Diagnosing Rheumatoid Arthritis With Blood Tests
Rheumatoid arthritis blood tests are only one way to help doctors reach a diagnosis. If a patient is positive for any of these tests, they must also exhibit specific symptoms of rheumatoid arthritis. Doctors look at multiple other criteria besides blood test results when determining their diagnosis.
In some cases, patients can still be diagnosed with rheumatoid arthritis even if they dont test positive for the various types of antibodies found in rheumatoid arthritis blood tests.
Read more about diagnosing rheumatoid arthritis and the different types of rheumatoid arthritis here.
Answers From Our Doctors
Your doctor will talk with you about your symptoms and also do some tests to decide if you have RA. With that knowledge, there are some guidelines commonly used.
These criteria were developed by the American College of Rheumatology in 1988 and are still used to diagnose rheumatoid arthritis. Of these seven criteria, four are needed for a diagnosis. Criteria 1 through 4 must have been present for at least 6 weeks.
1.Morning stiffness lasting at least 1 hour before major improvement
2.Arthritis in three or more of the following joint areas on either side of the body: middle joint of the fingers, the knuckles , wrist, elbow, knee, ankle, or the joint between the toes and the foot
3.Arthritis in the hand joints: specifically in the wrist, the knuckles, or the middle joint of the fingers
4.Joint swelling of the same joint on both sides of the body or joint swelling on both sides of the body affecting the middle joint of the fingers, the knuckles, and/or the joint between the toes and the foot
5.Bumps that develop under the skin over pressure points or areas where bones protrude.
6.Positive RF test
7.X-ray changes that show decalcified bone or uneven patches of bone erosion around only the joints affected by rheumatoid arthritis. Thinning bones throughout the body unrelated to rheumatoid joints do not qualify.
What Does Ra Feel Like
- The usual symptoms of rheumatoid arthritis are stiff and painful joints, muscle pain, and fatigue.
- The experience of rheumatoid arthritis is different for each person.
- Some people have more severe pain than others.
- Most people with rheumatoid arthritis feel very stiff and achy in their joints, and frequently in their entire bodies, when they wake up in the morning.
- Joints may be swollen, and fatigue is very common.
- It is frequently difficult to perform daily activities that require use of the hands, such as opening a door or tying one’s shoes.
- Since fatigue is a common symptom of rheumatoid arthritis, it is important for people with rheumatoid arthritis to rest when necessary and get a good night’s sleep.
- Systemic inflammation is very draining for the body.
Don’t Miss: What Causes Arthritis Flare Up In Hands
Stiffness In The Joints
In addition to pain, this disease causes stiffness in the affected joints. You may have difficulty getting out of bed or walking in the morning because of stiff and painful ankles, knees, or feet. This stiffness is usually worse in the mornings and can last for 45 minutes or more.
RA can also trigger swelling in the affected joints. Long-term inflammation can cause you to feel physically exhausted.
What Are The Symptoms Of Rheumatoid Arthritis
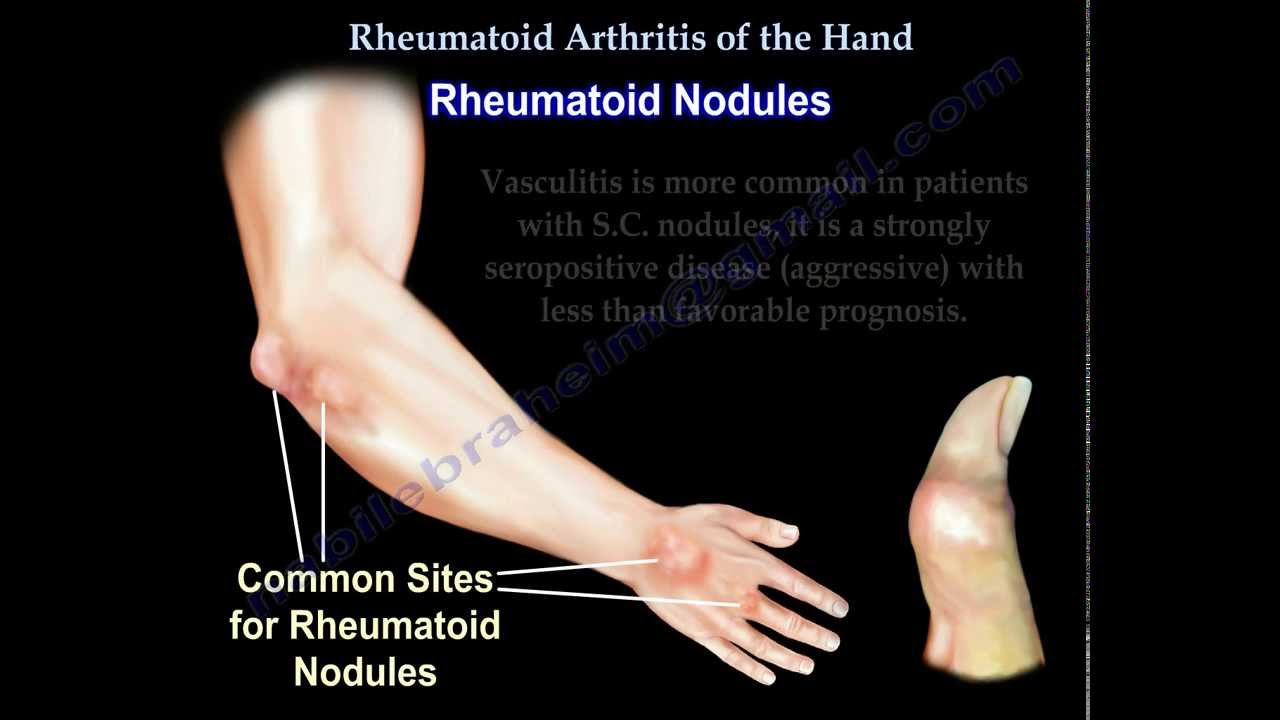
The symptoms of rheumatoid arthritis include the following:
- Stiffness, especially in the morning or after sitting for long periods
- Fatigue
Rheumatoid arthritis affects each person differently. In most people, joint symptoms may develop gradually over several years. In other people, rheumatoid arthritis may proceed rapidly. A few people may have rheumatoid arthritis for a limited period of time and then go into remission .
