Related Faq For How Long Does A Arthritis Flare Up Last
How long do rheumatoid arthritis flare ups last?
How long do RA flares last? The length of time an RA flare lasts can vary widely, from a few hours to several days or weeks. If a flare does not improve after 7 days, it may be a good idea to contact a physician. The doctor may suggest adjusting the person’s medication.
How long do autoimmune flare ups last?
Depending on the severity of the natural stressor that is causing the flare-up, symptoms can last anywhere from a few days to several months. For some autoimmune disease sufferers who are not receiving treatment, symptoms of an acute flare-up may subside on their own without medical intervention after one or two weeks.
Does arthritis ever stop hurting?
Overview. Many people who have arthritis or a related disease may be living with chronic pain. Pain is chronic when it lasts three to six months or longer, but arthritis pain can last a lifetime. It may be constant, or it may come and go.
Which is better for arthritis heat or cold?
Heat can relax muscles and help lubricate joints. Heat therapy may be used to relieve muscle and joint stiffness, help warm up joints before activity, or ease a muscle spasm. Cold can reduce inflammation, swelling, and pain related to arthritis and activity.
Is it good to put heat on arthritis?
Heat and cold.
Does squeezing a ball help arthritis?
What does arthritis in legs feel like?
What is the most painful form of arthritis?
What is the most painful arthritis?
Defining This As Uncontrollable Flare
This occurs with clusters of unprovoked, persistent symptoms that are not normal for their RA :
Well, definitely, my joints are swelling a lot more, but its lasting a lot longer, I get more pain, more fatigue, like Im having to make myself move
I would describe it as an attack , the sudden, unexpected occurrence. BANG! there it is. Without having exerted myself, for no reason
It doesnt go away as easily or readily, or the things that you normally do to make it go away dont seem to ease it
I knew it wasnt normal. It was now impacting my life. It was impacting what I could do, I didnt want to do anything. I was exhausted, I didnt want to go anywhere. It hurt. Everything just ached .
How Is Jia Treated
When JIA is diagnosed early and treated appropriately, it can usually be managed effectively. There’s no cure, but there’s a lot doctors can do to ease the symptoms of JIA and prevent or limit damage to joints.
For some people, taking medications like ibuprofen or naproxen can help reduce inflammation. Some patients need to take a weekly medication called methotrexate. Newer medications such as etanercept, adalimumab, abatacept, and tocilizumab can keep the immune system in check and control the disease far better than was possible a few years ago. For arthritis flare-ups, doctors may also use medicines called corticosteroids , but they try to limit these to avoid side effects.
Physical therapy exercises that improve flexibility and the use of heat can help people with JIA control symptoms. It’s rare that joints get damaged in a person’s teens, but surgery can repair damaged joints if needed.
Read Also: Is Peanut Butter Bad For Arthritis
What Causes Gout To Flare Up
Gout is a complex form of arthritis that can flare up suddenly and severely. It occurs as a result of having high levels of uric acid, which makes it easier for urate crystals to form. These sharp crystals can deposit in your joints, causing inflammation, swelling and pain.
“The most common trigger of gout is eating purine-rich foods, since high levels of purines can increase the amount of uric acid in your bloodstream,” explains Dr. Alam.
Gout-sufferers can help avoid flare-ups by avoiding foods rich in purines, including:
- Red meat
- Certain types of seafood, including tuna, scallops and trout
- Alcohol, particularly beer
- Fruit juices and other beverages that contain fructose
“Similar to rheumatoid arthritis, a flare-up of gout can be alleviated by using a cold compress on the affected joint, which helps reduce the inflammation that’s causing your pain, swelling and stiffness,” says Dr. Alam.
