Why Your Mental Health Matters When Living With Psoriatic Arthritis
Living with a chronic condition that requires life-long management to ease pain and reduce disease progression can take its toll on a persons mental and emotional reserves. Anxiety and depression are both prevalent in people with psoriatic arthritis, with data showing 1 in 3 patients with at least mild anxiety and 1 in 5 with at least mild depression.
Not only do anxiety and depression interfere with your quality of life, but they also are linked to greater disease activity.13 So it is important to recognize any mental or emotional challenges you may be feeling and seek help.
Misdiagnosis Is A Chronic Problem
Psoriatic arthritis shares some symptoms with other conditions, such as rheumatoid arthritis, osteoarthritis, fibromyalgia, lupus, and gout. This can make getting an accurate diagnosis difficult.
In a study published in June 2018 in the British Medical Journal, investigators found that 96 percent of people who were diagnosed with psoriatic arthritis received at least one prior misdiagnosis.
What Does Psoriatic Arthritis Pain Feel Like Symptoms Treatment
Psoriatic arthritis is a type of inflammatory arthritis that causes pain, stiffness, and swelling in the joints. The condition can develop in patients who have psoriasis, a chronic autoimmune skin condition that causes rapid skin cell growth and renewal.
The joint pain, swelling, and stiffness felt in psoriatic arthritis are often just on one side of the body. Psoriatic arthritis pain can affect any joint, but commonly occurs in large joints of the lower extremities such as the knees and ankles.
Pain may also occur in the neck, lower back, hips, shoulders, heels, and feet.
Psoriatic arthritis pain may be described as:
- Worse in the morning or after resting
- Tender
Don’t Miss: Rheumatoid Arthritis And Itching
Types Of Psoriatic Arthritis And Where Psa Shows Up On The Body
Most people will experience psoriatic arthritis in a few joints but there are different types and locations on the body where it may show up.
In fact, you may be told you have a specific type of PsA based on where the inflammation occurs. Some people experience asymmetric symptoms in which joints on one side of the body are affected, such as one wrist or one knee, while others have symmetricsymptoms, involving the same joints on both sides of the body, such as both knees.
The most common types are:
- axial spondyloarthritis which mainly affects your back, including your sacroiliac joints . About 40% of those with PsA joint pain experience spine and sacroiliac joint pain.4
- distal, small joint polyarthritis, especially involving what are called the distal interphalangeal joints thats your first knuckle from the top of the finger. About 50% of people with PsA experience inflammation in the entire finger this is clinically termed dactylitis you may hear people call it sausage digit or sausage finger. Toes may also be affected.
- symmetric, small joint polyarthritis, which affects multiple joints on both sides of your body and can be very similar to rheumatoid arthritis a rheumatologist can help to differentiate
- asymmetric oligoarthritis, meaning a few joints are affected on one side of your body, usually your lower body such as the knee, ankle, or foot.
How Will Psoriatic Arthritis Affect Me
Starting the right treatment as soon as possible will give you the best chance of keeping your arthritis under control and minimise damage to your body.
Psoriatic arthritis can vary a great deal between different people. This makes it difficult to offer advice on what you should expect.
It will usually have some effect on your ability to get around and your quality of life, but treatment will reduce the effect it has.
Psoriatic arthritis can cause long-term damage to joints, bones and other tissues in the body, especially if it isnt treated.