Cartilage normally acts as a shock absorber between the joints. Uncontrolled inflammation causes the destruction and wearing down of the cartilage, which leads to joint deformities. Eventually, the bone itself erodes, potentially leading to fusion of the joint . This process is aided by specific cells and substances of the immune system, which are produced in the joints but also circulate and cause symptoms throughout the body.
Don’t Miss: Rheumatoid Arthritis Leg Pain At Night
What To Expect During The Tests
You usually do not need to do anything before a blood test for RA, fasting is not required. Tell your healthcare provider if you are taking any prescription or over-the-counter medications that may affect your tests.
Wear a garment that allows access to your elbow area for the blood draw. Bring your identification. The healthcare professional drawing the blood will ensure your identification and label the blood draw sample tubes.
A tourniquet will be placed on your arm, the vein area sanitized, and a needle will be used to collect the blood into one or more vials.
After drawing the blood, the site will be bandaged. You should not have any side effects and usually do not need to take any precautions after the test.
These tests are sent to the lab rather than being done in the clinic as a rapid test. Your results will not be available immediately but will be reported to your healthcare provider in hours to a day or more.
Ra Blood Tests: What Lab Tests Show Rheumatoid Arthritis
To diagnose rheumatoid arthritis there is no one test that can on its own reach a diagnosis. Instead, there are a number of criteria that must be established in order to reach a rheumatoid arthritis diagnosis.
As part of the criteria for diagnosing rheumatoid arthritis, doctors will order multiple blood tests. These blood tests look for specific indicators that support the possibility that the patient could have rheumatoid arthritis.
Also Check: Can You Get A Rash With Rheumatoid Arthritis
Difference Between Osteoarthritis And Rheumatoid Arthritis
There are several different types of arthritis. Osteoarthritis and rheumatoid arthritis are two of the most common forms. Although the symptoms of these two types of arthritis can be similar, it’s very important to distinguish between them in order to determine the proper treatment.
At the University of Michigan Health System, our experienced rheumatologists will do appropriate tests to determine which type of arthritis you have. Then we will develop an effective treatment plan and will explain your options.
Osteoarthritis occurs when the smooth cartilage joint surface wears out. Osteoarthritis usually begins in an isolated joint.
Rheumatoid arthritis is an autoimmune disease, which means that the immune system malfunctions and attacks the body instead of intruders. In this case, it attacks the synovial membrane that encases and protects the joints. Rheumatoid arthritis often targets several joints at one time. The symptoms of rheumatoid arthritis include:
- the symmetrical nature of the disease ,
- fever
Diagnosing Ra In Outlier Patients
Some cases of RA may be different or more difficult to diagnose then others, and certain routine tests and exams might not be as helpful. These include patients with a very recent onset of disease, people whose RA is inactive, and those with seronegative RA.
In these situations, making an RA diagnosis may take more time, or more weight may be given to certain factors, but RA can still be accurately established.
In people with inactive RA, for example, a rheumatologist may rely less on CRP and ESR tests and more on RF and anti-CCP tests, as well as evidence of characteristic joint erosions on imaging, if the disease has been present for long enough to develop erosions.