What Causes An Arthritis Flare
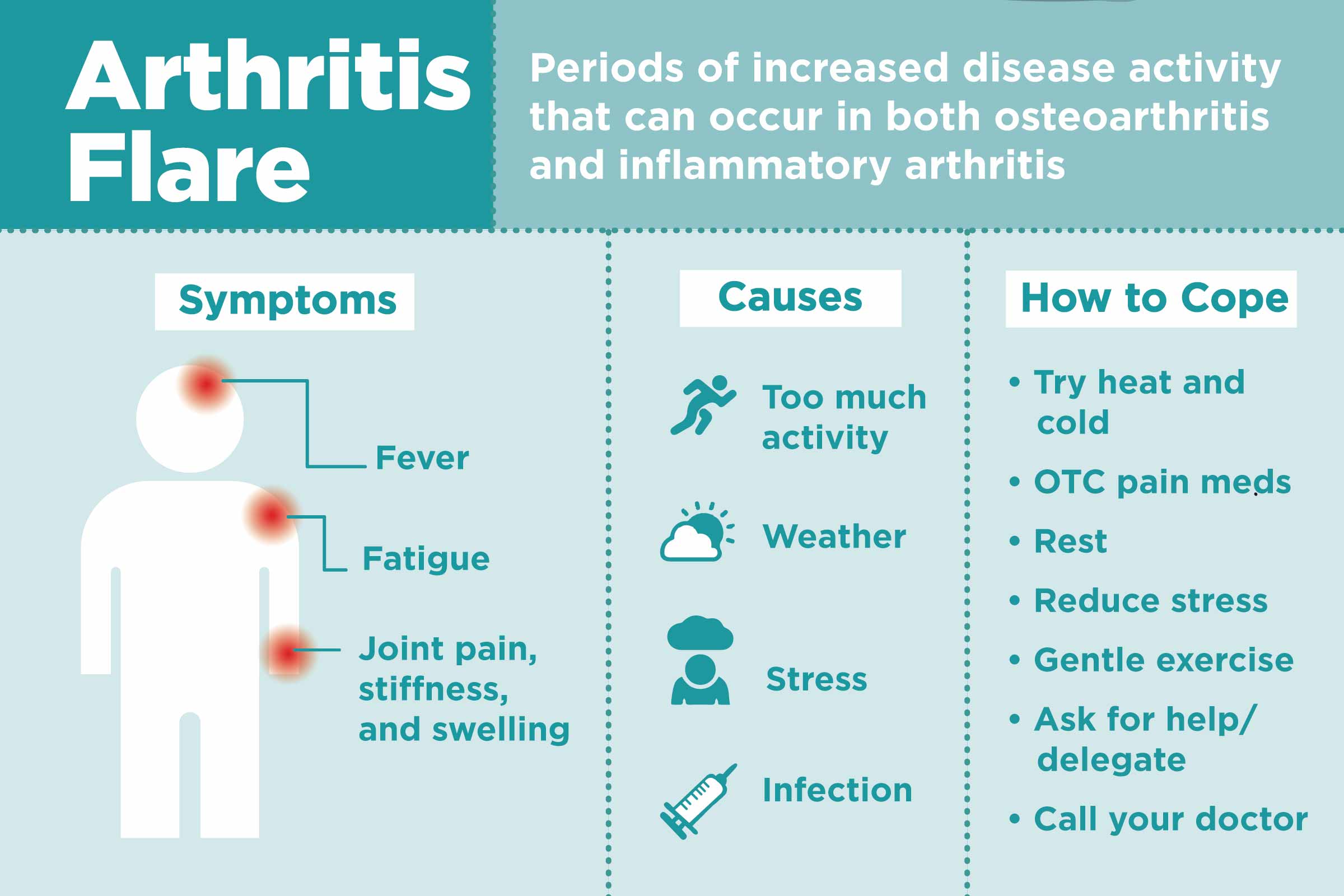
An arthritis flare-up can happen after a change in the weather, after an injury, or in response to a change in activity level. Anytime youre increasing your activity or doing something new, you could be at risk of having an arthritis flare-up, Clark said. Patients sometimes tell me that their joints feel worse after they do a lot of snow shoveling or yard work, for example.
