What Treatment Is Right For Me
The type of treatment will depend on how severe your symptoms are at the time of diagnosis with the goal being to control the disease to the point of remission and avoid complications. Medications may need to be changed over time to continue to maintain control and avoid disease progression and systemic effects. Some early indicators of more severe disease include onset at a young age, multiple joint involvement, and spinal involvement. Good control of the skin is important in the management of psoriatic arthritis. In many cases, you may be seen by two different types of healthcare providers, one in rheumatology and one in dermatology.
Early diagnosis and treatment can relieve pain and inflammation and help prevent progressive joint involvement and damage. Without treatment psoriatic arthritis can potentially be disabling, cause chronic pain, affect quality of life, and increase risk of heart disease. It is important to update your healthcare provider when you have a change in symptoms or if your medication regimen is no longer effective.
How Will Psoriatic Arthritis Affect Me
The effects of psoriatic arthritis can vary a great deal between different people. This makes it difficult to offer advice on what you should expect.
Psoriatic arthritis can cause long-term damage to joints, bones and other tissue in the body, especially if it isnt treated.
Starting the right treatment as soon as possible will give you the best chance of keeping your arthritis under control and minimise damage to your body allowing you to lead a full and active life with psoriatic arthritis.
You dont need to face arthritis alone. If you need support or advice, call our Helpline today on . Our advisors can give you expert information and advice about arthritis and can offer support whenever you need it most.
Joint Pain And Stiffness
Joint pain and stiffness is one of the hallmarks of psoriatic arthritis. It can affect one joint or multiple joints, anywhere in your body, from your knees to your fingers, toes, ankles, and lower back.
Its also one of the symptoms you should never ignore.
If you ignore signs of psoriatic arthritis, your joints can contract, meaning you cant move them, and this is permanent, says dermatologist Dr. Orit Markowitz. This is why it is very important to get treated if you notice any early signs of joint stiffness.
Read Also: How Can You Prevent Arthritis
Treatments For Your Skin
If your psoriasis is affecting your quality of life, or your treatment is not working, you may be referred to a dermatologist.
There are a number of treatment options for psoriasis.
Ointments, creams, and gels that can be applied to the skin include:
- ointments made from a medicine called dithranol
- steroid-based creams and lotions
- vitamin D-like ointments such ascalcipotriol and tacalcitol
- vitamin A-like gels such astazarotene
- salicylic acid
- tar-based ointments.
For more information about the benefits and disadvantages of any of these talk to your GP, dermatologist, or pharmacist.
If the creams and ointments dont help, your doctor may suggest light therapy, also known as phototherapy. This involves being exposed to short spells of strong ultraviolet light in hospital.
Once this treatment has started, youll need to have it regularly and stick to the appointments youve been given, for it to be successful. This treatment is not suitable for people at high risk of skin cancer or for children. For some people, this treatment can make their psoriasis worse.
Retinoid tablets, such as acitretin, are made from substances related to vitamin A. These can be useful if your psoriasis isnt responding to other treatments. However, they can cause dry skin and you may not be able to take them if you have diabetes.
Some DMARDs used for psoriatic arthritis will also help with psoriasis.
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else.
Psoriatic arthritis can be classed as a disability if it:
- makes daily tasks difficult
- lasts for more than 12 months.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Read Also: What Medication Is Used For Arthritis
What Causes Psoriasis And Psoriatic Arthritis
While no one knows the exact cause of psoriasis or PsA, experts believe that a faulty immune system is partly to blame. Specifically, the immune system attacks healthy skin cells and joints, causing the inflammation, swelling, and pain characteristic of psoriatic disease.
Genetics plays a part, too: Often will have other family members with psoriatic disease, says Dr. Haberman. In fact, roughly 40 percent of people with PsA have at least one close family member with psoriasis or psoriatic arthritis. Research is still ongoing, however, and its not clear whether having a family history of psoriasis alone increases PsA risk.
Obesity is also a common risk factor for people with psoriasis and PsA. According to a 2019 study in the journal Medicine, roughly 40 percent of people with psoriasis are obese. While it is unknown why obesity is so strongly linked to psoriatic diseases, we do know that obesity is associated with the production of inflammatory chemicals in the body, says Dr. Haberman. It may be that this underlying inflammatory environment helps predispose the body to the development of psoriasis and PsA, she says.
