Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Chronic Nature Of Psoriatic Arthritis
Psoriatic arthritis is an autoimmune condition in which the immune system mistakenly attacks healthy tissue, leading to pain and inflammation. PsA is chronic, which means that it is persistent and long-lasting, with no current cure. PsA requires ongoing medical attention and may require you to limit your daily living activities.
PsA symptoms can come and go and tend to vary from mild to severe. The onset of symptoms is called a flare, or flare-up. If left untreated, PsA inflammation can cause health problems, including damage to the joints, uveitis , gastrointestinal problems, lung problems, weak bones, and damage to the cardiovascular system.
Psoriatic Arthritis Treatment Injection Options
There are several different kinds of biologic injections used to treat psoriatic arthritis. These include:
- Stelara
- Taltz
There are additional forms of biologic injections available, but they are typically only used for the treatment of psoriasis and not psoriatic arthritis. These include:
- Ilumya
- Tremfya
The frequency of injections will depend on the specific type of medication that you are prescribed. Remicade is delivered intravenously at a hospital, infusion center, or another medical facility, and repeated every eight weeks.
All the other types of medication are injected subcutaneously, or under the skin, in your abdomen or thigh. Many of these injections can be done by yourself at home. Some medications require a frequent injection schedule, such as Enbrel, which has to be done every week, and Cimzia every other week.
Other medications require less frequent injections after initial doses, such as Cosentyx, Taltz, and Simponi and Skyrizi and Stelara every 12 weeks.
Don’t Miss: Side Effects Of Arthritis Medications
Complementary And Alternative Therapies
You can try:
- Acupressure and acupuncture: These ancient Chinese treatments involve putting pressure on or inserting needles into the bodyâs healing points or energy lines. Acupressure isnât proven to help, but studies show that acupuncture can ease your pain.
- Curcumin: Thereâs some proof that this substance, the active ingredient in the spice turmeric, can help curb inflammation.
- Massage: It can help stretch your muscles and joints, promote circulation in your lymph system, and help you relax.
- Reiki: This Japanese relaxation technique can help you manage stress.
- Tai chi: This gentle Chinese exercise helps with relaxation and can ease sore, stiff joints.
- Yoga: The controlled movements can relax stiff muscles, ease sore joints, and boost your range of motion. It can also help with pain.
- Vitamin D: As an ointment, itâs been used to treat psoriasis for years. You can also get it from foods like:
- Cod-liver oil
- Coldwater fish like Sockeye salmon, mackerel, tuna
- Vitamin D-fortified products like nonfat milk, orange juice, yogurt
- Eggs
- Swiss cheese
Always talk to your doctor before you add any supplement or treatment. Look for a practitioner who is certified and, if possible, has experience with people who have psoriasis and psoriatic arthritis.
Recommended Reading: What Does Arthritis Do To You
Psoriatic Arthritis: Is It Time For A Biologic
These therapies have been used in the treatment of psoriasis for over 15 years, says the National Psoriasis Foundation, and most are administered by injection or intravenous infusion. Janus kinase inhibitors have emerged as a new type of biologic treatment for psoriatic arthritis, and unlike most biologics, these drugs come in pill form.
Biologics come with some risks, according to Matteson. In general, theres concern about any drug that modifies the immune system because of the possibility of infections or cancer development, he says.
While these concerns are valid, Matteson says that the benefits of biologic medications outweigh the risks, even for people whose cases are not severe. People who have mild pain or swelling in a single joint may do just fine with NSAIDs alone. For people who have more joint swelling and pain, the use of biologics is justified, Matteson says.
You May Like: Symptoms Of Arthritis
Recommended Reading: Relief For Rheumatoid Arthritis In Hands
Who Gets Psoriatic Arthritis
Psoriatic arthritis has an incidence of approximately 6 per 100,000 per year and a prevalence of about 12 per 1000 in the general population. Estimates of the prevalence of psoriatic arthritis among patients with psoriasis range between 4 and 30 per cent. In most patients, arthritis appears 10 years after the first signs of skin psoriasis. The first signs of psoriatic arthritis usually occur between the ages of 30 and 50 years of age. In approximately 1317% of cases, arthritis precedes the skin disease.
Men and women are equally affected. The symptoms of psoriatic arthritis come and go but it is a lifelong condition that is usually progressive.
Patients with psoriasis who are more likely to subsequently get arthritis include those with the following characteristics:
- Elevated C-reactive protein at baseline.
How Is Psoriatic Arthritis Diagnosed
Your doctor usually bases the diagnosis on your symptoms, a physical examination, and a blood test.
During the physical exam, your doctor will look for signs of inflammation in your joints and tendons. Your doctor will monitor the mobility of your pelvis, hips, and back. Your doctor will physically examine your eyes, skin, and nails.
