Other Body Parts Ra Can Affect
- Bones. The chemicals that cause inflammation can also take a bite out of your bones. It often affects your hips and spine. Sometimes, itâs a byproduct of years of treating RA with steroids.
- Liver and kidneys. Itâs rare for RA to affect these organs. But the drugs that treat it can. Nonsteroidal anti-inflammatory drugs can be bad for both. Cyclosporine may cause kidney disease. Methotrexate can damage your liver.
- Immune system. The medications you take can slow it down. This makes you more likely to get infections.
- Mucous membranes. You might be more likely to get a condition called Sjogrenâs syndrome that dries out moist places in your body like your eyes, your mouth, and inside your nose.
- Muscles. When inflammation stops you from moving your joints, the attached muscles can get weak. Or you could get a condition called myositis that weakens them. The medications you take for RA can also be to blame.
- Nerves. RA causes symptoms that range from numbness and tingling to paralysis. It can result from joint damage that RA causes, the disease process itself, or medications that treat it.
- Blood vessels. RA can cause inflammation of your blood vessels. It can show up as spots on the skin or can cause ulcers in more severe cases.
How Ra Fatigue Feels
RA fatigue can be “multidimensional, overwhelming, and unpredictable, with physical, cognitive, and emotional components,” according to a 2016 report in BMC Musculoskeletal Disorders.
RA fatigue can feel like whole-body all-over exhaustion. Some people with the condition might describe it as deep tiredness or the slowing down of the body as if you are recovering from an illness like the flu.
What Is Ra Fatigue
No two people with RA experience the same disease symptoms, but some RA symptoms are more common than others, mainly fatigue.
According to a 2020 report in RMD Open, fatigue in RA affects about three-quarters of the people with the condition. This report also finds that fatigue affects the quality of life and is related to pain, co-morbidities , low mood, and sleep troubles.
Read Also: How To Eat For Arthritis
Osteoarthritis Versus Rheumatoid Arthritis
Osteoarthritis is a degenerative condition where the cartilage in joints is damaged, disrupting the smooth gliding motion of the joint surfaces. The result is pain, swelling, and deformity that can worsen over time. The most common joints affected are knees, hips, spine, and hands. The pain of osteoarthritis increases with overuse and improves with rest.
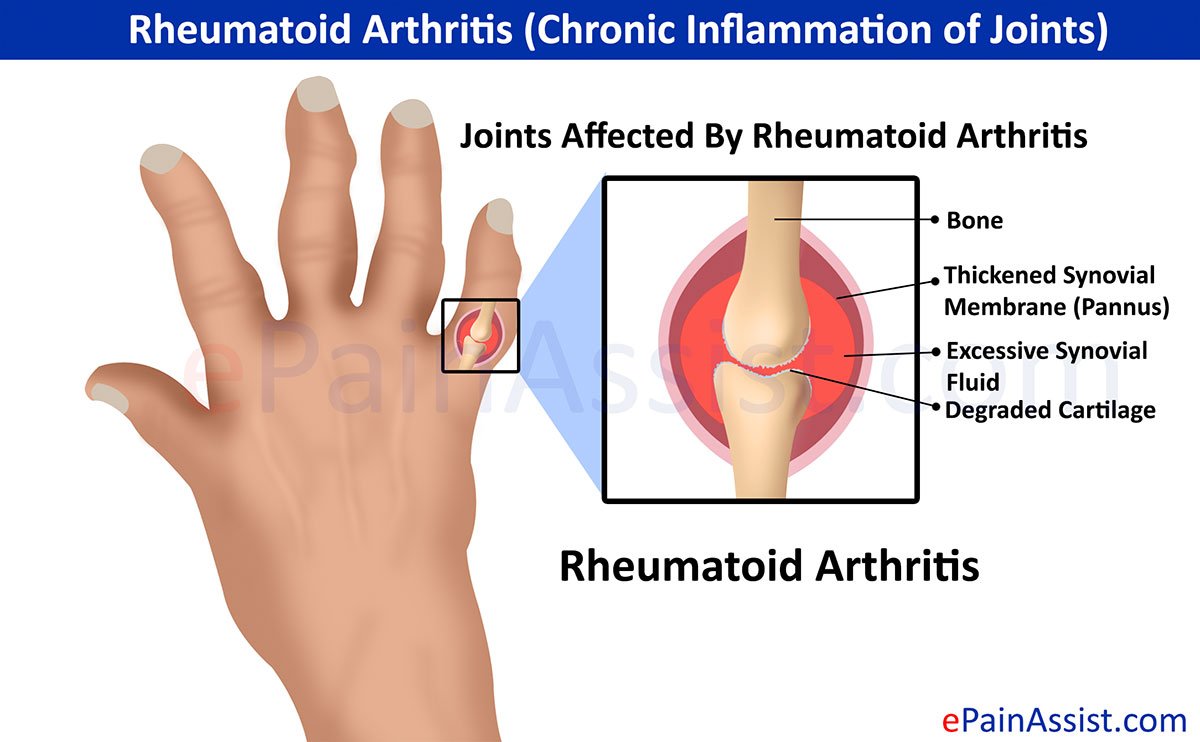
Rheumatoid arthritis , on the other hand, is an inflammatory autoimmune disease that affects connective tissue throughout the body. The most common result is redness, swelling, and tenderness in the joints. RA symptoms and severity can vary significantly between people. Some may have mild symptoms over a short period of time and some may have more severe forms that last many years. RA may occur in cycles of remission with no symptoms and flare ups where symptoms are more severe.