Other risk factors for psoriasis include:
- Family history
- Viral and bacterial infections
- Stress
- Obesity
- Smoking
- Alcohol consumption
Read more here about psoriatic arthritis risk factors.
Psoriasis Psoriatic Arthritis And Crohns Disease: Whats The Connection
Crohns disease and ulcerative colitis can be associated with psoriasis and psoriatic arthritis , which are comorbidities of CD and colitis. A comorbidity is when two or more disorders occur in the same person and cause adverse interactions.
CD and UC are the two main types of inflammatory bowel disease . CD is characterized by chronic inflammation in the lining and deeper layers of the digestive tract. UC causes sores and inflammation in the lining of the colon and rectum.
Psoriasis causes a proliferation of skin cells that become dry, itchy, and scaly with discolored patches of thickened skin . Skin can become infected during flares. Approximately 30 percent of people with psoriasis develop PsA, a type of inflammatory arthritis. Symptoms include joint pain, swollen and stiff joints, tendon pain, fatigue, and eye redness and pain .
For people with Crohns or colitis, the increased risk for psoriasis is approximately three times that of the general population.
MyCrohnsAndColitisTeam members have discussed their challenges with IBD, psoriasis, and PsA. Today, I meet with a dermatologist to discuss Stelara to treat both Crohn’s and psoriasis, one member wrote. The GI doctor gave me a prescription for prednisone to help, but I have severe osteoporosis, so before starting, I am trying to connect all medical providers to be on one page.
Recommended Reading: Where Does Psoriatic Arthritis Affect
Living With Psoriatic Arthritis
