Swimming And Water Aerobics
CDC , swimming is the fourth most popular sports activity in the United States. It may be a particularly beneficial form of exercise for people with RA, as the buoyancy of the water helps alleviate strain on the joints. Due to this, people with RA can often exercise for longer in the water than on land.
People with RA may also wish to consider trying other aquatic activities, such as water aerobics.
How Is It Diagnosed
RA is generally diagnosed by a rheumatologist. Diagnosis is based upon factors, such as inflammation of the tissues that line the joints, the number of joints involved, and blood-test results. A physical therapist may be the first practitioner to recognize the onset of RA the physical therapist will refer an individual with suspected symptoms to an appropriate clinician for further tests.
How Can A Physical Therapist Help
Physical therapists play a vital role in helping people with RA improve and maintain function. Your physical therapist will work with you to develop a treatment plan to help address your specific needs and goals, and keep you moving well. Physical therapists understand how bones, joints, and muscles work together. They can help you get your body back on track.
Because the signs and symptoms of RA can vary, the approach to your care also will vary. What works for you may not work for others. Your physical therapist will design a treatment plan to meet your needs and may:
- Provide advice and encouragement on how to improve your general fitness with regular exercise. As with many conditions, education is key to building and keeping good health.
- Design a personal exercise plan to improve your joint flexibility and muscle strength.
- Help you develop energy-saving measures to improve your daily functions at home and work.
- Suggest short-term, pain-relief methods, such as gentle heat and electrical stimulation.
Don’t Miss: What Type Of Doctor Handles Arthritis
How Can Physical Therapy Help In Rheumatoid Arthritis
There are different types of physical therapy that can be useful in treating rheumatoid arthritis . The goal of physical therapy is to help reduce pain and swelling, improve joint range of motion, and maintain or improve muscle strength.
It is often believed that rheumatoid arthritis physical therapy can help by:
If you are considering physical therapy for your RA, it is important to speak with your doctor first. Physical therapy can be an effective treatment for many people with RA, but it is not right for everyone. Your doctor will be able to help you determine if physical therapy is right for you.
Can Physical Therapy Make Arthritis Worse
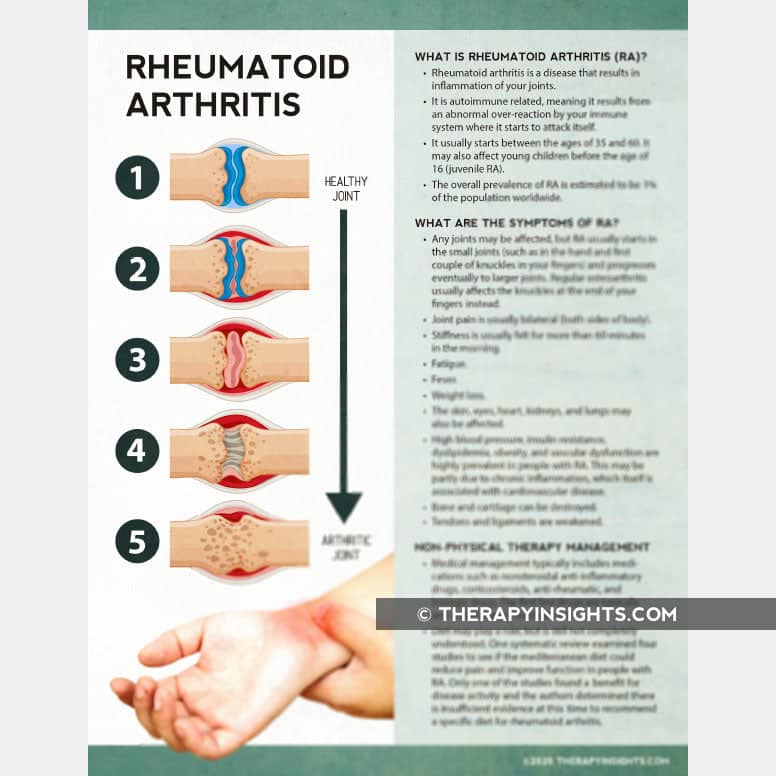
Physical therapy aims to improve function and decrease arthritis symptoms. Treatment should not make your symptoms worse or cause pain.
However, you may find some of the exercises challenging, especially in the beginning. After or during a PT session, its typical to experience a moderate amount of muscular discomfort or soreness.
Talk with your physical therapist about your treatment response and pain tolerance. Let them know if you have worsening symptoms, severe pain, or difficulties during and after a session.