Don’t Miss: How To Reduce Arthritis Swelling In Hands
Not All Patients With Early Polyarthritis Develop Persistent Disease
When a patient with inflammatory arthritis cannot definitely be labelled as having RA, it becomes important to decide whether the arthritis is likely to remit or to persist. Clearly, if spontaneous remission seems likely, the patient should be spared potentially toxic DMARD therapy. On the other hand, a patient with persistent inflammation should be started promptly on DMARDs since the condition may represent RA in evolution. From the Norfolk Arthritis Register there is evidence that an overwhelming majority of patients with persistent polyarthritis in due course come to satisfy diagnostic criteria for RA . Thus, since joint damage and functional loss occur early, most patients develop these irreversible changes before a definite diagnosis of RA can be made.
How can the clinician predict persistence of disease? Several research groups have tried to identify pointers in patients with early arthritis but their results are not easily combined because of heterogeneity in populations, predictive factors used and duration of follow-up. Among the predictive factors suggested, the most useful seems to be disease duration exceeding 12 weeks: a patient who has had inflammatory joint symptoms for this long is very unlikely to experience a spontaneous remission. Other features suggesting the unlikelihood of remission are positive tests for rheumatoid factor or cyclic citrullinated peptide antibodies and the presence of erosions on radiographs.
Measures To Reduce Bone Loss
Inflammatory conditions such as rheumatoid arthritis can cause bone loss, which can lead to osteoporosis. The use of prednisone further increases the risk of bone loss, especially in postmenopausal women.
You can do the following to help minimize the bone loss associated with steroid therapy:
- Use the lowest possible dose of glucocorticoids for the shortest possible time, when possible, to minimize bone loss.
- Get an adequate amount of calcium and vitamin D, either in the diet or by taking supplements.
- Use medications that can reduce bone loss, including that which is caused by glucocorticoids.
- Control rheumatoid arthritis itself with appropriate medications prescribed by your doctor.
Recommended Reading: What Rheumatoid Arthritis Feels Like
How Is Seronegative Rheumatoid Arthritis Diagnosed
Some patients still have RA but do not test positive for either anti-CCPs or RF they have seronegative RA.
Annals of the Rheumatic Diseases
Your doctor may also conduct a synovial biopsy, which involves removing a small piece of the tissue lining one of your joints.
RELATED: Psoriatic vs Rheumatoid Arthritis: Whats The Difference?
When To Seek Medical Advice

You should see your GP if you think you have symptoms of rheumatoid arthritis, so your GP can try to identify the underlying cause.
Diagnosing rheumatoid arthritis quickly is important because early treatment can help stop the condition getting worse and reduce the risk of further problems such as joint damage.
Read more about diagnosing rheumatoid arthritis.
Recommended Reading: Can You Get Rid Of Arthritis
Who Should Get Testing
Patients who experience inflammation, pain, or loss of mobility in joints should discuss testing for rheumatoid arthritis with their doctor, especially if symptoms occur in multiple joints or in matching joints on both sides of the body, such as both wrists. Other symptoms of rheumatoid arthritis include:
- Stiffness in the morning for 30 minutes or longer
- Fatigue
- Dry eyes and mouth
- Firm lumps beneath the skin
These symptoms are often due to something other than RA when they last less than six weeks. The longer a patient experiences symptoms, the more likely the symptoms are to be due to RA.
Diagnosing rheumatoid arthritis in its early stages can be challenging, as patients may experience few symptoms, but early diagnosis is important because early treatment may prevent joints from worsening or at least slow the process. When symptoms are present, they often differ from person to person and mimic the symptoms of other diseases. Testing is an important part of the process of determining whether symptoms are due to RA or another condition.
After receiving a diagnosis of RA, its important for patients to continue rheumatoid arthritis testing. Testing can assist doctors in assessing the severity of RA, as well as monitoring the efficacy of treatment, tracking disease progression, and detecting potentially serious side effects of treatment drugs.
What Are Complications Of Rheumatoid Arthritis
Common complications of rheumatoid arthritis include the following:
Overall, the rate of premature death is higher in people with rheumatoid arthritis than in the general population. The most common causes of premature death in people with rheumatoid arthritis are infection, vasculitis, and poor nutrition. Fortunately, the manifestations of severe, long-standing disease, such as nodules, vasculitis, and deforming are becoming less common with optimal treatments.
You May Like: Elevated Rheumatoid Levels
What Exactly Is Rheumatoid Arthritisand How Do You Know If You Have It
Rheumatoid arthritis is an autoimmune and inflammatory disease that mainly affects the body’s joints, according to the Centers for Disease Control and Prevention .
The condition, per the CDC, commonly affects the joints in the hands, wrists, and kneesand occurs when the lining of those joints becomes inflamed, damaging the joint tissue. That damage can eventually lead to long-lasting or chronic pain, unsteadiness, and deformity.