There is no cure for psoriatic arthritis. But you can reduce your symptoms by stickingto your treatment plan. Manage pain with medicine, acupuncture, and meditation. Getenough exercise. Good exercises include yoga, swimming, walking, and bicycling. Workwith a physical or occupational therapist. He or she can suggest devices to help you withyour daily tasks.
Diagnosing Psoriasis And Psa
Unfortunately, theres no one simple diagnostic test to check for psoriasis or psoriatic arthritis. This means your doctor will need to make a clinical diagnosis, which requires taking into account your symptoms, risk factors, as well as the results of bloodwork and X-rays or other imaging scans to assess any joint involvement.
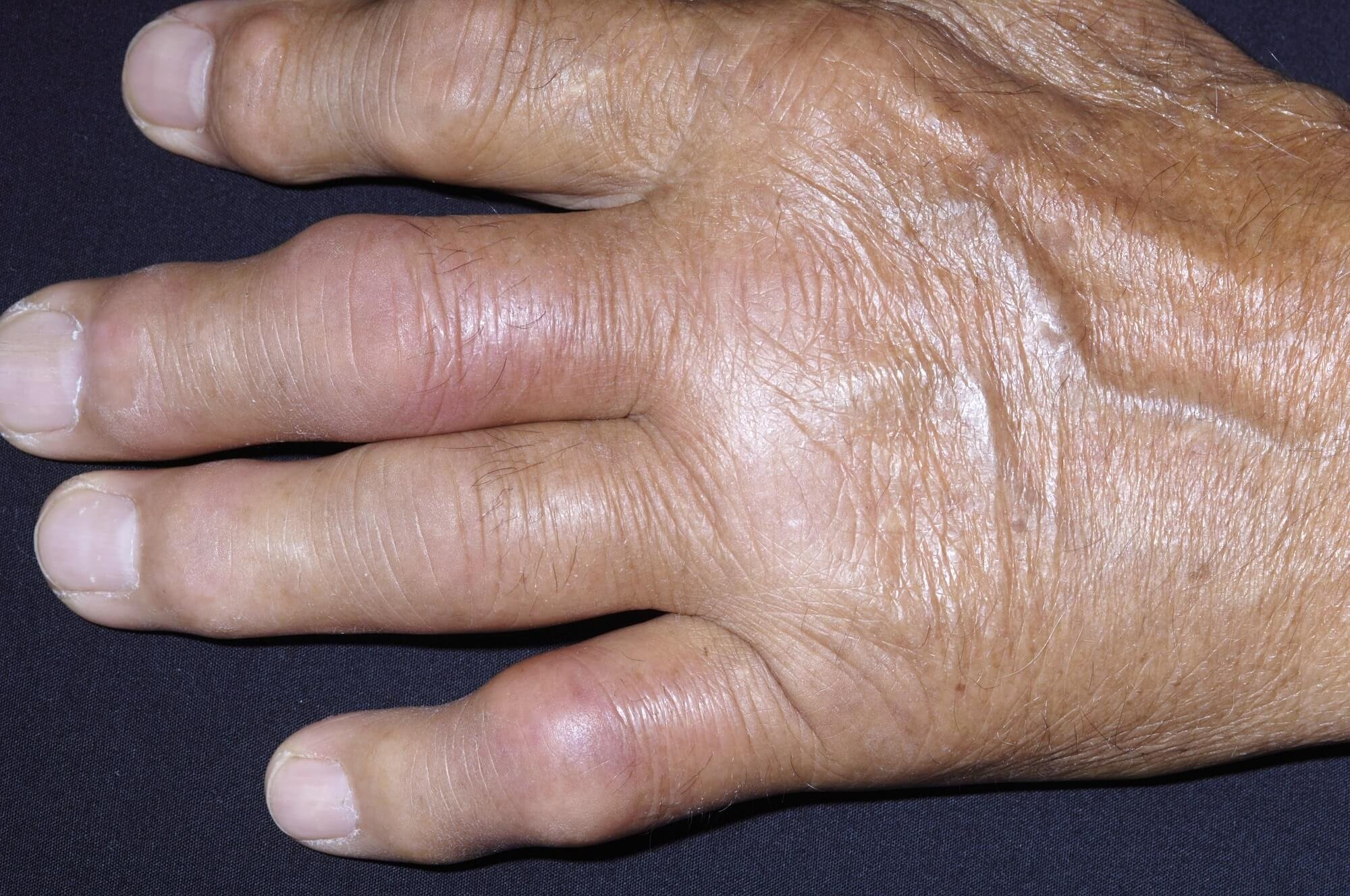
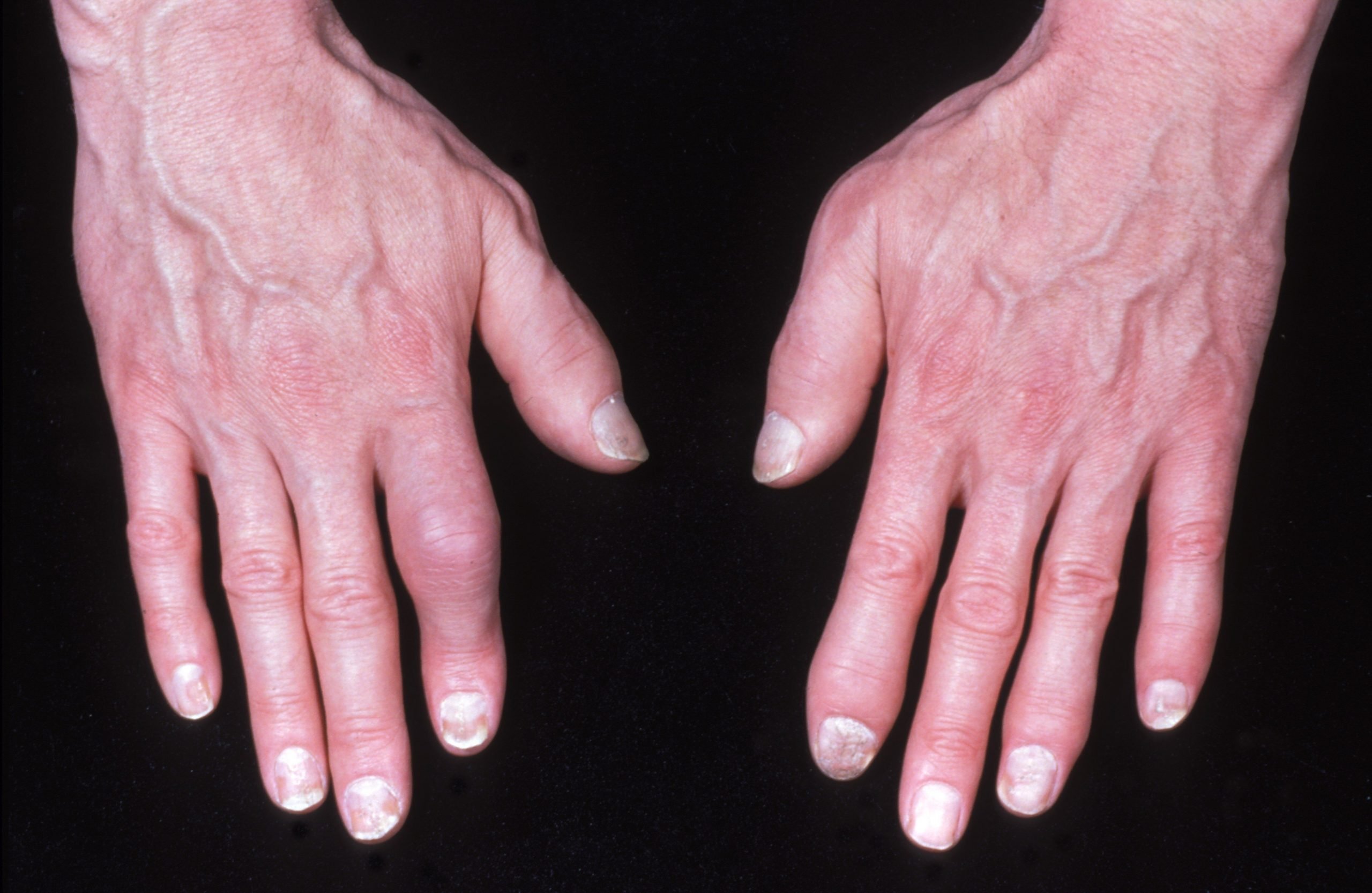
During the physical exam, your doctor might look for signs of psoriasis on the elbows and knees as well as less visible places like the scalp, belly button, intergluteal cleft, palms of hands, and soles of feet. Theyll also check for any fingernail or toenail abnormalities, like pitting or ridging, as well as swollen fingers or toes .
The presence of dactylitis and finger and toenail changes are evidence of psoriasis that can be used to aid in the diagnosis of psoriatic arthritis if there is no evidence of skin disease, says Dr. Haberman.
Here are some common steps used to diagnose psoriasis and PsA:
- A medical exam to discuss family history, risk factors, and symptoms
- Blood tests to check for markers of inflammation and antibodies , which can help rule out other types of arthritis, including rheumatoid arthritis
- Imaging tests to detect any joint damage, dislocation of small or large joints, disfiguration , new bone formation, and inflammation in the enthesis
