How Rheumatologists Diagnose Ra
Findings from a physical exam and medical history are important factors in diagnosing RA, say experts. Common RA symptoms include:
- Joints that feel tender, warm, or swollen for six weeks or more
- Multiple joints can be affected
- Joint pain that is commonly symmetrical
- Joint stiffness, especially first thing in the morning that lasts for an hour or more
- Fatigue
- Low-grade fever
- Loss of appetite
While many of these symptoms can occur with other diseases, infections, or injuries, there are subtle traits unique to RA that can help doctors make the diagnosis.
Pain, swelling, and stiffness in smaller joints in the hands, toes, and elbow, for example as opposed to one or two bigger joints, like the knee and hip, usually indicates a pattern more likely to be RA, says Dr. Husni. Pain from RA is usually more symmetric in nature, occurring on both sides of the body. When you injure yourself or have an overuse injury, however, pain usually occurs in just one joint. Joint stiffness can occur with injuries or other conditions, but stiffness with RA typically occurs in the morning and can be overwhelming, explains Dr. Husni. Its not a joint stiffness that passes after a few minutes, but more like you cant even move the covers to get out of bed.
Managing Symptoms Of Autoimmune Arthritis
Several medications work for both psoriatic arthritis and rheumatoid arthritis:
- Nonsteroidal anti-inflammatory medications reduce pain and swelling.
- Disease-modifying antirheumatic drugs protect joints and slow the disease, and less of the joint is destroyed, meaning theres less swelling, pain and less loss of joint function.
- Biologics target the specific parts of the immune system that drive inflammation.
As researchers learn more about the causes of inflammatory arthritis, theyre developing new medications to manage these diseases. Some of these new drugs are designed to specifically target one disease or the other.
Both psoriatic arthritis and rheumatoid arthritis are chronic diseases. They cant be cured, but they can be managed, Dr. Rosian says. By working with your doctor to get the correct diagnosis, you can manage symptoms to feel your best.
Will Dietary Changes Help My Rheumatoid Arthritis
Diet may play a role in some patients, but most patients should maintain a well-balanced diet rather than avoid specific foods. Keep a diary to determine whether certain foods are associated with your disease flares and then see if removing them from your diet is helpful.
Some studies do suggest that eating fish two or more times per week may be associated with fewer disease-related symptoms, and there is increasing evidence that achieving and maintaining a healthy weight is helpful for managing RA.
Read Also: Inflammatory Polyarthritis Symptoms
Gout Statistics And Facts
- 8.3 million people in the United States have gout .*
- Among people who have gout attacks, 90% have kidneys that dont remove enough uric acid from their urine while 10% make too much uric acid in their system.
- 90% of gout attacks start in a single joint. Most often, it is the bunion joint of the big toe.
- 90% of gout patients have one or more of the following conditions , which make it more difficult to manage gout: kidney dysfunction, coronary heart disease, obesity, high cholesterol and/or triglycerides, diabetes mellitus.**
*Prevalence of gout and hyperuricemia in the US general population: the National Health and Nutrition Examination Survey 2007-2008. Zhu Y, Pandya BJ, Choi HK. Arthritis Rheum. 2011.**Comorbidities of gout and hyperuricemia in the US general population: the National Health and Nutrition Examination Survey 2007-2008. Zhu Y, Pandya BJ, Choi HK. Am J Med. 2012.
