Psoriatic Arthritis By The Numbers
Psoriatic arthritis question and answer:
How many people have psoriatic arthritis? In the United States psoriasis occurs in about 2% of the population and equally among the sexes. In people diagnosed with psoriasis, about 5%to10% will go on to develop psoriatic arthritis.
When do individuals first begin noticing symptoms? Around 85% of individuals living with psoriatic arthritis have lived with psoriasis for years prior to the onset of arthritis. Symptoms of psoriatic arthritis typically occur between ages 30 and 50, with most cases starting between the fourth and fifth decade.
Does everyone with psoriasis get psoriatic arthritis? No. Studies have shown that anywhere from 5% to 30% of individuals living with psoriasis will go on to develop psoriatic arthritis. This wide discrepancy in incidence is due to variations in definitions and design from one clinical trial to another over time.
Are there different types of psoriatic arthritis? There are five types of psoriatic arthritis: symmetric , asymmetric , distal interphalangeal , spondylitis , and arthritis mutilans .
How many people are severely affected by psoriatic arthritis? About 20% of individuals living with psoriatic arthritis are characterized as suffering from severe psoriatic arthritis affecting four or more joints.
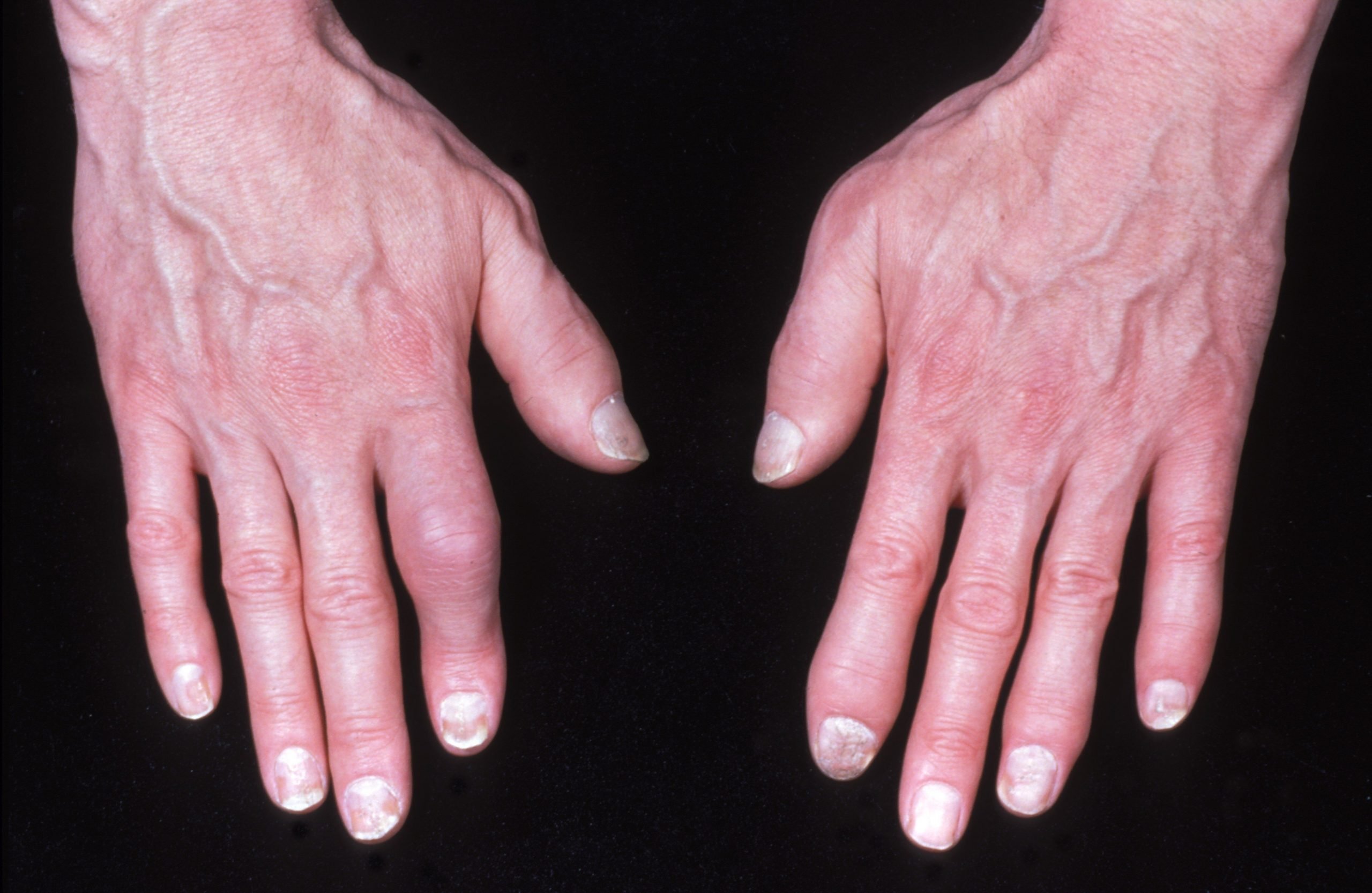
Does The Severity Of Skin Or Nail Psoriasis Matter
- Nail changes are found in 2 out of 5 individuals with psoriatic arthritis, compared with around half in those with psoriasis alone.
