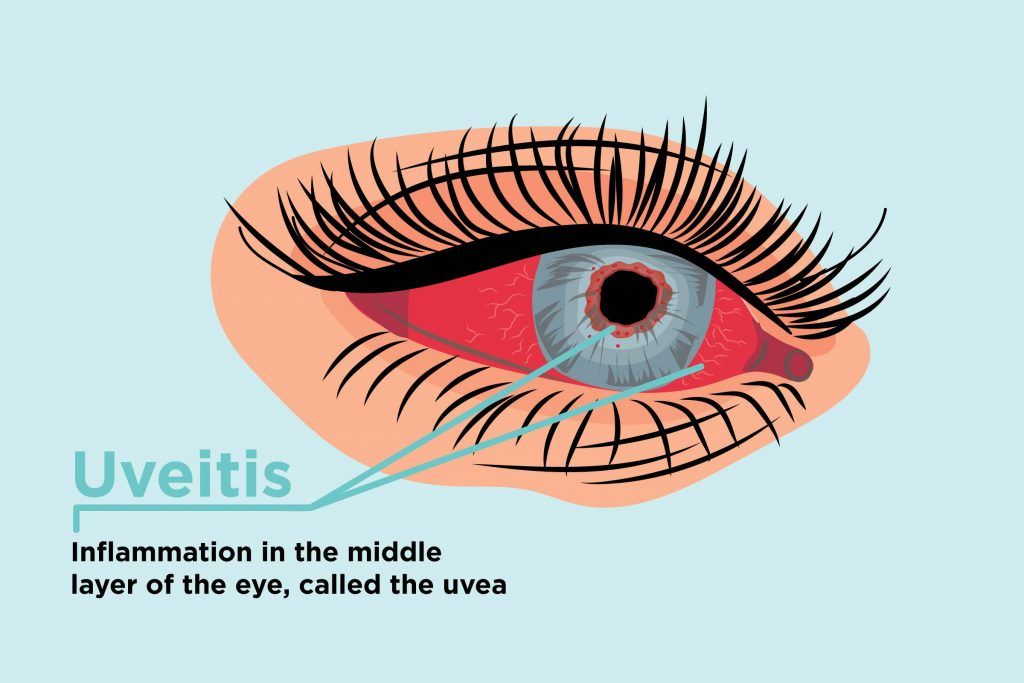
Eye Concern #: Vision Issues And Floaters From Uveitis
Below the episclera and sclera layers of the eye is another layer called the uvea, and when inflammation occurs here its known as uveitis. There are two types: Anterior uveitis, at the front of the eye, and posterior uveitis, which is at the back of the eye and very rare. Patients with uveitis start having vision problems and seeing floaters around the eye, says Dr. Bhatt. They may also experience redness and pain. Symptoms can have a quick onset and also worsen rapidly.
How Does Rheumatoid Arthritis Affect The Eyes
The main ways in which RA can affect your eyes are:
- Keratoconjunctivitis Sicca : The inflammation that RA causes can negatively affect tear glands, reducing fluid secretion resulting in dryness. The symptoms include a feeling of dirt or debris in the eyes, redness ad blurred vision.
- Scleritis: In this condition, RA causes inflammation on the sclera , which becomes thinner with the swelling and can easily split with a minor injury. It is more likely to happen among people between 40 to 70 years old. Symptoms of scleritis include reddening that does not fade, itchiness, sporadic vision problems, pain and swelling.
- Uveitis: In Uveitis, RA causes inflammation in the uvea. Uvea is the vascular section of the eye found between the retina and the sclera. Symptoms of the condition include pain, redness, light sensitivity, and blurred vision.
The different eye conditions that RA causes call for immediate doctor’s attention and treatment. Left unchecked, they could easily cause scratching, scarring, and even ulceration of the cornea. These or other negative effects of the conditions can lead to loss of vision.
How Rheumatoid Arthritis Can Affect Your Eyes
Rheumatology Symptoms
Rheumatoid arthritis can create a lot of severe impacts on your body. This inflammatory condition is commonly found to affect the joints, but it might also affect different other body parts including your internal organs.
The most significant organ affected by rheumatoid arthritis is your eyes. This condition can lead to a lot of issues that can affect your eye health, especially, if it is left untreated.
Apart from the common rheumatology symptoms including swelling, pain, and inflammation in the joints, you have to look for other symptoms in various body parts like skin, eyes, etc. to know the progress of rheumatoid arthritis. This condition will usually affect other body parts apart from your joints when it becomes severe.
Recommended Reading: Rheumatoid Arthritis Longterm Effects
The Importance Of Regular Eye Care With Arthritis
Its critical for anyone with inflammatory arthritis to get regular preventive eye care and to let your rheumatologist or eye doctor know if youre having new or unusual eye-related symptoms, no matter how minor they may seem. Annual dilated eye exams at the eye doctor are important to check for underlying damage early on. Some eye diseases might not cause a lot of pain or much change in vision, especially in earlier stages, so an eye exam is always necessary, Dr. Akpek says.