Usually, your doctor will have your blood tested. With the blood test, your doctor wants to find out whether inflammatory values are present in your blood and whether the hereditary factor HLA-B27 is present. The presence of HLA-B27 does not say everything because this factor also occurs in people who do not suffer from this condition.
However, if your doctor finds HLA-B27 in your blood, it can help to make the diagnosis with certainty. Often the rheumatoid factor and anti-CCP antibodies are also examined in the blood test. This helps to distinguish between psoriatic arthritis and rheumatoid arthritis.
Additional research
In addition, your doctor often conducts additional research. He will have one or more X-rays taken to see if any abnormalities are visible in the joints in your arms or legs.
How Does Psoriatic Arthritis Proceed?
Usually, periods in which you have many complaints alternate with periods in which the condition calms down on its own.
There is no connection between skin complaints and joint complaints.
Medicines also help to reduce your symptoms.
Occasionally, people with psoriatic arthritis have long-term inflamed joints.
Don’t Miss: Can Rheumatoid Arthritis Affect Your Back
Medications For Psoriatic Arthritis
There are several types of drugs that can effectively treat psoriatic arthritis. Certain over-the-counter medications, such as ibuprofen, may help reduce your symptoms.
If OTC drugs dont help your joint pain and swelling, your doctor may need to prescribe stronger medications. These include:
- traditional disease-modifying antirheumatic drugs
Lifestyle Changes For Psoriatic Arthritis
You can make some changes that will improve your quality of life:
- Eat healthy food. Focus on a healthy eating plan like the Mediterranean diet. Opt for foods that may ease inflammation, like:
- Coldwater fish
- Exercise: When your joints are sore, you may not want to move. But doing so can:
Keep your joints and tendons loose
- Keep the inflammation that comes with this disease in check
- Lessen the workload on your joints
- Lower your risk of other conditions that come with PsA, like heart disease, diabetes, and Crohnâs disease
Walking, biking, and swimming are all good options.
- Get to, and stay at, a healthy weight. Almost half the people with PsA are overweight. Studies show that losing just 10% of your body weight can improve your response to medications for psoriasis and psoriatic arthritis.
- Manage your stress. Things that make you worry can also make your PsA worse. Exercise, medication, and talk therapy can all help.
- Rest. Give an achy joint a break. You can go back to what you were doing when you feel better.
- Donât drink. Mixing some PsA medications with alcohol can lead to liver damage. Your doctor can let you know if you should quit.
Recommended Reading: What To Do For Arthritis Pain In Hands
Fda Approves New Treatment Option For Patients With Psoriatic Arthritis
The US Food and Drug Administration has approved risankizumab-rzaa for the treatment of active psoriatic arthritis in adults.
Previously approved in 2019 for the treatment of moderate to severe plaque psoriasis, this is the second indication for risankizumab-rzaa. Risankizumab-rzaa is administered via a single 150-mg injection subcutaneously 4 times per year following the administration of 2 starter doses at weeks 0 and 4. The injection can be administered alone or in combination with disease-modifying antirheumatic drugs .
This approval was based on the results from the KEEPsAKE-1 and KEEPsAKE-2 randomized, placebo-controlled studies. These studies evaluated the safety and efficacy of this medication in individuals with active PsA who have had an inadequate response with DMARDs and/or biologic therapy. Compared with placebo, risankizumab-rzaa met the primary endpoint of ACR20 and resulted in significant improvements for PsA symptoms such as painful joints, dactylitis, and enthesitis.
Associated serious adverse events include allergic reactions and infections. Upper respiratory infections, fatigue, fungal skin infections, headache, and injection site reactions are among the most common adverse events.
Reference:
What To Know About Insurance
One of the biggest challenges in your PsA treatment may be getting insurance approval. Most insurance companies require you to first try and fail a cheaper drug before theyll pay for something more expensive like a biologic, says Dr. Shoor. What is or isnt covered varies by insurer. Talk with your doctors billing department about any questions or concerns you have they may be able to help you get coverage for the medications you need.
Recommended Reading: Inflammatory Polyarthritis Symptoms
Who Is At Risk For Psoriatic Arthritis
Psoriasis affects 2-3 percent of the population or approximately 7 million people in the U.S. and up to 30% of these people can develop psoriatic arthritis. Psoriatic arthritis occurs most commonly in adults between the ages of 35 and 55 however, it can develop at any age. Psoriatic arthritis affects men and women equally.
It is possible to develop psoriatic arthritis with only a family history of psoriasis and while less common, psoriatic arthritis can occur before psoriasis appears. Children of parents with psoriasis are three times more likely to have psoriasis and are at greater risk for developing psoriatic arthritis. The most typical age of juvenile onset is 9-11 years of age.
