Routine Monitoring And Ongoing Care
Regular medical care is important because your doctor can:
- Monitor how the disease is progressing.
- Determine how well the medications are working.
- Talk to you about any side the effects from the medications.
- Adjust your treatment as needed.
Monitoring typically includes regular visits to the doctor. It also may include blood and urine tests, and xrays. Having rheumatoid arthritis increases your risk of developing osteoporosis, particularly if you take corticosteroids. Osteoporosis is a bone disease that causes the bones to weaken and easily break. Talk to your doctor about your risk for the disease and the potential benefits of calcium and vitamin D supplements or other osteoporosis treatments.
The 4 Stages Of Rheumatoid Arthritis
RA is a progressive disease. That means that if RA is left untreated, symptoms will continue to worsen over time. But while 30 years ago that might have meant a person with rheumatoid arthritis was eventually headed for a wheelchair, today that outcome is increasingly unlikely. Whats changed? The treatments available today can slow or even halt the disease, protecting the health of your joints and the rest of your body. Once appear, the goal of treatment remains the same no matter the stage: get RA into remission or at least make the disease less active.
The Treatments For Rheumatoid Arthritis
Thankfully, there are ways to reduce pain caused by rheumatoid arthritis. There are treatments that can help to reduce inflammation, soothe pain and prevent or slow down joint damage and disability. Treating rheumatoid arthritis can involve taking medication, lifestyle changes, physical therapy and surgery. For more information regarding the range of treatments you may be offered, visit the NHS website. A rheumatoid arthritis diagnosis can be life changing, but that doesnt mean your life has to completely change. Many people living with rheumatoid arthritis are able to live a healthy, active lifestyle with the help of treatments that can slow down the progression of the disease. Remember, the four stages of rheumatoid arthritis may sound scary, but a lot of people never reach the later stages within their lifetime, and it can take many years to advance through the different stages. For more information about rheumatoid arthritis, visit the NHS or Versus Arthritis website.
Also Check: Does Exercise Help Arthritis In Back
How Is Ra Treated
