We Report Seven Cases Of Patients With Seropositive Rheumatoid Arthritis In Whom Involvement Of The Thoracic And Lumbar Vertebrae Occurred
A plain radiographic examination of the patient’s thoracolumbar spine upon admission shows multiple thoracolumbar fractures on t11, l2, and 3, and sclerosis of the. It leads to swelling and inflammation of the joints. Psoriatic arthritis often develops in people with a personal or family history of psoriasis.
Causes Of Osteoarthritis And Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune disease in which the immune system mistakenly attacks the joints in the same way that the immune system normally would fight viruses or bacteria. The joint damage in this type of arthritis is caused by the bodys immune system, resulting in inflammation that leads to pain, swelling, redness, and warmth, as well as progressive damage.
Osteoarthritis is not caused by inflammation. With heavy usage or aging, cartilage breaks down and exposes the bones of the joints. This results in pain, stiffness, and a decrease in mobility.
Read more about causes of rheumatoid arthritis.
Different Types Of Arthritis Very Different Treatments
The goal of treatment for both is to improve movement, reduce pain, and minimize joint damage, but the way to that is different for each disease, says Dr. Rackoff. Here’s what to expect:
RA The first line of defense is using disease-modifying anti-rheumatic drugs to reverse chronic inflammation. Anti-inflammatories, pain meds, and physical therapy are also used. It may take some time to determine which medication works optimally for your specific circumstances. A person may even need to try a few different types of medicine or a combination of medications. No two people, even with the same diagnoses, are alike in how they respond to various treatments. Its a puzzle that has to be put together by you and your doctor, says Dr. Wilmarth. Its very important to keep an open and honest dialogue with your doctor and healthcare team in general and especially in order to ideally reach and maintain remission with RA.
The goal with RA and other autoimmune illnesses is to treat to target . This sets remission or low disease activity as a goal. Patients are monitored frequently with their rheumatologist and adjustments to their treatment protocol are made as necessary.
RELATED: Your Rheumatoid Arthritis Plan: When Remission Is the Target
Don’t Miss: How To Treat Arthritis In Your Hip