Small Joint Inflammation: Symptoms In The Fingers Wrists Toes And Ankles
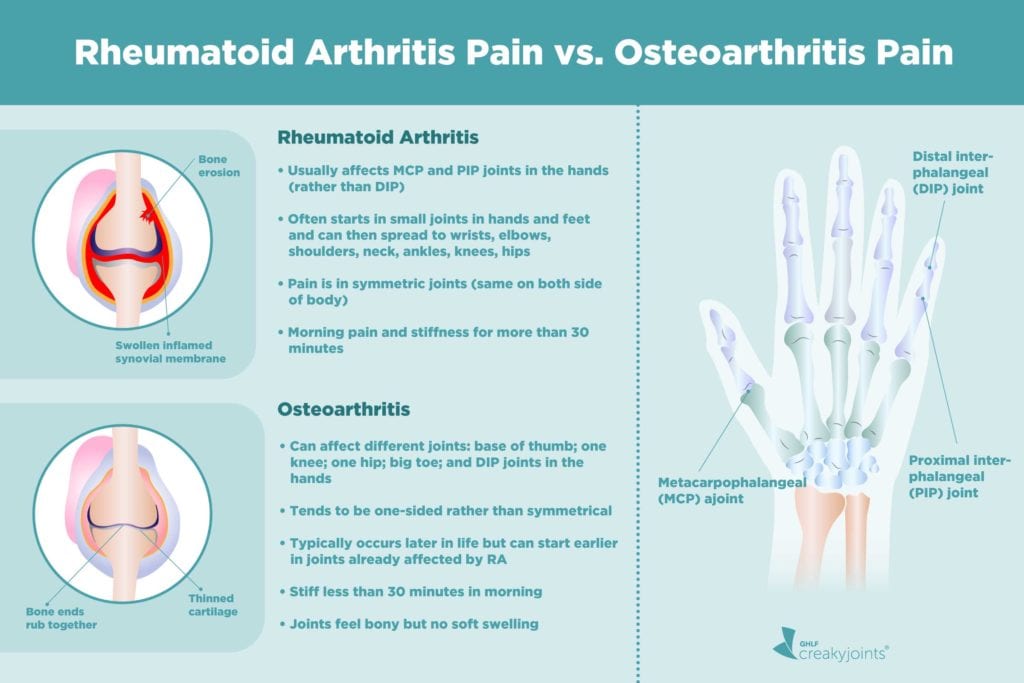
For more than half of RA patients, the first symptoms will occur in one or more of the small joints of the fingers , the wrists, the toes , or the ankles. Symptoms can begin slowly and subtly over a period of weeks or months, worsening over time.
In the majority of patients, this swelling and pain is symmetrical, meaning the same joints are affected on both sides of the body.
But this is not always the case. Its important not to wait to treat until the disease becomes symmetric. Early diagnosis and treatment are key to prevent joint damage even if only one joint on one side of the body is affected, notes Rebecca Manno, MD, a rheumatologist and adjunct assistant professor of medicine at the Johns Hopkins University School of Medicine in Baltimore.
Read Also: Rheumatoid Arthritis Pain Relief
The Importance Of Seeing A Rheumatologist
Thats why its important to see a rheumatologist if you think you might have arthritis symptoms, advises Elaine Husni, MD, MPH, vice chair of the department of rheumatic and immunologic diseases and director of the Arthritis Center at the Cleveland Clinic. A rheumatologist is a doctor who specializes in treating arthritis and certain autoimmune disease. They are trained to diagnose RA at an earlier stage, which may minimize unnecessary testing and treatment and help to improve overall patient outcomes.
That advice would have benefited CreakyJoints member Lindsey Stambaugh. Her symptoms also began after the birth of her son. Her first doctor told her the pain was psychological a few years later, she was sent to a pain clinic, where she was given medications and injections to mute the symptoms. It wasnt until Stambaugh started working in a rheumatologists office, who recognized symptoms during one of her flare-ups, that she was evaluated for and diagnosed with RA.
What Are The Signs And Symptoms Of Ra
With RA, there are times when symptoms get worse, known as flares, and times when symptoms get better, known as remission.
Signs and symptoms of RA include:
- Pain or aching in more than one joint
- Stiffness in more than one joint
- Tenderness and swelling in more than one joint
- The same symptoms on both sides of the body
- Weight loss
You May Like: Stiff Hands Treatment
Periodontitis And Rheumatoid Arthritis: The Same Inflammatory Mediators
1Department of Internal Medicine and Medical Specialties, Sapienza University of Rome, Rome, Italy
2Department of Oral and Maxillo-Facial Sciences, Sapienza University of Rome, Viale Regina Elena 287a, 00161 Rome, Italy
Abstract
The strict link between periodontitis and rheumatoid arthritis has been widely demonstrated by several studies. PD is significantly more frequent in RA patients in comparison with healthy subjects: this prevalence is higher in individuals at the earliest stages of disease and in seropositive patients. This is probably related to the role of P. gingivalis in inducing citrullination and leading to the development of the new antigens. Despite the many studies conducted on this topic, there is very little data available concerning the possibility to use the same biomarkers to evaluate both RA and PD patients. The aim of the review is to summarize this issue. Starting from genetic factors, data from literature demonstrated the association between HLA-DRB1 alleles and PD susceptibility, similar to RA patients moreover, SE-positive patients showed simultaneously structural damage to the wrist and periodontal sites. Contrasting results are available concerning other genetic polymorphisms. Moreover, the possible role of proinflammatory cytokines, such as TNF and IL6 and autoantibodies, specifically anticyclic citrullinated peptide antibodies, has been examined, suggesting the need to perform further studies to better define this issue.
1. Introduction
How Is Inflammatory Arthritis Treated
Inflammatory arthritis is usually treated with a combination of medications that relieve swelling and pain along with others, such as steroids or immunosuppressive drugs, that regulate the immune system. To prevent loss of mobility and joint function, it is essential that patients strive to balance between periods of rest and activity .