RA can be effectively treated and managed with medication and self-management strategies. Treatment for RA usually includes the use of medications that slow disease and prevent joint deformity, called disease-modifying antirheumatic drugs biological response modifiers are medications that are an effective second-line treatment. In addition to medications, people can manage their RA with self-management strategies proven to reduce pain and disability, allowing them to pursue the activities important to them. People with RA can relieve pain and improve joint function by learning to use five simple and effective arthritis management strategies.
What Are The Signs And Symptoms Of Ra
With RA, there are times when symptoms get worse, known as flares, and times when symptoms get better, known as remission.
Signs and symptoms of RA include:
- Pain or aching in more than one joint
- Stiffness in more than one joint
- Tenderness and swelling in more than one joint
- The same symptoms on both sides of the body
Recommended Reading: Can Psoriatic Arthritis Cause Fatigue
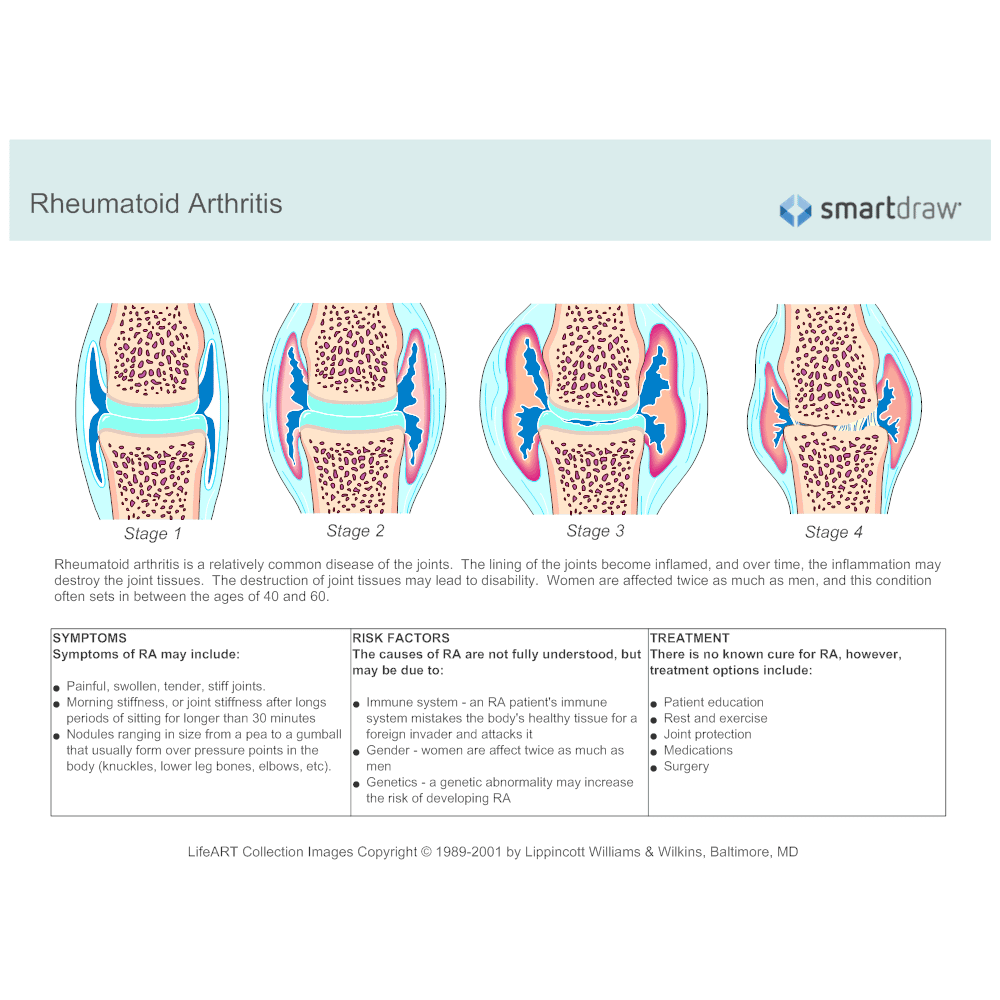
What Are The Four Stages Of Rheumatoid Arthritis
- Stage 1: In early stage rheumatoid arthritis, the tissue around your joint is inflamed. You may have some pain and stiffness. If your provider ordered X-rays, they wouldnt see destructive changes in your bones.
- Stage 2: The inflammation has begun to damage the cartilage in your joints. You might notice stiffness and a decreased range of motion.
- Stage 3: The inflammation is so severe that it damages your bones. Youll have more pain, stiffness and even less range of motion than in stage 2, and you may start to see physical changes.
- Stage 4: In this stage, the inflammation stops but your joints keep getting worse. Youll have severe pain, swelling, stiffness and loss of mobility.
Diagnosis Of Rheumatoid Arthritis
- Ordering laboratory tests.
- Ordering imaging studies, such as x-rays or ultrasound.
It can be difficult to diagnose rheumatoid arthritis when it is in the early stages because:
- The disease develops over time, and only a few symptoms may be present in the early stages.
- There is no single test for the disease.
- Symptoms differ from person to person.
- Symptoms can be similar to those of other types of arthritis and joint conditions.
As a result, doctors use a variety of tools to diagnose the disease and to rule out other conditions.
Read Also: Is Psoriatic Arthritis Considered An Autoimmune Disease
What Is Rheumatoid Arthritis
Rheumatoid arthritis, or RA, is an autoimmune and inflammatory disease, which means that your immune system attacks healthy cells in your body by mistake, causing inflammation in the affected parts of the body.