Rheumatoid Arthritis Vs Osteoarthritis
The first step in finding relief from joint pain, swelling, and stiffness is working with your doctor to determine if you could be having symptoms of certain types of arthritis, such as rheumatoid arthritis or osteoarthritis . The sooner you know, the sooner you can begin treatment and find relief from your symptoms.
Weve put together a quick guide to help you understand the differences between RA and OA. While RA and OA can both lead to joint pain and stiffness, there are important differences that can help you have a conversation with your doctor to assist in identifying which type of arthritis you might haveand ultimatelyhow to treat it. Use the chart below to learn more about RA and OA.
Dont Miss: Rheumatoid Arthritis Better With Movement
How To Tell The Difference Between Oa And Ra
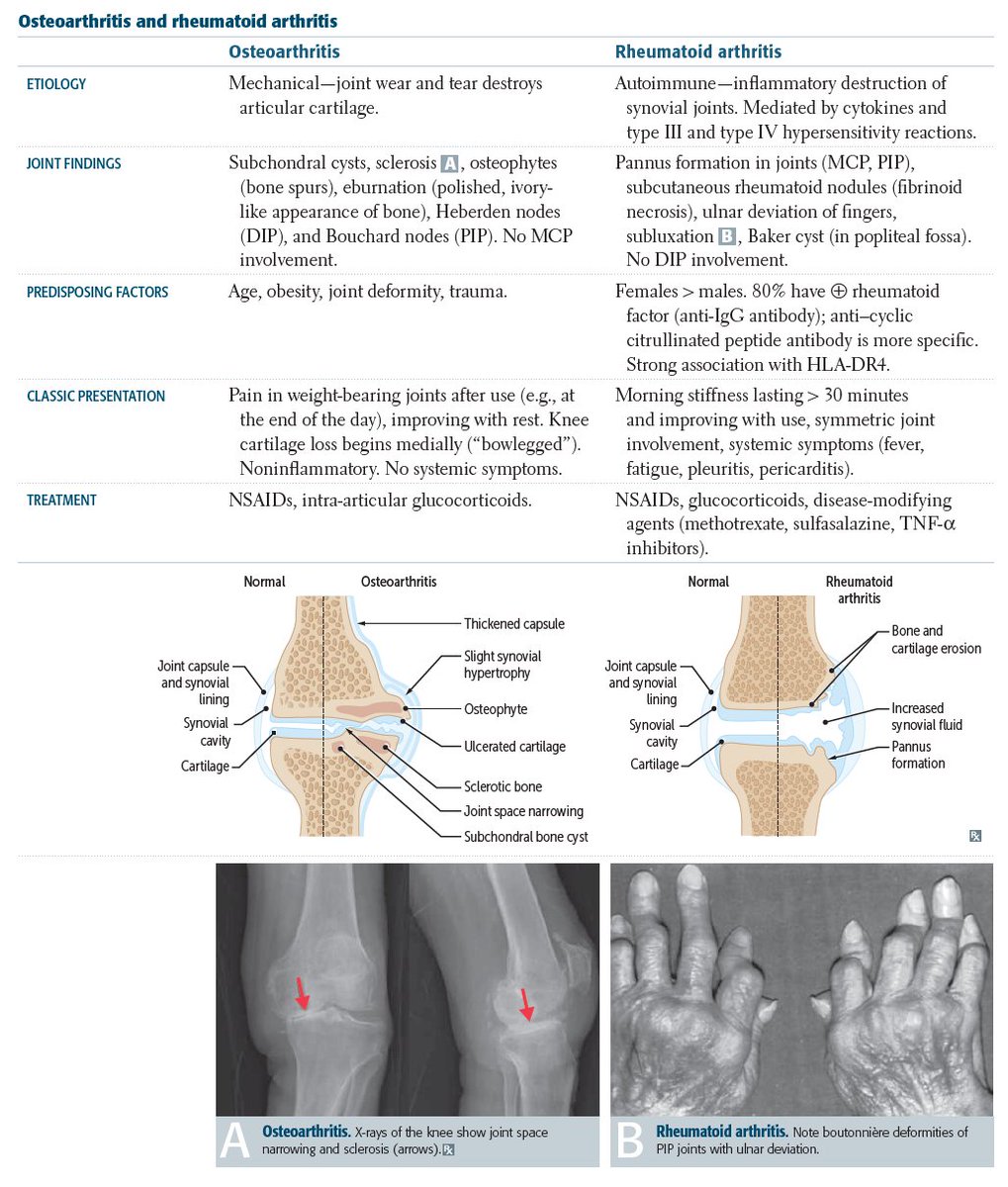
Both types of arthritis can lead to pain, stiffness, and a decrease in mobility in the joints. In RA, joint stiffness and arthritis pain are symmetrical, occurring on both sides of the body. In addition to pain and morning stiffness, RA often causes affected joints to swell and feel warm. Unlike RA, osteoarthritis in the joints is not necessarily symmetrical in nature since it’s based on wear. In other words, one hand or wrist may be impacted, but not the other.
RA is a systemic disease that can cause general symptoms, such as fatigue and fever, as well as inflammation in other parts of the body including the eyes, blood vessels, and the membrane that surrounds the heart. RA raises risk factors for lung disease and cardiovascular disease. Osteoarthritis is limited to the joints.
Read more details about rheumatoid arthritis symptoms.
Also Check: What Can I Drink For Arthritis
What Is The Safest Drug For Rheumatoid Arthritis
The safest drug for rheumatoid arthritis is one that gives you the most benefit with the least amount of negative side effects. This varies depending on your health history and the severity of your RA symptoms. Your healthcare provider will work with you to develop a treatment program. The drugs your healthcare provider prescribes will match the seriousness of your condition.
Its important to meet with your healthcare provider regularly. Theyll watch for any side effects and change your treatment, if necessary. Your healthcare provider may order tests to determine how effective your treatment is and if you have any side effects.