Dr. Wu requires annual exams from her inflammatory arthritis patients if there are no issues and wants to see patients more frequently if there are any problems.
All of the physicians we interviewed stressed the importance of fostering communication between rheumatologists and ophthalmologists. As a patient, you can help make sure your health care providers are sharing medical records and are up to date on any new symptoms, diagnoses, or treatment changes. Dont ever assume one doctor knows what the other does.
Ra Eye Problems: What Eye Problems Result From Rheumatoid Arthritis
Rheumatoid arthritis is a disease that is probably best known for affecting your joints. If you suffer from RA, you are most likely working through those symptoms with your doctor. However, sometimes this chronic inflammatory autoimmune disease can affect other parts of your body too. Ana-Maria Orbai, MD, a Rheumatology specialist at Johns Hopkins University School of Medicine states that RA can be extra-articular, meaning they affect parts of your body outside of the joints. Did you realize that the issues you are experiencing with your eyes can be actually caused by RA? We will discuss the ways that it can affect your eyes and what you should do to protect yourself.
You May Like: Best Thing For Arthritic Knees
Can Medications Like Hydroxychloroquine That Treat Autoimmune Diseases Cause Eye Damage
Hydroxychloroquine is a medication used to treat many autoimmune diseases. It can be very effective, with few side effects. Rarely, hydroxychloroquine can cause damage to the cells in the macula the center of the retina and hurt your vision. This problem, called hydroxychloroquine maculopathy, is more likely if youre taking higher doses for 5 years or more. If youre taking hydroxychloroquine, you should have regular eye exams to watch for early signs of hydroxychloroquine maculopathy.
Steroids are often prescribed to control autoimmune diseases. Steroids work very well in most cases and rarely cause serious side effects if used short term. However, they have many side effects if used long term. Steroids can cause problems with the eyes like cataracts and glaucoma.
The Structure Of The Eye And Where Arthritis Strikes
The eye is a complicated structure. Different types of arthritis can cause different types of eye problems. Its important to understand some general eye anatomy:
The entire eye is covered by a white outer coat called the sclera. The sclera is covered by a thin semi-transparent mucous membrane that has blood vessels, which is called conjunctiva.
At the very front of the eye is the cornea, which is the transparent layer that transmits and focuses light.
Behind the cornea is the iris, which is the colored part of the eye that helps regulate the amount of light that enters the eye like the diaphragm of a camera. The pupil is the dark hole in the middle of the iris, which adjusts in size to let in more or less light.
Just behind iris and pupil is the lens, which is like the lens of the camera. The lens is suspended in the eye cavity through some fine fibrils that attach to the ciliary body.
The back of the eye contains these important structures:
- Choroid: A layer that contains blood vessels, located between the sclera and retina
- Retina: A nerve layer that lines the back of the eye it creates electrical impulses from light that are sent to the brain via the optic nerve
- Macula: An area in the retina with special light-sensitive cells
- Optic nerve: A bundle of nerves that transmits visual messages from the eye to the brain
Don’t Miss: Side Effect Of Arthritis
Eye Concern #: Retinal Toxicity
Cruel irony: Some of the medications that we use to treat rheumatoid arthritis can potentially cause eye problems, says Dr. Feinberg. One top culprit? Quinolines , which are classified as anti-malaria drugs but are commonly used for RA because they treat inflammation. They can build up in the eye and affect vision or even damage the back of the eye and cause loss of vision, Dr. Feinberg explains, a condition called retinal toxicity.
Can Rheumatoid Arthritis Affect Your Eyes
Medications and Treatments23 Jun 2018 Michael M. Hall
Any inflammatory condition that affects collagen â the main component of connective tissue â such as rheumatoid arthritis , can affect the sclera (the white of .The same inflammation that damages your joints can also affect your eyes. Here’s how to protect your vision.Did you realize that issues you are having with your eyes can be an effect of RA? We will discuss the ways that it can affect your eyes and what you should do to .in a few people with rheumatoid arthritis less than 5% the disease makes their eyes red, painful, or dry..rheumatoid arthritis can affect the eyes in several ways. inflammation of the episclera, a thin membrane that covers the white of your eye, is common.It is common for RA to affect the eyes. About 30% to 40% of people. RA can cause inflammation in other parts of the eye, including: Scleritis: inflammation of the .Rheumatoid arthritis causes inflammation and is a systemic disease meaning it can affect the entire body. As it relates to the eye, rheumatoid arthritis may lead to .Having rheumatoid arthritis can put you at a higher risk of developing other. Carpal tunnel syndrome Widespread inflammation Joint damage. Scleritis can cause eye redness and pain, whereas Sjogren’s syndrome can cause dry eyes.How Juvenile Rheumatoid Arthritis Affects the Eyes. Although it might not seem possible, a disease that affects the joints can sometimes also affect the eyes.
