In Practice: Which Activities Can Promote The Onset Of Osteoarthritis
Professional activities which provoke or maintain pain must be temporarily or definitively stopped. In some cases, a job reclassification may be necessary .
Even if you do not have osteoarthritis, beware of practising a sport in an intensive and prolonged way!
If you suffer from osteoarthritis it is advisable to maintain a moderate and regular exercise routine, eventually including a sport. In the event of osteoarthritis of the hip and/or knee, you can pursue sports activities that do not require sudden effort such as swimming, cycling or even jogging on condition of doing it on loose soil and with good quality running shoes. Any sport that makes joint pain worse or leads to synovial effusion should be avoided!
How Common Is Osteoarthritis
Women are more likely to develop osteoarthritis than men. Australian studies show that about 1 in 10 women report having the condition, compared with about 1 in 16 men.
Osteoarthritis can develop at any age, but it is more common in people aged over 40 years or in those who have previously injured a joint. One in 5 Australians over the age of 45, and one in 3 over 75 years have osteoarthritis.
What Are The 4 Stages Of Osteoarthritis
The four stages of osteoarthritis are:
- Stage 1 Minor. Minor wear-and-tear in the joints. Little to no pain in the affected area.
- Stage 2 Mild. More noticeable bone spurs.
- Stage 3 Moderate. Cartilage in the affected area begins to erode.
- Stage 4 Severe. The patient is in a lot of pain.
Read Also: Can Rheumatoid Arthritis Cause Back Pain
Don’t Miss: Is Massage Therapy Good For Arthritis
You Were Diagnosed Late
Your RA symptoms may be worse if you had the disease for years before you knew it. If it isnt spotted and treated early, inflammation can lead to joint pain, damage, and deformity that wont get better. Physical therapy may help you move better and ease your pain. Surgery can also replace your damaged joint with a new one.
Show Sources
Early Stages Of Psoriatic Arthritis

Recognizing the signs of psoriatic arthritis can be tricky since symptoms differ from patient to patient. For example, one person can experience psoriasis skin involvement and peripheral arthritis, another may experience axial disease , and someone else could have a combination of all three.
Whats more, especially during early disease, you may confuse your symptoms with other conditions. People can mistake enthesitis, inflammation of the entheses for tennis elbow or dactylitis for an infection, explains Dr. Mikulik.
If you have psoriasis and are having pain in your tendon and musculature and you think maybe Ive been too active lately, that may be the first sign of PsA, says Dr. Haberman. Doctors commonly hear people chalk up their symptoms to overuse, such as getting more exercise than usual or doing work around the house.
If you experience any of the following signs of early psoriatic arthritis its important to see your doctor as soon as possible:
- Back pain
- Changes in your fingernails or toenails, including holes, pitting, discoloration, or softness
- Eye inflammation
- Sausage-like swelling of an entire finger or toe
- Scalp psoriasis
- Skin rash
- Tendon or ligament pain at the Achilles tendon, bottom of the foot , or elbow
Don’t Miss: What Can Cause Arthritis In The Knee
When Should I See My Doctor
Check with your doctor or health professional if you feel pain in your joints or experience other symptoms of osteoarthritis. If you have any concerns about osteoarthritis, or other health issues, they can suggest ways to manage your arthritis and refer you to a specialist if needed.
Can Osteoarthritis Be Prevented Or Avoided
Theres not much you can do to avoid getting osteoarthritis as you age. However, the following may help:
- Try to not overuse your joints.
- Try to avoid jobs or activities that require repetitive movement.
- Maintain a healthy body weight.
- Do strength-training exercises to keep the muscles around your joints strong. This is especially important for weight-bearing joints, such as the hips, knees, and ankles.
You May Like: What Is The Treatment For Arthritis
How Is Oa Treated
There is no cure for OA, so doctors usually treat OA symptoms with a combination of therapies, which may include the following:
- Increasing physical activity
- Medications, including over-the-counter pain relievers and prescription drugs
- Supportive devices such as crutches or canes
- Surgery
In addition to these treatments, people can gain confidence in managing their OA with self-management strategies. These strategies help reduce pain and disability so people with osteoarthritis can pursue the activities that are important to them. These five simple and effective arthritis management strategies can help.
Physical Activity for Arthritis
Some people are concerned that physical activity will make their arthritis worse, but joint-friendly physical activity can actually improve arthritis pain, function, and quality of life.
Gout And Calcium Crystal Diseases
Gout is a type of inflammatory arthritis that can cause painful swelling in joints. It typically affects the big toe, but it can also affect other joints in the body.
