How Do You Treat Psoriatic Arthritis Symptoms In The Hands And Feet
Treatment of PsA symptoms in the hands and feet is the same as treatment for PsA in general. Medications called immunosuppressants treat the cause of inflammation in the hands and feet: an overactive immune system that is attacking the skin, joints, and tendons.
The goal is to find a medication regimen that clears your skin and improves joint pain and swelling, everywhere youre affected. It can take some time to find the medication or medications that work for you, but there is a regimen out there that can do both!
During a PsA flare , anti-inflammatory medications like steroids or non-steroidal anti-inflammatory drugs can quiet down symptoms in a short amount of time. A quick course of anti-inflammatories may be particularly helpful for dactylitis and enthesitis.
While its rare, steroid injections near tendons and joints may be performed, too. Steroid shots are typically a last resort since there are potential side effects.
Left untreated, PsA can cause complications, including permanent joint damage. This can cause deformities in the hands and feet and difficulty performing daily activities. So starting treatment early is important. It might feel overwhelming, but talk to your provider about treatment options. You can work together to find a regimen that you feel comfortable with.
Distal Interphalangeal Predominant Psoriatic Arthritis
Distal interphalangeal psoriatic arthritis may sound complicated, but it simply means that the distal joints of the phalanx are affected.
This type of psoriatic arthritis is characterized by pain and stiffness near the tips of the fingers or toes. When viewed on an X-ray, the ends of the bones often narrow like the tip of a pencil, while the adjacent joints take on a compressed, cup-like appearance.
Nail changes, including pitting, thickening, and lifting are also common.
Psoriasis / Psoriatic Arthritis
Psoriasis is a painful skin-related auto-immune disease that affects various body parts, including the feet. Psoriasis causes excessive skin cell build-up, which accumulates and leads to red, bumpy, scaly, itchy patches .
Psoriasis can be debilitating and cause throbbing soreness when its particularly bad, making it difficult to enjoy life. Sometimes, its effects can come and go. That said, it is a chronic disease and treatment is always the best course of action to help soothe sudden, severe flare-ups.
There is also a chronic inflammatory arthritis that causes both joint pain and psoriasis symptoms, called psoriatic arthritis. Psoriatic arthritis causes swelling in the toes, warm joints, and thickening or detachment of the toenails.
Don’t Miss: What Can Be Done For Arthritis In The Back
How Does Psoriatic Arthritis Affect Your Feet
Psoriatic arthritis can also cause painful inflammation in the feet. You may feel it in the joints of your toes or ankles. Similar to your fingers, psoriatic arthritis can cause swelling of your entire toe and changes in your toenails.
Enthesitis, which is inflammation where your tendons and ligaments attach to bone, can develop with psoriatic arthritis. This may occur in the bottom of your foot as the result of plantar fasciitis or in your heel due to Achilles tendonitis. Pain is often worst when you first wake up in the morning or after periods of inactivity.