As with osteoarthritis, joint replacement surgery may need to be considered when these nonsurgical methods have failed to provide lasting benefit.
Learn more about IA from the articles below or find the best arthritis doctor at HSS for your condition and insurance by selecting treating physicians.
You May Like: Vicks Vaporub For Joint Pain
Heart Disease Risk Increases With Ra
One of the most concerning conditions that can evolve in people with RA is cardiovascular disease, especially ischemic heart disease, in which there’s a reduced blood supply in the heart.
Other cardiovascular issues people with RA are at increased risk for include heart attack, stroke, congestive heart failure, peripheral vascular disease, and atrial fibrillation.
Its crucial that people with RA continue to be monitored for heart disease risks by their general practitioner or cardiologist. In a review of preventative measures for people with RA, published in June 2020 in the journal Nature Reviews Rheumatology, the authors noted that catching risk factors early, such as high blood pressure or high blood lipids, is especially important for preventing a serious cardiac event.
In addition, people with RA are more likely to develop type 2 diabetes another cardiovascular risk factor as those without RA, possibly because the inflammation of RA affects blood sugar levels and insulin resistance.
When Should I See My Doctor
If you notice symptoms of rheumatoid arthritis, or you are concerned that you may have rheumatoid arthritis, you should see your doctor as soon as possible. Your doctor may refer you to a rheumatologist who is a doctor that specialises in joints. It is important to act quickly. The sooner you start treatment, the less likely you are to experience permanent joint damage and deformity.
You May Like: Stop Arthritis In Fingers
What Are The Warning Signs Of Arthritis
Pain from arthritis can be ongoing or can come and go. It may occur when you’re moving or after you have been still for some time. You may feel pain in one spot or in many parts of your body.
Your joints may feel stiff and be hard to move. You may find that it’s hard to do daily tasks you used to do easily, such as climbing stairs or opening a jar. Pain and stiffness may be more severe during certain times of the day or after you’ve done certain tasks.
Some types of arthritis cause swelling or inflammation. The skin over the joint may appear swollen and red and feel hot to the touch. Some types of arthritis can also cause fatigue.
Polymyalgia Rheumatica Vs Rheumatoid Arthritis: Whats The Connection
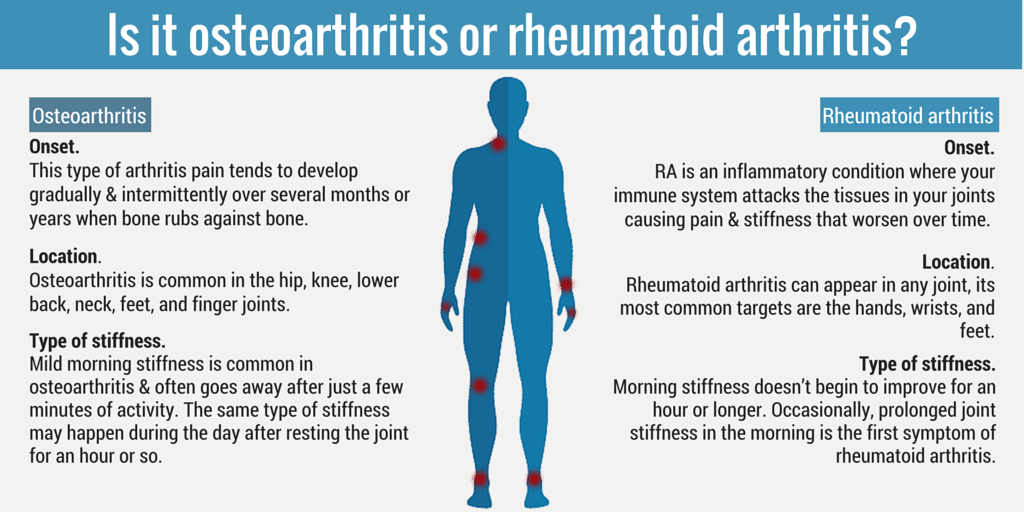
PMR is known for causing acute musculoskeletal inflammation in the elderly, whereas RA causes joint pain that can affect anyone of any age, but is often diagnosed in middle age.While both conditions cause pain and stiffness, PMR mostly affects the shoulders. RA is known for affecting joints throughout the body, although it seems to wreak the most havoc to the smaller joints of the hands and feet.
About 30% of people with PMR develop symptoms similar to those that are commonly seen in people with RA. This may include joint swelling and pain and degenerative changes in their joints.