Joints Affected by Osteoarthritis:
Rheumatoid Arthritis:
Factors That Influence Chronic Arthritis Pain
Arthritis often causes chronic pain, which is often defined as pain lasting for twelve weeks or more. Over time, it tends to be variable rather than constant. You may have long stretches lasting for weeks or months during which you can experience milder or more intense pain, and you may even notice a difference in intensity throughout the day. Treatment can often control or diminish the pain, but so can identifying some of the factors that can play into the chronic pain of arthritis so you can either address them or make modifications with them in mind.
You May Like: What Is The Best Pain Medication For Knee Arthritis
Transcutaneous Electrical Nerve Stimulation
This form of therapy uses low-voltage electric currents to stimulate nerves and interfere with pain pathways. TENS is usually used for stubborn, chronic pain and not as a first-line treatment for RA, Ali says. One of the benefits of this treatment is the low occurrence of side effects. If youre interested in trying TENS for pain relief, talk with your physical therapist. If you have a pacemaker, a heart problem, or epilepsy or youre pregnant get your doctors approval first before trying TENS.
How Is Ra Diagnosed
RA is diagnosed by reviewing symptoms, conducting a physical examination, and doing X-rays and lab tests. Its best to diagnose RA earlywithin 6 months of the onset of symptomsso that people with the disease can begin treatment to slow or stop disease progression . Diagnosis and effective treatments, particularly treatment to suppress or control inflammation, can help reduce the damaging effects of RA.
You May Like: What To Do For Arthritis In Hip
Does Rheumatoid Arthritis Cause Fatigue
Everyones experience of rheumatoid arthritis is a little different. But many people with RA say that fatigue is among the worst symptoms of the disease.
Living with chronic pain can be exhausting. And fatigue can make it more difficult to manage your pain. Its important to pay attention to your body and take breaks before you get too tired.
What are rheumatoid arthritis flare symptoms?
The symptoms of a rheumatoid arthritis flare arent much different from the symptoms of rheumatoid arthritis. But people with RA have ups and downs. A flare is a time when you have significant symptoms after feeling better for a while. With treatment, youll likely have periods of time when you feel better. Then, stress, changes in weather, certain foods or infections trigger a period of increased disease activity.
Although you cant prevent flares altogether, there are steps you can take to help you manage them. It might help to write your symptoms down every day in a journal, along with whats going on in your life. Share this journal with your rheumatologist, who may help you identify triggers. Then you can work to manage those triggers.
Whats The Age Of Onset For Rheumatoid Arthritis
RA usually starts to develop between the ages of 30 and 60. But anyone can develop rheumatoid arthritis. In children and young adults usually between the ages of 16 and 40 its called young-onset rheumatoid arthritis . In people who develop symptoms after they turn 60, its called later-onset rheumatoid arthritis .
Read Also: What Can Help Rheumatoid Arthritis
When Should I See My Doctor
If you notice symptoms of rheumatoid arthritis, or you are concerned that you may have rheumatoid arthritis, you should see your doctor as soon as possible. Your doctor may refer you to a rheumatologist who is a doctor that specialises in joints. It is important to act quickly. The sooner you start treatment, the less likely you are to experience permanent joint damage and deformity.
Rheumatoid Arthritis Pain Management
While the overall goal of rheumatoid arthritis therapy is to prevent disease progression and further joint damage, pain management is a necessary daily practice for patients, in order to maximize their quality of life. Chronic pain can adversely affect a patients ability to work, participate in physical and social activities, and can generally interrupt day-to-day life.