- Skin biopsy of a skin plaque, if you have previously undiagnosed psoriasis
You May Like: What To Take For Arthritis In Hands
Consider Natural Supplements And Spices
Omega-3 fatty acids have anti-inflammatory properties. These healthy fats, found in many supplements, reduce inflammation and stiffness in joints.
While research suggests there are health benefits, the Food and Drug Administration doesnt monitor the purity or quality of supplements. Its important to talk with your doctor before you begin taking supplements.
Turmeric, a potent spice, also serves up a dose of anti-inflammatory properties and may help reduce inflammation and PsA flare-ups. Turmeric can be added to any dish. Some people even stir it into tea or lattes, like golden milk.
Early Warning Signs You Have Psoriatic Arthritis
Autoimmune disorders can be difficult to diagnose, especially in the earlier stages, and psoriatic arthritis is no different. Because there is no definitive blood test that can identify this form of arthritis and the similarities in symptoms it shares with rheumatoid arthritis, diagnosing can be tricky.
Research suggests that more than half of people with psoriatic arthritis must wait at least two years for a diagnosis, so it can be helpful to recognize the symptoms early on. Keep reading to learn about the early signs of psoriatic arthritis and how to find someone who can help provide you some relief.
Also Check: Does Epsom Salt Help Arthritis
What Can An Mri Detect
MRI can detect a variety of conditions of the brain such as cysts, tumors, bleeding, swelling, developmental and structural abnormalities, infections, inflammatory conditions, or problems with the blood vessels. It can determine if a shunt is working and detect damage to the brain caused by an injury or a stroke.