Other symptoms of psoriatic arthritis in your feet include:
Diagnosing Psoriatic Arthritis In The Feet
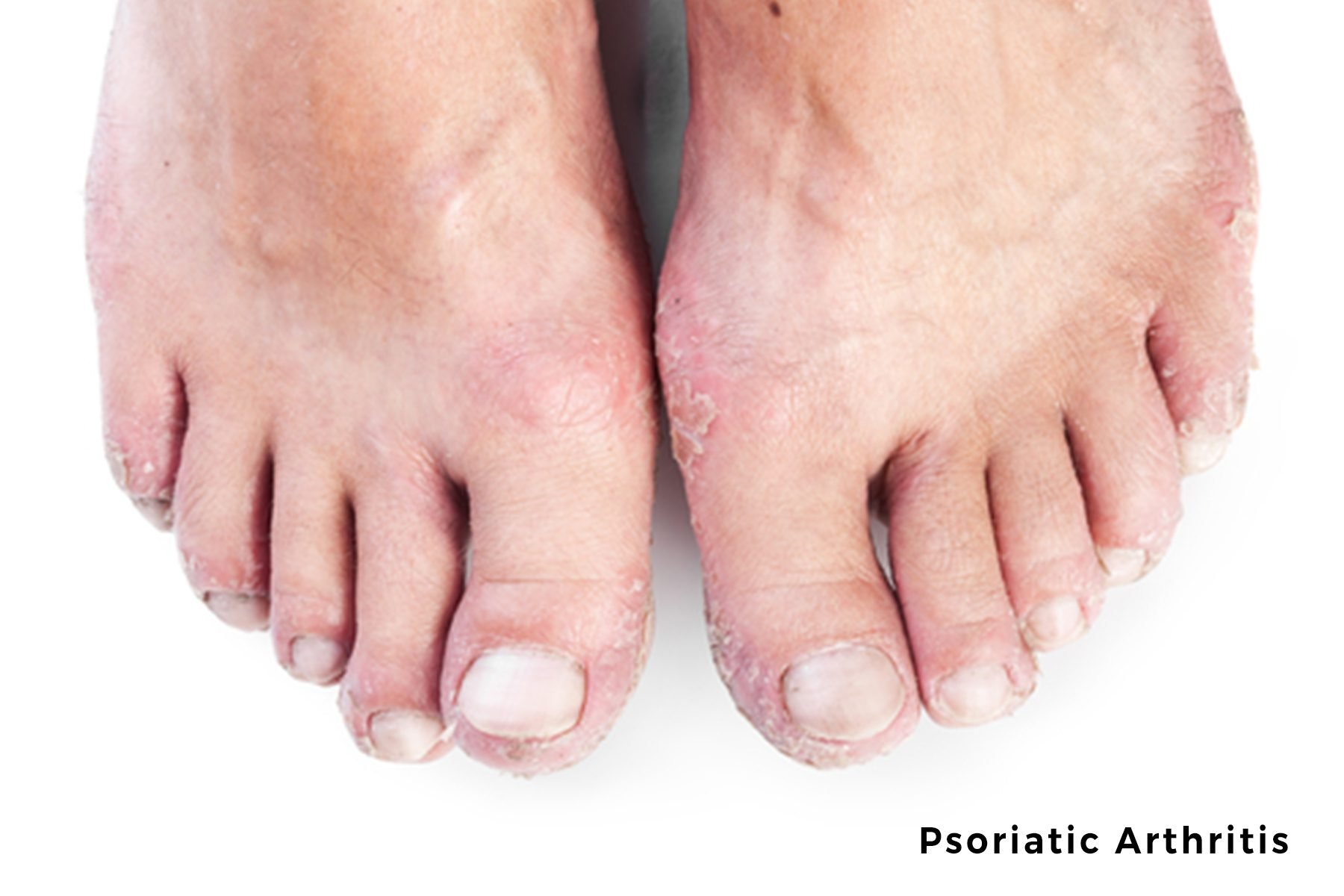
Because theres no definitive test for psoriatic arthritis in the feet and symptoms are similar to other forms of inflammatory arthritis some members of MyPsoriasisTeam go months, even years, before receiving a correct diagnosis. My feet are my worst part, with so much pain in one deformed foot, said one member who waited more than a year to get a diagnosis. A 2018 study found about 30 percent of people with psoriatic arthritis waited more than five years for a diagnosis after symptom onset.
In my experience PsA can be difficult to diagnose unless you have all the standard symptoms, pointed out one MyPsoriasisTeam member. I was told if blood tests come back negative, it doesnt mean you dont have it.
Early recognition, diagnosis, and treatment of foot PsA is critical to preventing disease progression. Delaying treatment by as little as six months can result in permanent joint damage.
Your doctor will take a medical history, and may order a physical exam, blood tests, an MRI scan, and X-rays of joints. They may also refer you to a rheumatologist, a doctor who specializes in arthritis. I went to podiatrists and orthopedic doctors trying to figure out what was happening, explained one member. All of their treatments failed. My primary doctor took one look and said, Something else is going on. Im referring you to a rheumatologist.