Your physical therapist can make the appropriate modifications to your treatment plan. They may use different techniques or reduce the frequency and intensity of your sessions.
exercise program for arthritis , consult your doctor or physical therapist. They can recommend appropriate exercises and suggest modifications.
Recommended Reading: Can Vicks Vapor Rub Help Arthritis Pain
What Exercises Are Best For Rheumatoid Arthritis
Exercise is vital for people with rheumatoid arthritis.However, it can be hard for patients to find the motivation to move around whentheyre dealing with so much pain.
If they dont stay active, their muscles become weaker.Muscle strength is important because it helps you stay mobile and stabilizesthe joints. Exercise therapy may not slow the progression of the disease, butit can increase your physical capacity.
Our physicaltherapists customize treatment for each patient. We take into account yourage, range of motion, disease stage and strength before creating an exerciseplan for you.
If youd like to try exercising at home, consult with aprofessional first. Some of the most effective types of exercise for rheumatoidarthritis therapy include:
Stretching Relieves symptoms, improves flexibility andreduces stiffness
Walking Low-impact exercise that improves heart healthand mood
Tai chi or yoga Enhance balance and range of motion whilereducing stress
Pilates Strengthens the muscles and stabilizes thejoints
Water exercise Water reduces gravity, which diminishesstress on the joints as you move to enhance strength and range of motion
Cycling Cycling indoors allows you to move at your ownpace, improving mobility and building leg strength
Hand exercises Increases flexibility and power in thehands, which are often affected by rheumatoid arthritis
No Comments
Heat And Cold Therapy
Heat and cold therapy can help relieve pain and stiffness associated with rheumatoid arthritis. This type of heat therapy, such as using a heating pad, can help relax muscles and ease the pain. Cold therapy, such as ice packs or cool compresses, can help reduce inflammation. There is some evidence that alternating between heat and cold therapy may be more effective than using one or the other.
The reason heat and cold work are not entirely clear, but it is thought that the heat dilates blood vessels, which increases blood flow and delivers more oxygen and nutrients to muscles. The cold numbs pain receptors and reduces inflammation.
Also Check: What Do You Do For Arthritis In The Hands
Preserves The Ability To Perform Daily Activities
Physical therapists can assist in preserving the ability to perform daily activities in patients suffering from rheumatoid arthritis.
Physical therapists may assist patients in doing the following:
- Increasing range of motion and warming up the muscles before they attempt a strenuous activity, such as gardening or housework.
- Learning how to perform daily activities, such as doing the dishes or taking a shower.
- Completing basic tasks, such as getting dressed without assistance.
Physical Therapy For Rheumatoid Arthritis
The goal of it is to keep you moving. It uses exercise and other methods to stimulate muscles, bones, and joints. The result is more strength, tone, and overall fitness.
Physical therapists understand the mechanics of bones, joints, and muscles working together, the problems that can happen, and what to do about them. Itâs a good idea to work with a therapist, whether youâve had RA for a long time, youâre newly diagnosed, and no matter how severe it is.
In the early stages of the disease, your physical therapist can check on your strength, fitness, and how well your joints work. They’ll make an exercise plan to keep your joints as healthy as possible.
If you have moderate or advanced rheumatoid arthritis, physical therapy can help you keep or improve your strength and flexibility.
Together, youâll make a plan for each muscle and joint group, and for your overall fitness. It will probably include:
Exercise. This is the cornerstone of any physical therapy plan. It will match your ability and fitness level, and include flexibility, strength, and cardio .
Heat or ice. Treating inflamed or painful joints with heat or ice packs helps some people feel better.
Massage. It can also help you feel better.
Motivation and encouragement. Itâs a big plus to have a pro to cheer you on and push you to keep going.
Don’t Miss: How To Know If You Have Arthritis In Knee
Infrared Sauna Therapy Is The Best Natural Treatment For Rheumatoid Arthritis
There is no denying that rheumatoid arthritis can be debilitating and painful. Thankfully, several treatments available can help ease the symptoms and improve the quality of life. Among the most effective of these is infrared sauna therapy.
Infrared saunas work when infrared light penetrates the body and provides several health benefits.
There are many benefits of using an infrared sauna, including:
- Relief from pain and inflammation
- Increased circulation
- Reduced stress and anxiety
- Improved sleep quality
A growing body of research has shown that infrared sauna therapy can effectively treat RA. Overall, the results of these studies have been positive, with many patients reporting significant improvements in their symptoms after using an infrared sauna.