- Nail changes include pitting and discolouration of the nail due to abnormalities in the growth of tissue in the nailbed.
- The risk of developing psoriatic arthritis is greater in individuals with severe psoriasis, yet severe psoriatic arthritis may occur with minimal skin disease.
Your Energy Level Is Like A Bank Account
Psoriatic arthritis can cause extreme fatigue. For every task you complete, or plan to complete, you drain your daily energy bank. Putting on mascara or talking to a neighbor on the street costs you energy. And sometimes, even if its the first thing you do after waking up, a shower may be all it takes to put you right back in bed.
Its important to rest when you need to and not push yourself too hard, especially on days when your symptoms are particularly severe, says Joseph Markenson, MD, a rheumatologist at Hospital for Special Surgery in New York City. Its also important for the loved ones of those who have psoriatic arthritis to understand how draining the condition can be for example, people with psoriatic arthritis may have to cancel plans frequently or head home early.
Recommended Reading: How To Deal With Arthritis
Can Psoriatic Arthritis Affect Other Parts Of The Body
Having psoriatic arthritis can put you at risk of developing other conditions and complications around the body.
The chances of getting one of these are rare. But its worth knowing about them and talking to your doctor if you have any concerns.
Eyes
Seek urgent medical attention if one or both of your eyes are red and painful, particularly if you have a change in your vision. You could go to your GP, an eye hospital, or your local A& E department.
These symptoms could be caused by a condition called uveitis, which is also known as iritis. It involves inflammation at the front of the eye.
This can permanently damage your eyesight if left untreated.
Other symptoms are:
- blurred or cloudy vision
- sensitivity to light
- not being able to see things at the side of your field of vision known as a loss of peripheral vision
- small shapes moving across your field of vision.
These symptoms can come on suddenly, or gradually over a few days. It can affect one or both eyes. It can be treated effectively with steroids.
Heart
Psoriatic arthritis can put you at a slightly higher risk of having a heart condition. You can reduce your risk by:
- not smoking
- staying at a healthy weight
- exercising regularly
- eating a healthy diet, thats low in fat, sugar and salt
- not drinking too much alcohol.
These positive lifestyle choices can help to improve your arthritis and skin symptoms.
Talk to your doctor if you have any concerns about your heart health.
Crohns disease
Non-alcoholic fatty liver disease
Can I Get Financial Support
Many people worry about what happens if they cannot work or need financial help because of the effects of psoriatic arthritis. Fortunately for many, with good therapy and management the condition can be controlled and allow for a full and active working life. But if you do find that even for a short period of time you are likely to need help, visit the national government websites online. If it is easier, contact your local government or council office, where you should be directed to the appropriate resource and information.
Always consult your doctor or healthcare provider.
This article is adapted from the What is Psoriatic Arthritis? leaflet.
Other leaflets are also available to or order FREE from our shop and include the following:
- About Us
- Occupational Therapy and Psoriatic Arthritis
- Physiotherapy and Exercise: Psoriatic Arthritis
- Psoriasis and Sensitive Areas
- Psoriatic Arthritis – Did you know?
- Psoriatic Arthritis – When to treat?
- Psoriatic Fatigue
- Treatments for Psoriasis: An overview
- Treatments for Psoriatic Arthritis: An overview
- What is Psoriasis?
Also Check: Rheumatoid Arthritis In Neck And Shoulders
Progression Of Psoriasis And Psa
Most people who develop PSA will already have had psoriasis for around 10 years, but this is not always the case.
In 2016, researchers noted that among people who have both PsA and psoriasis, 70% experience skin changes before the symptoms of PsA appear, while 15% develop skin changes after having symptoms of PsA for about 2 years. The other 15% develop both at the same time.
Early diagnosis and treatment can help a person manage symptoms of psoriasis and PsA and reduce the risk of flares and future complications.
