What Happens If You Dont Treat Your Psoriatic Arthritis
While some people may have fairly mild disease, others can have serious problems all over their body. PsA is a systemic disease. That means inflammation can affect you all over, and strike different joints or organs.
Your heart health could also be at serious risk if you dont get PsA in inflammation under control. Its not just your skin and joints that are affected. There is a much higher risk of cardiovascular problems among people with PsA. So get treated, and make sure you get regular check-ups to be aware of any health problems like signs of heart disease.
If you dont treat your PsA, theres a chance you could have joint pain and damage. In some people, this could impact your ability to work, do day-to-day tasks around the house, or enjoy physical activities you love. So see your doctor as soon as possible and stick with your treatment plan.
If you have trouble affording your care or treatments, we have tips that may help you here in this guide, and you can also talk to your doctors office to find help.
What Are Some Of The Symptoms Of Psoriatic Arthritis
Many people feel pain and stiffness in their joints, especially in the morning. The pain is often only in a joint on one side of your body and not in the same joint on the other side of your body. But there are also cases where the joints on either side of your body hurt. People may have entire fingers or toes that swell, which gives them a sausage-like appearance. There are also skin symptoms. People often get lesions . Usually, skin symptoms start first and joint pain begins later.
Papers Of Particular Interest Published Recently Have Been Highlighted As: Of Importance Of Major Importance
Moll JMH, Wright V. Psoriatic arthritis. Seminars Athritis Rheum. 1973 3:5578.
Feld J, Chandran V, Haroon N, Inman R, Gladman D. Axial disease in psoriatic arthritis and ankylosing spondylitis: a critical comparison. Nat Rev Rheumatol. 2018 14:36371 This is a critical review of the literature addressing the question whether axial disease in psoriatic arthritis is different from that of ankylosing spondylitis and highlights some clinical, imaging, genetic, and therapeutic differences.
Feld J, Ye JY, Chandran V, et al. Is axial psoriatic arthritis distinct from ankylosing spondylitis with and without concomitant psoriasis? Rheumatology . 2020 59:13406 This study was triggered by the literature review noted above which identified cross-sectional studies but no longitudinal studies comparing the axial disease in PsA to that of AS with or without psoriasis. Patients with AS and PsA were followed by the same protocol in a single centre. Axial PsA was clearly different from AS with or without psoriasis suggesting that it is a distinct entity.
Yap KS, Ye JY, Li S, et al. Back pain in psoriatic arthritis: defining prevalence, characteristics and performance of inflammatory back pain criteria in psoriatic arthritis. Ann Rheum Dis. 2018 77:15737 This study demonstrated that the definition of inflammatory back pain developed for ankylosing spondylitis may not be appropriate for patients with PsA.
You May Like: Side Effects Of Arthritis
Can Psoriatic Arthritis Make You Gain Weight
When someone has PsA, painful joints can make it difficult to exercise.This can lead to weight gain, which in turn puts extra pressure on the joints, making symptoms worse. Studies have shown that people living with PsA who are overweight have more severe symptoms and find it more difficult to control their condition.
Is psoriasis inherited? Psoriasis is an autoimmune disorder that can run in families. Your skin cells grow too quickly and pile up into bumps and thick scaly patches called plaques. Youre more likely to get psoriasis if your blood relatives also have it. Thats because certain genes play a role in who gets the condition.
Can psoriasis cause fatigue? Fatigue may be an early symptom or sign of inflammatory activity in people who may have psoriasis and or psoriatic arthritis both are classed as long-term inflammatory conditions. Inflammation is linked with the release of powerful chemicals.
Would psoriatic arthritis show up in a blood test?
No single thing will diagnose psoriatic arthritis, but blood tests, imaging, and other tests can help your doctor. They may want to give you certain tests that check for rheumatoid arthritis, because it can look a lot like psoriatic arthritis.