RA mainly attacks the joints, usually many joints at once. RA commonly affects joints in the hands, wrists, and knees. In a joint with RA, the lining of the joint becomes inflamed, causing damage to joint tissue. This tissue damage can cause long-lasting or chronic pain, unsteadiness , and deformity .
RA can also affect other tissues throughout the body and cause problems in organs such as the lungs, heart, and eyes.
How Your Ra Treatment Plan Prevents Disease Progression
Perhaps the biggest factor that affects how RA progresses is if youre in treatment with a specialist who can put you on medications to slow the disease. Being on a DMARD or biologic therapy for RA is the best way to prevent progression, Dr. Lally says.
Disease-modifying anti-rheumatic drugs are usually the first line in medication. Methotrexate is the anchor drug for rheumatoid arthritis, Dr. Bhatt says. Some patients are scared because methotrexate is also used for cancer chemotherapy so they dont want to take a chemo pill, but those we use for RA are a very small dose with lesser chance of side effects. Your doctor will reassess in a month or so and see if its necessary to add in other drugs.
If after three to six months they have still not responded then we progress to medications called biologics, Dr. Bhatt says. These genetically engineered drugs target the inflammation process specifically, and are usually self-injected or infused via IV in your doctors office or a medical center. There are sub-classes and different types, Dr. Bhatt says. Your doctor will try various medications to see which you respond best to.
Also Check: What Can I Do For Arthritis In My Big Toe
What Are The Risk Factors For Ra
Researchers have studied a number of genetic and environmental factors to determine if they change persons risk of developing RA.
Characteristics that increase risk
- Age. RA can begin at any age, but the likelihood increases with age. The onset of RA is highest among adults in their sixties.
- Sex. New cases of RA are typically two-to-three times higher in women than men.
- Genetics/inherited traits. People born with specific genes are more likely to develop RA. These genes, called HLA class II genotypes, can also make your arthritis worse. The risk of RA may be highest when people with these genes are exposed to environmental factors like smoking or when a person is obese.
- Smoking. Multiple studies show that cigarette smoking increases a persons risk of developing RA and can make the disease worse.
- History of live births. Women who have never given birth may be at greater risk of developing RA.
- Early Life Exposures. Some early life exposures may increase risk of developing RA in adulthood. For example, one study found that children whose mothers smoked had double the risk of developing RA as adults. Children of lower income parents are at increased risk of developing RA as adults.
- Obesity. Being obese can increase the risk of developing RA. Studies examining the role of obesity also found that the more overweight a person was, the higher his or her risk of developing RA became.
Characteristics that can decrease risk
The Stages Of Osteoarthritis
- Early-Stage Osteoarthritis: In the early stage of osteoarthritis, the cartilage located in a joint begins to thin. This continues until the person begins to experience occasional pain, as friction develops between the bones at the joint. In this stage of the condition, losing weight and reducing stress on the joints can help reduce the pain. In the early stage of osteoarthritis, it is common to have one or more joints experiencing symptoms.
- Moderate-Stage Osteoarthritis: In this stage, patients often begin to take medications to control the pain. The joints become inflamed and painful much more often during this stage. While its common to experience more pain when pressure is put on joints in this stage, living a moderately active lifestyle actually helps reduce pain.
- Late-Stage Osteoarthritis: In this stage of osteoarthritis, pain, stiffness, and inflammation are common in multiple joint areas. Its common to take stronger pain medications to help reduce pain. Its also common to get joint replacement surgery in this stage, because medications and other treatment methods are not working to reduce pain and to increase mobility.
Don’t Miss: How To Manage Rheumatoid Arthritis Naturally
Rheumatoid Arthritis Stages And Progression
Rheumatoid arthritis is an inflammatory autoimmune disease that leads to joint inflammation, swelling, and pain, which often appear symmetrically on both sides of the body. RA has four stages, with joint damage becoming progressively worse with each stage. Rheumatologists determine each stage of RA depending on how severe it is.
Although there is no cure for RA, several treatments can help limit the disease progression and slow the damage to joints. Those treatments can vary from stage to stage.