How PsA affects a person can vary depending on how severe the symptoms are and which part of the body they affect.
Here are some types of PsA a person might experience:
- Oligoarticular PsA affects up to four joints.
- Polyarticular PsA affects more than four joints and is more severe.
- Psoriatic spondylitis refers to inflammation of the spine. It affects 732% of people with PsA and can affect movement in the neck, the lower back, and where the pelvis meets the spine.
- Enthesitis is inflammation that affects the place where the tendons or ligaments meet the bone. Around half of those with PsA will experience enthesitis.
- Dactylitis causes swelling of a finger or toe due to inflammation in and around the small joints. Around 40% of people with PsA will experience it.
- Arthritis mutilans is a severe and uncommon type of PsA that develops in around 5% of those with the condition. Severe inflammation can cause joint damage and bone loss.
Spondylitis With Or Without Sacroiliitis
This occurs in approximately 5% of patients with psoriatic arthritis and has a male predominance.
Clinical evidence of spondylitis and/or sacroiliitis can occur in conjunction with other subgroups of psoriatic arthritis.
Spondylitis may occur without radiologic evidence of sacroiliitis, which frequently tends to be asymmetrical, or sacroiliitis may appear radiologically without the classic symptoms of morning stiffness in the lower back. Thus, the correlation between the symptoms and radiologic signs of sacroiliitis can be poor.
Vertebral involvement differs from that observed in ankylosing spondylitis. Vertebrae are affected asymmetrically, and the atlantoaxial joint may be involved with erosion of the odontoid and subluxation . Therapy may limit subluxation-associated disability.
Unusual radiologic features may be present, such as nonmarginal asymmetrical syndesmophytes , paravertebral ossification, and, less commonly, vertebral fusion with disk calcification.
Also Check: What Is The Rheumatoid Arthritis Blood Test
Who Develops Psoriatic Arthritis
About 1 person in 10 with psoriasis develops psoriatic arthritis. About 2 in 100 people develop psoriasis at some stage in their lives.
In most cases, the arthritis develops after the psoriasis – most commonly within 10 years after the psoriasis first develops. However, in some cases the arthritis develops much later. In a small number of cases the arthritis develops first, sometimes months or even years before the psoriasis develops. Men and women are equally affected.
Psoriasis most commonly first occurs between the ages of 15 and 25 and psoriatic arthritis most commonly develops between the ages of 25 and 50. However, both psoriasis and psoriatic arthritis can occur at any age, including in childhood.
Note: people with psoriasis also have the same chance as everyone else of developing other types of arthritis such as rheumatoid arthritis and osteoarthritis. Psoriatic arthritis is different, and is a particular type of arthritis that occurs only in some people with psoriasis.
How Can Psoriatic Arthritis Patients Manage Their Psoriasis
Psoriasis can affect your ability to carry out daily activities due to joint pain, swelling and other symptoms. While it cannot be cured, certain things help control the condition, which includes:
Do not stop your treatment unless advised
- As advised by your doctor, continue taking your medication despite a dramatic relief in symptoms. A disease-free period does not mean that your psoriatic arthritis is cured. Failing to keep up with your treatment could lead to a recurrence of the previous signs and symptoms within a few months.
Maintain healthy body weight
- Weight gain can put stress on your knee joints, while excess fat accumulation can aggravate inflammation in the body. Maintaining an ideal body weight can prevent psoriasis from worsening and decrease your risk of other conditions, such as heart disease and fatty liver.
Manage your pain
- Massages, occupational therapy and physiotherapy can help relieve pain and stiffness, as well as restore joint mobility.
- Orthotic devices, such as braces and splints, can help you manage your daily activities with comfort and ease.
Manage your stress
Know your triggers
- Maintain a diary by writing which activities or foods trigger your psoriasis flares or worsen your joint pain and swelling. Check if avoiding those foods or activities helps improve your condition. You should also inform your doctor about them.
Educate yourself
Don’t Miss: How To Ease Arthritis Pain In Fingers
Infection Rates In Psoriatic Arthritis Patients On Biologics Have Decreased According To National Data
by American College of Rheumatology
New research presented this week at ACR Convergence, the American College of Rheumatology’s annual meeting, shows significant decreases in infections among people with psoriatic arthritis over the years 2012-2017.
Psoriatic arthritis is a type of inflammatory arthritis that occurs in some patients with psoriasis. This particular arthritis can affect any joint in the body, and symptoms vary from person to person. Persistent inflammation from psoriatic arthritis can lead to joint damage.