How Is Psoriatic Arthritis Diagnosed
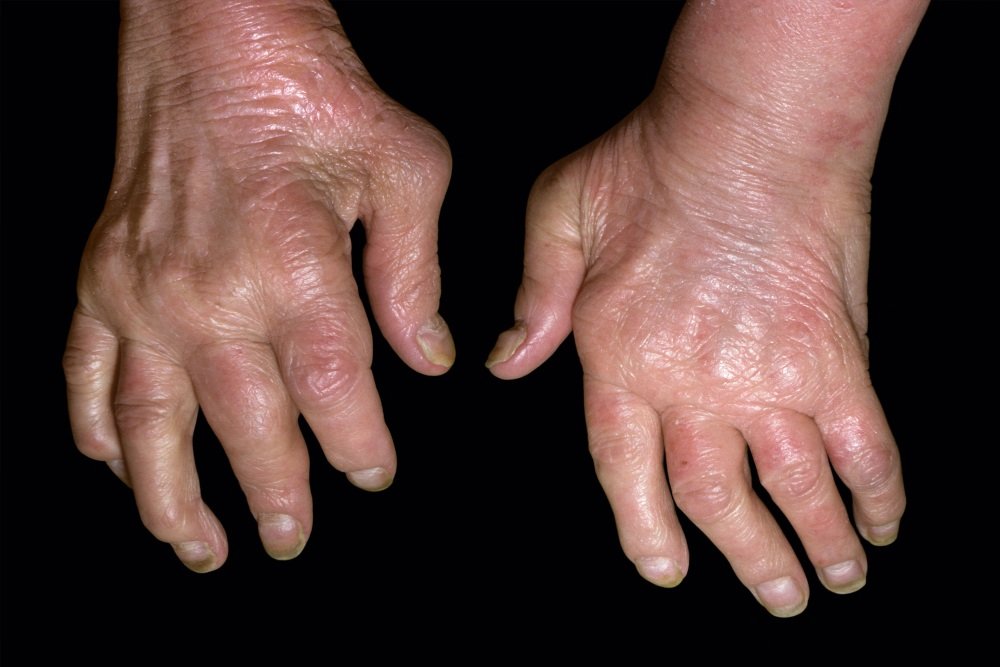
Psoriatic arthritis is easier to confirm if you already have psoriasis. If you donthave the skin symptoms, diagnosis is more difficult. The process starts with a healthhistory and a physical exam. Your healthcare provider will ask about your symptoms. Youmay have blood tests to check the following:
- Erythrocyte sedimentation rate . This test looks at how quickly red blood cells fall to the bottom of a test tube. When swelling and inflammation are present, the bloods proteins clump together and become heavier than normal. They fall and settle faster at the bottom of the test tube. The faster the blood cells fall, the more severe the inflammation.
- Uric acid. High blood uric acid levels can be seen in psoriatic arthritis but are not used for diagnosis or monitoring.
- Imaging. X-rays, CT scans, ultrasound, MRI, and skin biopsies may all be used to help diagnosis.
You May Like: How To Help Arthritis In Ankle
What Tests Will I Be Required To Take During My Diagnosis And Treatments
A full case history will be taken, urine and blood tests requested, x-rays, sometimes specialist x-rays, images and scans may also be requested, plus a full examination of your affected parts i.e. back, hands, feet etc.
In summary points to remember when seeing your doctor:
Ask about your medicines:
Psa Symptoms: What Are The First Signs Of Psoriatic Arthritis
Jump to:What is Psoriatic Arthritis?SymptomsNext Steps
Arthritis, by definition, is characterized by the breakdown of the cartilage within the joints. If you are suffering from any type of arthritis, this is the general cause of the pain and stiffness in your joints. With over 100 types of arthritis, the top three most common are osteoarthritis, rheumatoid arthritis, and psoriatic arthritis. In this article, we will discuss the third most common type of arthritis: psoriatic arthritis .
Also Check: What Drugs Are Used For Rheumatoid Arthritis
Up To 30 Percent Of People With Psoriasis Will Go On To Develop Psa And 85 Percent Of People With Psa Also Have Skin Psoriasis
Writing and reporting by Susan Jara and Steven Newmark
Psoriasis and psoriatic arthritis are distinct conditions, but they are connected. In fact, data show that up to 30 percent of people with psoriasis will go on to develop PsA and 85 percent of people with PsA also have skin psoriasis.
Although people can be diagnosed with PsA without having any skin involvement, most often they will have a family member with skin psoriasis, says Rebecca Haberman, MD, a rheumatologist at NYU Langone Health in New York City.
