What Are The Possible Side Effects Of Rituxan
Rituxan can cause serious side effects, including:
-
Tumor Lysis Syndrome : TLS is caused by the fast breakdown of cancer cells. TLS can cause you to have:
- Kidney failure and the need for dialysis treatment
- Abnormal heart rhythm
TLS can happen within 12 to 24 hours after an infusion of Rituxan. Your healthcare provider may do blood tests to check you for TLS. Your healthcare provider may give you medicine to help prevent TLS.
Tell your healthcare provider right away if you have any of the following signs or symptoms of TLS:
- nausea
- diarrhea
- lack of energy
Side Effects Of Infusion Therapy
As with any medication, there are potential side effects to infusion therapy with biologic DMARDs. These drugs work by inhibiting the immune system, an effect that can increase the risk of infections. The most common infections include:
- Upper respiratory infections
- Urinary tract infections
More serious infections can occur, especially in people who already have underlying conditions.
This administration of biologics can also lead to infusion reactions , which are most common after the first infusion. Most cases are mild and can be treated with antihistamines. Symptoms of an infusion reaction include:
- Itching
- Chills or fever
- Changes in blood pressure
In some cases, treatment with Rituxan can lead to reactivation of viral infections that are dormant in the body, such as hepatitis B infection. This can be prevented by screening for hepatitis B before beginning treatment.
Different Rheumatoid Arthritis Infusion Types
There are different medications used for infusion treatments. Each one targets, or turns off, a different part of the immune system. You and your doctor can decide which medication is best for you.
- Tocilizumab . This medication works by blocking interleukin-6 . IL-6 is a protein made in the immune system. It is used to reduce joint pain and swelling.
- Tumor necrosis factor inhibitors. Golimumab and infliximab are two biologics that work by inhibiting tumor necrosis factor . TNF is a protein found in the immune system. These medications are used to prevent joint damage. They may be prescribed for use in conjunction with methotrexate, an oral medication.
- Rituximab .This drug may also be marketed under the name Mab Thera. It works by targeting B cells. Rituximab is used to slow down the progression of joint and bone damage. Its often prescribed for use in conjunction with methotrexate.
- Abatacept . This treatment works by targeting T cells. It may help to prevent further joint and bone damage.
Infusion medications are expensive, and can cost upwards of $45,000 annually.
Many health insurance plans only cover one or two of the medications used for these treatments. You may have to take what your insurer is willing to pay for into account when you are deciding which type to get.
Recommended Reading: Rheumatoid Arthritis In Arms
How Effective Is Infusion Therapy For Ra
Rheumatologists may prescribe infusion therapy for arthritis treatment to people for various reasons including symptom alleviation. When opposed to oral drugs, many people like not having to take medication regularly and find the infusions to be a better experience.
Many people prefer infusion therapy to regular oral drugs because of the advantages it provides. These advantages include, but are not limited to, the following:
What Is Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune condition that affects the joints, skin, and blood vessels. When it affects the lining of the joints, it results in swelling and chronic pain. The aches increase and become worse as the illness erodes joint cartilage sometimes causing deformity. In addition to painful, swollen joints, other symptoms may include fatigue, stiffness, and loss of appetite.
You May Like: What Really Causes Arthritis
Who Shouldnt Take Them
Biologics may cause some dormant chronic diseases to flare. They may not be a good idea if you have multiple sclerosis or other conditions like severe congestive heart failure. Your doctor will give you a skin or blood test for tuberculosis before you start a biologic. You also need a test for chronic hepatitis B and C.
Although animal studies of biologics show they donât affect fertility or hurt the baby, they canât always predict what will happen to humans who take the drugs. Because we donât know how they affect a developing child, pregnant women should use them only if the need is great.
Your doctor will tell you to stop your biologic before surgery. You can start again when your wounds have healed and your chance of getting an infection has passed.