Read Also: Does Arthritis Always Show Up In Blood Tests
Follow Your Healthcare Provider’s Advice
Because arthritis flares are somewhat inevitable, you should know what your healthcare provider wants you to do when a flare occurs. Have a conversation with your healthcare provider ahead of time. Flares are typically inconvenient, meaning they can occur during the night or on the weekend when your healthcare provider is unavailable.
Know the maximum limits of your pain medication. Discuss whether you should always have a backup on hand or ready to be refilled. Know what your healthcare provider wants you to do.
Does Osteoarthritis Pain Come And Go
The main symptoms of osteoarthritis are pain and stiffness in your joints, which can make it difficult to move the affected joints and do certain activities. The symptoms may come and go in episodes, which can be related to your activity levels and even the weather. In more severe cases, the symptoms can be continuous.
Don’t Miss: Peanuts And Arthritis
What Are The 5 Worst Foods To Eat If You Have Arthritis
Foods to stay away from
- Trans fats are unhealthy fats. Trans fats should be avoided because they can cause or exacerbate inflammation and are harmful to your heart.
- Gluten is a protein that is used in many foods Gluten avoidance is more than just a fitness fad there are compelling reasons to do so.
- White Sugar & Refined Carbs
- Beans are a type of legume.
- Fruit of the citrus family.
When To Get Medical Advice
See a GP if you think you have symptoms of rheumatoid arthritis, so they can try to identify the underlying cause.
Diagnosing rheumatoid arthritis quickly is important, because early treatment can prevent it getting worse and reduce the risk of joint damage.
Find out more about diagnosing rheumatoid arthritis.
Read Also: Arthritis Pain In Hands Relief
How Fast Does Osteoarthritis Progress
Generally, radiological lesions gradually and slowly increase. However, the pace of this progression can be very variable. In extreme cases, some cases of osteoarthritis may remain stable for decades, while others progress very rapidly to complete destruction of the cartilage in the space of a few months.
What Happens When Someone Has Jia
People with JIA may have pain and stiffness that can change from day to day or from morning to afternoon. These symptoms can come and go. When the condition becomes more active and the symptoms worsen, it’s known as a “flare” or a “flare-up.”
JIA often causes only minor problems, but in some cases it can cause serious joint damage or limit growth. Although JIA mostly affects the joints and surrounding tissues, it can also affect other organs, like the eyes, liver, heart, and lungs.
JIA is a condition, meaning it can last for months and years. Sometimes the symptoms just go away with treatment, which is known as remission. Remission may last for months, years, or a person’s lifetime. In fact, many teens with JIA eventually enter full remission with little or no permanent joint damage.
Page two
Don’t Miss: Rheumatoid Arthritis In Shoulders And Neck
How Is Rheumatoid Arthritis Treated
The goals of rheumatoid arthritis treatment are to:
- Control a patient’s signs and symptoms.
- Prevent joint damage.
- Maintain the patients quality of life and ability to function.
Joint damage generally occurs within the first two years of diagnosis, so it is important to diagnose and treat rheumatoid arthritis in the window of opportunity to prevent long-term consequences.
Treatments for rheumatoid arthritis include medications, rest, exercise, physical therapy/occupational therapy, and surgery to correct damage to the joint.
The type of treatment will depend on several factors, including the person’s age, overall health, medical history, and the severity of the arthritis.
Going Through The Peak Of A Flare

A dramatic worsening of pain marks the peak of a flare. This pain may be characterized as burning or stabbing and may affect different muscles and joints simultaneously. During the peak of a flare, you may find it difficult or impossible to sleep soundly. With a lack of sufficient rest, you may not be able to concentrate or function normally. This loss of normal functioning can affect every facet of life, from meal preparation to grooming and hygiene. Consequently, flares may be accompanied by a loss of weight and neglect in appearance.2
Recommended Reading: How To Get Rid Of Arthritis In Wrist
What Is A Rheumatoid Arthritis Flare Up
A rheumatoid arthritis flare up describes a short-term escalation of your RA symptoms. A flare up can subside within a day or two, or it can persist for several weeks or months.
