Learning When You’re Stiff
RA-related stiffness is usually worst in the morning and lasts about an hour, Dr. Khan says: The fingers are tight. They have a hard time movingthey feel like the Tin Manand then as they get moving, in half an hour to an hour, symptoms get better. Any extended period of sitting or just not moving can cause RA joints to stiffen up, too. Osteoarthritis stiffness typically happens for less time later in the day, after physical activity.
How Is Ra Treated
RA can be effectively treated and managed with medication and self-management strategies. Treatment for RA usually includes the use of medications that slow disease and prevent joint deformity, called disease-modifying antirheumatic drugs biological response modifiers are medications that are an effective second-line treatment. In addition to medications, people can manage their RA with self-management strategies proven to reduce pain and disability, allowing them to pursue the activities important to them. People with RA can relieve pain and improve joint function by learning to use five simple and effective arthritis management strategies.
My Experience With Seronegative Ra
Five years ago I was such a case of seronegative arthritis. Over a period of four years I had two ankle surgeries and a bad case of inflammation in both eyes called uveitis. Then I started to have pain and swelling in my fingers coupled with general fatigue. I went to my primary care physician and after taking a history and conducting a physical exam, he immediately sent me to a rheumatologist. All of the blood tests came back negative. Yet, I had bone erosion in my fingers as shown by x-rays and the doctor put me on disease modifying drugs. After symptoms continued unabated, I quickly progressed to using biological treatments.
Donât Miss: Is Colchicine Good For Rheumatoid Arthritis
Don’t Miss: What Makes Tylenol Arthritis Different
What Foods Are Good For Rheumatoid Arthritis
It is important to maintain a healthy diet if you have rheumatoid arthritis to help reduce your risk of developing serious symptoms. This includes:
- eating lots of fruits, vegetables and wholegrain cereal food, such as brown rice or oats
- eating foods that contain fish oil
- avoiding fatty, sugary or very salty foods
- not drinking alcohol often
- maintaining a healthy body weight
Ra Progression: What Are The Signs Of Rheumatoid Arthritis Progression
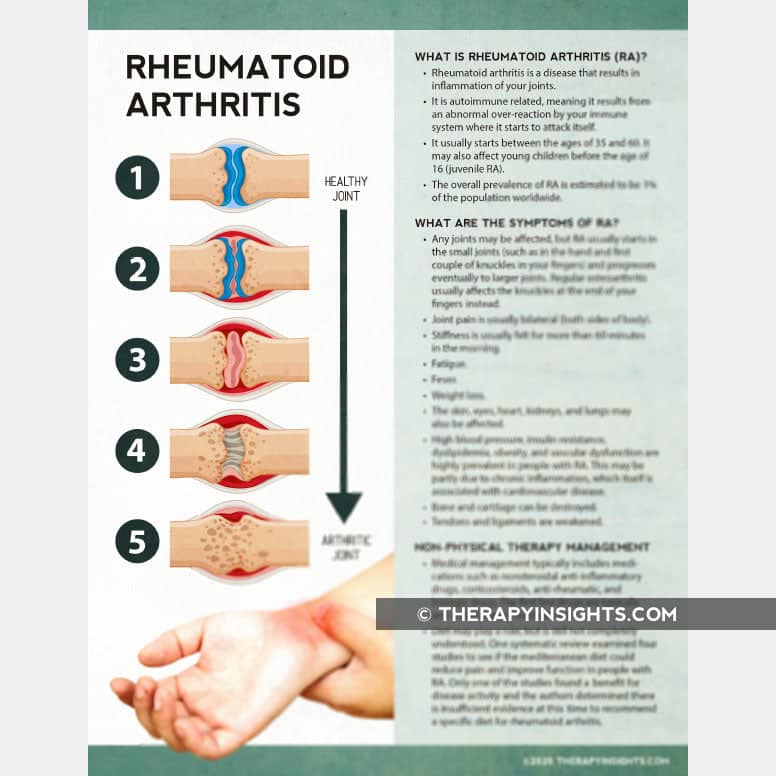
If you suspect you have rheumatoid arthritis or have been recently diagnosed with RA, you will likely have lots of questions and be feeling uncertain about what this disease means for your future. What is the normal RA progression? Will my symptoms get worse? How can I manage the disease? Do I have to have a surgery?