Show Sources
Pediatric Ulcerative Colitis Trial Study Design
The REMICADE® Pediatric Ulcerative Colitis trial was a multicenter, phase 3, randomized, open-label, parallel-group trial to evaluate the safety and efficacy of REMICADE® in pediatric patients aged 6 to 17 years with moderately to severely active UC and an inadequate response to conventional therapies. The primary objectives of the study were to evaluate clinical response after a 3-dose induction regimen of REMICADE® 5 mg/kg IV and the safety of REMICADE® during induction and maintenance regimens. Secondary objectives included the evaluation of 2 REMICADE® maintenance dosing regimens in maintaining remission, as measured on the Pediatric Ulcerative Colitis Activity Index the efficacy of a 3-dose regimen of REMICADE® in the induction of clinical remission, as measured by the Mayo score and the induction of remission, as measured on the PUCAI.1,5
All patients received induction dosing of REMICADE® 5 mg/kg IV at Weeks 0, 2, and 6. Patients who did not respond to REMICADE® at Week 8 received no further REMICADE® and returned for safety follow-up. At Week 8, 45 patients were randomized to a maintenance regimen of REMICADE® 5 mg/kg IV given either every 8 weeks through Week 46 or every 12 weeks through Week 42.1,5
Note: REMICADE® 5 mg/kg IV every 12 weeks is not an FDA-approved maintenance dosing regimen for REMICADE® in the treatment of pediatric patients with moderately to severely active UC.1
Recommended Reading: Arthritis Symptoms In Leg
Biologic Injections Vs Infusions
When you and your doctor decide that its time for you take a biologic drug to manage your arthritis, whether or not you take one thats injected or infused depends on a number of factors. Some drugs are available only as injections or only as infusions some are available in both formulations.
All of the medications are efficacious so its a shared decision between you, your doctor, and your insurance company, says Vinicius Domingues, MD, a rheumatologist in Daytona Beach, Florida and CreakyJoints medical advisor. Your doctor may recommend a specific biologic they think will be best for you. Your health insurance coverage may also influence which biologics you can take. In other cases, your personal preference about the following considerations may play a role:
- Your willingness to give yourself injections vs. having a health care provider administer infusions
- How close you live to an infusion center vs. the convenience of giving yourself medication at home
- How often you want to deal with taking medication: Injections are usually given weekly, every other week, or once a month infusions are given less often anywhere from monthly to once every six months, after you get up and running with the first few doses
- How much time you can spare: Injections take very little time to administer infusions can take hours
For patients who dont want to give themselves shots at home or freak out at the sight of a needle, Dr. Domingues notes, infusions are a good alternative.
I Trust It Gets Easier
I remember how terrified I was before each needle. My heart would be racing I would be sweating even in the coldest of months. Before my RA diagnosis I would often need to lie down before blood draws. However, exposure therapy over the years has helped me get through the intense feelings. Because Ive gotten through it before, I know I can get through it again. Working with a therapist and developing coping skills to help with anxiety helps so much during any uncomfortable medical procedure.
Read Also: Remedies For Arthritis In Back
What Are The Types Of Biologics
There are several. They include:
- B-cell inhibitor. They affect B cells, which are white blood cells that carry a protein that can trigger your immune response.
- Interleukin-1 blocker. Stops production of an inflammatory chemical your body makes
- Interleukin-6 or interleukin-17 blocker. Stops inflammatory chemicals from attaching to cells
- Blocks proteins that trigger the inflammation process
- T-cell inhibitor. Blocks communication between T cells, a type of white blood cell
- Tumor necrosis factor inhibitor. Blocks a chemical your body makes that drives the inflammation process
Sticking To Your Treatment Plan
A 2018 report in the journal Arthritis & Therapy found that 50% to 70% of people with RA were nonadherent with their recommended treatment plans. Nonadherence to treatment is one of the main reasons RA treatments fail.
Your rheumatologist has prescribed biologic drug therapy because they believe that the benefits outweigh the risks. The good news is that many of the newer biologic drugs are safe and effective.
If you feel you need to stop your biologic drug because of side effects, cost, or another reason, talk to your rheumatologist first. The decision to stop, change, or reduce the dosing of a drug should be made by you and your doctor, and not one you make alone.
Also Check: Medical Term For Joint Pain
Can I Stop Getting Infusions If I Go Into Remission
Dont stop any course of treatment unless or until your doctor tells you its clear. As of today, theres no cure for RA, Dr. Domingues says. The reason youre in remission is because of your therapy. Most patients who achieve remission do better when they stay on medication, though you and your doctor can discuss whether you can taper to a lower dose or less frequent schedule.