Can Psoriatic Arthritis Affect Other Parts Of The Body
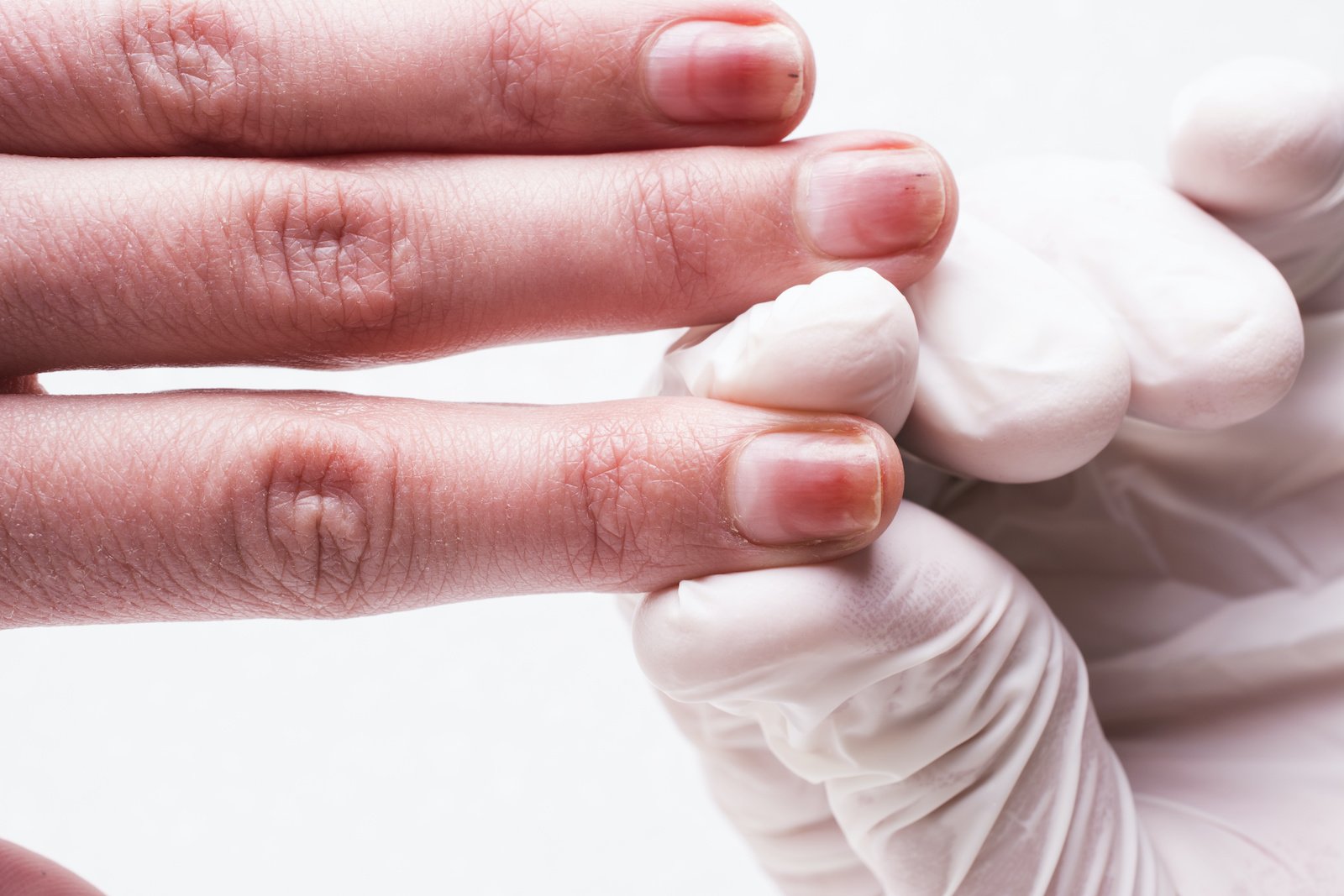
Having psoriatic arthritis can put you at risk of developing other conditions and complications around the body.
The chances of getting one of these are rare. But its worth knowing about them and talking to your doctor if you have any concerns.
Eyes
Seek urgent medical attention if one or both of your eyes are red and painful, particularly if you have a change in your vision. You could go to your GP, an eye hospital, or your local A& E department.
These symptoms could be caused by a condition called uveitis, which is also known as iritis. It involves inflammation at the front of the eye.
This can permanently damage your eyesight if left untreated.
Other symptoms are:
- blurred or cloudy vision
- sensitivity to light
- not being able to see things at the side of your field of vision known as a loss of peripheral vision
- small shapes moving across your field of vision.
These symptoms can come on suddenly, or gradually over a few days. It can affect one or both eyes. It can be treated effectively with steroids.