Recommended Reading: Rheumatoid Arthritis Sores
Most Common Eye Problems With Ra
The inflammation of RA can do a lot of damage to your eyes, but so can a lack of tear production, and even the medication you use to treat your condition. Therefore, there are some uncomfortable eye problems you should watch out for and never ignore.
Dry Eye Syndrome
Probably the most common eye problem that affects RA sufferers, dry eyes can be a mild irritation or a precursor to a serious problem. A lack of lubricating tears can make it feel like you have dirt in your eye, or a mild burning, and you may be more sensitive to light. Once the cornea begins to dry out, your vision may become blurry.
A healthy coating of natural tears not only keeps your eye moist and comfortable, it also protects against infection. Since medications are sometimes to blame for dry eyes, it may be worth looking into switching to another drug.
If your doctor detects Sjögrens syndrome an inflammatory disease that can occur alongside RA good anti-inflammatory management and hydrating eye drops can help bring the symptoms under control.
Scleritis
RA can cause the whites of your eyes to thin, which sets the stage for serious trauma if you were to get a scratch or any foreign object lodged in your eye. The most obvious symptom of scleritis is redness over the white part that wont go away, but it often brings severe pain and vision problems, too.
Corneal Infection
Common Vision Complications Associated With Rheumatoid Arthritis
The underlying cause of rheumatoid arthritis is a problem with the immune system. Rather than just attacking bacteria or viruses, this body system may begin to attack the synovium, which is the membrane lining your joints. This leads to chronic inflammation, which can damage the cartilage and bone underneath, eventually destroying these tissues. Joints will lose their shape and alignment, which can cause your fingers to become crooked, stiff, and painful.
Your immune system may attack tissues associated with your eyes too, leading to vision problems. About 25 percent of people who have rheumatoid arthritis will develop an eye problem.
- Chronic dry eye, or conjunctivitis sicca, occurs in 15 to 25 percent of people with RA.
- Sjogrens syndrome can occur as a secondary autoimmune disease if your body attacks glands that produce tears or saliva.
- Episcleritis, or redness in your eyes from inflammation that produces discomfort but not pain, occurs in about 5.6 percent of people with RA.
- Scleritis is a more severe form of redness due to eye inflammation that particularly affects people between 40 and 70 years old with RA. Around 6.7 percent of people with RA develop this painful condition.
- Uveitis can occur, which is when the pigmented part of your eye becomes inflamed.
- Conjunctivitis, or inflammation of the white part of the eye due to an infection, is common in those with RA.
- Keratitis, when the cornea becomes inflamed and damaged, can occur.
Also Check: Can Arthritis In The Knee Be Cured
Rheumatoid Arthritis And Your Eyes
While rheumatoid arthritis primarily affects the joints, it can also affect other body parts, including the eyes. The main reason the eye is susceptible to rheumatoid arthritis is that most of its parts are made of collagen. Thus, any disease affecting the collagen, which RA does, will affect the eyes. The sclera and the cornea are entirely collagen.
Treating Dry Eye Syndrome
In good news, dry eye syndrome is relatively easy to treat with moisturizing eye drops and eye ointments at night, says Dr. Feinberg. Mainly we use over-the-counter drops they dont have to be prescription. He recommends choosing a brand thats free from preservatives to avoid irritating the eye further. If over-the-counter fixes arent doing the job, there are prescription medications that stimulate the glands to produce moisture, such as Salagen or Evoxac .
Also Check: Ra Pain In Hands
Ways Rheumatoid Arthritis Can Affect Your Eyes
Most people think of Rheumatoid Arthritis as a joint disease. But did you know that RA often causes eye complications that may result in inflammation, pain, and even loss of vision?
Unfortunately, its true. But being informed about the danger to your eyes can help you manage complications before its too late.
Clinical Trials Impacting Management Of Scleritis
The clinical trials for scleral inflammation utilize the following grade scale after the application of 10% phenylephrine drops, 0 , 0.5+ , 1+ , 2+ , 3+ , and 4+ .
A total of 17 studies are registered for scleritis.
Sirolimus sub-conjunctival injections for autoimmune scleritis, was a phase 1/2, single-center, open-label, non-randomized, prospective pilot study. Sirolimus is a macrocyclic lactone antibiotic with immunosuppressive properties that leads to inactivation of T cells. Sirolimus binds to the same intracellular receptor as tacrolimus and cyclosporine, but does not inhibit calcineurin, but rather blocks the âmammalian target of rapamycinâ which interrupts signaling pathways for several cytokines and growth factors including IL-2. Five participants with scleral inflammatory grade of â¥1+ received a baseline injection. The primary outcome was a 2-step reduction or reduction to zero in scleral inflammation by eight weeks. All participants met the primary outcome by week 8 however, 3/5 patients experienced flares requiring re-injection. No systemic toxicities were observed. Two participants experienced a localized sterile inflammatory reaction at the site of the injection which resolved without complication .