Also Check: Rf Negative Rheumatoid Arthritis
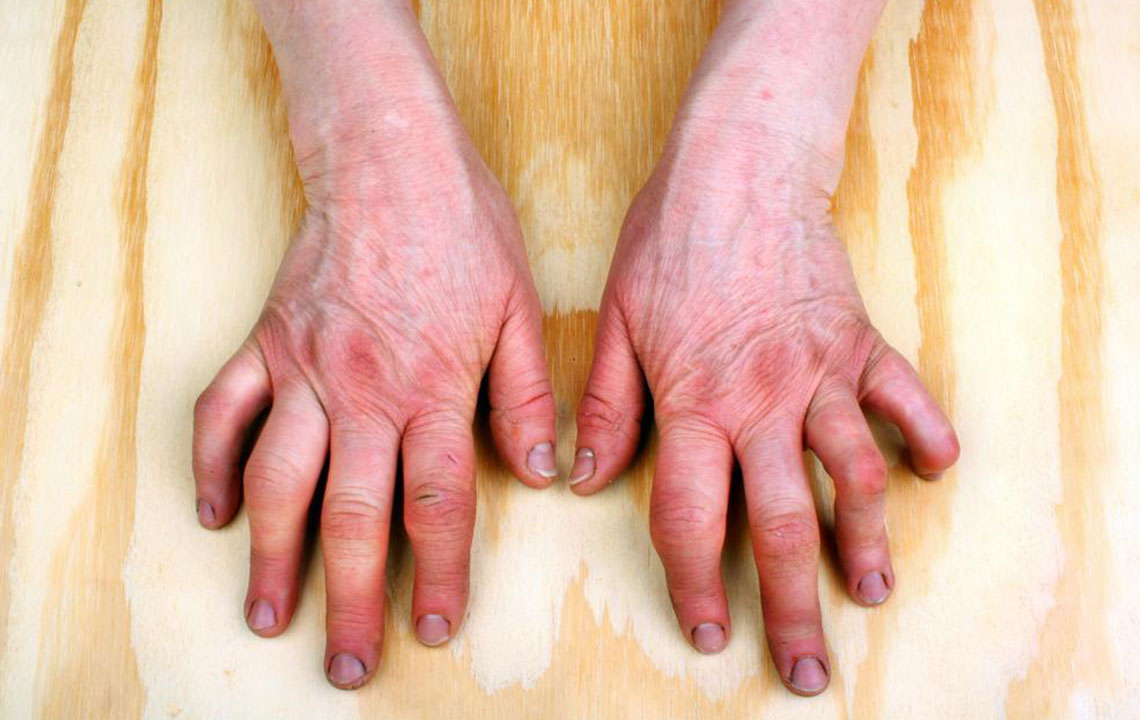
Swollen Joints Fingers And Toes
Often you’ll notice swelling in your knees, ankles, feet, and hands. Usually, a few joints are inflamed at a time. They get painful and puffy, and sometimes hot and red. When your fingers or toes are affected, they might take on a sausage shape. Psoriatic arthritis might affect pairs of joints on both sides of your body, like both of your knees, ankles, hips, and elbows.
Can Psoriatic Arthritis Affect Other Parts Of The Body
Having psoriatic arthritis can put you at risk of developing other conditions and complications around the body.
The chances of getting one of these are rare. But its worth knowing about them and talking to your doctor if you have any concerns.
Eyes
Seek urgent medical attention if one or both of your eyes are red and painful, particularly if you have a change in your vision. You could go to your GP, an eye hospital, or your local A& E department.
These symptoms could be caused by a condition called uveitis, which is also known as iritis. It involves inflammation at the front of the eye.
This can permanently damage your eyesight if left untreated.
Other symptoms are:
- blurred or cloudy vision
- sensitivity to light
- not being able to see things at the side of your field of vision known as a loss of peripheral vision
- small shapes moving across your field of vision.
These symptoms can come on suddenly, or gradually over a few days. It can affect one or both eyes. It can be treated effectively with steroids.
Heart
Psoriatic arthritis can put you at a slightly higher risk of having a heart condition. You can reduce your risk by:
- not smoking
- staying at a healthy weight
- exercising regularly
- eating a healthy diet, thats low in fat, sugar and salt
- not drinking too much alcohol.
These positive lifestyle choices can help to improve your arthritis and skin symptoms.
Talk to your doctor if you have any concerns about your heart health.
