Seeking Help And Getting Through It
I know now that the anger, self-pity, and suicidal thoughts with which I struggled were not just me being dramatic. It was me suffering from disease and going through the cycle of pain and stages of grief.
This was especially heightened during the postpartum depression I experienced after the birth of my son, when my hormones and inflammation were raging uncontrollably. That was when I saw that I needed help from a health care professional.
A clinical social worker was a key component in my health care team and helping me accept my new life. Before my diagnosis I had no idea what mental health care could offer me, and how much I needed that compassion. Not all health care providers who save you are patching up wounds or prescribing medication. Some simply listen to you and help you understand you are not alone.
As I went through medication after medication, I found myself having to stop many because the side effects exasperated my poor mental health state. I learned why some drug commercials say that medications may cause suicidal thoughts and actions or increased depression. It takes time to find the right RA medication that works for your symptoms and doesnt cause too many side effects.
What Is An Ra Flare
Flare-ups are episodes of increased disease activity in which the body is fighting itself. With RA flare-ups, inflammation increases.
With a flare-up, you experience a short-term increase in RA symptoms. A flare-up can last a few days or persist for weeks or months.
Flare-ups typically involve joint stiffness and pain, but all RA symptoms can worsen, including fatigue. If a flare-up is especially severe, it can affect your ability to perform daily tasks.
Fingers Toes And Skin
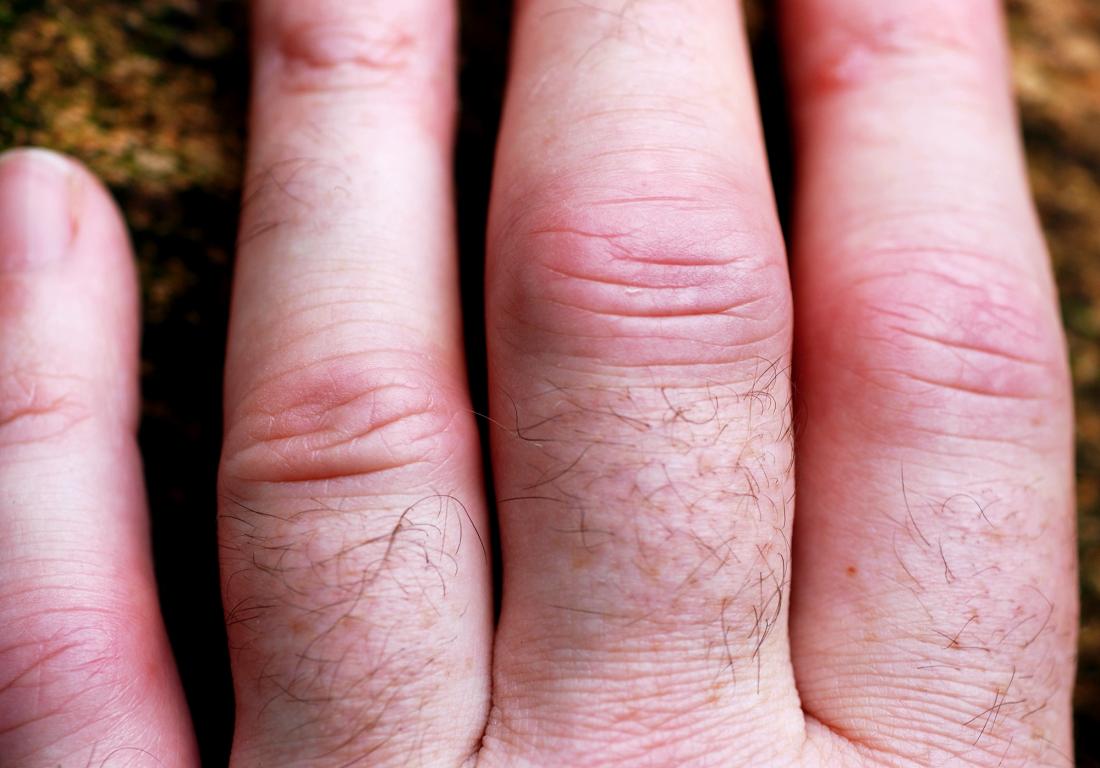
Another telling clue is the presentation of the disease on the fingers and toes. With PsA, the distal joints will be the focus of pain, swelling, and stiffness. By contrast, RA primarily involves the proximal joints .
With severe PsA, the fingers can also take on a sausage-like appearance , making it difficult to ball your fist. While this can occur with RA, it is not the hallmark that it is with PsA.
Around 85% of people of PsA with also have the most typical form of psoriasis, characterized by dry, flaky skin plaques. Moreover, half will have nail psoriasis at the time of their diagnosis. Neither of these occurs with RA.