Psoriasis is an inflammatory condition of the skin, while psoriatic arthritis also includes inflammation of the joints and entheses , .
Read on to find out the different symptoms of psoriasis vs. PsA, how they are diagnosed and treated, and what you need know about the link between these health conditions.
Psoriasis Presentation And Diagnosis
Genetic predisposition and certain environmental factors are known to trigger psoriasis, which can present in many forms.4 Chronic plaque psoriasis, or psoriasis vulgaris, is the most common skin pattern with a classic presentation of sharply demarcated erythematous plaques with overlying silver scale.4 It affects the scalp, lower back, umbilicus, genitals, and extensor surfaces of the elbows and knees. Guttate psoriasis is recognized by its multiple small papules and plaques in a droplike pattern. Pustular psoriasis usually presents with widespread pustules. On the other hand, erythrodermic psoriasis manifests as diffuse erythema involving multiple skin areas.4 Erythematous psoriatic plaques, which are predominantly in the intertriginous areas or skin folds , are known as inverse psoriasis.
A psoriasis diagnosis is made by taking a history and a physical examination. Rarely, a skin biopsy of the lesions will be required for an atypical presentation. The course of the disease is unpredictable, variable, and dependent on the type of psoriasis. Psoriasis vulgaris is a chronic condition, whereas guttate psoriasis is often self-limited.4 A poorer prognosis is seen in patients with erythrodermic and generalized pustular psoriasis.4
Also Check: How To Ease Arthritis Pain In Fingers
Psoriasis And Psoriatic Arthritis Overview
Alan Menter, MDSupplements and Featured Publications
Psoriasis and psoriatic arthritis are chronic immune-mediated diseases that primarily affect the skin and joints, respectively these diseases are also associated with high rates of cardiovascular and other comorbidities. Despite over 40 genes proven to be related to the disease, the exact causes of psoriasis and PsA are still to be determined. Recent insights into the underlying pathophysiology of these diseases have revealed novel therapeutic targets. Effective management requires timely diagnosis and initiation of treatment. Yet, both psoriasis and PsA remain underrecognized and undertreated in current clinical practice. Recognizing the true physical, social, and emotional burden of psoriasis and PsA, as well as their associated comorbidities, is the first step to improving the prognosis for affected patients.
Am J Manag Care. 2016 22:S216-S224
PSORIASIS OVERVIEW
Psoriasis is a chronic, multifactorial, immune-mediated skin disease. The characteristic erythematous plaques of psoriasis are often painful and disfiguring, leading to a substantial decrease in quality of life.1 Cardiovascular disease , diabetes, and other autoimmune disorders are common among patients with psoriasis, contributing to the overall burden of disease and increasing healthcare
resource utilization.1
Epidemiology
Immunologic Mechanisms
Genetics of Psoriasis
Environmental triggers
Other immune-mediated diseases
Disease Classification
Mild
Who Gets Psoriatic Arthritis
Anyone can get psoriatic arthritis, but it is most common in adults, affecting men and women equally.
Most people who get it already have psoriasis. Psoriatic arthritis usually develops about 7 to 10 years after skin symptoms begin. You may be more likely to get psoriatic arthritis if you:
- Are obese.
- Experience stress, joint or bone injuries, or infection.
You May Like: Is Coconut Water Good For Arthritis
When Do Psoriatic Arthritis Symptoms Appear
Symptoms of psoriatic arthritis typically appear in people between the ages of 30 and 50. They may arise gradually or suddenly, or flare up periodically. PsA may also affect one or more joints most commonly in the hand, foot, or knee and worsen over time.
PsA typically develops about 10 to 20 years after the onset of psoriasis, but PsA can present even before skin symptoms appear. Most people are first examined by a dermatologist or internist to identify PsA symptoms, before being referred to a rheumatologist, who specializes in arthritis.
Talk With Others Who Understand
On MyCrohnsAndColitisTeam, the social network for people with Crohns or colitis, more than 150,000 members come together to ask questions, give advice, and share their stories with others who understand life with Crohns and colitis.
Are you living with Crohns or colitis and have questions about psoriasis and psoriatic arthritis? Share your experience in the comments below, or start a conversation by posting on your Activities page.
You May Like: What Can I Use For Arthritis