Fulfilment Of Caspar Mny And Asas Criteria
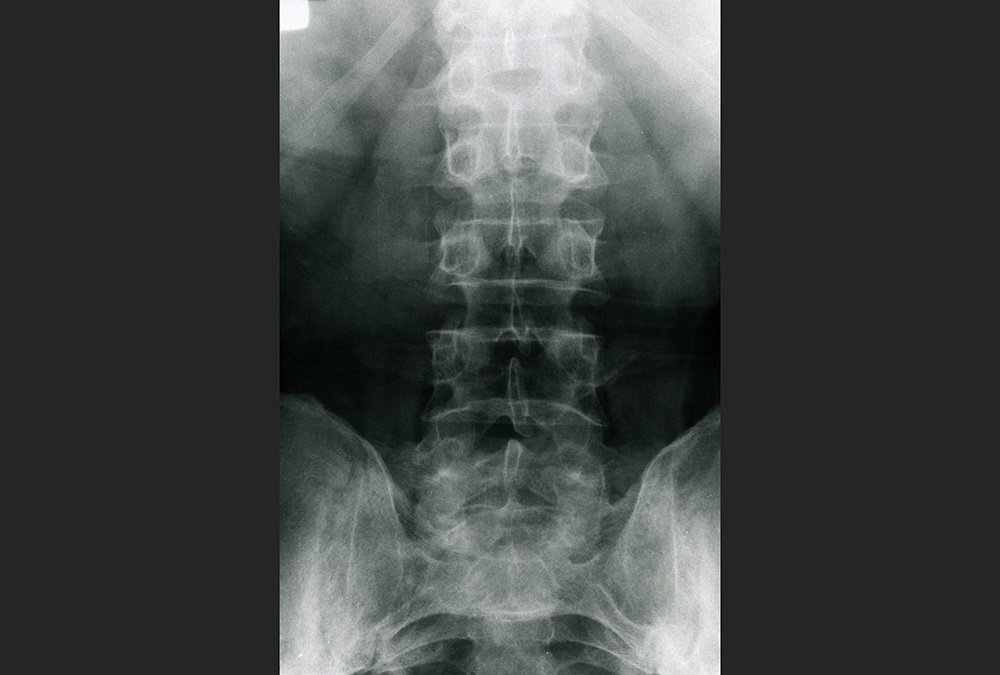
Forty-eight of 201 participants with PsA attending the PsA clinic also fulfilled mNY criteria for AS. Forty-nine of 201 participants with AS attending the AS clinic also fulfilled CASPAR criteria for PsA. Although a lack of MRI data prevented us from fully applying the ASAS classification for axial SpA across our cohort, we did find that 157/157 of AS cases, 85/118 of PsSpA cases and 9/127 of pPsA cases fulfilled ASAS criteria for axial SpA by either or both clinical-only or radiographic imaging streams.
You May Like: Ra In Hand Symptoms
Axial Psoriatic Arthritis: Correlation Between Whole Spine Mri Abnormalities And Clinical Findings
Pamela Diaz1, Iris Eshed2, Joy Feld3 and Lihi Eder1, 1University of Toronto, Toronto, ON, Canada, 2Sheba Medical Center, Ramat Gan, Israel, 3Carmel and Zvulun Medical Centre, Haifa, Israel
Session Type: Abstract Session
Session Time: 2:30PM-2:45PM
Background/Purpose: Psoriatic Arthritis typically affects peripheral joints, but in some patients the disease can involve the spine. While magnetic resonance imaging is an important diagnostic tool for spondyloarthritis, especially in early phases, there is minimal information about MRI features of axial PsA.The purpose of the study was to describe the prevalence of inflammatory and structural lesions by whole-spine MRI in patients with psoriatic disease, and assess the correlation of MRI-defined spondyloarthritis with clinical and laboratory features and with classification criteria for axial spondyloarthritis .
The overall prevalence of axial inflammatory and structural spondylitis by whole-spine MRI was low despite the high prevalence of axial symptoms. Poor correlation was found between imaging and clinical findings highlighting the need for further research of the underlying mechanisms of axial involvement in PsA.
* Inflammatory back pain according to rheumatologist impression at the clinical visit 1. Rudwaleit M, et al. Arthritis Rheum. 2006 54:569-78. 2. Sieper J, et al. Ann Rheum Dis. 2009 68:784-8.
Disclosures: P. DiazI. EshedJ. FeldL. Eder
To cite this abstract in AMA style:
Arthritis Rheumatol.