Patients who stop taking medication when they enter remission have a high potential for flaring again. This is also true if your infusion schedule gets off track for any reason.
Its essential to stay on your schedule, Nurse Luna adds emphatically. Any gap in treatment can really interrupt how you feel and affect the medications benefits. Shes had patients feel so great that they didnt think they needed the meds anymore. They stop coming on their own, to return months later even worse off than before. And then the medications might not work the exact same way again.
Dr. Domingues recommends being strict about keeping your infusion appointments. You may have to miss a week or two here and there life happens and sometimes you have to reschedule. But if you go more than a month past your scheduled infusion, you may have to do catch-up treatments. Im guilty of this and Ill never skip it again now that I know how bad it is for me. We dont want you to flare because it may be hard to go back to the good state you were in, he says.
How Long Before The Medication Starts Working
It depends on the medication and how you react to it. Some patients may notice an improvement within weeks of getting the first infusion, but it could take up to a couple of months before you start feeling noticeably better.
Some patients feel great after the first infusion, Luna says. Thats wonderful, Im not gonna argue with that. Just remember not to lose faith if you dont feel anything right away. Dr. Domingues says that if his patients arent feeling better after three infusions, he rethinks what were doing and considers another mechanism of action.
You May Like: What Can You Take For Arthritis In Your Fingers
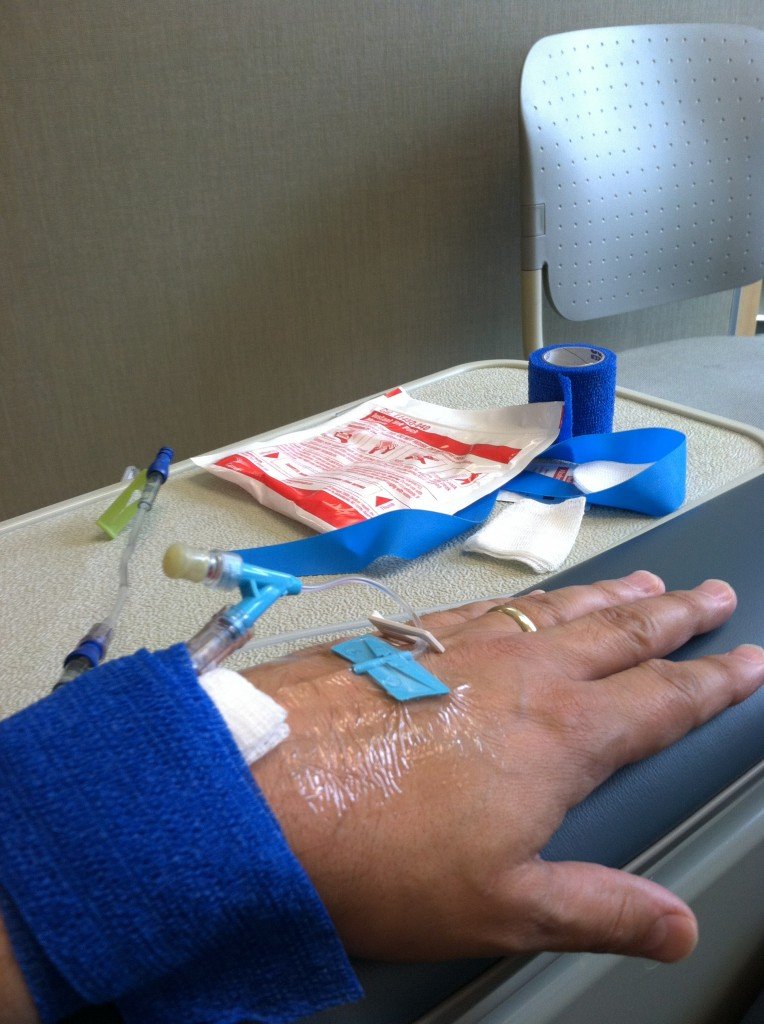
What To Expect During The Infusion
A doctor or nurse will check your temperature, blood pressure, and pulse before you start. They’ll monitor these vital signs throughout your treatment.
You’ll feel a pinch when they put a needle into your arm, but the infusion itself shouldn’t hurt. You may get medicine before your treatment to relax you if you’re nervous. While the medicine goes in, you can read a book or watch a movie.