These are all frequent questions asked by RA sufferers. The reality though is that each patient will experience a unique progression of this disease. RA progression depends on multiple unpredictable variables. Because it is still unclear exactly what triggers RA, it can be nearly impossible to predict an exact outcome.
Below is some general information about what to expect as well as the different stages of RA including the advanced condition known as progressive rheumatoid arthritis.
Recommended Reading: What Bread Is Good For Arthritis
What Are The Diagnostic Criteria For Rheumatoid Arthritis
Diagnostic criteria are a set of signs, symptoms and test results your provider looks for before telling you that youve got rheumatoid arthritis. Theyre based on years of research and clinical practice. Some people with RA dont have all the criteria. Generally, though, the diagnostic criteria for rheumatoid arthritis include:
- Inflammatory arthritis in two or more large joints .
- Inflammatory arthritis in smaller joints.
- Positive biomarker tests like rheumatoid factor or CCP antibodies.
- Elevated levels of CRP or an elevated sed rate.
- Your symptoms have lasted more than six weeks.
Can You Have Oa If You Have Rheumatoid Arthritis
However, drugs that are specifically for rheumatoid arthritis, such as biologic drugs, will have no effect on OA. They target the autoimmune response and donÕt do anything directly to your joints. The good news is that treatments for one condition shouldnÕt exacerbate the other condition or conflict with its treatment.
Read Also: Is Krill Oil Better Than Fish Oil For Arthritis
What Medications Treat Rheumatoid Arthritis
Early treatment with certain drugs can improve your long-term outcome. Combinations of drugs may be more effective than, and appear to be as safe as, single-drug therapy.
There are many medications to decrease joint pain, swelling and inflammation, and to prevent or slow down the disease. Medications that treat rheumatoid arthritis include:
Non-steroidal anti-inflammatory drugs
Biologics tend to work rapidly within two to six weeks. Your provider may prescribe them alone or in combination with a DMARD like methotrexate.
Can I Prevent Rheumatoid Arthritis
You cannot prevent rheumatoid arthritis because the cause of the disease is not known.
Quitting smoking, or never smoking, will reduce your risk of developing rheumatoid arthritis. You are more likely to develop rheumatoid arthritis if someone in your close family has it, but unfortunately there is no way to reduce this risk.
People who have rheumatoid arthritis often experience flare ups, which are times when their joints are particularly sore. Learning what triggers your flare ups can help reduce or prevent them.
For some people, stress can trigger a flare up, so can being run down or pushing yourself beyond your limits. Having an infection, missing a dose of your medicine or changing your treatment plan can also cause a flare up.
Keeping a food and activity diary may help work out your personal triggers but keep in mind that sometimes flare ups happen without any obvious cause.
Also Check: How To Relieve Neck Pain From Arthritis
How Is Ra Diagnosed
RA is diagnosed by reviewing symptoms, conducting a physical examination, and doing X-rays and lab tests. Its best to diagnose RA earlywithin 6 months of the onset of symptomsso that people with the disease can begin treatment to slow or stop disease progression . Diagnosis and effective treatments, particularly treatment to suppress or control inflammation, can help reduce the damaging effects of RA.
Routine Monitoring And Ongoing Care
Regular medical care is important because your doctor can:
- Monitor how the disease is progressing.
- Determine how well the medications are working.
- Talk to you about any side effects from the medications.
- Adjust your treatment as needed.
Monitoring typically includes regular visits to the doctor. It also may include blood and urine tests, and xrays or other imaging tests. Having rheumatoid arthritis increases your risk of developing osteoporosis, particularly if you take corticosteroids. Osteoporosis is a bone disease that causes the bones to weaken and easily break. Talk to your doctor about your risk for the disease and the potential benefits of calcium and vitamin D supplements or other osteoporosis treatments.