Talk To People Who Understand

By joining myRAteam the social network for people with rheumatoid arthritis and their loved ones you can connect with more than 191,000 members who understand life with RA. Every day, members come together to ask questions, give advice, and share their stories.
What stage is your RA, and how are you managing it? Share your experience in the comments below, or share your story on myRAteam.
Don’t Miss: Do I Have Gout Or Arthritis
Can Rheumatoid Arthritis Go Away
No, rheumatoid arthritis doesnt go away. Its a condition youll have for the rest of your life. But you may have periods where you dont notice symptoms. These times of feeling better may come and go.
That said, the damage RA causes in your joints is here to stay. If you dont see a provider for RA treatment, the disease can cause permanent damage to your cartilage and, eventually, your joints. RA can also harm organs like your lung and heart.
A note from Cleveland Clinic
If you have rheumatoid arthritis, you may feel like youre on a lifelong roller coaster of pain and fatigue. Its important to share these feelings and your symptoms with your healthcare provider. Along with X-rays and blood tests, what you say about your quality of life will help inform your treatment. Your healthcare provider will assess your symptoms and recommend the right treatment plan for your needs. Most people can manage rheumatoid arthritis and still do the activities they care about.
Last reviewed by a Cleveland Clinic medical professional on 02/18/2022.
References
Who Treats Rheumatoid Arthritis
Diagnosing and treating rheumatoid arthritis requires a team effort involving you and several types of health care professionals. These may include:
- Rheumatologists, who specialize in arthritis and other diseases of the bones, joints, and muscles.
- Primary care providers, such as internists, who specialize in the diagnosis and medical treatment of adults.
- Orthopaedists, who specialize in the treatment of and surgery for bone and joint diseases or injuries.
- Physical therapists, who help to improve joint function.
- Occupational therapists, who teach ways to protect joints, minimize pain, perform activities of daily living, and conserve energy.
- Dietitians, who teach ways to eat a good diet to improve health and maintain a healthy weight.
- Nurse educators, who specialize in helping people understand their overall condition and set up their treatment plans.
- Mental health professionals, who help people cope with difficulties.
You May Like: What Can Cause Arthritis In The Knee
When To Get Medical Advice
See a GP if you think you have symptoms of rheumatoid arthritis, so they can try to identify the underlying cause.
Diagnosing rheumatoid arthritis quickly is important, because early treatment can prevent it getting worse and reduce the risk of joint damage.
Find out more about diagnosing rheumatoid arthritis.
Home Remedies For Managing Ra
In addition to medication and surgery, patients may want to ask their doctor about simple therapies they can do at home, such as exercise and diet.
Exercise
Low impact exercises can strengthen muscles and improve flexibility. These include walking, water aerobics, swimming and yoga.
According to a 2012 review published in Open Access Journal of Sports Medicine by Shirley Telles and Nilkamal Singh, yoga has shown some promise in reducing pain, improving function and providing mental health benefits.
A small 2019 study by researcher Surabhi Gautam and colleagues published in Restorative Neurology and Neuroscience found that yoga eased physical symptoms and improved mental health.
Diet
Evidence suggests that eating a healthy diet with anti-inflammatory foods can ease RA symptoms. There isnt a specific regimen to follow, but a 2018 review recommended the Mediterranean diet and fish oil for people with RA, Today reported.
In general, keeping a healthy weight and getting the proper nutrition helps manage inflammation that can worsen RA.
Foods that may manage RA symptoms include:
- Fatty fish like salmon, sardines and tuna
- Fruits and vegetables
Getting Enough Sleep
People with RA often suffer from fatigue and pain that can get worse during flare-ups. Make sure to get plenty of rest.