Joints affected by gout can become red and hot. The skin may also look shiny and can peel.
Its caused by having too much urate, otherwise known as uric acid, in the body. We all have a certain amount of urate in our body.
However, being overweight or eating and drinking too much of certain types of food and alcoholic drinks can cause some people to have more urate in their bodies. The genes you inherit can make you more likely to develop gout.
If it reaches a high level, urate can form into crystals that remain in and around the joint. They can be there for a while without causing any problems and even without the person realising they are there.
A knock to a part of the body or having a fever can lead to the crystals falling into the soft part of the joint. This will cause pain and swelling.
There are drugs that can reduce the amount of urate in the body and prevent gout attacks. Examples are allopurinol and . If youre having a gout attack, youll also need short-term pain relief. Non-steroidal anti-inflammatory drugs as well as paracetamol can be good drugs to try first.
Men can get gout from their mid-20s, and in women its more common after the menopause. Taking water tablets can increase the risk of gout.
There are also conditions that cause calcium crystals to form in and around joints.
Read Also: What Happens If You Have Arthritis In Your Knee
Osteoarthritis In Young People: It Doesnt Just Affect The Elderly
Osteoarthritis is the most common form of arthritis in the UK. Its a chronic, debilitating condition that affects over 9 million people.
However, misconceptions about osteoarthritis proliferate perhaps most notably, the myth that it only affects the elderly. This is not the case: although old people are more likely to get osteoarthritis , about 15,000 children and young people also develop this condition.
King Edward VIIs Hospital physician Dr David Porter specialises in all aspects of orthobiologics, substances that sports medicine physicians and orthopaedic surgeons use to help broken bones and injured tissues heal more quickly. Hes an internationally renowned senior physician in sports medicine and was previously the Club Doctor at Chelsea FC.
In this article, Dr Porter explains what osteoarthritis is, how it can affect young people as well as old and how it can be treated.
Loss Of Significant Joint Mobility
For example, you were able to flex your wrist 60 degrees, and two years later, you lost 50 percent of that range of motion. Its possible to feel okay and still experience loss of range of motion, says Dr. Domingues. But the idea is to prevent joint damage and to make you have less pain. If you have less pain and are still progressing, that means your treatment could be working better.
Recommended Reading: What Natural Supplements Help Arthritis
Read Also: Can You Have Arthritis In Your Heel
Trigger: You Dont Work On Your Flexibility
Flexibility exercises, such as yoga, tai chi, or Pilates, can improve joint mobility, reduce stiffness, and help prevent tightening of the tissues around the joint. Yoga has been found to be particularly beneficial for people with osteoarthritis. Not only can it help reduce stress, but a 2018 study of people with knee osteoarthritis found that after just one week of yoga therapy, patients reported a decrease in knee pain and stiffness, and significant improvement in mobility.
Working on your flexibility can also help with compensation. You may not be aware of your own imbalances in strength and flexibility, says Dr. Lingor. This asymmetry may put extra stress on one side of the body resulting in injury. Doing exercise like yoga, Pilates, or tai chi can help make you more aware of and correct these imbalances.
What Is Hip Arthritis
Hip arthritis is deterioration of the cartilage of the hip joint. The hip is a ball-and-socket joint with the ball at the top of the thighbone . The ball is separated from the socket by cartilage. The cartilage acts as a slippery coating between the ball and the socket that allows the ball to glide and rotate smoothly when the leg moves. The labrum, a strong cartilage that lines the outer rim of the socket, provides stability.
When cartilage in the hip is damaged, it becomes rough. Thinning of cartilage narrows the space between the bones. In advanced cases, bone rubs on bone, and any movement can cause pain and stiffness. When there is friction at any point between bones, it can also lead to bone spurs bone growths on the edges of a bone that change its shape.
Also Check: Is Cheese Good For Rheumatoid Arthritis
Trigger: You Compensate For Pain
When you have arthritis in one joint, nearby muscles and joints have to work a little harder to pick up the slack, explains Dr. Lingor. This compensation can contribute to pain or injury from extra stress in that new area.
A study published in the journal Arthritis and Rheumatology found people who develop knee pain associated with osteoarthritis often subsequently develop pain in other joints. Researchers concluded the heightened risk of pain likely occurs for many reasons including pain avoidance, pain sensitivity, and generalized OA.
This shows the importance of using as many tools as you can to manage OA in affected joints to avoid causing additional pain and problems in other areas.
