Complementary And Alternative Therapies
You can try:
- Acupressure and acupuncture: These ancient Chinese treatments involve putting pressure on or inserting needles into the bodyâs healing points or energy lines. Acupressure isnât proven to help, but studies show that acupuncture can ease your pain.
- Curcumin: Thereâs some proof that this substance, the active ingredient in the spice turmeric, can help curb inflammation.
- Massage: It can help stretch your muscles and joints, promote circulation in your lymph system, and help you relax.
- Reiki: This Japanese relaxation technique can help you manage stress.
- Tai chi: This gentle Chinese exercise helps with relaxation and can ease sore, stiff joints.
- Yoga: The controlled movements can relax stiff muscles, ease sore joints, and boost your range of motion. It can also help with pain.
- Vitamin D: As an ointment, itâs been used to treat psoriasis for years. You can also get it from foods like:
- Cod-liver oil
You May Like: Is Bee Pollen Good For Arthritis
How Are Biologic Dmards Used To Treat Psa
It is a traditional drug that targets the entire immune system. In recent years, however, biologic DMARDs have played an increasing role in PsA treatment. Biologics are a type of targeted drug made from genetically engineered proteins. They reduce inflammation by blocking the action of specific proteins or cells in the immune system.
Dont Miss: Is Tomatoes Bad For Arthritis
Table 2 How And When To Take A Biologic Drug
| Drug name | How the drug is given | How often |
| Adalimumab | Under the skin |
Psoriasis: Two injections the first week, followed by another injection the second week. Every other week after. Psoriatic arthritis: Every other week. |
| Certolizumab | ||
|
Psoriasis: Twice weekly for 3 months, followed by once weekly. Psoriatic arthritis: Once weekly. |
||
| Given in weeks 0, 2, and 6, then every 8 weeks. | ||
| Ustekinumab | Under the skin | Two injections separated by 4 weeks repeat treatment every 12 weeks. |
Some of the biologics have multiple uses and are also approved for treating other diseases such as ankylosing spondylitis, Crohns disease, rheumatoid arthritis, ulcerative colitis, and other autoimmune diseases.
Also Check: Best Treatment For Arthritis In Fingers
There Are Many Drug Options For Managing Active Psa Heres What Happened When A Study Compared Them With Each Other
New psoriatic arthritis treatment guidelines from the American College of Rheumatology say that most people with active psoriatic arthritis should choose an anti-TNF drug, such as adalimumab or infliximab , as their first line of therapy.
If a patient doesnt respond well to one or more of these drugs or cant take them for some reason, they might then consider a newer type of biologic an interleukin inhibitor like ustekinumab or secukinumab .
Although interleukin inhibitors have also been proven to help patients with psoriatic arthritis, there havent been many large studies directly measuring them against anti-TNF drugs.
A new study published in the Journal of Rheumatology aimed to compare these classes of medication in terms of how well they work for two specific complications of psoriatic arthritis: enthesitis and dactylitis .
This study, a literature review that analyzed data from 18 previous trials, included information on a total of nearly 7,000 psoriatic arthritis patients who had enthesitis and dactylitis. Researchers determined that both types of drugs beat out placebos and that they worked equally well for PsA patients with enthesitis and dactylitis.
After 24 weeks, the anti-TNF drugs demonstrated significant resolution of these complications, the authors reported. The two classes also worked similarly in terms of improving disease activity scores as well as quality of life scores.
What Is A Biologic
Biologics are medications that can be used to treat certain types of arthritis. They are a type of medication called a disease-modifying anti-rheumatic drug or DMARD for short which may prevent the development of joint damage. DMARDs, including biologics, are different to medicines that simply block the pain or other symptoms youre feeling. They work by blocking specific substances in the immune system.
Usually the immune system fights infections to keep you healthy. In autoimmune diseases such as rheumatoid arthritis, the immune system mistakenly takes aim at itself, attacking its own healthy tissues. This leads to very high levels of certain natural substances, called cytokines, in the body that then cause joint inflammation and pain. Biologics are very effective at blocking these substances. This dampens down the immune system, and reduces inflammation, pain and damage to the joint.
Biologics mimic substances naturally produced by the body. They are made from living cells, which is the key difference from most other medicines that are made from man-made or chemical compounds. They can be very effective in treating inflammatory arthritis and tend to work more quickly than conventional DMARDs . There are a number of biologics that target different parts of the immune system. If your arthritis does not respond to one type of biologic, your rheumatologist may use a different biologic to see if it works better for you.