An RA flare up generally involves joint stiffness and pain, although it can manifest itself as a worsening of any symptom. If the flare up is especially severe, it can affect your ability to perform your everyday activities.
Ai Mukai, MD, a physiatrist with Texas Orthopedics Sports and Rehabilitation in Austin, Texas, emphasizes that RA flare ups are a known part of rheumatoid arthritis and its course and symptoms. Dr. Mukai, who possesses board certifications in pain medicine and physical medicine & rehabilitation, is also a SpineUniverse Editorial Board member.
Inflammatory Arthritis Versus Osteoarthritis
Knowing the type of arthritis, you have is the key to recognizing and managing a flare up. Osteoarthritis is the most common type of arthritis. It is caused by wear and tear of the cartilage linings of your joints. Since wear and tear takes time, this type occurs mostly in older people. It may be more common in a joint that you injured at some time. It causes pain, stiffness, and swelling, but not inflammation.
Inflammatory arthritis may be caused by a disorder of your immune system. Your immune system is your bodys defense system against foreign invaders like germs. If you have an immune system disease called an autoimmune disease, your immune system attacks normal body tissues, including your joints. The symptom of the attack is inflammation of tissue in around your joints.
Autoimmune inflammatory arthritis affects many joints all over your body at the same time. This is also called inflammatory polyarthritis. This type of arthritis is a long-term disease that is often diagnosed in young adults. Both rheumatoid arthritis and psoriatic arthritis are common types. Inflammation adds symptoms of redness and a feeling of warmth to affected joints along with pain and swelling.
Also Check: Arthritis Pain Feels Like
What Triggers Osteoarthritis Flare
Flare-ups can be caused by several factors. However, the most common triggers of the episodes are overdoing an activity or trauma to the joint. The following are some of the primary risk factors associated with OA flare-ups:
Too much activity
When you feel good about a physical activity you are doing, there is a high chance of overdoing it and creating the perfect conditions for a flare-up. OA often flares after overexertion of the joint or joints involved in vigorous physical activities.
Weather
Pressure changes and humidity can also lead to increased joint pain in persons living with osteoarthritis. Patients with OA and other types of arthritis or inflammatory conditions often complain that their joints are achier in cold and humid weather². However, studies are not conclusive on the relationship between flare-ups and the weather.
Infection
Infections that affect the immune system, including respiratory viruses, can also cause OA flare-ups.
Stress
Several studies³ reveal stress can induce OA flares. Typically, stress leads to the production of high amounts of pro-inflammatory cytokines responsible for worsening OA symptoms.
Injury
If you have suffered an injury to the part of the body affected by OA, you may suffer a flare-up as the symptoms will be aggravated by the injury.
Weight gain
Rapid weight gain can trigger flare-ups due to the relatively sudden and large increase in weight that the joints need to support.
What Is An Arthritis Flare
Summit physician assistant Abby Clark, PA-C, explains the term arthritis flare-up and shares what you can do when you experience one.
Arthritis is a common and painful condition that happens when a joints cartilage wears away. Without cartilage to cushion the joint and act as a buffer, the bones can rub together. This causes pain, stiffness, and inflammation. Its a chronic condition that can make everyday activities difficult. But what does it mean to have an arthritis flare-up?
An arthritis flare-up refers to an acute increase in pain, swelling, and stiffness in an arthritic joint, said Abby Clark, PA-C, one of Summits physician assistants. Its a worsening of the chronic symptoms that people generally have.
During an arthritis flare-up, you have more disability associated with that joint. Your symptoms are worse, and youre less able to do the things you normally would, whether thats climbing stairs or playing tennis.