Spondyloarthritis Two Other Conditions
Two other conditions fall under spondyloarthritis. The first is enthesitis-related arthritis , which is a type of juvenile idiopathic arthritis. Juvenile means beginning before age 16. JIA-ERA was known as juvenile spondyloarthritis .
The second is undifferentiated spondyloarthritis. Undifferentiated spondyloarthritis describes someone with all the features of spondyloarthritis but without the confirming characteristics.
Although spondyloarthritis is form of inflammatory arthritis, it differs from rheumatoid arthritis because people with SpA do not have rheumatoid factor antibodies in their blood. They are seronegative whereas people with RA are seropositive.
Also Check: How To Prevent Arthritis In Fingers
Predominately In White Western European Population
The HLA-B27 gene is found in about 7% of the white western European population with higher and lower rates in other ethnic groups. It tends to be higher in far northern groups such as Inuit and Samis and in certain North American tribes on the Pacific coast and lower in African populations. It is non-existent in Australian Aboriginal populations.
Sociodemographic Treatment Laboratory And Genetic Characteristics
PsSpA, pPsA and AS cases were broadly similar in terms of age, disease duration, treatment and other sociodemographic characteristics . Any differences were adjusted for in the multivariable models. HLA-B*27 alleles were present in 9/127 pPsA, 47/118 PsSpA and 140/157 AS cases . Compared with PsSpA cases, the presence of HLA-B*27 was significantly more likely in AS and significantly less likely in pPsA .
Axial radiographic pattern and morphology in PsSpA and AS cases
Of 118 cases classified as PsSpA: 45/118 had sacroiliitis with spondylitis, 39/118 had spondylitis alone and 34/118 had sacroiliitis alone. The majority of PsSpA cases with spondylitis alone were symptomatic although were less likely to be symptomatic than PsSpA cases with sacroiliitis with or without spondylitis . Thoracic spine radiographs, MRI and CT scans were available on 32/39 PsSpA cases with spondylitis alone, and none demonstrated diffuse idiopathic hyperostosis , defined as per the criteria of Resnick.
Correlation of radiographic pattern with HLA-B*27 status in PsSpA cases
HLA-B*27 was present in 6/39 of PsSpA cases with spondylitis alone, 11/34 of cases with sacroiliitis alone and 30/45 of cases with both sacroiliitis and spondylitis. Logistic regression demonstrated a significantly increased probability for the presence of HLA-B*27 in PsSpA cases with both sacroiliitis and spondylitis, compared with spondylitis alone .
Axial radiographic morphology
Axial radiographic severity
You May Like: What Does Rheumatoid Arthritis Feel Like In Hands
What Is The Most Important Information I Should Know About Enbrel
ENBREL is a medicine that affects your immune
ENBREL is a medicine that affects your immune system. ENBREL can lower the ability of your immune system to fight infections. Serious infections have happened in patients taking ENBREL. These infections include tuberculosis and infections caused by viruses, fungi, or bacteria that have
What Causes Spondyloarthritis
We dont know what causes spondyloarthritis, but we do know that there is a genetic factor. About 90% of people with spondyloarthritis carry the HLA-B27 gene, a gene that is found in about 7% of the white western European population. The involvement of this gene has been known since 1973 but there is no defining mechanism known by which B27 causes SpA.
Confusingly, the other 10% of people with SpA do not have the HLA-B27 gene, so there must be other factors at play. Researchers have now identified at least twenty genes that have been linked to SpA but their role is not well understood. It is known that the genes ERAP 1 and 2 are closely related to B27, and it may be that it is the interaction of these genes with B27 that causes the disease. It is also known that another gene, that codes for the receptor of IL-23 is involved.
A great deal of genetic research is going on worldwide to identify the genes associated with SpA and the susceptibility of someone, with these genes, developing disease.
Also Check: What Relieves Arthritis Pain
What Is Psoriatic Arthritis
PsA is a lifelong condition that causes your joints to hurt and swell.People with psoriatic arthritis can also have patches of red, thick skin with silvery scales. About 1 million American adults have it.
PsA is a lifelong condition that causes your joints to hurt and swell. People with psoriatic arthritis can also have patches of red, thick skin with silvery scales. About 1 million American adults have it.
- Overview
Take a few minutes to learn more about psoriatic arthritis.