In people who have mild joint inflammation with RA, a PMR misdiagnosis may occur. In fact, up to 20% of people who are diagnosed with PMR are eventually diagnosed with RA.
Proper nutrition, activity, rest and medicinal treatment are important for the management of both PMR and RA. When symptoms are managed, a person can typically return to daily activity and enjoy a quality life.
Recommended Reading: Tell Me About Arthritis
What Are The Different Types Of Arthritis
Arthritis is a broad term that describes more than 100 different joint conditions. The most common types of arthritis include:
- Osteoarthritis, or wear and tear arthritis, which develops when joint cartilage breaks down from repeated stress. Its the most common form of arthritis.
- Ankylosing spondylitis, or arthritis of the spine .
- Juvenile arthritis , a disorder where the immune system attacks the tissue around joints. JA typically affects children 16 or younger.
- Gout, a disease that causes hard crystals of uric acid to form in your joints.
- Psoriatic arthritis, joint inflammation that develops in people with psoriasis .
- Rheumatoid arthritis, a disease that causes the immune system to attack synovial membranes in your joints.
Amplification In The Synovium
Once the generalized abnormal immune response has become established which may take several years before any symptoms occur plasma cells derived from B lymphocytes produce rheumatoid factors and ACPA of the IgG and IgM classes in large quantities. These activate macrophages through Fc receptor and complement binding, which is part of the intense inflammation in RA. Binding of an autoreactive antibody to the Fc receptors is mediated through the antibody’s N-glycans, which are altered to promote inflammation in people with RA.
This contributes to local inflammation in a joint, specifically the synovium with edema, vasodilation and entry of activated T-cells, mainly CD4 in microscopically nodular aggregates and CD8 in microscopically diffuse infiltrates. Synovial macrophages and dendritic cells function as antigen-presenting cells by expressing MHC class II molecules, which establishes the immune reaction in the tissue.
Read Also: Ra And Tendonitis
Physical Therapy And Assistive Devices
Physical therapy can help improve muscle strength, flexibility, and range of motion. Stronger muscles can better support a joint, possibly easing pain during movement.
Assistive devices, like canes, raised toilet seats, or equipment to help you drive a car and open jar lids, are available to help you maintain independence and daily function.
Heart And Blood Vessels
People with RA are more prone to atherosclerosis, and risk of myocardial infarction and stroke is markedly increased.Other possible complications that may arise include: pericarditis, endocarditis, left ventricular failure, valvulitis and fibrosis. Many people with RA do not experience the same chest pain that others feel when they have angina or myocardial infarction. To reduce cardiovascular risk, it is crucial to maintain optimal control of the inflammation caused by RA , and to use exercise and medications appropriately to reduce other cardiovascular risk factors such as blood lipids and blood pressure. Doctors who treat people with RA should be sensitive to cardiovascular risk when prescribing anti-inflammatory medications, and may want to consider prescribing routine use of low doses of aspirin if the gastrointestinal effects are tolerable.
Recommended Reading: Things To Help Arthritis In Hands
What Are The Treatments For Rheumatoid Arthritis
RA is usually treated with a combination of medications to relieve swelling and pain while regulating the immune system. Joint surgery to relieve pain and disability, including joint replacement, may also be considered when these nonsurgical methods have failed to provide lasting benefit.
With early detection and intervention, RA and other forms of inflammatory arthritis can be treated very effectively. The connects patients quickly and efficiently with a rheumatologist who can evaluate their joint pain and get each patient started on an appropriate course of treatment. HSS also offers specialized for people with RA.
Today, we are blessed with a deeper understanding of the pathogenesis and characteristics of RA and the availability of safe and effective medications that can alter the natural history of RA and improve function. We start with the premise that RA is eminently controllable, and the goal of our therapies is “no evidence of disease.” That means no signs of redness, warmth, swelling or tenderness and normal function. Since we would not accept uncontrolled illness in angina, chronic obstructive lung disease, hypertension or diabetes, we should similarly not accept it in RA. Luckily, today, we have the therapeutic tools to make this happen.
Rheumatoid Arthritis Can Impact A Large Number Of Other Organs
RA can significantly affect a number of other organs as it progresses, especially if the disease is not controlled with medications, including:
- The Eyes Episcleritis, an inflammation of the episclera a tissue in the white part of the eye can occur.
- The Lungs Lungs can show scarring or develop interstitial lung disease, which can cause difficulty breathing, breathlessness, or a mild cough. Usually this is seen as the disease progresses, but it can show up in some early-stage patients, says Mannon.