Despite medications and aggressive forms of treatment, many rheumatoid arthritis patients experience ongoing pain and stiffness. The reality is, it may never completely go away. But there are specific things patients can do to manage pain and limit its impact on their lives.
You May Like: What Are The Symptoms Of Arthritis In Your Fingers
Research On Rheumatoid Arthritis
In the last decade, much research has been conducted to increase our understanding of the immune system and what makes it malfunction. There have also been new therapies developed to help treat the disease. Some of the topics of intense research include:
What are the genetic factors that predispose people to develop rheumatoid arthritis?
Some white blood cells, commonly known as T cells, are important in maintaining a healthy and properly functioning immune system. However, scientists have discovered a variationcalled single nucleotide polymorphism in a gene that controls T cells. When the SNP gene variation is present, T cells attempt to correct abnormalities in joints too quickly, causing the inflammation and tissue damage associated with RA. The discovery of SNP may help determine peoples risk for getting RA and might help explain why autoimmune diseases run in families.
At conception, twins have an identical set of genes. So why would only one twin develop RA?
Tailbone Pain In People With Ra
RA is an inflammatory and autoimmune disease. The immune system attacks the bodys healthy cells, causing inflammation. Inflammatory symptoms can appear throughout the body, manifesting as pain and swelling, usually in the joints.
Autoimmune conditions are often associated with back pain because of the immune systems attack on healthy cells, including cells that make up the vertebrae. Although the tailbone is not the most common location for RA pain, research has reported cases of coccydynia in individuals with RA. People with RA could have tailbone pain due to a fall or another common cause thats unrelated to an inflammatory condition.
Tailbone pain in people with RA could be caused by a related autoimmune condition. The most common autoimmune cause of coccydynia is ankylosing spondylitis, an inflammatory disease that causes the fusion of bones in the body over time.
Tailbone pain may also be associated with other conditions, such as osteoarthritis of the spine, psoriatic arthritis, and systemic lupus. In such conditions, tailbone pain likely progresses over time, so it is important to seek medical advice from your rheumatologist to receive appropriate medical treatment.
You May Like: What Type Of Dr Treats Arthritis
Does Stress Affect Rheumatoid Arthritis
Patients commonly report that stress, either physical or emotional, was present or severe when their RA began. This is true in other autoimmune disorders as well. Since the mind-body connection is very real, most doctors agree that there is a link between stress and disease onset or flares.
Because there are clear interactions between the nervous, immune and endocrine systems, the impact of stress on disease presentation and severity is explainable in physiologic terms. Obviously, life is stressful. Thus, how to employ stress reduction in a therapeutic regimen is up to the individual patient, in concert with the physician. Many patients have found benefits from mindfulness programs that facilitate learning tools to reduce the impact of stress.
What Is The Difference
Rheumatoid arthritis vs. osteoarthritis
Rheumatoid arthritis and osteoarthritis are both common causes of pain and stiffness in joints. But they have different causes. In osteoarthritis, inflammation and injury break down your cartilage over time. In rheumatoid arthritis, your immune system attacks the lining of your joints.
Rheumatoid arthritis vs. gout
Rheumatoid arthritis and gout are both painful types of arthritis. Gout symptoms include intense pain, redness, stiffness, swelling and warmth in your big toe or other joints. In gout, uric acid crystals cause inflammation. In rheumatoid arthritis, its your immune system that causes joint damage.
Recommended Reading: Can I Get Rid Of Rheumatoid Arthritis
Difficulty With Daily Tasks
The combination of joint pain, stiffness, and fatigue can make it difficult to carry on daily activities, and the loss of function can be extremely frustrating. Especially when the hands are affected, its hard to hold a toothbrush, do up buttons or a zipper, open a water bottle, type on a keyboard, says Dr. Bykerk. It can even be difficult to hold a grocery bag or a child. Not being able to function normally and deal with daily life understandably sends many people to the doctor to find out whats wrong.
Who Should Diagnose And Treat Ra
A doctor or a team of doctors who specialize in care of RA patients should diagnose and treat RA. This is especially important because the signs and symptoms of RA are not specific and can look like signs and symptoms of other inflammatory joint diseases. Doctors who specialize in arthritis are called rheumatologists, and they can make the correct diagnosis. To find a provider near you, visit the database of rheumatologistsexternal icon on the American College of Rheumatology website.
Read Also: What Are The Early Symptoms Of Psoriatic Arthritis
Why Do Joints Make Popping And Cracking Noises
Joints can make different noises–some are serious and some are not.
Some people learn how to “pop their knuckles.” By pushing or pulling a joint in a certain way an air bubble can suddenly appear in the joint with a “pop.” Once the bubble is there the joint cannot be popped again until the air has been reabsorbed.