Heart
Psoriatic arthritis can put you at a slightly higher risk of having a heart condition. You can reduce your risk by:
- not smoking
- staying at a healthy weight
- exercising regularly
- eating a healthy diet, thats low in fat, sugar and salt
- not drinking too much alcohol.
These positive lifestyle choices can help to improve your arthritis and skin symptoms.
Talk to your doctor if you have any concerns about your heart health.
Crohns disease
Non-alcoholic fatty liver disease
Also Check: Remedy For Arthritis Pain In Hands
Infection Rates In People With Psoriatic Arthritis Arent Rising Theyre Declining
Whats New Biologic therapies now available are an important tool for treating people with psoriatic arthritis because they may control disease activity and prevent joint damage. One limitation of these drugs, however, is that they can increase the risk of infection.
Researchers from Boston University Medical Center decided to see if infection rates have indeed gone up in recent years, a time when the use of biologics has grown.
What they found is that, during the years studied, infection rates actually went down.
Research Details The scientists examined data from the National Inpatient Sample, a database that includes a sample of discharge information from community hospitals, containing approximately seven million records.
They compared the discharge records by type of infection during the five-years studied, from 2012 and 2017, standardizing the results to match the age distribution in the U.S. population during that time.
These hospital records revealed that major infections of the skin, soft tissue, and urinary tract, as well as the blood infection known as , all declined. Pneumonia was the only infectious disease whose rate stayed the same.
With infection rates declining, people can feel more comfortable knowing that the increasing use of biologics has not translated into a corresponding growth in serious infections.
Treatment For Psoriatic Arthritis
There are many treatments available for psoriatic arthritis. Your PsA treatment plan may include medications, physical therapy and/or occupational therapy, exercise, rest, and complementary therapies like massage and acupuncture. Following your treatment plan can help reduce the symptoms of the disease and prevent joint damage caused by arthritis.
Read Also: Ra Pain Relief
There Are Many Drug Options For Managing Active Psa Heres What Happened When A Study Compared Them With Each Other
New psoriatic arthritis treatment guidelines from the American College of Rheumatology say that most people with active psoriatic arthritis should choose an anti-TNF drug, such as adalimumab or infliximab , as their first line of therapy.
If a patient doesnt respond well to one or more of these drugs or cant take them for some reason, they might then consider a newer type of biologic an interleukin inhibitor like ustekinumab or secukinumab .
Although interleukin inhibitors have also been proven to help patients with psoriatic arthritis, there havent been many large studies directly measuring them against anti-TNF drugs.
A new study published in the Journal of Rheumatology aimed to compare these classes of medication in terms of how well they work for two specific complications of psoriatic arthritis: enthesitis and dactylitis .
This study, a literature review that analyzed data from 18 previous trials, included information on a total of nearly 7,000 psoriatic arthritis patients who had enthesitis and dactylitis. Researchers determined that both types of drugs beat out placebos and that they worked equally well for PsA patients with enthesitis and dactylitis.
After 24 weeks, the anti-TNF drugs demonstrated significant resolution of these complications, the authors reported. The two classes also worked similarly in terms of improving disease activity scores as well as quality of life scores.
What Are The Symptoms Of Psoriasis
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
Recommended Reading: How To Deal With Arthritis
Is Walking Good For Psoriatic Arthritis
The best endurance exercises for people who have psoriatic arthritis are walking, swimming, and biking, Lindsey says. If youre able, running is fine too.
What is worse lupus or psoriatic arthritis? The symptoms of psoriasis and lupus may take effect throughout the body, but they can be particularly apparent on the skin or in the joints. While psoriasis and psoriatic arthritis can be uncomfortable, they are generally less serious than lupus and may cause less severe symptoms.
Join our Advertising Community and share you ideas today !
Are Biologics Worth The Risk
Biologic meds raise your risk of infection because they weaken your immune system. You could get a cold, a sinus infection, an upper respiratory tract infection, bronchitis, or a urinary tract infection . One study found that people who take these drugs may also be more likely to test positive for COVID-19.
Is Cosentyx safer than Humira?
And Cosentyx causes fewer side effects, particularly serious side effects, than Humira. But its also important to consider your health history. For example, if you have inflammatory bowel disease, taking Cosentyx could make it worse. On the other hand, Humira is approved to treat this condition.
How I cured my psoriatic arthritis naturally? Natural remedies
- Turmeric. Curcumin, which is an ingredient in turmeric, appears to have anti-inflammatory properties.
- Capsaicin. Capsaicin is the compound that makes chili peppers hot.
- Epsom salts.
- Avoid or quit smoking.
- Massage therapy.
Is psoriatic arthritis considered a disability? If you have psoriatic arthritis, you may qualify for Social Security disability insurance. Your level of benefits depends on your ability to work and how long youve been paying into Social Security. Youll need a lot of documentation to make your case, but the effort is worth it.
Also Check: Ra And Leg Cramps