What Drugs Should I Be Taking For Rheumatoid Arthritis
Q) I’m 61 and I’ve had rheumatoid arthritis in both my hands for about five years.
At first I was in complete denial and refused to go onto any sort of medication, which, looking back on it, was extremely foolish. Since then I’ve been on several types of medication, including methotrexate. I lasted precisely 11 weeks on it before developing nausea and shortness of breath. I consequently got very frightened and came off it immediately.
For the past 18 months, I’ve been on sulfasalazine, which, although is keeping it at bay, isn’t preventing the damage to my joints. I’ve had several flare-ups, which have rendered me almost immobile at times.
My rheumatologist is now trying to persuade me to try methotrexate again, this time by injection, or biological medication, which will also be by injection.
I’ve got to the stage where I feel like coming off all drugs, as I feel that I keep taking all this awful, toxic medication yet nothing is working. My left hand is constantly swollen and my right hand is extremely disfigured. I dont have much pain, which is a good thing, but my main concern is that nothing is stopping the damage to my joints.
I know I’m lucky that it’s only in my hands but it really can render me useless at times. I’m afraid to pick up my grandson for fear of dropping him.
I’m at a loss as to what to do for the best. I just want something that works.
Rhona, via email – 2015
I wish you all the best in whatever decision you make.
Recommended Reading: Can Rheumatoid Arthritis Make You Feel Tired
How Rheumatoid Arthritis Differs From Osteoarthritis
- Most people with arthritis have osteoarthritis, which commonly occurs with age.
- But theres another type called rheumatoid arthritis , a serious autoimmune disease. The two are often confusedwhich can be endlessly frustrating for those with RA.
- Everybody says that arthritis is one word, says Christopher Evans, DSc, PhD, the Maurice Mueller Professor of Orthopaedic Surgery at Harvard Medical School in Boston. But the conditions are quite different.
- Here are 13 ways to tell the two apart.
Recommended Reading: Bee Pollen For Arthritis
Joint Pain Onset: What Did You Notice First
RA It may be first noticed as tenderness and pain. If it lasts more than six weeks then you definitely want to seek medical care. If you have sudden onset of pain, redness, and swelling, this should be addressed right away. Often, the small joints in the hands and feet are affected first and equally on both sides.
RA is an autoimmune disease with inflammation. Many people experience fatigue and low-grade fevers. At times the fatigue may be one of the first things that a patient notices, either before or along with the joint pain. Some of the symptoms can wax and wane, including flares.
OA Osteoarthritis was long believed to be caused by the wearing down of joints over time. But scientists now see it as a disease of the entire joint, involving the cartilage, joint lining , ligaments, and bone. OA is a common joint disease that affects from middle-aged to elderly people, women more than men. OA joint pain can build up gradually over time. However, it can become worse after use for example, after a hike.
Also Check: What Is Juvenile Idiopathic Arthritis
Is A Fear Of Falling A Symptom Of Osteoarthritis
Q) I’m 86 and have had osteoarthritis for many years. This has worsened during the past five years, with me requiring a walking stick and now a tri-wheel walker. The worst side effect is that I can’t go down slopes and am nervous even with the help of the walker, feeling that I will fall over. Initially I believed that this was a psychological reaction, but I was assured that it was a symptom of the condition. Is this correct, please, and is there anything I can do about it?
Robert, via email – 2013
This answer was provided by Dr Philip Helliwell in 2013, and was correct at the time of publication.
Osteoarthritis Vs Rheumatoid Arthritis
Many individuals mistakenly think these are the same diseases, but there are many differences between the characteristics of these two causes of arthritis. In this post, we will discuss the similarities and differences between osteoarthritis and rheumatoid arthritis and also touch on some other forms of arthritis.
Arthritis can be defined as the inflammation of a joint. Arthritis is actually considered a symptom of a disease, not a disease itself. There are more than 100 diseases that have a common symptom of arthritis.