Hot and Cold Therapy
On This Page
Don’t Miss: Can You Get Ssdi For Rheumatoid Arthritis
How Is Severe Rheumatoid Arthritis Pain Treated
Your doctor may recommend a combination of medication and self-management strategies for treating severe RA pain. While there is no cure for RA, medications can help, according to the Centers for Disease Control and Prevention .
What Is The Rheumatoid Arthritis Severity Scale
Rheumatoid arthritis is a chronic and progressive disease. Understanding its severity is an important factor in helping you and your doctor evaluate whether treatments are working, what treatments to consider next, and how to prevent progression and damage in the future.
The Rheumatoid Arthritis Severity Scale was designed to help doctors determine disease activity, as well as functional impairment and physical damage caused by RA.
Different doctors use different assessments to measure disease activity. Besides the RASS, other measurement methods exist. They include the Disease Activity Score-28 , Clinical Disease Activity Index , and Routine Assessment of Patient Index Data .
In recent years, these assessments have generally replaced the RASS.
The CDAI and RAPID3 tend to be the methods doctors prefer, due to the short amount of time it requires to make assessments, according to
You May Like: Can You Get Arthritis In Your Brain
Treatment Of Stage 4 Ra
After trying all medical options, surgery may be the next option for patients with stage 4 RA. Surgery may be required to repair joint damage, repair tendons, remove the synovium or nodules, separate fused joint, or replace a damaged joint.
Patients usually rely on assistive mobility devices to perform their daily tasks.
Joint Damage Pain Deformities Loss Of Function: Late
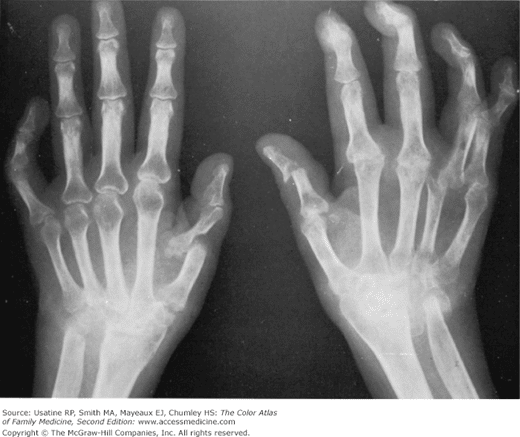
It is important for people with these symptoms to be diagnosed as soon as possible, because if RA isnt diagnosed and treated early the synovial lining can become so inflamed that it damages and erodes the cartilage this makes bone loss more likely.
Moving joints becomes more difficult, and flare-ups can occur with greater frequency. These joint changes are called erosions, and they can lead to deformities of the bone, such as crooked fingers, says Daniel Solomon, MD, MPH, chief of the section of clinical sciences in the division of rheumatology at Brigham and Womens Hospital in Boston. In severe cases, bones may eventually fuse together. All of this further contributes to pain and loss of function.
You May Like: What Foods To Not Eat With Arthritis
You May Like: How Young Can You Get Arthritis
What Is Osteoarthritis
Osteoarthritis is the most common type of arthritis and affects millions of people. Osteoarthritis causes the protective cartilage located at the joints to deteriorate and break down. This results in inflammation and pain caused by the bones rubbing against each other.
Cartilage serves a very important role in the joints of the body. Its a rubber-like covering that serves as a shock absorber and allows the bones in a joint to glide around each other painlessly. When the cartilage breaks down, the bones no longer have a protective barrier between them.
Osteoarthritis has a slow progression, and it can take years to move from stage to stage.
Stage : The End Stage
In the end stage, much of the inflamed tissue surrounding the affected joints has completely eroded away, and bone has eroded as well. The joint no longer functions. There is pain, and mobility is compromised.
In terms of treatment, controlling pain is the most important factor. Many patients benefit from pain killers, muscle relaxers and even mild doses of antidepressants or a combination of these treatments.
In some cases, the medical team may recommend joint replacement to bring back mobility and minimize the need for painkillers.
Also Check: What Can I Give My Dog For Arthritis Pain Natural