Recommended Reading: What Can I Do For Arthritis In My Hands
Will I Need Surgery For Arthritis
Healthcare providers usually only recommend surgery for certain severe cases of arthritis. These are cases that havent improved with conservative treatments. Surgical options include:
- Fusion: Two or more bones are permanently fused together. Fusion immobilizes a joint and reduces pain caused by movement.
- Joint replacement: A damaged, arthritic joint gets replaced with an artificial joint. Joint replacement preserves joint function and movement. Examples include ankle replacement, hip replacement, knee replacement and shoulder replacement.
Symptoms Of Ra And Psa
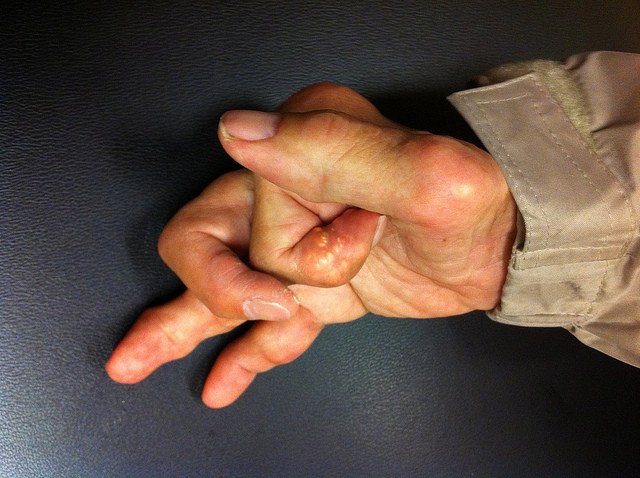
Both RA and PsA cause joint swelling, stiffness, and pain. Although both conditions affect joints in the fingers and toes, they do it in slightly different ways. And each one can cause other symptoms, too.
Rheumatoid arthritis:
- Often starts in the smaller joints, like the ones in your fingers and toes over time, it may affect other joints, too, like your wrists, knees, hips, and ankles.
- Usually shows up on the same joints on both sides of your body that means it’s symmetric.
- Often makes joints feel stiffer in the morning
- Can lead to fatigue, low-grade fever, and weight loss
Psoriatic arthritis:
- Can affect joints in the back and pelvis in addition to the ones in fingers and toes
- Often affects only one side of your body that means it’s asymmetric.
- Sometimes causes foot pain, especially on the sole of your foot or the back of your heel
- May make your fingers swell up like sausages
- May make your nails pit and flake
- Tends to affect entheses, areas where tendons or ligaments attach to bones
With both conditions, you’ll probably have times when your symptoms get worse. These are called flares. In between these flares are times without symptoms called remissions.
Recommended Reading: Signs Of Arthritis In Legs
Common Types Of Arthritis
Commonly associated with older age, arthritis affects more than 50 million Americans, including more than 300,000 children each year. There are over 100 different forms of arthritis. Depending on the type, it can be extremely painful and affect everyday activities or go relatively unnoticed and be easily managed for years.
Simply put, arthritis is the inflammation of one or more joints. Most individuals experience common symptoms like joint pain, swelling, stiffness and/or decreased range of motion.
Here are 5 of the most common types of arthritis:
Ra Fatigue: How Do I Control Chronic Fatigue From Ra
Rheumatoid arthritis is a debilitating condition that causes a wide range of symptoms. One of the most prevalent symptoms experienced in suffering from rheumatoid arthritis is chronic fatigue. Fighting fatigue for rheumatoid arthritis patients seems like an ongoing uphill battle.
For those who suffer from rheumatoid arthritis, feelings of fatigue and constant tiredness can make it difficult to get through each day. But there are some ways to help beat fatigue, stay alert, and feel more rested and happy.
You May Like: Is Vicks Vaporub Good For Knee Pain
Amplification In The Synovium
Once the generalized abnormal immune response has become established which may take several years before any symptoms occur plasma cells derived from B lymphocytes produce rheumatoid factors and ACPA of the IgG and IgM classes in large quantities. These activate macrophages through Fc receptor and complement binding, which is part of the intense inflammation in RA. Binding of an autoreactive antibody to the Fc receptors is mediated through the antibody’s N-glycans, which are altered to promote inflammation in people with RA.
This contributes to local inflammation in a joint, specifically the synovium with edema, vasodilation and entry of activated T-cells, mainly CD4 in microscopically nodular aggregates and CD8 in microscopically diffuse infiltrates. Synovial macrophages and dendritic cells function as antigen-presenting cells by expressing MHC class II molecules, which establishes the immune reaction in the tissue.