Recommended Reading: How To Diagnose Arthritis
Signs Of A Rheumatoid Arthritis Flare
Whats more, people with rheumatoid arthritis have different receptors on their immune cells MHC receptors which are more likely to bind to self-proteins, explains Ashira Blazer, MD, a rheumatologist at New York University’s Langone Medical Center in New York City. Environmental triggers can aggravate the immune system and cause these proteins to end up in the joint space, which can lead to inflammation and damage. Also, during a flare, antigens make their way into the joints, and when immune cells in the joints become activated, the linings of the joints become inflamed. The result: Red, hot, tender, swollen joints signs of a flare.
Previously She Had Experienced Joint Flares But Then A Severe Whole Body Flare ‘crept’ Upon Her
Many flares came on without warning, but overuse of or trauma to a particular joint could produce a joint flare. Other flare triggers included cold or hot weather, getting too cold, stressful situations and certain types of food .Flares reduced general mobility and affected walking, eating and personal care. They also disturbed sleep.People found relief from the symptoms of a flare in many different ways. Changing medication included increasing the dose of painkillers, anti-inflammatories or steroids and if the flare persisted people had steroid pulses/injections and joint injections . Getting rest and sleep and using heat or cold were most often used. Some people said that hot baths, hot water bottles, electric blankets, heat pads and putting affected joints, e.g. hands, in hot water worked for them. However another group of people we interviewed felt that keeping joints cool if they were hot and swollen was the answer. People used ice, cold water, cold wet towels, cooling foot cream and wet wipes. One man described the relief he got for his hands. TENS machines, wrist splints, a supportive foam knee cushion and rubbing Tiger Balm on joints and fasting for 48 hours were also mentioned.
Recommended Reading: Rheumatoid Arthritis Medicine Side Effects
Related Faq For How Long Does A Gerd Flare Up Last
What are the usual signs and symptoms of GERD how will it be managed?
A burning sensation in your chest , usually after eating, which might be worse at night. Chest pain. Difficulty swallowing. Regurgitation of food or sour liquid.
When should I worry about GERD?
If you have any of the following heartburn or gastroesophageal reflux disease symptoms or conditions, contact your doctor. Your heartburn symptoms have become more severe or frequent. You are having difficulty swallowing or pain when swallowing, especially with solid foods or pills.
Can GERD cause shortness of breath?
Shortness of breath, also called dyspnea, occurs with GERD because stomach acid that creeps into the esophagus can enter the lungs, particularly during sleep, and cause swelling of the airways. This can lead to asthma reactions or cause aspiration pneumonia.
Can GERD make you feel ill?
Nausea and GERD
Partnered with difficulty swallowing, coughing, and belching with GERD, many patients feel nauseated or experience vomiting. Indigestion has also been reported by some patients.
What do doctors recommend for GERD?
Your doctor may prescribe one or more medicines to treat GERD.
Can GERD cause chest tightness and shortness of breath?
Can acid reflux cause chest pain for days?
What does GERD feel like in your chest?
Does GERD cause headaches?
Can GERD cause a runny nose?
What Is Knee Osteoarthritis

4.1million people in England have osteoarthritis of the Knee. 18% of the population aged over 45 years old has the condition.
Arthritis Research UK suggest that only 18% of people with arthritis have a care plan to help them manage their symptoms. Sub-optimal management of osteoarthritis permits people to suffer symptoms unnecessarily.
Not everyone who has arthritis will suffer with symptoms, but those that do can experience pain, stiffness, reduced mobility and function. The experience of OA is often unique to each individual.
Some people may just have pain, whereas others may simply have stiff joints. Typically, symptomatic people with knee OA will have a combination of symptoms. Stiff knees often hinder daily functional tasks like walking, getting in and out of the bath or car, and putting on shoes .
Recommended Reading: What’s Good For Arthritis In Your Hands
Question: How Long Does A Camping Flare Last
To the question how long does a flare last? the answer is that they can persist for weeks or months unless there is a change in treatment. Usually your symptoms are reliable indicators of an arthritis flare, so it is important to keep tabs on them, as well as what you are doing to treat your arthritis.