Some joints crack as the ligaments and tendons that pass over them slide past bumps on the bones. Individuals who “crack their neck” make noise in this way.
Other joints lock up intermittently–often with a loud pop–because something gets caught in between the joint surfaces. A torn cartilage in the knee or a loose piece of bone or cartilage in the joint can do this. Once a joint is stuck in this way, it may need to be wiggled around to unlock it. This may also cause a pop.
Finally joints that are arthritic may crack and grind. These noises usually occur each time the joint is moved. This noise is due to the roughness of the joint surface due to loss of the smooth cartilage.
What Are The Early Signs Of Rheumatoid Arthritis
Early signs of rheumatoid arthritis include tenderness or pain in small joints like those in your fingers or toes. Or you might notice pain in a larger joint like your knee or shoulder. These early signs of RA are like an alarm clock set to vibrate. It might not always been enough to get your attention. But the early signs are important because the sooner youre diagnosed with RA, the sooner your treatment can begin. And prompt treatment may mean you are less likely to have permanent, painful joint damage.
Read Also: Where Can I Buy Tiger Balm Arthritis Rub
Differential Diagnosis Of Rheumatoid Arthritis
It is mainly performed with other types of arthritis, in particular, with a reactive form. In addition, work is carried out on a thorough examination, in order to exclude osteoarthritis. Thus, we get two diseases that can give adjacent symptoms, increasing the likelihood of an incorrect diagnosis – it’s reactive arthritis and osteoarthritis.
Considering these three diseases in the framework of differential diagnostics, compare the existing symptoms and complaints with the presence and specificity of this symptom in adjacent diagnoses.
It is most convenient to explain using a specific example. Let’s consider some data that are important for an accurate diagnosis and compare three diseases. So, we are interested in:
- Age of the patient.
- Indicators of ESR.
- Presence of a rheumatoid in the blood.
These indicators in three cases will, by and large, be different. With such a disease as rheumatoid arthritis, the picture will be as follows: the patient’s age is medium or slightly above average, severe pain in the joints, with the presence of a feeling of stiffness in the limbs in the morning. The joints are symmetrical. In the blood excessively high index of ESR. Revmofactor is positive for seropositive form of the disease.
The same parameters for the two other diseases we consider through an apostrophe, in the sequence – reactive arthritis / osteoarthritis:
Effect Of Pain On Disease Assessment
Two recent manuscripts have reported that pain significantly affects patient assessment of RA disease activity. The first study included 7,028 RA patients from the Quantitative Standard Monitoring of Patients with RA database . These patients were from 83 sites across 30 countries, receiving usual care from their rheumatologists. In this cohort, pain was the single most important determinant of patient global assessment, with a partial R2> 0.2 whereas the partial R2 for all other potential determinants was less than 0.05. The second study included 646 RA patients starting methotrexate treatment at an academic outpatient clinic. Similar to the QUEST-RA study, this study concluded that pain was the major determinant of patient global assessment scores, explaining 75.6 % of the variability in scores .
You May Like: What Is The Treatment For Rheumatoid Arthritis
Will Dietary Changes Help My Rheumatoid Arthritis
Diet may play a role in some patients, but most patients should maintain a well-balanced diet rather than avoid specific foods. Keep a diary to determine whether certain foods are associated with your disease flares and then see if removing them from your diet is helpful.
Some studies do suggest that eating fish two or more times per week may be associated with fewer disease-related symptoms, and there is increasing evidence that achieving and maintaining a healthy weight is helpful for managing RA.
The Condition Of People And Rheumatoid Arthritis
Rheumatologists also classify the functional state of people who suffer from rheumatoid arthritis, this is as follows:
- Class I: a person is fully able to perform ordinary daily activities
- Class II: a person is able to perform ordinary activities for self-care and work, but is limited in activities outside of work
- Class III: the ability to perform routine self-service activities, but has limitations in work and other activities
- Class IV: a person is limited in his ability to perform routine self-service, work and other activities
The doctor can choose another method of diagnosing the disease, this procedure is called joint puncture. In this procedure, sterile needles and syringes are used to drain articular fluid from the joint and are intended for study in the laboratory.
An analysis of the articular fluid in the laboratory can help to eliminate the presumed causes, such as infections and gout. Sometimes, cortisone drugs are injected into the joint during joint puncture in order to quickly remove the inflammation of the joint of the diseased leg and ensure a further reduction in symptoms.
Also Check: What Drugs Are Used To Treat Rheumatoid Arthritis