You May Like: Is Vicks Vaporub Good For Knee Pain
Psoriatic Arthritis Treatment For Feet
There is no cure for psoriatic arthritis but there are medications that help control inflammation and pain. Each of these psoriatic arthritis treatments work differently, and your doctor will make a recommendation based on your particular situation.
Some of the most commonly prescribed medications include:
- Nonsteroidal anti-inflammatory drugs are available over the counter and by prescription to help ease pain and inflammation. These do not prevent psoriatic arthritis from progressing.
- Disease-modifying antirheumatic drugs are available only by prescription. These drugs can prevent psoriatic arthritis from worsening and preserve joint tissue.
- Immunosuppressants target your immune system to prevent it from attacking healthy tissue.
- Biologics are a new form of DMARDs that target the specific part of the immune system triggering inflammation. Sometimes biologics are used in conjunction with another DMARD.
Doctors may also administer corticosteroid injections into the affected foot joints to help with pain, according to Gottlieb.
Arthritis In The Heel And Ankle
Several types of arthritis, including OA, RA, AS, and PsA, can affect the heels and the ankles.
Symptoms of arthritis in the heel might include:
- Stiffness upon awakening in the morning
- Recurring pain in the heel
- Swelling of the heel
- Limited movement
- Skin changes, including rashes and growths
Inflammation at the heel from RA, AS, or PsA can lead to conditions that cause heel pain. This might include Achilles tendonitis, plantar fasciitis, or retrocalcaneal bursitis, a condition in which the bursa becomes inflamed, causing pain and swelling.
The ankle is not affected by arthritis as often as other joints, but it can be a source of severe pain and instability when it is affected. Additional symptoms of ankle arthritis include swelling and stiffness of the ankle and problems with mobility. Ankle arthritis will eventually affect gaitthe way a person walks.
Recommended Reading: What Does Arthritic Knee Pain Feel Like
Other Treatments For Psoriatic Arthritis
Members of MyPsoriasisTeam also use several nonprescription treatments to alleviate PsA pain, including ice and topical painkillers, and lifestyle changes to their diet and exercise habits.
- Topical painkillers Icy Hot with lanolin helps my feet. The sprays are great for sleeping, shared one member.
- Ice Rolling your feet on a small bottle of frozen water wrapped in a towel or applying ice packs to sore areas can help reduce inflammation in feet joints.
- Apple cider vinegar I soak in 1/2 cup of apple cider vinegar and water every other day for 15 minutes. Its an anti-inflammatory that helps soothe my feet, one member said.
- Diet and exercise Adopting a healthy diet and gentle exercise program can help manage symptoms and contribute to overall well-being. Members say losing weight helps them keep stress off their joints. Slow gentle movement, such as yoga and tai chi, as well as physical therapy, helps build strength, reduce stiffness, and maintain foot mobility.
Always speak to your doctor before starting any new diet or exercise program.
Psoriatic Arthritis Signs And Symptoms
Early symptoms with psoriatic arthritis are important. People will complain of pain and swelling in their joints hands, feet, wrists, etc. They may have a small patch of psoriasis or have psoriasis covering many areas of the body. There may be complaints of stiffness and fatigue. For example, studies in Toronto showed the year before they were diagnosed, people had reported joint pain, fatigue, and stiffness. Early in the disease, people will often have episodes of worsening of the psoriatic arthritis and then episodes of improvement.
Also Check: Ra Hand Pain
What Can I Do To Help My Feet
The most important action is to seek advice and help when you notice any changes in your foot, whatever they may be. You can talk to your GP or local pharmacist for advice. Some problems can be resolved simply. For issues that are more persistent you may be referred to a specialist, such as a dermatologist, rheumatologist, physiotherapist, surgeon or chiropodist/podiatrist.
For general foot care, personal hygiene is important, particularly in avoiding fungal and viral infections. Change shoes and socks regularly, avoid shoes which are ill-fitting or cause bad posture. If you are overweight, losing weight could relieve the pressure on your joints and improve your walking gait.
If you are diagnosed with psoriasis, develop a treatment regime that works for you often, applying treatment after a bath or shower, along with the use of an emollient, can make the process easier.