Talk To People Who Understand
On myRAteam, the social network for people with rheumatoid arthritis and their loved ones, more than 145,000 members come together to ask questions, give advice, and share their stories with others who understand life with RA.
Have you used physical therapy to manage your RA? Share your experience in the comments below, or share your story on your myRAteam Activities page.
References
Recommended Reading: Is Dark Chocolate Good For Arthritis
Finding Arthritic Pain Relief
If you experience pain, stiffness, or limited range of motion due to arthritis, contact us today to schedule an appointment. Whether your arthritis is constant, intermittent, severe, or mild, our physical therapists will work diligently to find you relief and improve your quality of life.
Benefits Of Physical Therapy For Rheumatoid Arthritis

While Rheumatoid Arthritis can have an effect on the joints and organs of the body, physical therapy can provide several meaningful benefits. Physical therapy can help ease symptoms and enhance your quality of movement, making everyday life easier for people suffering from RA.
When seeing a physical therapist about pain resulting from RA, a therapist will evaluate your posture, muscle imbalances, and the overall mechanics of your body. Theyll teach you to improve how to move to prevent injury and reduce pain.
Your therapist can also create a customized stretching and exercise plan that helps ease pain, increase your range of motion, and improve your movement patterns.
Things that physical therapy can do to help with RA include:
- Improve your overall level of fitness
- Increase your endurance
- Improve your balance and stability
- Increase coordination
Read Also: What Rheumatoid Arthritis Feels Like
Physical Therapy To Help Rheumatoid Arthritis
Physical therapy is important for athletes that are facing injuries from their sport or exercising, but it is also important and helpful for many other ailments. Rheumatoid arthritis is one of the many cases where physical therapy can help. Physical Therapy can help you move better, get stronger, and may even mean less pain.
One important thing is to talk with your rheumatologist and pick out goals that you are wanting to achieve. Start with smaller goals like holding your kids or grandkids, or increasing mobility. By picking out goals you will be able to tell your physical therapist what kind of therapy plan you are looking for to reach your goals. Physical therapist can help RA patients with moves and stretches to increase mobility and range of motion.
One way to help your RA is to make sure that you are staying active regardless of your situation. Previous studies concluded that high-impact exercise could be damaging, but it turns out that staying active will actually keep your joints and muscles stronger and healthier as you get older. RA can contribute to heart disease so it is important to keep a healthy heart. But working through some aerobic exercises here at Oahu Spine & Rehab you will be increasing cardiovascular involvement which will help prevent heart disease.
Let OSR help make you the best version of yourself and dont let your Rheumatoid arthritis take control of your life! Give us a call today at 488-5555 or Contact Us!
Teaching You How To Exercise Safely
Keeping active is very important when you have arthritis. Many people are afraid that exercise will increase their pain or cause further damage to their joints, but your joints are designed to move and the muscles and tissues around them become weaker if theyre not used. This can reduce your mobility and independence, and make your day-to-day activities more difficult.
Regular exercise can:
- increase your general fitness and stamina
- help you to lose weight or keep to a healthy weight
- strengthen your muscles and joints
- improve your general mobility
- make you feel more self-confident.
- stimulate production of your bodys own natural pain-relieving hormones .
Your physiotherapist will assess your muscle strength and the range of movement in your joints, and advise you about activities and exercises that will help keep your joints working as well as possible.
The important thing is to find a form of exercise you enjoy so you do it regularly. Think about this and discuss it with your physiotherapist they can help you plan a programme if youre new to exercise and advise on any special equipment or training that youll need to get started.
Some physiotherapists have access to a hydrotherapy pool where you can perform exercises in warm water. Many people find it easier to move in water the warmth is soothing and the water supports your weight so that you can move your joints and muscles without straining them.
Read more about exercise and hydrotherapy and arthritis.
Don’t Miss: How To Take Care Of Arthritis
What Physiotherapy Can Offer You
After diagnosis, the physiotherapist will offer education and advice, which is likely to include:
information regarding how to recognise and manage a flare,
when to rest and when to exercise,
advice on how to modify activities in order to protect the joints.
Physiotherapists can help by teaching and encouraging safe stretching and strengthening exercises to increase movement and strength, allowing better function.
Physiotherapists will also analyse the way you stand and walk, looking for whether it may be necessary to suggest, for example, balance exercises, insoles to reduce pain and restore good foot posture, or even a walking aid. Some physiotherapists will also have access to a hydrotherapy pool, where patients can do strengthening exercises while the water supports their joints.