Signs Your Ra Is Progressing
How can you tell your RA is getting worse? There’s no easy way, but some general signs include:
- Flares that are intense or last a long time
- Diagnosis at a young age, which means the disease has more time to become active in your body
- Rheumatoid nodules — bumps under your skin, often around your elbows
- Active inflammation that shows up in tests of joint fluid or blood
- Damage on X-rays when you were diagnosed
- High levels of rheumatoid factor or citrulline antibody in blood tests
Also Check: What Happens If You Have Rheumatoid Arthritis
You’re Having A Flare
Red, warm, swollen joints are inflamed. A flare is when inflammation in your body spikes. Your symptoms can get worse. You might also have a mild fever, fatigue, and feel sick all over. To treat a flare, your doctor might adjust your medicine to lower the inflammation. To feel better, get more rest and apply hot or cold packs to sore, swollen joints.
2
Your Range Of Motion Changes
Commonly, people will say their fingers dont straighten anymore or they cant bend or straighten them all the way, Dr. Wallace says. Their fingers dont necessarily hurt more, but they dont work like they used to work. Any range of motion or function changes like these can indicate rheumatoid arthritis progression, even without accompanying pain or tenderness.
Most people with active rheumatoid arthritis have a limited range of motion in the joints most affected by the disease, Dr. Wallace says. For many people, this includes the joints in their hands, which makes it hard to do everyday things, like drink coffee. A lot of people with active rheumatoid arthritis have problems with things like holding coffee cups, gripping steering wheels, chopping vegetables, things that require a tight grip, she says. This is often worse in the morning and gets worse when a person is experiencing a flare.
Depending on your situation, your doctor may recommend using supportive devices, like finger splints, to correct mild deformities. In situations where you have scar tissue or your joint function is severely limited, surgery may be necessary to regain proper functioning, according to Merck Manual.
Recommended Reading: What Doctor Do You See For Psoriatic Arthritis
I Have Been Told That I Have Osteoarthritis Because Of My X
Not necessarily. Some people with osteoarthritis can have no pain at all, yet their X-rays can look very abnormal, and some people with normal x-rays can have a lot of pain. Joint replacement surgery is done to improve pain and function and the decision to have surgery is never just based on x-ray results, so if you can manage your pain and stiffness well by yourself, then you may never need to have surgery.
If your pain is severe and you have tried all the simple self-management techniques that you can to improve the pain, then you may benefit from joint replacement surgery. The most commonly replaced joints are the hips and knees but other joints such as the shoulders, elbows, ankles and wrists and even the small finger joints can now be replaced. Joint replacement surgery can be extremely effective at reducing pain and more than 90% of people who have a hip or knee replaced are happy or very happy with the results. Modern joint replacements can last for 20 years or more.
Why Is My Hip Arthritis Getting Bad So Fast
A common symptom in patients who present to us with hip arthritis isnt just pain, but pain that progresses very quickly. Patients often ask, Why is my arthritis getting bad so fast? While the breakdown of cartilage in the hip and decreased range of motion are common factors it shares with arthritis in other joints, an issue that commonly occurs in hip arthritis is deterioration of the bone. This can result in bone marrow lesions and eventually voids in the bone called bone cysts left by areas of bone that have died.
Last week, we briefly mentioned bone cysts as one of the key features of hip arthritis that separate it from knee arthritis, as though bone cysts can occur in the knee, they arent common in the knee. Today, were going to expand on this and explain the unique bone issues that occur in hip arthritis as todays entry in our arthritis series for National Arthritis Month.