- The Skin Some patients may develop blisters or nodules under the skin that are caused by inflamed blood vessels. Rashes and skin ulcers can erupt as well.
- The Mouth People with RA are twice as likely to have gum disease as those without RA. Research suggests that underlying gum disease may be a trigger for developing RA, and that getting treated for gum disease can improve joint symptoms.
- The HeartHeart failure is twice as common in people with RA, and theyre also 50 percent more likely to have a heart attack.
- The Kidneys RA can also damage the kidneys, especially when RA is not well controlled.
Don’t Miss: How To Get Rid Of Arthritis In Fingers
Chronic Swelling And Inflammation In Synovial Lining In Joints
No one knows exactly why RA targets the small joints of the feet and hands first, but experts do know that the synovial lining is involved.
The synovial lining is the thin layer of cells between all joints. A joint is where two bones meet, and the synovial lining is the thin layer of cells between them. Joints are covered in cartilage to cushions them, and the synovial lining between joints nourishes both the cartilage and bones.
Experts believe that RA develops when the white blood cells that normally protect the body turn on the joints instead, causing inflammation. This may occur because a person is predisposed, due to genes or environmental factors.
This inflammation is why people with RA experience pain, heat, and swelling early in the disease process .
Treatment Of Osteoarthritis Vs Rheumatoid Arthritis
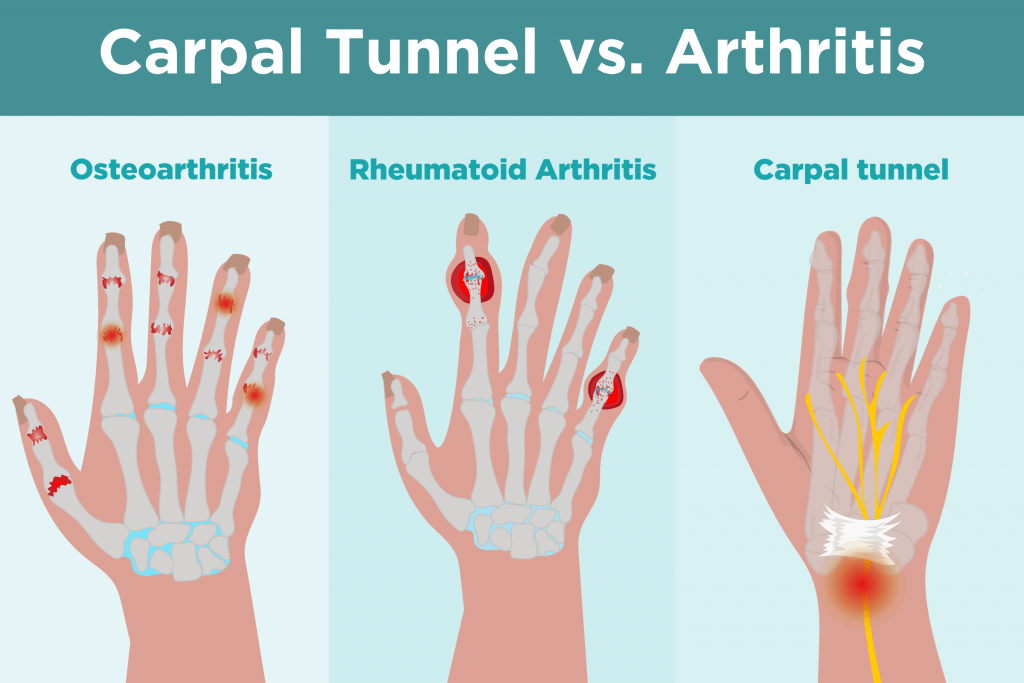
Rheumatoid arthritis treatment options are typically aimed at modulating the immune system to calm inflammation, reduce autoimmune attacks on the joints, and ease symptoms. Nonsteroidal anti-inflammatory drugs such as Ibuprofen, Aleve , and Aspirin may be used to relieve mild to moderate pain and inflammation in both forms of arthritis. However, the mainstays of RA treatment are disease-modifying antirheumatic drugs, or DMARDs. DMARDS are designed to modulate the immune system to control the processes that cause inflammation and joint damage. In severe cases, surgery may be needed to repair or replace joints. Read more about rheumatoid arthritis treatments.
With osteoarthritis, symptoms can be managed with over-the-counter and prescribed treatments, including NSAIDs. Heating and icing joints can provide pain relief. Cortisone or hyaluronic acid injections may improve symptoms too. Surgery may be recommended in some cases. DMARDs would not help in cases of osteoarthritis, since OA is not an autoimmune disease.
Condition Guide
Read Also: Arthritis Knuckle Pain