Statement Of Literature Search
For the development of this narrative review, publications were identified by a series of searches on PubMed between September 2020 and July 2021. Search terms included AND AND AND AND . Publications that detailed the characteristic clinical manifestations, comorbidities, pathogenesis, biomarkers, treatment recommendations, and differential diagnosis for PsA, RA, and OA were included. References that were determined to be irrelevant on the basis of the authors judgment were excluded from consideration. Relevant references that were cited within the publications included in this review and articles previously known by authors were considered on the basis of the criteria. This review is based on studies that were previously completed and does not contain any novel studies with human participants that were conducted by any of the authors.
Also Check: How To Slow Arthritis In Hands
Psoriatic Arthritis Often Affects People Who Have Psoriasis
Having psoriasis, a disease that often causes inflamed, scaly patches of skin on areas like your knees, elbows, and scalp, puts you at greater risk of getting psoriatic arthritis down the road. The Cleveland Clinic estimates that up to 30% of people with psoriasis get diagnosed with psoriatic arthritis. However, its possible to get psoriatic arthritis even if you dont have psoriasis, and vice versa. Psoriatic arthritis affects people of all genders at relatively equal rates and typically shows up in people between the ages of 30 and 50, says the Cleveland Clinic.
NYU Langone Health explains there are five types of psoriatic arthritis, and depending on which one you have, the disease can show up in very different ways in your body. Around three-quarters of people with the condition have a type called asymmetric oligoarthritis, which impacts up to five joints, though not necessarily the same ones on each side of the body. When the same joints are affected on each side, it may be due to symmetric arthritis, a type of psoriatic arthritis thats similar to rheumatoid arthritis. Theres also spondylitic arthritis, which affects the spine, and distal interphalangeal predominant psoriatic arthritis, which mainly involves the joints near your fingernails and toenails. The rarest form of psoriatic arthritis is arthritis mutilans. Its a severe form of the disease that can destroy the bones in your hands, per the Mayo Clinic.
Types Of Psoriatic Arthritis
Here are the five different types of psoriatic arthritis:
- Symmetric psoriatic arthritis As its name implies, this type affects joints on both sides of your body at the same time. About half of people with psoriatic arthritis have the symmetric kind.
- Asymmetric psoriatic arthritis With the asymmetric type, problems dont develop in the same joints on both sides of the body. It occurs in about 35 percent of people with the disease and often causes more mild symptoms.
- Spondylitis This form of psoriatic arthritis is characterized by pain and stiffness in the neck and spine.
- Arthritis mutilans People with arthritis mutilans experience deformities in the small joints at the ends of the fingers and toes. This type is considered the most severe form of psoriatic arthritis, but it only affects about 5 percent of people with the condition.
- Distal psoriatic arthritis It causes inflammation and stiffness near the ends of the fingers and toes, while also affecting the nails.
Read Also: What Can Be Done For Arthritis
Take Care Of Yourself
Taking care of yourself and staying on top of the disease is a big part of RA treatment. Take your medicine as directed. Try not to skip a dose. Tell your doctor about any side effects. Talk to them or your pharmacist if you have questions.
Even when your pain and stiffness is less of a problem, keep up with your medical appointments. Check in with your doctor two to four times a year.
If you dont already see a rheumatologist, consider asking for a referral. This is a doctor who specializes in arthritis. They can review your treatment plan and see if it needs any tweaks. Studies show that people with RA who see a rheumatologist several times a year do better.
Who Will Be Responsible For My Healthcare
Youre likely to see a team of healthcare professionals.
Your doctor, usually a rheumatologist, will be responsible for your overall care. And a specialist nurse may help monitor your condition and treatments. A skin specialist called a dermatologist may be responsible for the treatment of your psoriasis.
You may also see:
- a physiotherapist, who can advise on exercises to help maintain your mobility
- an occupational therapist, who can help you protect your joints, for example, by using splints for the wrist or knee braces. You may be advised to change the way you do some tasks to reduce the strain on your joints.
- a podiatrist, who can assess your footcare needs and offer advice on special insoles and good supportive footwear.
Also Check: Best Remedy For Arthritis In Hands
Psoriatic Arthritis Is A Lot Like Rheumatoid Arthritis But With A Nasty Skin Rash This Probably Sounds Terrible But I Was Secretly Happy When I Heard Phil Mickelson The Golfer Was Diagnosed With Psoriatic Arthritis Not That I Would Wish
Psoriatic arthritis is a lot like rheumatoid arthritis but with a nasty skin rash.
This probably sounds terrible but I was secretly happy when I heard Phil Mickelson the golfer was diagnosed with psoriatic arthritis. Not that I would wish the diagnosis on anyone! But I thought, wow, maybe it will increase awareness and maybe, just maybe, more studies and treatment options will become available.