Don’t Miss: How To Cure Arthritis In Hands
What Are The Early Stages Of Psoriatic Arthritis
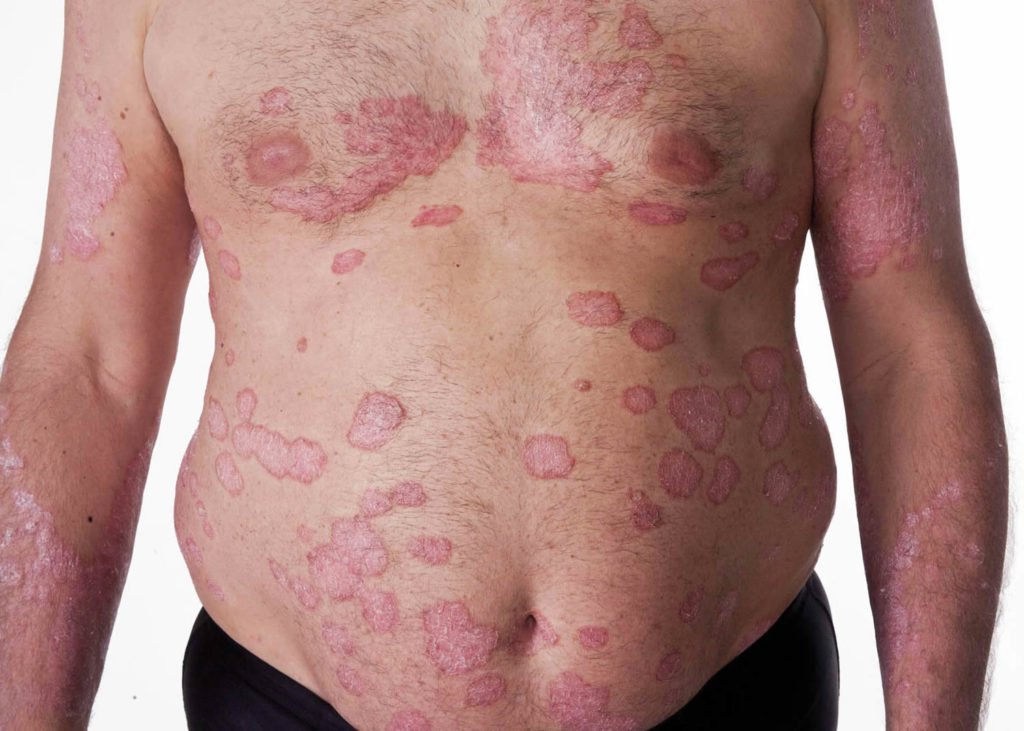
In most cases, psoriatic arthritis begins years after the initial presentation of psoriasis symptoms. Psoriasis symptoms include flare-ups of itchy, red, scaly skin.
If you have psoriasis, several things can make you more likely to develop psoriatic arthritis. These risk factors include:
- having psoriasis on your fingernails
- having a family history of psoriatic arthritis
- being between the ages of 30 and 50
- having scalp psoriasis
Like other types of arthritis, psoriatic arthritis often starts with pain and swelling in one or more of your joints. It tends to begin in the smaller joints, such as those in the fingers and toes. But you might also first notice it in larger joints, such as your knees or ankles.
You may also notice swelling in your fingers or toes. This swelling can affect the entire toe or finger, not just the joint.
How Your Treatment Changes As Ra Progresses
Early stage. A key focus is to control the inflammation. Thatâs especially critical in the early phase of the disease to prevent joint damage. You may get:
- A disease-modifying antirheumatic drug , such as methotrexate
- Nonsteroidal anti-inflammatory drugs , such as aspirin and ibuprofen, for pain
Quitting smoking and losing any extra weight also can help slow your RA.
Moderate stage. This is when you may have trouble with regular daily activities because of pain. You also may tire more easily. There are several options. Your doctor may have you try combining methotrexate with two other DMARD medications, sulfasalazine and hydroxychloroquine. Another option is a stronger form of DMARDs, called biologic DMARDs, including:
- Tofacitinib
- Upadacitinib
If a certain joint is particularly inflamed, your doctor may give the joint steroid shots. Once your pain is under control, itâs important to exercise to keep ahead of your RA. You also may need physical therapy.
Severe stage. If a TNF inhibitor fails to improve your symptoms, your doctor may recommend you try a different TNF inhibitor or a different class of biologic. If you donât respond to one, you may respond to another.
Surgery is a last-resort treatment for very severe RA. That includes when your joints are deformed and damaged and limit your mobility. The three most common surgeries for RA are:
Don’t Miss: How Can You Help Arthritis
What’s New In Arthritis Research
Progress is so fast in some areas of arthritis research today that the media often report new findings before the medical journal with the information reaches your doctor’s office. As a result, you need to know how to evaluate reports on new arthritis research.
Arthritis researchers are looking at four broad areas of research. These include causes, treatments, education and prevention.
Researchers are learning more about certain conditions. For example in osteoarthritis, researchers are looking for signs of early destruction of cartilage and ways to rebuild it. For rheumatoid arthritis and other types that involve inflammation, researchers are trying to understand the steps that lead to inflammation and how it can be slowed or stopped. An initial study suggests that fibromyalgia affects more older people than originally thought and often may be overlooked in this group. Your doctor can tell you about other new research findings. If you would like to take part in arthritis research, ask your doctor for a referral to a study in your area.
Many people help make arthritis research possible. The federal government through its National Institutes of Health is the largest supporter of arthritis research. Drug companies do the most research on new medications.