Since rheumatoid arthritis can affect other organs, your doctor may also monitor you for cardiovascular or respiratory health. Many of the medications used to treat rheumatoid arthritis may increase the risk of infection. Doctors may monitor you for infections. Vaccines may be recommended to lower the risk and severity of infections.
Recommended Reading: Can An Accident Cause Arthritis
Finding The Right Treatment
With so many ways PsA expresses itself, from skin plaques to joint pain, approaches to treatment vary. For Snedden, an integrated approach works best. Luckily for me, the biologic I am on not only clears up my skin, but for the most part has also kept the inflammation down, he says. When Snedden does have PsA flare ups, he gets pain-relieving steroid injections in his knees or uses pain-stopping creams for his hands. I also found an occupational therapist who works with me and has also developed an app that helps with my hands, he explains.
Combining PsA and psoriasis treatments is also Bells approach. My treatment is mainly geared towards my PsA, however my biologic therapy is for PsA and psoriasis so it is starting to help my psoriasis flares as well, she says. Bells path to treatment was anything but easy, though. After a nasty running injury and surgery caused her PsA to go haywire, she was put on a low dose of steroids for three months in order to qualify for financial assistance with biologics. When she finally did qualify, the first biologic helped with inflammation but not morning stiffness or joint pain. Shes now on a different biologic and methotrexate injections. In addition, Bell takes folic acid, probiotics, and a variety of vitamin supplements, and uses CBD oil at night.
Even with all that, finding relief isnt easy. My psoriasis is flaring up again currently and I manage it with steroid creams and body butter to help calm my skin down, Bell says.
What Are The Signs And Symptoms Of Ra
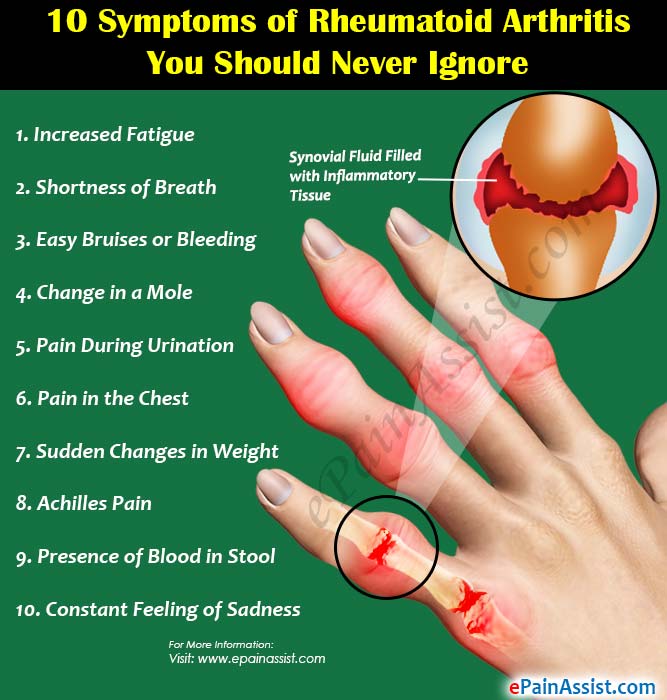
With RA, there are times when symptoms get worse, known as flares, and times when symptoms get better, known as remission.
Signs and symptoms of RA include:
- Pain or aching in more than one joint
- Stiffness in more than one joint
- Tenderness and swelling in more than one joint
- The same symptoms on both sides of the body
Recommended Reading: How Do You Test For Arthritis In Hands
Treatment For Rheumatoid Arthritis Types
is typically the same, regardless of your RA type. Since rheumatoid arthritis can be a fairly debilitating disease for many, standard over-the-counter medications likely wont cut it. Its a condition that requires a doctors close care and often disease modifying antirheumatic drugs , a group of medications prescribed for RA that can help slow down the progression of the disease. These can include methotrexate and plaquenil.
And, says Dr. Kteleh, newer biologics that target specific inflammatory molecules can be even more effective for the right person. Most biologics are injections or infusions, he says. This includes many medicines such as Remicade , Humira , Orencia , and Cimizia .