Crohns disease
Non-alcoholic fatty liver disease
Recommended Reading: Psoriatic Arthritis Rash Hands
Your Fingers And Toes Are Very Swollen
Dactylitis, a fancy term for when your fingers or toes swell up to an extreme and painful degree, is considered one of the hallmark symptoms of psoriatic arthritis. In addition to the swelling and pain, it can cause the affected parts of your body to redden and feel warm, and it often comes along with enthesitis, which essentially means that the various connective tissues that link to your bones feel tender and sore. Research suggests that dactylitis affects between 16% and 49% of people with psoriatic arthritis.
This symptom is the result of inflammation in small joints and the spots where ligaments and tendons connect to bones. As youll see, this inflammation can result in a number of symptoms, but this is one of the most classic that people with psoriatic arthritis experience.
Reduced Range Of Motion
One possible sign of PsA is a reduced range of motion in your joints. You might find it harder to extend your arms, bend your knees, or bend forward.
You may also have problems using your fingers effectively. This can lead to problems for people who work with their hands in any way, including typing and drawing.
When the joint becomes permanently fixed or unable to move beyond a certain point, its known as a contracture deformity. This can lead to complications such as:
- Dupuytrens contracture, a thickening of the tissue layer beneath the skin in the hands and wrist
- Volkmanns contracture, or lack of blood flow to the forearm that causes muscle shortening
Prevention involves range of motion exercises prescribed by a doctor or done with a physical therapist.
Fatigue is a common symptom in people with PsA. You may begin to have difficulty making it through the day without taking a nap.
According to a , up to 50 percent of people with skin conditions report having moderate to severe fatigue, while 25 percent experience severe levels of fatigue.
In the case of PsA, fatigue may be due to symptoms or complications like:
- inflammation
Recommended Reading: Rheumatoid Arthritis Longterm Effects
What Can I Do Right Now
The Effects Of Psoriatic Arthritis On The Body
PsA is an autoimmune disorder that causes the immune system to attack healthy parts of the body, mostly the skin and the joints.
This causes pain, stiffness, and swelling in the joints, either singly or throughout the body. Early treatment is essential to avoid long-term joint and tissue deterioration.
Psoriatic arthritis usually develops within 10 years of developing psoriasis. Skin psoriasis causes flare-ups of red, patchy skin that can occur anywhere on the body.
According to the National Psoriasis Foundation, about 30 percent of people with psoriasis eventually develop PsA.
In some cases, PsA is diagnosed before you have skin psoriasis because the arthritic symptoms might be more noticeable.
Its also possible to develop PsA without having psoriasis, especially if you have a family history of psoriasis. Both skin psoriasis and inflammatory types of arthritis are considered autoimmune disorders.
PsA is a chronic, or long-term, condition. Anyone can get it, but its most common between ages 30 and 50 years. Since theres no cure, treatment is aimed at managing symptoms and preventing permanent joint damage.
Research theorizes that genetics play a part in the development of psoriatic arthritis. Scientists are trying to find out which genes are involved. Identifying the genes may allow the development of gene therapy treatment.
Don’t Miss: Can You Get Rheumatoid Arthritis In Your Back
Who Will Be Responsible For My Healthcare
Youre likely to see a team of healthcare professionals.
Your doctor, usually a rheumatologist, will be responsible for your overall care. And a specialist nurse may help monitor your condition and treatments. A skin specialist called a dermatologist may be responsible for the treatment of your psoriasis.
You may also see:
- a physiotherapist, who can advise on exercises to help maintain your mobility
- an occupational therapist, who can help you protect your joints, for example, by using splints for the wrist or knee braces. You may be advised to change the way you do some tasks to reduce the strain on your joints.
- a podiatrist, who can assess your footcare needs and offer advice on special insoles and good supportive footwear.
Treatment For Psoriatic Arthritis
Treatment for psoriatic arthritis aims to:
- relieve symptoms
- slow the condition’s progression
- improve quality of life
This usually involves trying a number of different medicines, some of which can also treat the psoriasis. If possible, you should take 1 medicine to treat both your psoriasis and psoriatic arthritis.