I had worked for a rheumatologist/internal medicine doctor back in the early years of my nursing career. We had patients with rheumatoid arthritis, osteoarthritis, lupus, Sjogrens, a few cases of temporal arteritisI even saw my first HIV positive patient working in that clinic in the mid 80s. But I never once heard of psoriatic arthritis. I dont even remember hearing about it in nursing schooland I still hadnt heard of psoriatic arthritis when I was diagnosed in my late 40s. I was baffled by my diagnosis partly because I had no idea what it was but also it never even occurred to me since the psoriasis I had on my scalp had been diagnosed as just a bad case of dandruff and my sausage toes had been diagnosed as Mortons Neuroma.
What Are Psoriatic Arthritis And Rheumatoid Arthritis
Psoriatic arthritis occurs when the immune system mistakenly attacks the bodys own healthy tissues instead of foreign invaders, like viruses and bacteria. Unlike rheumatoid arthritis, psoriatic arthritis is related to another condition called psoriasis. The autoimmune disease psoriasis causes scaly, red patches on the skin, which can burn or itch.
Rheumatoid arthritis is the most common type of inflammatory arthritis, affecting more than 1.3 million people in the United States. Like PsA, it occurs when the immune system attacks the joints healthy cells and tissues. RA, in particular, targets the lining of the membranes surrounding the joints , causing inflammation and permanent joint damage.
Also Check: Rheumatoid Arthritis Rash Itchy
How Is Psoriatic Arthritis Mutilans Diagnosed
ishonestNo.364 Acne Scars
In some cases, people diagnosed with psoriatic arthritis didnt know they had psoriasis. In 85 percent of psoriatic arthritis cases, symptoms of psoriasis are obvious before arthritis is apparent.
To diagnose psoriatic arthritis mutilans, your doctor will first confirm you have arthritis. After checking your joints for signs of swelling or tenderness, youll receive diagnostic testing.
Your doctor may order lab tests to check for inflammation or the presence of certain antibodies. Both can point to arthritis. You doctor will also likely recommend an X-ray or other imaging test to assess joint damage.
Once your doctor has diagnosed you with arthritis, theyll test a blood sample to find out what kind of arthritis you have. For example, if the rheumatoid factor and cyclic citrullinated peptide antibodies are in your blood, you may have rheumatoid arthritis .
At this time, there isnt a lab biomarker for psoriatic arthritis or the psoriatic arthritis mutilans subset. Psoriatic arthritis mutilans is diagnosed by checking the severity of the bone destruction. There are very few conditions associated with such severe bone loss.
Also Check: Mayo Clinic Arthritis
Diagnosing Psoriatic Arthritis Vs Ankylosing Spondylitis
The right diagnosis is vital to treating both PsA and AS, and is best done by a rheumatologist. There is no single test for either condition, so health care providers must rule out other disorders.
To begin, they will take your family and medical history, ask about symptoms and perform a physical exam. They will look for joint pain patterns and locations, as well as other distinguishing symptoms, like skin and nail issues for PsA and the presence of related symptoms, like eye or GI problems.
Lab testing is done to help diagnose AS and PsA. Providers may take blood or joint fluid samples to look for levels of inflammation and discount the possibility of other illnesses, such as gout or rheumatoid arthritis. Patients suspected to have AS or PsA will likely have X-rays to check for damage to the joints. If more information is needed, additional imaging such as MRI or ultrasound can be used. Sometimes skin biopsies are involved.
Many times, especially if AS is suspected, patients will be tested for a genetic marker called HLA-B27. The gene is present in only about 8 percent of the general population but can be found in up to 95 percent of white AS patients and about 50 percent of black AS patients. In PsA, identifying the gene can help predict whether you may have problems with your spine.
Read more here about how ankylosing spondylitis is diagnosed and how psoriatic arthritis is diagnosed.
Read Also: Best Remedy For Arthritis In Fingers
How Are Psoriatic Arthritis And Rheumatoid Arthritis Diagnosed
Unfortunately, there’s enough overlap between these two conditions that diagnosis can be a little difficult, though a doctor may be able to know right away which kind of arthritis is affecting their patient.
For example, Dr. Domingues notes that the distal joints aren’t affected in RA, so asking a patient about where they experience pain can be a useful tool. Likewise, if a patient has diagnosed psoriasis or crumbling, pitting nails and visits their doctor complaining of new joint pain, they probably have PsA, not RA.
Just as often, however, further testing is needed to truly determine whether the cause of symptoms is RA or PsA.
“The good thing about RA is there are blood tests that can help us diagnose, but they aren’t terribly helpful with psoriatic arthritis,” says Dr. Domingues. “There’s no gene or blood test for PsA, but inflammatory markers can be elevated in both conditions.”
Radiology can also be helpful for diagnosing both conditions, Dr. Domingues explains: “Both x-rays and MRIs can allow us to see inflammation and bone issues .”
RELATED: ‘I Was Diagnosed With Rheumatoid Arthritis at 40Right After I Had a Baby’