I Distract Myself And Look Away
I never look at the needle when they place it in. Im pretty sure that would make my anxiety far worse. Another trick Ive been doing for years: I pinch myself or dig my nail into a finger or palm of my hand and focus on that sensation rather than on the needle going on. Another distraction I use is focusing on my breathing.
You May Like: Skin Rashes And Arthritis
Fda Approves A New Infusion Drug For Rheumatoid Arthritis
NBN Infusions provides a comprehensive nursing and pharmacy program that services patients of all ages from pediatrics to geriatrics. NBNs on-site, licensed pharmacy provides all required medications and equipment that patients will need for the duration of their home infusion therapy. Home Infusion Therapy involves the administration of medications using intravenous, subcutaneous and epidural routes. This care is administered to patients in the convenient and comfortable surroundings of their own home and allows them to take a more active role in their own health care. Home Infusion Therapy is not only more cost-effective than inpatient treatment, it eases the stress and anxiety of treatment resulting in better patient outcomes.
There are 1.3 million people in the United States that are currently living with Rheumatoid Arthritis, which is a chronic inflammatory condition. Symptoms include pain, stiffness and inflammation of the joints, which can sometimes lead to destruction of the joints and even disability in some cases. Although there are medications for the treatment of RA, there is no known cure for Rheumatoid Arthritis.
Due to the amount of people living with this condition there is always a driving need to develop better treatments, thats why the success of clinical trials are so exciting. One of the clinical trials that held so much promise may be in route to providing help to so many people in need.
Are There Any Severe Side Effects From Infusions
While rare, infusion reactions from Remicade can be severe and life-threatening, causing low blood pressure, swelling, restricted airways, and anaphylaxis, a severe allergic reaction.
Because biologic medication weakens your immune system, it can also increase your risk of getting an infection or reactivating a prior infection such as hepatitis B or tuberculosis.
Also Check: I Think I Have Arthritis
How Does Getting An Infusion Work Exactly
After being hooked up to an IV in your hand or arm, the medication will be infused into your body through a vein. You wont feel an immediate change in your pain or other symptoms. These are not pain relief medications, Nurse Luna explains. They are working on your immune system to reduce inflammation and with that reduction in inflammation, you will hopefully have pain reduction.
Which Infusion Medication Will I Get
Your doctor will discuss with you which biologic is most appropriate for your diagnosis. You should talk about the pros and cons of each as part of the . Biologics target different specific parts of the immune system. Your doctor may feel one drug is better for you than another because of how it works on the immune system.
- Golimumab and infliximab inhibit an immune system protein called tumor necrosis factor
- Abatacept blocks signaling to a different part of the immune system called a T cell
- Rituximab targets B cells
- Tocilizumab blocks an immune system protein called interleukin-6, or IL-6
The other big factor is your insurance. Your coverage may dictate a certain medication over another.
Read Also: Arthritis Articles
Having Needle Anxiety Is Tough When You Take Medication That Requires Monthly Intravenous Infusions Heres How Rheumatoid Arthritis Patient Eileen Davidson Learned To Get Through Infusion Day Without As Many Jitters
I know this may sound strange coming from someone who has dozens of tattoos, but I am afraid of needles. For some reason, I can stand the discomfort of getting inked, but when my need for needles is related to bloodwork or medical procedures, it gives me a lot of anxiety.
Many people ask me if my tattoos hurt. The truth is that the pain from tattoos and piercing is temporary, whereas the pain from my rheumatoid arthritis is consistent, as is the need for regular bloodwork and infusions that require me to frequently face my needle fear and anxiety.
I would rather get tattooed than get any medical procedure, especially one that requires needles.
But living with rheumatoid arthritis has forced me to confront this fear, or at least develop some strategies for coping with it.
To even get diagnosed with RA meant dealing with needles, as I needed to work up courage to get the bloodwork that would reveal the antibodies and inflammation driving my rheumatoid arthritis pain. What I didnt expect was how that test would lead to regular bloodwork, self-injections, and IV medications for the rest of my life.
It hasnt been easy adjusting to life with RA for many reasons, and dealing with my needle issues is just one of many. But I actually look forward to my IV infusion days now, even though I still have to overcome some of my needle fears officially called trypanophobia as I approach my monthly infusion appointments.