The main medicines used to treat psoriatic arthritis are:
- non-steroidal anti-inflammatory drugs
- biological therapies
Don’t Miss: Arthritis In Fingers Prevention
Enthesitis As A Psoriatic Arthritis Symptom
Unfortunately, many doctors and other health care officials overlook or dismiss patients with enthesitis as a symptom of psoriatic arthritis. Patients can go additional months and often even years without the correct diagnosis and treatment because it often isnt identified as a primary symptom in psoriatic arthritis.
Thats part of what makes psoriatic arthritis so sneaky. In reality, it presents itself in so many different ways and enthesitis seems more common than doctors give it credit for. Not to mention that enthesitis is also present in quite a large number of other conditions as well.
How To Treat Psoriatic Arthritis
The main goals in managing PsA are to stop disease progression, reduce inflammation, treat skin symptoms, relieve pain, and keep your joints moving as much as possible.11 A dermatologist and rheumatologist should coordinate your treatment plan. A physical therapist may also be helpful to help increase your flexibility and strength.11
For those people with psoriatic arthritis and psoriasis, your doctor will design a treatment plan that addresses both conditions.
The foundation of PsA treatment includes medications that control inflammation in the body and reduce pain. Medications may include the following and are usually recommended based on the severity of your PsA symptoms.
Mild Disease: The goal of treating mild PsA is primarily to ease pain and reduce inflammation. A number of anti-inflammatory drugs may be recommended, such as:
- Nonsteroidal anti-inflammatory drugs : NSAIDs include drugs like ibuprofen and naproxen sodium that can be purchased over-the-counter as well as prescription-grade NSAIDS, such as celecoxib or diclofenac.
- Corticosteroids: These are more powerful anti-inflammatory drugs that are prescribed by a doctor and can be taken either by mouth or injected in the doctors office. These medications are only used for brief periods of time for disease flare-ups because of their adverse long-term side effects.
Don’t Miss: Arthritis Triggers
Most Rheumatologists And Public Health Experts Want People Living With Rheumatic Diseases Like Psoriatic Arthritis To Get The Vaccine As Soon As They Can
Learn more about our FREE COVID-19 Patient Support Program for chronic illness patients and their loved ones.
If you live with psoriatic arthritis, an inflammatory and autoimmune form of arthritis that affects about 30 percent of people with psoriasis, you may understandably have many questions and concerns about getting the COVID-19 vaccine.
Heres the bottom line: Especially if you have an autoimmune condition like psoriatic arthritis, most rheumatologists and public health experts recommend you get vaccinated against COVID-19. In its COVID-19 Task Force Guidance, the National Psoriasis Foundation says that in most cases, patients with psoriatic disease who dont have contraindications should take the first authorized COVID-19 vaccine that becomes available to them.
Similarly, the American College of Rheumatology states that autoimmune and inflammatory rheumatic disease patients , which includes people with psoriatic arthritis, should receive the vaccine when theyre eligible.
The ACR also states that disease activity and severity should not delay you from getting the vaccine except in extreme cases . That said, vaccination would ideally take place in the setting of well-controlled disease.
Heres everything you need to know about getting the COVID-19 vaccine if you have psoriatic arthritis.
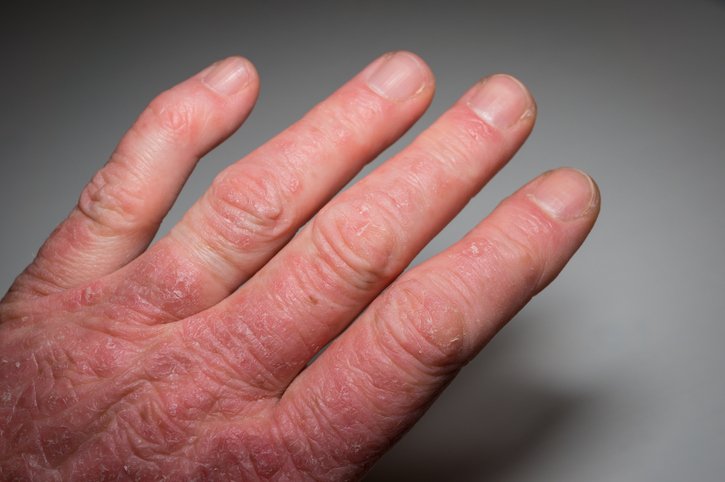
Swollen Fingers Or Toes
PsA may begin in smaller joints, such as those of the fingers or toes, and progress from there.