If you have nail involvement, keep nails trimmed and clean. If they are thick, try trimming them after soaking them in a bath or shower, as this makes them softer and easier to cut. Alternatively, seek an appointment with a chiropodist, which is often available via the NHS.
If you have psoriatic arthritis, it is important to rest inflamed joints. Sourcing footwear that supports the foot and helps to reduce the pressure on the inflamed areas can help, as can inner soles and orthotic supports. Once again, a chiropodist is best placed to advise you.
This article is adapted from The psoriatic foot leaflet.
Still Not Sure What Causes Your Itchy Feet
- Bug bites: You should remember seasonality when it comes to itchy feet. If you notice an itch, especially an itchy big toe, a pesky mosquito could be the cause. If the itch is accompanied by a small, swelling roundness and occurs after spending time outside, you may just have an annoying bug bite!
- Scabies: Likely one of the worst-case scenarios for itchy feet, its important to ensure scabies isnt the cause. Scabies is a skin condition caused by Sarcoptes scabiei, a microscopic mite that actually burrows into your skin! With scabies, the itch in your feet will be intense and feel worse at night. There may also be bumps that form a path on the skin.
- Diabetes: A common symptom of diabetic neuropathy is a regular burning or tingling sensation in the feet. Dry skin is also common with diabetes, which can cause itchy feet.
- Thyroid problems: If your itch seems inexplicable, you may have an overactive or underactive thyroid gland. This condition can lead to itchiness on the feet and many other areas of the body.
Don’t Miss: Autoimmune Leg Pain
What Are Symptoms Of Psoriatic Arthritis In The Nails
Sometimes, psoriasis can cause more than just rashes. It can also affect the fingernails and toenails. Signs of nail psoriasis include:
-
Tiny dents
-
Thin lines of dark blood underneath the nails
-
Color changes
Nail psoriasis, while treatable, can be a bit stubborn because nails grow so slowly. It can take 6 months or longer for nails to grow back normally.
How Is Psoriatic Arthritis Treated

Treatment will depend on your symptoms, age, and general health. It will also depend on the severity of your condition.
Boththe skin condition and the joint inflammation are treated. Early diagnosis andtreatment helps prevent joint damage. Some medicines used to treat psoriatic arthritisinclude:
- Nonsteroidal anti-inflammatory medicines to ease symptoms
- Corticosteroids for inflammation
- Immunosuppressive medicines such as methotrexate to reduce inflammation if NSAIDs don’t work
- Biologic medicines to ease inflammation
- Vitamins and minerals such as calcium and vitamin D to slow bone deformation
Other treatment may include:
- Obesity
Recommended Reading: Does Psoriatic Arthritis Itch
Foot Problems Are Common In Psoriatic Arthritis Heres What You Can Do About It
Psoriasis you can usually spot: the autoimmune disease often causes red patches of skin topped with thick, silvery scales. It occurs when your bodys immune system goes into overdrive, attacking healthy tissue and causing an overproduction of skin cells. But what you cant see is that same abnormal immune response may also cause inflammation in your joints.
About one-third of people with psoriasis develop psoriatic arthritis a chronic, inflammatory disease of the joints and entheses, or places where tendons and ligaments connect to bone.
Most people with psoriatic arthritis develop psoriasis first, and are later diagnosed with psoriatic arthritis. But joint problems from psoriatic arthritis can sometimes begin before skin signs appear. Or sometimes skin issues are so mild that patients dont connect psoriasis with joint pain and realize they could have PsA.
Psoriatic arthritis can cause pain, stiffness, and swelling in any joint in your body, from your hands to your back and often, in your feet. You can read here about common psoriatic arthritis symptoms.
What Does Psoriatic Arthritis In The Feet Feel Like
When your feet are affected by psoriatic arthritis, you may have pain, tenderness, and swelling in your foot. This occurs when the membranes that line the joints, tendons, and connective tissue in the foot become inflamed. Similar to other forms of inflammatory arthritis, such as rheumatoid arthritis, joints may feel may warm to the touch, and stiffness may be worse in the morning or after periods of inactivity.