Read Also: Does Rheumatoid Arthritis Cause A Rash
Impact Of Biologics On Comorbidities
Psoriasis imposes a psychological burden on patients. The prevalence of having depression or anxiety is higher in psoriasis patients than in controls . A systematic review and meta-analysis investigating 18 studies including a total of 1,767,583 participants, of whom 330,207 had psoriasis, reported that patients with psoriasis had a significantly higher likelihood of suicidal ideation, suicide attempts, and completed suicides . Strober et al. evaluated the effect of biologic therapy on depression in psoriasis patients utilizing Psoriasis Longitudinal Assessment and Registry . The incidence rates of depressive symptoms were 3.01 , 5.85 , and 5.70 per 100 patient-years for biologics, phototherapy, and conventional therapy, respectively. Compared with conventional therapy, biologics reduced the risk for depressive symptoms , whereas phototherapy did not .
Kaushik and Lebwohl also described specific comorbidities and insights to choose the appropriate systemic treatment in patients with moderate-to-severe psoriasis . The choice of appropriate biologic therapy for a patient is often determined by the presence of comorbidities.
Biologics Are Typically Prescribed To Those With Moderate
Only your doctor can tell you for sure if youre a good candidate for biologic treatment, but in general, they tend to be prescribed to people with moderate-to-severe psoriatic arthritis.
Biologics are also prescribed if other treatments havent worked for you or theres a reason you wouldnt be a good candidate for other first-line treatments. For example, someone who has a lot of stomach issues may not do well with treatments that can cause more stomach problems, so a doctor might go straight to a biologic for them.
Read Also: Arthritis In Fingers Prevention
What If My Needle Phobia Is Severe
The majority of people do get more comfortable self-injecting their biologics over time. However, some people do have serious fears or even phobias of needles. There are a couple options if you cant overcome your fear of needles and its getting in the way of your treatment success.
First, your doctor may decide that a different type of medicine is better for you. For example, there are oral and infusion options. However, theres always a risk that these options may not treat you as well as the biologic could have. This decision will involve weighing the risks and benefits for your health and well-being.
Second, theres a possibility that you might benefit from anti-anxiety medicines to help with severe injection phobias. You would take the prescribed dose beforehand to help avoid anxiety symptoms or even panic attacks during the injection. This isnt the right path for everyone, but it may help for some.
Theyre Administered By Injection Or Infusion
Biologics differ from other psoriatic arthritis treatments because they are not available as a pill. Instead, biologics are often given at home by self-injection, which a doctor can show you how to do. Most self-injections are administered every one to four weeks, Zashin says.
Other biologics are given through an intravenous infusion, which is done in a doctors office every four to eight weeks.
Read Also: Overcome Arthritis
Where Does The Information Come From
Researchers funded by the Agency for Healthcare Research and Quality , a Federal Government research agency, reviewed 16 studies on medicines for psoriatic arthritis published before January 2011. The report was reviewed by clinicians, researchers, experts, and the public. You can read the report at www.effectivehealthcare.ahrq.gov/dmardspsa.cfm.
How Long Can You Live With Psoriatic Arthritis
Psoriatic arthritis is not life-threatening, but affected patients do have a reduced life expectancy of around three years compared to people without the condition. The main cause of death appears to be respiratory and cardiovascular causes. However, treatment can substantially help improve the long-term prognosis.
You May Like: Remedies For Arthritis In Back
Treatment For Psoriatic Arthritis
Treatment for psoriatic arthritis aims to:
- relieve symptoms
- slow the condition’s progression
- improve quality of life
This usually involves trying a number of different medicines, some of which can also treat the psoriasis. If possible, you should take 1 medicine to treat both your psoriasis and psoriatic arthritis.
The main medicines used to treat psoriatic arthritis are:
- non-steroidal anti-inflammatory drugs
- biological therapies
Biological Dmards Other Than Tnfi
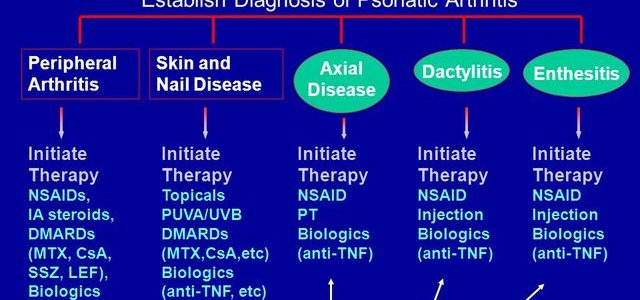
Although TNFi therapy remains central in the management of PsA, new insights into its pathogenesis led to identification of new therapeutic targets, including IL-12, IL-23, and IL-17. The IL-17 signaling pathway plays a relevant role in the pathogenesis of PsA. This proinflammatory cytokine is richly expressed in psoriatic skin lesions and in the synovial fluid of patients and can induce activation and proliferation of keratinocytes and endothelial cells. On the other side, IL-23 has been shown to play an important role in the polarization of CD4+ T-cells to become IL-17 producers. In the last few years, therapeutic agents targeting the IL-23/IL17 axis have been studied for the treatment of PsA.