Spondylitis may be accompanied by dactylitis, or swelling of the toe or finger joints. This is sometimes called sausage fingers.
Dactylitis is estimated to affect up to 50 percent of patients with PsA, and is uncommon in other types of arthritis, except gout or pseudogout.
When caused by PsA, dactylitis may affect individual digits differently. For example, your left hand may be swollen while your right is not.
Unlike other types of arthritis, PsA tends to make your entire finger or toe appear swollen, rather than just the joint.
People with PsA may experience eye problems, such as inflammation and redness. Symptoms of eye inflammation include:
- red eyes
- dry eyes or feeling of grit or sand in the eyes
- difficulty focusing or blurred vision
- pain or sensitivity, especially to bright light
- floaters, or small specks, lines, or other shapes in your field of vision
If you develop new or large floaters along with flashing lights in your field of vision, it may be a sign of a medical emergency. Seek immediate treatment from a qualified medical professional.
You may also experience uveitis, or inflammation of the middle layer of the eye called the uvea. Between 7 and 25 percent of people with PsA develop uveitis.
Symptoms of uveitis include:
Read Also: Rheumatoid Arthritis Better With Movement
If You Have These Symptoms Heres Where To Get Professional Help
Just because you have one of these symptoms doesnt necessarily mean you have psoriatic arthritis. Tons of other things can cause fatigue, for example, like stress, anxiety disorders, and sleep apnea, which makes it difficult to use a list of symptoms alone to figure out if you have psoriatic arthritis. The only way to know for sure is to talk to a doctor and get a proper diagnosis as soon as possible if you need one. Remember: Psoriatic arthritis can lead to permanent joint damage without treatment, not to mention make a big impact on your daily life.
If someone has persistent joint pain or stiffness, especially if accompanied by joint swelling or tenderness, and even more so if its affecting more than one joint simultaneously, this should be brought to the attention of a physician. Most internists or family practitioners can do the preliminary evaluation to determine what condition may be responsible, says Dr. Rosenstein.
Your doctor may need to refer you to a rheumatologist, a dermatologist, or potentially both for diagnosis and treatment. If you realize in your search for care that you have access to a combined rheumatology-dermatology clinic, that can be a really excellent way to land on a treatment plan that collaborates between the two types of care, says Mikulik. The National Psoriasis Foundation can help you find specialist providers and prepare for your first appointment.
Related:
Q: How Often Do You Get Flares What Causes Them And How Do You Know One Is Coming
Donaldson: The longer you live with psoriatic arthritis, the more aware you become of your personal warning signals. For example, my PsA will often flare up in my ears and make very noticeable changes to my hearing. If I wake up and can barely hear anything, then I know Im headed for trouble. Other times, the weather will shift, and a flare will come out of nowhere. Sometimes it feels like danger lurks around every corner.
Cohen: The length of time between flare-ups ranges. It can strike randomly but is often a response to exertion, stress or what Ive eaten. If Ive eaten a lot of carbs and sugar at night, I pay a price in pain and stiffness the next morning and throughout the day.
I moved out of my home of 30 years last August as part of a divorce and into a new home with my college-age daughters. That was of course emotionally stressful but VERY hard work physically. It took me a couple of weeks to recover.
Pellegrin: PsA is always there. It can strike at any time and there usually is no warning. During the winter months it is more intense and the use of a heating pad in the morning or a pain patch is needed to help wake up the stiff joints. I use warm baths to relax.
You May Like: Does Arthritis Pain Come And Go