Symptoms may also flare, then go into periods of remission. Heres more information about coping with psoriatic arthritis flares.
But unlike with rheumatoid arthritis where symptoms typically occur in the same joints on both sides of your body , PsA is usually asymmetrical. You can have psoriatic arthritis in the ankle joint of one foot and the toe of another, explains Dr. Kor, who also serves as spokesperson for the American Podiatric Medical Association.
Specific foot problems caused by PsA include:
Recommended Reading: Can You Get Rid Of Arthritis
Sex Fertility And Pregnancy
Sex can sometimes be painful for people with psoriatic arthritis, particularly a woman whose hips are affected. Experimenting with different positions and communicating well with your partner will usually provide a solution.
Psoriatic arthritis wont affect your chances of having children. But if youre thinking of starting a family, its important to discuss your drug treatment with a doctor well in advance. If you become pregnant unexpectedly, talk to your rheumatology department as soon as possible.
The following must be avoided when trying to start a family, during pregnancy and when breastfeeding:
Psoriatic Arthritis And Your Feet: What Is It
Psoriatic arthritis can inflame any of the foots 26 bones, 33 joints, and connective tissues that surround the joints. I have so much pain where my toes and foot connect. Feels like a constantly moving charley horse in my foot, said one member.
Similar to rheumatoid arthritis, joints may feel warm, sore, and tender. Members report that stiffness is often worse in the morning. Getting out of bed, I have a lot of pain in my feet, said one member. I woke up with pain in my ankle. Thanks psoriasis, said another member. Unlike rheumatoid arthritis, PsA often only affects one side of the body, so just one foot or toe may be affected.
Although PsA can develop slowly with mild symptoms, several members of MyPsoriasisTeam report rapid and severe onset. I was diagnosed with psoriatic arthritis very quickly after discovering my first tiny sign of psoriasis, and unfortunately, it progressed quickly, explained one member. Another said, This disease came out of nowhere! I was literally fine, then boom, my feet started hurting and getting worse and worse.
Psoriatic arthritis flares on-and-off periods of worsening symptoms can make coping with foot PsA even more challenging, say members of MyPsoriasisTeam. Some days I am totally fine and other days, the flares are so bad I can barely walk, said one member. During a flare I need walking sticks to help me along, said another.
Recommended Reading: What Is Considered A High Level Of Rheumatoid Factor
Causes Of Psoriatic Arthritis
Researchers arent entirely sure what causes psoriatic arthritis but speculate genetics are involved. One theory is that psoriatic arthritis is connected to a family of genes called the human leukocyte antigen complex, which helps the immune system differentiate between proteins that are from the body, and those that are made by bacteria, viruses, and other pathogens. Some experts believe that trauma from an injury may trigger psoriatic arthritis in people who are already prone to the condition. Although anyone can develop psoriatic arthritis, its most common in people between 30 and 50 years old.
To be clear, psoriasis doesnt cause psoriatic arthritis. However, having psoriasis is the single largest risk factor for developing psoriatic arthritis. In particular, people who have nail psoriasis symptoms4 have a higher risk of developing psoriatic arthritis.
Pain On The Sole Of Your Foot
The plantar fascia is a thick tissue that runs along the bottom of your foot. It connects the toes to the heel bone, and often becomes inflamed when you have psoriatic arthritis. Its common for people to assume they have only plantar fasciitis, or inflammation of the plantar fascia, when they actually have psoriatic arthritis.
Recommended Reading: Rheumatoid Arthritis Itching Skin
Past Research And Achievements In This Area
In 2015, research led by our centre for genetics and genomics at the University of Manchester identified genetic variants associated with psoriatic arthritis, but not with psoriasis or rheumatoid arthritis. This helped to establish psoriatic arthritis as a condition in its own right. The findings could lead to the development of drugs specifically for psoriatic arthritis.
Later in the same year, our TICOPA trial looked at the benefits of early aggressive drug treatment for people with psoriatic arthritis followed by an increase in drug dosage if initial treatment isnt working. The trial found that patients treated this way, required fewer hospital- and community-based services than patients receiving the standard care.