Tofacitinib, a selective inhibitor of the Janus kinase family inhibits JAK 1, JAK2 and JAK3. A phase 2 intervention model utilizing 11mg of tofacitinib was initiated in January 2019 to treat inflammatory eye disease including scleritis and/or uveitis .
Read Also: Arthritic Knee Symptoms
Eye Concern #: Dry Eye Syndrome
Dry eye syndrome is the most common eye condition among RA patients, with research suggesting as many as 46 percent experience it. It occurs when inflammation in moisture-producing glands causes them to stop secreting fluid. Patients have irritated, itchy eyes, or a sandy, gritty feeling in the eye, says Howard L. Feinberg, D.O., a professor of rheumatology at Touro University California College of Osteopathic Medicine. They think its a nuisance, but dry eye can cause a lot of damage, including scratches and thinning on the eyes surface, and scar tissue that could block vision.
Cataracts & Glaucoma: Vision Problems Linked With Rheumatoid Arthritis
Everyone should go to regular appointments with their optometrist, but if you are diagnosed with rheumatoid arthritis, you may need to go more often. Two chronic eye diseases, cataracts, and glaucoma are more likely to develop if you have rheumatoid arthritis. If your optometrist or ophthalmologist can diagnose these diseases early, they can help you maintain your sight with treatment.
- Cataracts: This is a condition in which damaged proteins in the lens of your eye bunch together, creating darker spots, cloudy film, or white clumps of material. As they grow larger, these obstruct your vision. Eventually, your lens must be removed and replaced with an artificial lens.
- Glaucoma: This eye disease is caused by damage to the retina from high fluid pressure in your eye. You will develop spots of lost vision or poor peripheral vision. Over time, these become tunnel vision as your retina degenerates. Glaucoma is treatable with special eye drops that lower your fluid pressure, laser surgeries to relieve fluid pressure, or more permanent shunts that allow for ongoing drainage in your eye.
RA may damage the tissues of your eyes because your cornea and sclera are made from collagen, just like your connective tissues. This is what the autoimmune disease attacks.
Recommended Reading: Rheumatoid Arthritis Medicine Side Effects
Ra And Your Eyes: What You Need To Know
Rheumatoid arthritis is known for joint pain, but it can also affect other parts of the body, including your eyes. Learn which rheumatoid arthritis symptoms and eye issues are most common, and how to manage them.
Most people think of rheumatoid arthritis as a joint disease, but like other autoimmune disorders, it can impact different areas of the body as well. One of the more common complications for people with rheumatoid arthritis is eye problems, which can lead to corneal damage and ultimately impact vision if left untreated.
Some common eye conditions, like the ones described below, may affect people with rheumatoid arthritis . But there are steps to take to safeguard eye health and avoid permanent damage.
Dry Eyes
RA can be associated with extra-articular manifestations, and dry eyes are one of the most common problems, says Ana-Maria Orbai, MD, instructor of medicine in the division of rheumatology at the Johns Hopkins University School of Medicine in Baltimore. A person with dry eyes might experience itching, a sand-like sensation in the eyes, and redness. They may also notice a lack of moisture or tears in the eyes, as well as blurred vision.
If you decide to go the over-the-counter route, avoid eye-drop products that have preservatives or vasoconstrictive agents, such as some from Visine and Clear Eyes, which often promise to relieve redness or take the red out, Orbai explains.
Eye Conditions And Jia
Juvenile Idiopathic Arthritis is an inflammation of the joints that occurs in children. It is also known as Juvenile Rheumatoid Arthritis .
Patients with JIA are at risk for an inflammation inside the eye, a condition known as iritis or anterior uveitis. Unlike the typical patient with iritis or uveitis who tends to have obvious eye symptoms, children with iritis/uveitis due to JIA usually have no symptoms. Despite a lack of symptoms, the inflammation can lead to serious damage within the eye and can result in permanent loss of vision.
Because of the high chance of eye damage, patients with JIA are required to have routine, regular eye exams to check for iritis. The eye exam will involve looking at the eye with special instrument called a slit-lamp. The frequency of the eye exams will depend on the type of JIA the patient has.
If left untreated, iritis or uveitis can cause glaucoma, cataracts, calcium deposits in the cornea or swelling in the retinal or optic nerve . These problems can result in decreased vision and even blindness.
Don’t Miss: Is Peanut Butter Bad For Arthritis