Additionally, Dr. Nuelle says that short-term use of steroids can be helpful to calm down inflammation.
Good habits and lifestyle changes, such as a nutritious diet, topical creams, and relaxation techniques like meditation and deep breathing can also ease rheumatoid arthritis symptoms.
Is Rheumatoid Arthritis Hereditary
Rheumatoid arthritis isnt considered a hereditary disease, but it does run in some families. This may be due to environmental causes, genetic causes, or a combination of both.
If you have family members who have or have had RA, talk to your healthcare provider, especially if you have any symptoms of persistent joint pain, swelling, and stiffness unrelated to overuse or trauma.
Having a family history of RA increases your risk of getting the disease, and early diagnosis can make a big difference in how effective treatment will be.
Also Check: What Can You Do To Help Arthritis Pain
What Is The Treatment For Rheumatoid Arthritis
While theres no cure for rheumatoid arthritis, there are many strategies to help manage the condition and its symptoms so you can continue to lead a healthy and active life. Its helpful to understand the nature of your condition and build good relationships with your doctor, rheumatologist and healthcare professionals.
What Are Rheumatic Diseases
Rheumatic diseases are autoimmune and inflammatory diseases in which the immune system attacks the joints, muscles, bones, and organs.
If you cannot see a rheumatologist for your RA, your primary healthcare provider can manage your RA care if they are knowledgeable about the condition. If you live in a remote area or do not have access to a rheumatologist locally, consider seeing one remotely using telehealth options.
In addition to your rheumatologist and primary care provider, you might need to include additional specialists to your care team as the need arises. Additional healthcare professionals you may need to see include pain specialists, physical therapists, occupational therapists, mental health professionals, orthopedists, surgeons, and dietitians.
Don’t Miss: What Kind Of Doctor Do You See For Psoriatic Arthritis
Leading A Sedentary Lifestyle
Regular physical activity is necessary for everyone, including people with RA, and there are numerous health benefits associated with it. Improved muscle strength, as well as better bone and joint health, is essential for people with RA. Rest is also needed, to restore the body from the episodes of intense pain and fatigue that are characteristic of RA. But rest cant become a way of life striking a balance between rest and activity is optimal. A sedentary lifestyle actually does the opposite of what you want, leading to increased pain, fatigue, and weakness.
RELATED: Best and Worst Exercise Trends for Rheumatoid Arthritis
What To Watch For
Joints are more likely to be stiff first thing in the morning or after you rest for a while.
Joint warmth and swelling. Along with pain, inflammation can make your joints swollen and warm to the touch.
Nail problems. Psoriatic arthritis can make your fingernails and toenails to lift from their nail beds. Its a symptom unique to psoriatic arthritis.
Lower back pain. For about 20% of people with psoriatic arthritis, inflammation causes problems with the joints between your vertebrae, a condition called spondylitis. In more severe cases, this can cause joints to fuse together.
Dactylitis. This is when entire fingers or toes swell to look like sausages. Signs of dactylitis can help doctors distinguish psoriatic arthritis from rheumatoid arthritis, which may affect more than one joint.
Eye problems. In some cases, people with psoriatic arthritis also experience eye problems. The same inflammatory process that causes joint problems in can also damage other areas of the body such as eyes. Problems can include:
- Conjunctivitis, which is inflammation of the layer that lines the white of your eye and the inside of your eyelid
- Disturbed vision
Foot pain. Two of the most common places to find psoriatic arthritis are at the Achilles tendon, which is between the calf muscle and heel, or the bottom of your foot.
Trouble moving hands and fingers. The swelling and joint pain that can come with psoriatic arthritis can make even simple, day-to-day tasks hard.
Also Check: What Do I Give My Dog For Arthritis
What Is Rheumatoid Arthritis
Rheumatoid arthritis, or RA, is an autoimmune and inflammatory disease, which means that your immune system attacks healthy cells in your body by mistake, causing inflammation in the affected parts of the body.
RA mainly attacks the joints, usually many joints at once. RA commonly affects joints in the hands, wrists, and knees. In a joint with RA, the lining of the joint becomes inflamed, causing damage to joint tissue. This tissue damage can cause long-lasting or chronic pain, unsteadiness , and deformity .