Pooled meta-analysis was conducted by Mourad et al identifying RCTs evaluating the efficacy of TNF-i, anti-IL12/23 , and anti-IL17 in treating PsA and conducting a meta-analysis of these agents for treatment of dactylitis and enthesitis. Their results showed that TNF-i and IL inhibitors brought dactylitis to a significant resolution at week 24, with pooled risk ratios versus placebo of 2.57 and 1.88 respectively. For resolution of enthesitis at week 24, RR for TNF-i was 1.93 versus 1.95 for IL inhibitors. According to these results, TNF-i demonstrated the same efficacy of IL inhibitors in treating the two PsA manifestations.
Recommended Reading: Am I Getting Arthritis
Clinical Features Associated With Predicting Treatment Response
Recent ACR PsA guidelines advocate the early introduction of biologic treatment in cases of aggressive disease, even if no csDMARDs have been used . The European guidelines support the use of early biologic therapy if axial or entheseal disease is the predominant issue . The recommended first-line biologic therapy is TNFi treatment unless it is contraindicated. There is a paucity of data in the literature to guide treatment decisions in PsA . Data from prospective research has demonstrated that obesity, female gender, old age, and a longer duration of the disease were associated with a lower probability of achieving sustained remission . Moreover, a low HAQ score and a high CRP level at baseline were associated with a better response . Unfortunately, to date there has been no suggestion that different musculoskeletal subtypes of PsA do better or worse on TNFi treatment .
These findings underpin the importance of IL-12, IL-23 and IL-17 in enthesitis. However, as stated, there are limitations to the reliability of clinical examination in enthesitis, and thus there is not yet enough data to support the superiority of any. The extent of PsO is the only emerging clinical domain that could potentially be used to decide between these therapies at present, especially after the failure of a TNFi. Other considerations for a switch of drug class include the presence of IBD , and preference for an oral medication or a reduced dosing schedule .
What Are The Symptoms Of Psoriatic Arthritis
Symptoms of psoriatic arthritis may come and go. This is known as flareups and remission. They can affect the joints on only one side of the body although some patients may experience them on both sides. These symptoms often include:
- Fatigue
- Developing red patches on your skin
- A throbbing sensation on the joints
- Nails separating from the nail bed
If youre an adult and youve been taking oral prescription medications but are still experiencing chronic flare-ups, you may need more effective infusion medication, such as Simponi Aria.
Also Check: Can Osteoarthritis Turn Into Rheumatoid Arthritis
I Wrote A Childrens Book
Terysa Ridgeway, 38, didnt think shed be the one diagnosed with a health condition after taking her daughter to the doctor for an ear infection eight years ago. Ridgeway mentioned the swelling she had in her hands and feet to the doctor, which led to a whirlwind of tests that lasted three weeks. By the time she finished her last test, Ridgeway says the pain and stiffness were so bad that she couldnt even get out of bed.
It was the most horrific thing, Ridgeway tells SELF. She was eventually diagnosed with psoriatic arthritis and rheumatoid arthritis.
Her doctor recommended several disease-modifying anti-rheumatic drugs : a family of medications that help prevent the immune system from going haywire and causing inflammation, according to the Cleveland Clinic. None of them worked for her, but she found temporary pain relief through steroid injections, which reduced the inflammation that was setting off her symptoms. But these eventually stopped working, so Ridgeway began taking a biologic medication: a type of DMARD that targets a specific immune pathway connected to arthritis.
Genetic Markers Associated With Treatment Response
We know that PsA has a strong genetic component. Key single nucleotide polymorphisms are implicated in the pathogenesis, including HLA and non-HLA loci. A number of key genetic associations are strongly associated with the development of enthesitis .