Osteoarthritis is the inflammation of weight bearing joints that causes the breakdown of the cartilage, bone thickening, and bone spurs within the joint. It is not a systemic disease, which means it could affect only a single joint in your body. For example, you may have a significant degree of osteoarthritis in one knee, but not as significant arthritis in the other. However, osteoarthritis can affect multiple joints. There are many risk factors for the development of OA in a joint, but it is mostly due to wear and tear from excessive stress on a joint over time.
Rheumatoid arthritis is a chronic autoimmune disease causing inflammation of the synovial membrane that surrounds the joint. The synovial membrane is connective tissue that lines the inside portion of the joint. It holds the synovial fluid, a fluid that provides protection and lubrication for the joint. This inflammation leads to swelling and joint and tissue destruction over time.
Gout:
Read Also: How Does Copper Help Arthritis
Can You Have Both Ra And Oa
Yes, its possible to have both RA and OA.
While OA usually develops after years of wear and tear on cartilage, people with RA may have it earlier in life due to causes such as sports injuries that result in damage to the cartilage, joints, or ligaments.
People with RA may also develop OA as they get older.
People older than 65 who may have OA can also develop a condition called . Unlike RA, EORA more frequently affects large joints.
Rheumatoid Arthritis And Osteoarthritis Are Two Forms Of Arthritis That Affect The Joints Differently
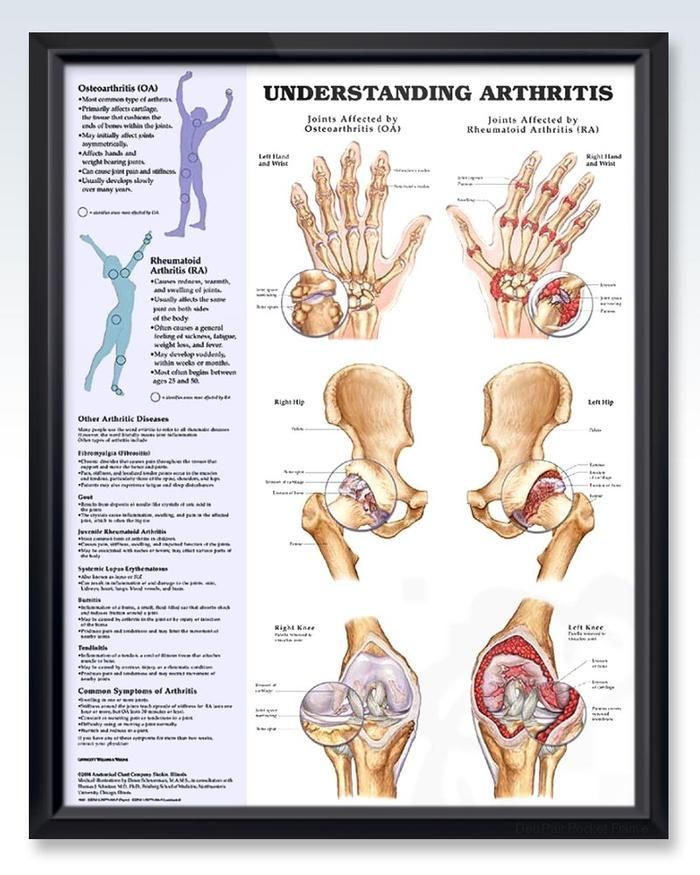
When I tell people I have rheumatoid arthritis and osteoarthritis, Im usually met with shock and confusion. Shock because I, a 30-something, dont match the image in their head of a typical person living with arthritis. Confusion because, despite all the efforts to raise awareness about arthritis, many people dont know there are multiple types of arthritis.
Arthritis is not a single disease that affects only the elderly. Rather, it is a category of diseases characterized by joint pain, swelling, and stiffness. While arthritis becomes more common with age, it can affect anyone even kids can have arthritis. Some of the diseases that fall within the broader category of arthritis or rheumatic diseases include lupus, gout, fibromyalgia, and, of course, my conditions osteoarthritis and rheumatoid arthritis.
Although each of these diseases affect the joints, they do so in different ways.