Fatigue management and pain relief will also be considered, and non-drug treatment recommended.
Where Does Ra Happen
Rheumatoid arthritis is the most common form of autoimmune arthritis. This disease occurs because of a faulty immune response that causes the body to attack its own tissue. Specifically, RA attacks the lining, or synovium, of a joint, leading to swelling and eventually erosion in the joint itself over time.
While the causes of RA are unknown, there is strong evidence of a genetic predisposition to this disease.
Early on, rheumatoid arthritis typically affects smaller joints. In particular, the hand, wrist, and toe joints are commonly impacted. However, as the disease develops, larger joints and organs like the eyes, lungs, and heart can also be impacted.
Recommended Reading: Do I Have Carpal Tunnel Or Arthritis
Physical Therapist’s Guide To Rheumatoid Arthritis
Rheumatoid arthritis is a chronic inflammatory disease that affects approximately 1% of the United States population. RA often results in pain and inflammation in joints on both sides of the body, and can become disabling due to its effect on the immune system. A physical therapist can help manage the symptoms of RA, enhancing an individual’s quality of life.
Prevents Further Joint Damage
Physical therapists can assist in preventing further joint damage for patients with rheumatoid arthritis.
For instance
Patients can learn the following adaptations from physical therapists:
- Taking short breaks often to avoid developing pressure sores on the buttocks and heels from prolonged sitting.
- Wearing orthotics , such as sneakers with low-heeled soles that provide good arch support.
- Learning to use assistive devices, such as a cane or walker.
Read Also: Are Tomatoes Bad For You If You Have Arthritis
Hot And Cold Applications
Many physical therapists will recommend that patients use ice or heat ontheir joints, depending on their pain level and history with the disease. Iceis usually used for acute flare-ups, while heat is suggested to manage chronicsymptoms.
Heat relieves pain, reduces muscle spasms and enhances theelasticity of the joint tissues. Hot compresses or hydrotherapy may be used for10 to 20 minutes at a time, a few times a day. Applying heat can make thejoints more mobile and comfortable during exercise.
Cold can reduce discomfort. Cooling the joint alsodiminishes the negative effects of cartilage-destroying enzymes, which are moredamaging at higher temperatures.
Types Of Physical Therapy
Once you decide to seek a therapist for your rheumatoid arthritis, it can be confusing to make sense of your treatment options. Both physical therapy and occupational therapy can provide valuable benefits to people with this condition.
- Physical therapy typically addresses mobility problems during tasks like walking, transferring between positions , or climbing stairs.
- Occupational therapy tends to focus more on maximizing your independence by making activities of daily living like dressing, cooking, and bathing easier to accomplish.
Admittedly, there can be a lot of crossover in the treatment components between these two disciplines.
In addition, several different types of treatments may be performed during a PT or OT session. These interventions can generally be grouped into two categoriesâactive and passive:
- Active treatments require the patient to take a hands-on role. Examples of this include balance drills, strengthening exercises, and transfer or ADL practice.
- Passive treatments involve the therapist administering the intervention without an active patient component. Treatments in this category include massage, stretching, splint fabrication, and modalities like electrical stimulation.
You May Like: How To Treat Arthritis In Knee At Home
How To Manage Rheumatoid Arthritis With Physical Therapy
1. Relative Rest
Rest and energy conservation can assist with locally inflamed joints, but they should be avoided in the long run as it has the risk of negative side effects. Acutely, resting the affected joints can help with pain management and reduce inflammation in the joint. Reduced range of motion, loss of strength, altered joint-loading response, and diminished aerobic capacity are possible adverse consequences of inactivity.
2. Exercise
Individuals with rheumatoid arthritis might benefit substantially from a planned fitness regimen that improves their general well-being and function. Stretching, strengthening, and aerobic conditioning should be encouraged while conserving energy in such a program.
3. Stretching
Acutely inflamed joints should be rested to avoid worsening symptoms. Active or active-assisted stretching of the major joints is required for non-inflamed joints to prevent contracture formation and preserve the existing range of motion needed to conduct most daily tasks. Contractures are usually assumed to be prevented by once-daily range-of-motion exercises. Most notably, appropriate posture is required for bedridden patients to avoid joint contracture. Contracture treatment must be done safely so that overly severe stretching does not occur. Furthermore, the presence of a bony block as a causative component in the restriction of full joint motion must be ruled out.
4. Strengthening
5. Aerobic Conditioning
6. Superficial Heat
7. Deep Heat
8. Cryotherapy