Polymorphisms in the TNF promoter regions have relevance in predicting response to treatment. The TNF-induced protein 2 gene or A20 have been associated with response to TNFi treatment . TNFAIP3 was first described as a negative feedback inhibitor of TNF, terminating activation of the NFB transcription factor.IL-17 also induces expression of the TNFAIP3 gene. Interestingly A20 interacts with IL-17 differently compared with other pathways, and research is needed to clarify whether polymorphisms at A20 alter the effectiveness of IL-17 inhibitors compared with TNFi. Other SNPs that have been under investigation include polymorphisms at the TNF- gene , TNF receptor 1A gene and the TNF-related apoptosis-inducing ligand receptor 1 gene , along with the FCGR2A polymorphism FCGR2A-131H .
You May Like: Arthritis Remission
Basics Of Psoriatic Arthritis
PsA is a type of inflammatory arthritis that often affects people who already have the inflammatory skin condition psoriasis.
Psoriasis is known for causing patches of red, inflamed skin with white, silvery flakes. PsA affects up to 30% of people with psoriasis.
Joint pain, stiffness, and swelling are the main symptoms of PsA. These symptoms can affect any part of the body, including the fingers and spine, and symptoms range from mild to severe.
PsA, much like psoriasis, causes periods of flare-ups and periods of remission .
There’s no cure for PsA. Healthcare providers focus on controlling symptoms and preventing joint damage. Without treatment, PsA can lead to permanent damage and disability.
Biologics are a type of disease-modifying anti-rheumatic drug designed to manage PsA symptoms and slow down PsA disease progression.
Researchers consider biologic drugs to be the most targeted therapies for treating PsA.
Traditional DMARDs, like methotrexate, suppress the entire immune system. Biologics only target parts of the immune system that are linked to PsA. This includes immune cells and inflammatory proteins such as:
- T-cells
- Interleukins 12, 17, and 23
These cells and proteins play a significant part in the development and progression of PsA and psoriasis.
Who Can Take Biosimilars
All biologics, including biosmilars, are typically prescribed for people with more advanced disease, including individuals with moderate-to-severe psoriasis and active PsA. But each of the three approved biosimilars are indicated for different groups within this population.
You should not take biosimilars if:
- Your immune system is significantly compromised
- You have an active infection
Screening for tuberculosis or other infectious diseases is required before starting treatment with all biologics, including biosimilars.
Also Check: Rheumatoid Arthritis One Side Of Body
Can Imaging Help In Assessing Treatment Response
Going forward, we have a choice to scan and research each domain of PsA separately or attempt to cover all domains with one composite score. The PsA-Son scores include entheses examination, and other composite US scores have attempted to reflect the heterogeneity of PsA. The five Targets PwD for Psoriatic Disease is another example . This score recognizes the various domains in PsA and can be used to monitor power Doppler at the joint, enthesis, skin, nail, tendons and synovial sheath. This score is much more feasible, but it focuses on areas that are difficult to scan, including the skin and nails.
There is evidence of an association between nail disease and enthesitis at the DIP joint in PsO . US is able to assess the nail bed, matrix and plate as well as its relationship with the DIP joint of the finger. A high transducer probe can diagnose subclinical psoriatic nail disease and potentially monitor response to treatment. Interestingly a study of PsO patients with nail disease noted a higher incidence of subclinical systemic enthesitis . Thus, nail bed disease merits further investigation to again better stratify patients by phenotype.
Clinical and US imaging of psoriatic nail disease
Should You Take A Biologic
It depends on 5 things:
1. How much of your skin is affected by psoriasis
Doctors often use biologic drugs on people with moderate to severe psoriasis.
- Moderate psoriasis means that 3% to 10% of your body is covered with red, scaly patches.
- Severe psoriasis means that more than 10% of your body is covered.
You may also want to take a biologic drug if you have mild psoriasis but it really bothers you.
2. How much psoriasis affects your life
- If your psoriasis doesnât really bother you, the doctor may tell you that a biologic drug isn’t worth the risks. Biologics suppress your immune system. That means they can make you more likely to get an infection.
- They may not be worth the cost, either. Biologic drugs are expensive. Depending on the drug and the dose, they can cost $10,000 to $30,000 or more a year.
3. Your health
The doctor will take a careful look at your health history. Biologic drugs may not be best for people with certain health conditions, including:
- A history of infections such as tuberculosis
- A history of cancer
- A weak immune system because of a disease like HIV or cancer
Biologics may cause a recurrence of some chronic diseases that are in remission. Also, because biologics suppress the immune system, they could make serious infections more likely.
4. Insurance coverage
5. Your preferences
Don’t Miss: Cabbage Good For Arthritis