Unveiling Axial Involvement In Psoriatic Arthritis

- Seminars in Arthritis and Rheumatism
You’ve saved your first item
You can find your saved items on your dashboard, in the “saved” tab.
You’ve recommended your first item
Your recommendations help us improve our content suggestions for you and other PracticeUpdate members.
You’ve subscribed to your first topic alert
What does that mean?
Don’t Miss: Rheumatoid Arthritis Arm Pain
Axial Vs Peripheral Spondyloarthritis
More recently, clinicians have started dividing spondyloarthropathies into axial spondyloarthritis and peripheral spondyloarthritis.
In axial spondyloarthritis, the arthritis symptoms affect the axial jointsthe joints of the spine, chest, and the sacroiliac joint .
In peripheral spondyloarthritis, people usually dont have symptoms affecting these joints. Instead, they might have symptoms that affect the other joints, such as the knees or finger or toe joints.
However, it isnt always that clear cut. Some people with axial spondyloarthritis have problems with one or more of their peripheral joints as well.
Regardless of type, diagnosis of all spondyloarthropathies requires a physical exam, a conversation about your symptoms, and usually imaging and lab tests. There is also quite a bit of overlap in terms of the ways these different forms of spondyloarthropathy are treated.
How Are Axial Spondyloarthritis And Ankylosing Spondylitis Related
When learning about spondyloarthritis, it’s easy to get confused about terminology and categories. The terminology is particularly confusing because doctors have been changing the way these conditions are categorized over recent years, and not even medical professionals always use the terms consistently. But, there are some general things you can learn to help you keep the categories straight and to better understand them.
Spondyloarthritis refers to a family of inflammatory rheumatological conditions that can affect the joints, including the joints of the spine, as well as other bodily systems.
Axial spondyloarthritis can be considered a subset of spondyloarthritis that affects primarily the axial joints .
Ankylosing spondylitis is generally considered a specific subset of axial spondyloarthritis.
You May Like: Relief For Rheumatoid Arthritis In Hands
Whats Going On Inside Your Body
Your immune system is designed to help protect your body from many harmful things. But when your immune system doesnt work right, it can make you sick. When you have psoriatic arthritis, cells from your immune system move into your joints and skin. These cells make several proteins that can cause swelling and pain. One of these proteins is called tumor necrosis factor, or TNF. Too much TNF may lead to inflammation. Inflammation is what causes the pain, swelling, and damage of your joints over time. Too much TNF may also make skin cells grow too quickly, forming plaques that you see on your skin.
Does Voltaren Help Psoriatic Arthritis
One percent voltaren gel, a new drug manufactured by Ciba-Geigy , Switzerland, was used in the treatment of 57 patients with psoriasis in the progressive stage and psoriatic arthritis symptoms. The drug is characterized by antiinflammatory, analgesic, and antipyretic effects.
Does caffeine make psoriatic arthritis worse? People with PsA should avoid drinks that are high in sugar. This means soft drinks, juices, energy drinks, mixed coffee drinks, and other beverages that contain added sugars. High sugar intake can contribute to increased inflammation and weight gain, which can exacerbate PsA symptoms.
What foods affect psoriatic arthritis?
Foods like fatty red meats, dairy, refined sugars, processed foods, and possibly vegetables like potatoes, tomatoes, and eggplants may all cause inflammation. Avoid them and choose fish, like mackerel, tuna, and salmon, which have omega-3 fatty acids.
Read Also: Autoimmune Leg Pain
European League Against Rheumatism
-
In patients with predominantly axial disease that is active and has insufficient response to NSAIDs, therapy with a bDMARD should be considered, which according to current practice is a tumor necrosis factor inhibitor
-
Given the lack of data for secukinumab in patients with PsA with axial involvement, TNFis are the first choice of a biologic disease-modifying anti-rheumatic drug in these patients. There are sufficient published data on efficacy of secukinumab in patients with axial disease associated to PsA
Reviewed by Sarah A. Fantus, MD
Is Your Psoriatic Arthritis Getting Worse
Psoriatic arthritis can get worse quickly. If your joints hurt, it could mean your joints are being damaged. However, joint damage can also continue to occur even when pain is controlled. That damage cant be undone. Thats why its important to talk to your doctor and find the best way to manage your condition.