RA can also affect other tissues throughout the body and cause problems in organs such as the lungs, heart, and eyes.
Can Rheumatoid Arthritis Be Cured
Although there is no guaranteed cure for rheumatoid arthritis, there are many early treatment options that can reduce permanent joint damage and the overall impact of the condition. These treatments are called disease-modifying agents and Biologics. Biologics can be given by subcutaneous injections or through intravenous infusions.
Other arthritis treatment options include arthritis IV infusion therapy, medication and changes in lifestyle or diet. Incorporating diet changes and exercise into your daily routine is a great way to prevent joint pain and damage in the future.
Also Check: What Is The Diagnostic Test For Rheumatoid Arthritis
Who Should Diagnose And Treat Ra
A doctor or a team of doctors who specialize in care of RA patients should diagnose and treat RA. This is especially important because the signs and symptoms of RA are not specific and can look like signs and symptoms of other inflammatory joint diseases. Doctors who specialize in arthritis are called rheumatologists, and they can make the correct diagnosis. To find a provider near you, visit the database of rheumatologistsexternal icon on the American College of Rheumatology website.
How Is Rheumatoid Arthritis Diagnosed
Your healthcare provider may refer you to a physician who specializes in arthritis . Rheumatologists diagnose people with rheumatoid arthritis based on a combination of several factors. Theyll do a physical exam and ask you about your medical history and symptoms. Your rheumatologist will order blood tests and imaging tests.
The blood tests look for inflammation and blood proteins that are signs of rheumatoid arthritis. These may include:
- Erythrocyte sedimentation rate or sed rate confirms inflammation in your joints.
- C-reactive protein .
- About 80% of people with RA test positive for rheumatoid factor .
- About 60% to 70% of people living with rheumatoid arthritis have antibodies to cyclic citrullinated peptides .
Your rheumatologist may order imaging tests to look for signs that your joints are wearing away. Rheumatoid arthritis can cause the ends of the bones within your joints to wear down. The imaging tests may include:
In some cases, your provider may watch how you do over time before making a definitive diagnosis of rheumatoid arthritis.
You May Like: What Is The Best Arthritis Cream On The Market
What Are The Types Of Biologics
There are several. They include:
- B-cell inhibitor. They affect B cells, which are white blood cells that carry a protein that can trigger your immune response
- Interleukin-1 blocker. Stops production of an inflammatory chemical your body makes
- Interleukin-6 or interleukin-17 blocker. Stops inflammatory chemicals from attaching to cells
- Selective co-stimulation modulators. Blocks T-cell activity in your body
- T-cell inhibitor. Blocks communication between T cells, a type of white blood cell
- Tumor necrosis factor inhibitor. Blocks a chemical your body makes that drives the inflammation process
What Are The Risk Factors For Ra
Researchers have studied a number of genetic and environmental factors to determine if they change persons risk of developing RA.
Characteristics that increase risk
- Age. RA can begin at any age, but the likelihood increases with age. The onset of RA is highest among adults in their sixties.
- Sex. New cases of RA are typically two-to-three times higher in women than men.
- Genetics/inherited traits. People born with specific genes are more likely to develop RA. These genes, called HLA class II genotypes, can also make your arthritis worse. The risk of RA may be highest when people with these genes are exposed to environmental factors like smoking or when a person is obese.
- Smoking. Multiple studies show that cigarette smoking increases a persons risk of developing RA and can make the disease worse.
- History of live births. Women who have never given birth may be at greater risk of developing RA.
- Early Life Exposures. Some early life exposures may increase risk of developing RA in adulthood. For example, one study found that children whose mothers smoked had double the risk of developing RA as adults. Children of lower income parents are at increased risk of developing RA as adults.
- Obesity. Being obese can increase the risk of developing RA. Studies examining the role of obesity also found that the more overweight a person was, the higher his or her risk of developing RA became.
Characteristics that can decrease risk
You May Like: What Foods To Avoid When You Have Psoriatic Arthritis