- Osteoarthritis is the result of wear and tear on your bones protective cartilage.
- Rheumatoid arthritis, on the other hand, occurs when your immune system turns against your bodys tissues, causing inflammation, swelling, and pain that impacts the lining of your joints.
Recommended Reading: Are Bananas Bad For Rheumatoid Arthritis
What Are The Risk Factors For Developing Rheumatoid Arthritis
There are several risk factors for developing rheumatoid arthritis. These include:
- Family history: Youre more likely to develop RA if you have a close relative who also has it.
- Sex: Women and people designated female at birth are two to three times more likely to develop rheumatoid arthritis.
- Smoking:Smoking increases a persons risk of rheumatoid arthritis and makes the disease worse.
- Obesity: Your chances of developing RA are higher if you have obesity.
Is Chronic Inflammatory Arthritis The Same As Rheumatoid Arthritis
Q) Im 63 and have suffered from osteoarthritis for around 10 years. Ive recently been diagnosed with chronic inflammatory arthritis, at which time my consultant also used the words rheumatoid arthritis. Although the blood markers were negative, which he said applied to around 30 per cent of sufferers, an MRI showed inflammation and degeneration around the joints of my hands. Hes prescribed methotrexate and folic acid. Are these conditions the same? Id like to refer to my condition correctly.
Nigel, Horsham, East Sussex 2011
This answer was provided by Dr Philip Helliwell in 2011, and was correct at the time of publication.
You May Like: What Arthritis Mean
Read Also: What Medicine To Take For Arthritis Pain
Whats The Age Of Onset For Rheumatoid Arthritis
RA usually starts to develop between the ages of 30 and 60. But anyone can develop rheumatoid arthritis. In children and young adults usually between the ages of 16 and 40 its called young-onset rheumatoid arthritis . In people who develop symptoms after they turn 60, its called later-onset rheumatoid arthritis .
When To See A Doctor For Osteoarthritis Or Rheumatoid Arthritis
If you have pain, discomfort, stiffness, or swelling in your joints that isnt going away, its best to see a doctor as soon as you can. These symptoms may indicate that you have either osteoarthritis or rheumatoid arthritis. Getting an early diagnosis for either of these conditions is vital to help slow down their progression. A primary care physician will likely be able to diagnose you, or you may be referred to a rheumatologist or orthopaedist.
Recommended Reading: How Do You Treat Gout Arthritis
Diagnosing Osteoarthritis Vs Rheumatoid Arthritis
Rheumatoid arthritis is generally diagnosed through a combination of a physical examination, blood tests, and imaging scans. The evaluation is usually undertaken by a rheumatologist.
Osteoarthritis is also diagnosed with a physical examination and may be followed up with imaging scans, such as an X-Ray. While there is currently no blood test that can identify whether you have osteoarthritis, a joint fluid analysis may be undertaken to rule out other causes for joint pain, such as gout.
How Osteoarthritis Differs From Rheumatoid Arthritis
While similar, there are differences between the two diseases.
Most people with arthritis have osteoarthritis, which commonly occurs with age.
But there’s another type called rheumatoid arthritis , a serious autoimmune disease. The two are often confusedwhich can be endlessly frustrating for those with RA.
“Everybody says that arthritis is one word,” says Christopher Evans, DSc, PhD, the Maurice Mueller Professor of Orthopaedic Surgery at Harvard Medical School in Boston. “But the conditions are quite different.”
Here are 13 ways to tell the two apart.
Recommended Reading: How To Help Arthritis In Your Hands
How Is Knee Arthritis Diagnosed
Your doctor may use some of the following diagnostic tests and procedures to determine if you have knee arthritis:
- Medical history and physical examination
- Blood tests for genetic markers or RA antibodies
- X-rays to determine cartilage loss in the knee
- Joint aspiration: drawing out and testing the synovial fluid inside the knee joint
Cartilage cannot be seen on X-ray, but narrowing of the joint space between the bones indicates lost cartilage. X-rays show bone spurs and cysts, which can be caused by osteoarthritis. Other tests such as MRI or CT scans are rarely needed for diagnosis.