Read Also: Joint Pain Medical Term
Axial Involvement In Psa Linked To Greater Risk For Moderate Severe Psoriasis
We were unable to process your request. Please try again later. If you continue to have this issue please contact .Philip J. Mease
Axial involvement in psoriatic arthritis is associated with a greater risk for moderate-to-severe psoriasis, with higher disease activity and a more pronounced impact on the patients quality of life, according to findings published in the Journal of Rheumatology.
The characteristics of psoriatic arthritis patients with and without axial spondyloarthritis have not been well characterized,Philip J. Mease, MD, of the University of Washington, told Healio Rheumatology. In previously published series, SpA, defined by features such as sacroiliitis and inflammatory spine lesions seen on MRI and inflammatory back pain clinical features, occurs in up to 40% of PsA patients. In 1,530 PsA patients in the Corrona registry, 12.5% were classified as having spondylitis based on investigator evaluation and/or imaging of the spine and sacroiliac joints.
Axial involvement was defined as physician-reported presence of spinal involvement at enrollment, or radiograph or MRI showing sacroiliitis. Both groups of patients were similar in sex, race, BMI, disease duration, presence of dactylitis and prevalence of most comorbidities. Mease and colleagues analyzed patient data on demographics, clinical measures, patient-reported outcomes and treatment.
An Update For Rheumatologists On The Diagnosis And Management Of Axial Psoriatic Arthritis
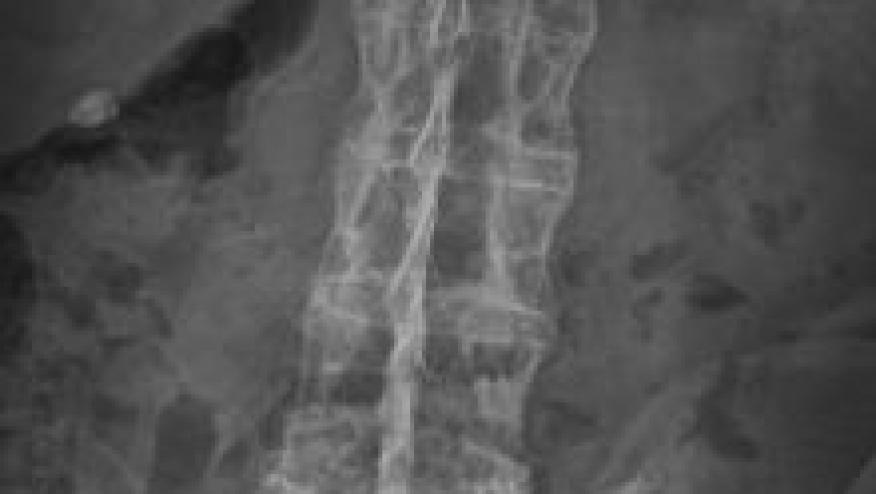
Psoriatic arthritis is a heterogeneous, chronic, progressive, inflammatory condition associated with enthesitis, dactylitis, and skin and nail psoriasis that can affect peripheral joints. However, axial involvement may also occur in PsA.1
In a recent review published in Seminars in Arthritis and Rheumatism, Poddubnyy and colleagues provided an overview on the clinical presentation, diagnosis, and treatment of axial PsA to improve rheumatologists knowledge of this phenotype.1
Risk Factors for Axial Involvement in PsA
Reported data of axial involvement in PsA are variable, with approximately 25% to 70% of patients with PsA experiencing axial involvement of their disease.1 The variability was found to be related to the various definitions of axial involvement in PsA definitions can range from isolated unilateral sacroiliitis to criteria similar to those used for ankylosing spondylitis.1,2 Less than 5% of patients with PsA have axial disease alone the majority of patients with axial PsA also have peripheral arthritis.2,3
Axial involvement in patients with PsA typically develops at a later stage in the disease course. Prevalence of axial disease increases with disease duration, with studies suggesting that up to 70% of patients with long-standing PsA may have axial involvement, compared with up to 28% of patients with early-stage PsA.4
Clinical Presentation Differential Diagnosis of Axial PsA
What Are the Treatment Goals and Options for Axial PsA?
References
Read Also: Bee Pollen For Arthritis