. The severity of ocular inflammation does not necessarily correlate with extent of joint findings but may correlate with skin disease.
Since the latency period for development of symptomatic ocular abnormalities may be longer than 5 years, continued surveillance and continued use of appropriate ocular protection by all patients treated with PUVA is indicated.
Recommended Reading: How Do You Get Arthritis In Your Lower Back
Ocular Manifestations Of Autoimmune Disease
SAYJAL J. PATEL, LT, MC, USNR, and DIANE C. LUNDY, CAPT, MC, USN
Naval Medical Center, San Diego, California
Am Fam Physician. 2002 Sep 15 66:991-998.
Patients with autoimmune diseases are frequently encountered by family physicians. It is important to understand not only the systemic effects of these diseases but also their ocular manifestations . Most ocular complications involve the cornea but may also include the conjunctiva, uvea, sclera, retina, and surrounding structures . The majority of these diseases will ultimately need to be referred to an ophthalmologist.
Ocular Manifestations of Autoimmune Disease
Rheumatoid arthritis
Ocular Manifestations of Autoimmune Disease
Rheumatoid arthritis
Cross section of the eye.
FIGURE 1.
Cross section of the eye.
What Are Your Next Steps
If you have psoriasis or PsA, you should familiarize yourself with the symptoms of the two key autoimmune thyroid diseases and the conditions they cause:
-
Hashimotos thyroiditis and the resulting hypothyroidism
-
Graves disease and the resulting hyperthyroidism
Common symptoms of Hashimotos and hypothyroidism include fatigue, weight gain, depression, hair loss, constipation, puffiness, hoarseness, neck discomfort, and brain fog. Common symptoms of Graves disease and hyperthyroidism include insomnia, weight loss, anxiety, diarrhea, neck enlargement , muscle weakness, and eye and vision problems.
If you have psoriasis/PsA and notice any of these symptoms, your first step should be a complete thyroid screening and evaluation. This should include:
-
A hands-on clinical examination to detect irregularities in the size and shape of your thyroid
-
Thyroid blood tests, including a thyroid stimulating hormone ,
-
free thyroxine and free triiodothyronine
-
Blood tests for thyroid antibodies, including thyroid peroxidase antibodies for Hashimotos, and thyroid stimulating immunoglobulin for Graves disease
Your physician may also order a thyroid ultrasound to check for the thyroid enlargement or shrinkage commonly seen in autoimmune thyroid disease.
You May Like: How To Cure Arthritis In Shoulder
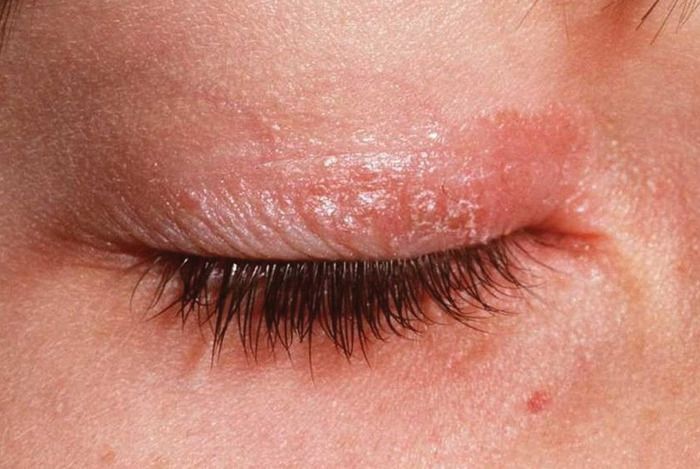
Eye Inflammation And Psoriatic Arthritis
Your joints are not the only things affected by PsA. Learn what secrets your eyes could hold.
For those living with psoriatic arthritis , achy joints and difficulty moving are just the beginning of the story. From an increased risk of cardiovascular disease to the emotional impact of PsA, balancing your joint health while properly monitoring and treating comorbidities is a lot to consider, and it may require a team of specialists. So you visit the rheumatologist for your joints, a dermatologist for your skin. But how can optometrists and ophthalmologists play a role in your psoriatic disease care?
About 7 percent of those with PsA will develop uveitis , a medical term referring to several different diseases related to inflammation within the eye. The most common form is anterior uveitis, which affects the inner wall of the ciliary body . This 7 percent figure is much higher than for the general population, which sees a risk of uveitis closer to 0.1 percent.
The reason for the increased risk is not explicitly clear, according to James Rosenbaum, M.D., a rheumatologist and ophthalmologist at Oregon Health and Science University. He discussed uveitis and the risk to those living with psoriatic disease in a 2019 NPF Psound Bytes⢠podcast episode titled âPsoriatic Arthritis and Uveitis: Whatâs It All About?â
âWhy do you get uveitis with arthritis together? That is a mystery â just getting skin disease and joint disease together,â says Dr. Rosenbaum.
Effects On The Eyes And Vision
The PsA can also affect the vision and eyes. As a matter of fact, inflammation and red dots in and around the eyes can affect vision.
It has been estimated that approximately 7 percent of people with PsA will develop uveitis, which is a full pack of the diseases related to eye inflammation. If it is not diagnosed on time, then Psoriasis-related eye conditions can cause a loss of vision.
Don’t Miss: How To Ease Arthritis Pain In Ankle
Uveitis And How Psoriasis Can Affect The Eyes
What people with psoriasis and psoriatic arthritis can do to help keep their eyes healthy.
While the most well-known and common symptoms of psoriasis affect the skin, psoriatic disease can impact many different areas of the body. One example is psoriatic arthritis, a type of arthritis that affects up to 30 percent of people who have psoriasis. Both psoriasis and psoriatic arthritis are the result of abnormal immune system activity. With psoriasis, this abnormal immune system activity causes skin lesions, and with psoriatic arthritis, it causes inflammation in the joints.
Here, we look at an inflammatory eye condition called uveitis, which is a potential complication of psoriasis.
What is uveitis? Uveitis is inflammation of the middle layer of the eye, which is called the uvea. Redness, pain, sensitivity to light, and visual disturbances are all symptoms of uveitis. These symptoms can progress suddenly or gradually. Uveitis can have a number of different causesinjuries, infections, medication side effects, certain cancersor it can have no identifiable cause. Uveitis is also associated with autoimmune and inflammatory disorders. Treatment involves a combination of therapies to alleviate symptoms and therapies to treat the cause of uveitisfor example, medications to treat an infection, or medications to regulate an immune disorder.
Youre Tired As All Get Out
More fatigue than usual could signify increased inflammatory disease activity, also known as a flare. According to the National Psoriasis Foundation, proteins called cytokines that are released during inflammatory reactions lead to the fatigue. The zap in energy could also be related to medications that are sometimes prescribed for psoriatic arthritis, or it could be an indication that you just need to slow down and rest . But if the fatigue is frequent, its worth letting your rheumatologist know.
Recommended Reading: What Are The Signs And Symptoms Of Rheumatoid Arthritis
What Can Blood Tests Tell Me Or The Doctor
To make a diagnosis of psoriatic arthritis most doctors would require you to have psoriasis, or a history of psoriasis in a close relative, together with arthritis and inflammation in at least one joint. If several joints are affected the doctor would expect to find a pattern of joints involved which matches one of the patterns usually seen in psoriatic arthritis. Blood tests for rheumatoid arthritis are usually negative but often blood tests of general inflammation in the blood are positive. These latter bloods are called the erythrocyte sedimentation rate C-Reactive protein or plasma viscosity all are measures of inflammation and abnormal, if the value exceeds a certain level.