Rheumatoid Arthritis And An Anti
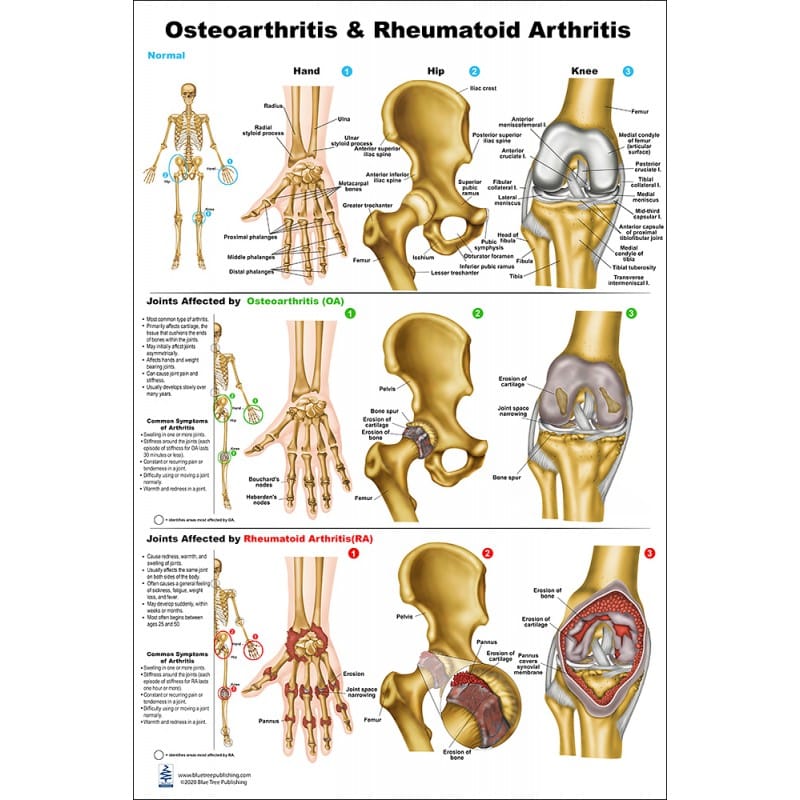
As rheumatoid arthritis is so widespread, there is a lot of research related to it. For example, several studies have examined the effect of an anti-inflammatory diet on rheumatoid arthritis. However, from a purely scientific perspective, no specific diet has been shown to be more effective. For this reason, simply a varied and nutritional diet is recommended.
Recommended Reading: What Does Degenerative Arthritis Mean
What Are The Symptoms Of Rheumatoid Arthritis
Rheumatoid arthritis affects everyone differently. In some people, joint symptoms develop over several years. In other people, rheumatoid arthritis symptoms progress rapidly. Many people have time with symptoms and then time with no symptoms .
Symptoms of rheumatoid arthritis include:
- Pain, swelling, stiffness and tenderness in more than one joint.
- Stiffness, especially in the morning or after sitting for long periods.
- Pain and stiffness in the same joints on both sides of your body.
Want To Get More Involved With Patient Advocacy
The 50-State Network is the grassroots advocacy arm of CreakyJoints and the Global Healthy Living Foundation, comprised of patients with chronic illness who are trained as health care activists to proactively connect with local, state, and federal health policy stakeholders to share their perspectives and influence change. If you want to effect change and make health care more affordable and accessible to patients with chronic illness, learn more here.
Recommended Reading: What Foods Make Rheumatoid Arthritis Worse
What Are The Different Symptoms Between Osteoarthritis And Rheumatoid Arthritis
Osteoarthritis causes pain, stiffness, swelling, and decreased flexibility mainly in the knees, hands, and hips. Rheumatoid arthritis causes pain, stiffness, swelling, tenderness, and aching in the hands, wrists, and knees. It can also cause fatigue, weight loss, and weakness. One of the most significant differences in the symptoms of RA and OA is that rheumatoid arthritis causes morning stiffness that takes about an hour to wear off.