The symptoms of RAwhich can include pain, stiffness, tenderness, and swellingcan go through phases where they’re worse and better . But some symptoms of RA can mimic those of other conditionshere’s what to look out for, and how to know if it’s due to RA or something else.
What Are Rheumatoid Arthritis Symptoms
The following are common signs and symptoms of rheumatoid arthritis:
- Swollen, warm, and tender joints
- Joint stiffness
- Fever
- Loss of appetite
You also may experience symptoms in some non-joint areas, which is why you may not realize whats ailing you is rheumatoid arthritis. For example, this condition can affect bone marrow, nerve tissue, your skin, eyes, salivary glands, blood vessels, and some organs.
The good news is that rheumatoid arthritis symptoms can come and go they may flare and fade and even disappear. However, this condition can cause joint deformity over time.
Also Check: Best Remedy For Arthritis In Fingers
Distinguishing Between Osteoarthrosis & Rheumatoid Arthritis
There are several ways to distinguish between osteoarthritis and rheumatoid arthritis. The most common way to distinguish rheumatoid arthritis from other forms of arthritis is by using an X-Ray.
These two conditions can be easily diagnosed with a clear history, but X-ray, MRI and blood tests can be used to confirm the diagnosis. Deterioration of joints, lack of cartilage and spurs can be seen on a radiograph of a patient with osteoarthritis. ESR, CPR, anti-CPC can be increased in rheumatoid arthritis while there will be no changes in osteoarthritis.
How Ra Affects Feet
Rheumatoid arthritis is an autoimmune condition. When you have RA, your immune system tries to destroy the lining of your joints, called synovium. It also attacks the fluid in your joints, called synovial fluid. It does this because it mistakes these parts of your body for disease-causing invaders.
RA causes damage and inflammation that makes your joints swell and feel warm. The small joints, like those in the feet, are the most common targets of these attacks.
Eventually, long-term inflammation thickens the synovium. This causes cartilage and bone to wear away. In the feet and toes, the joints may become deformed. This leads to poor range of motion and considerable pain. Walking, standing, and even wearing shoes can become difficult.
Proper treatment may help reduce the damage and inflammation to your foot joints. It may also prevent or delay deformities and other problems.
You May Like: Remedy For Arthritis Pain In Hands
Diagnosis And Tests For Rheumatoid Arthritis
There is no definitive test for rheumatoid arthritis and other conditions can cause similar symptoms. Your GP will ask about your symptoms, check the movement of your joints and perform a physical examination.
If they think you have rheumatoid arthritis, theyll recommend a blood test and refer you to a rheumatologist .
A blood test will check for several different proteins that can indicate rheumatoid arthritis. Your blood test may measure:
- Anti-cyclic citrullinated peptide antibodies that attack healthy tissue in your body
- C-reactive protein levels a measure of inflammation
- Erythrocyte sedimentation rate a measure of inflammation
- Rheumatoid factors proteins produced by your immune system when it mistakenly attacks healthy tissue
- Your full blood count this can:
- Check if you have anaemia, which is common in people with rheumatoid arthritis
- Help rule out other conditions
- Indicate your general health
To identify the type of arthritis you have and monitor how the disease progresses over time, your rheumatologist may also take images of your joints, such as:
If you receive a diagnosis of rheumatoid arthritis, your rheumatologist may assess how you cope with everyday tasks.
You May Like: Is Banana Good For Rheumatoid Arthritis
What Does My Ra Treatment Look Like
My treatment will be overseen by a specialist in autoimmune diseases, known as a rheumatologist. A treatment plan can include specific medicine including disease-modifying anti-rheumatic drugs , pain management , proper nutrition, massage therapy, occupational and physical therapy, etc.
My rheumatologist needs to find the right medicine to help my RA. Please know finding the right medication and combination of treatments may take time.
Read Also: Arthritis And Skin Rash
What Are The Signs And Symptoms Of Ra
With RA, there are times when symptoms get worse, known as flares, and times when symptoms get better, known as remission.
Signs and symptoms of RA include:
- Pain or aching in more than one joint
- Stiffness in more than one joint
- Tenderness and swelling in more than one joint
- The same symptoms on both sides of the body
- Weight loss
A Compromised Immune System
The disease makes it hard to fight off viruses and infections. A simple cold could be the cause of a visit to the hospital for me. I need to be extra careful to sanitize my home frequently and practice proper self-hygiene. Large crowds of people can present problems because my immune system is low, and I run a high risk of catching a virus. I have to be careful when I plan my outings.
Recommended Reading: Reduce Arthritis Swelling In Fingers
When Do The Signs Of Ra Start
Rheumatoid arthritis affects 1.3 million people in the United States. It is 2.5 times more common in women. RA often affects people between the ages of 20 and 50, but young children and older adults can also have RA.
Younger adults and older adults, who make up a smaller number of the people RA, often have a different disease course than people in middle adulthood.