Biologic therapies now available to treat psoriatic arthritis can help control disease activity and prevent damage, but these medications increase infection risk. Since use of biologics to treat PsA has increased in recent years, researchers conducted this study to find out if infections had increased among these patients. Researchers looked at national trends in serious infections in people with PsA from 2012 to 2017 across the U.S using the national inpatient sample.
“While the National Inpatient Sample does not have information on individual treatment for patients in the study, the data show a decrease in hospital discharges for sepsis, skin and soft-tissue infections, and UTI over the past several years. This information may help guide patients to make decisions regarding the management of their arthritis while understanding their infection risk,” says Dr. Murugesan.
Explore further
What Is Cdc Doing About Psoriasis
In 2010, CDC worked with experts in psoriasis, psoriatic arthritis, and public health to develop a public health perspective that considers how these conditions affect the entire population. The resulting report is Developing and Addressing the Public Health Agenda for Psoriasis and Psoriatic Arthritis pdf icon. You can read a short article about the agendaexternal icon in The American Journal of Preventive Medicine.
CDCs National Health and Nutrition Examination Survey , an intermittent source of national psoriasis data, has included questions about psoriasis as late as the 2013-2014 cycle. A recent analysis of NHANES data estimates that 7.4 million adults had psoriasis in 2013external icon.
- Psoriasis causes patches of thick red skin and silvery scales. Patches are typically found on the elbows, knees, scalp, lower back, face, palms, and soles of feet, but can affect other places . The most common type of psoriasis is called plaque psoriasis.
- Psoriatic arthritis is an inflammatory type of arthritis that eventually occurs in 10% to 20% of people with psoriasis. It is different from more common types of arthritis and is thought to be related to the underlying problem of psoriasis.
- Psoriasis and psoriatic arthritis are sometimes considered together as psoriatic disease.
Who is at risk for psoriasis?
Anyone can get psoriasis. It occurs mostly in adults, but children can also get it. Men and women seem to have equal risk.
Can I get psoriasis from someone who has it?
Read Also: Are There Tests For Arthritis
What Are The Symptoms Of Psoriatic Arthritis
Thepsoriasis symptoms may start before or after the arthritis. Psoriasis causes red, scalyrashes and thick, pitted fingernails. About 3 in 20 to 3 in 10 people with psoriasismay develop psoriatic arthritis. Symptoms of psoriatic arthritis may include:
- Inflamed, swollen, and painful joints, often in the fingers and toes
- Deformed joints from chronic inflammation
The symptoms of psoriatic arthritis can look like other health conditions. Make sure to see your healthcare provider for a diagnosis.
National Trends In Hospitalizations For Serious Infections In People With Psoriatic Arthritis Using The National Inpatient Sample 2012 2017
Vagishwari Murugesan1, Eleni Pilitsi2, Gabriela Rabasa3 and Maureen Dubreuil4, 1Boston University Medical Center, Boston, MA, 2Boston Medical Center, Boston, MA, 3Boston University, Boston, MA, 4Boston University School of Medicine/ VA Boston, Boston, MA
Session Type: Poster Session D
Session Time: 8:30AM-10:30AM
Background/Purpose: Given that uptake of biologic therapies has increased over recent years, we sought to investigate the national trends in serious infections in patients with psoriatic arthritis from the years 2012 2017 in the United States.
Methods: The NIS approximates a 20% stratified sample of all discharges from U.S. community hospitals, excluding rehabilitation and long-term acute care hospitals, with approximately 7 million discharge records. We examined data from 20122017 and identified any discharge diagnosis for PsA with a principal or secondary diagnosis of pneumonia, sepsis, urinary tract infection and/or skin and soft tissue infections using ICD-9 & ICD 10 codes. We standardized results for years 2012-2017 to match age distributions in the US population in the year 2012. We then tested for a trend over years 2012-2017 using chi squared tests, evaluating for an increase in serious infections over the years.
Disclosures: V. MurugesanE. PilitsiG. RabasaM. Dubreuil
To cite this abstract in AMA style:
Arthritis Rheumatol.
Don’t Miss: Best Pain Reliever For Rheumatoid Arthritis
Causes Of Psoriatic Arthritis
Almost 1 in 3 people with psoriasis also have psoriatic arthritis.
It tends to develop 5 to 10 years after psoriasis is diagnosed, although some people may have problems with their joints before they notice any skin-related symptoms.
Like psoriasis, psoriatic arthritis is thought to happen as a result of the immune system mistakenly attacking healthy tissue.
But it’s not clear why some people with psoriasis develop psoriatic arthritis and others do not.
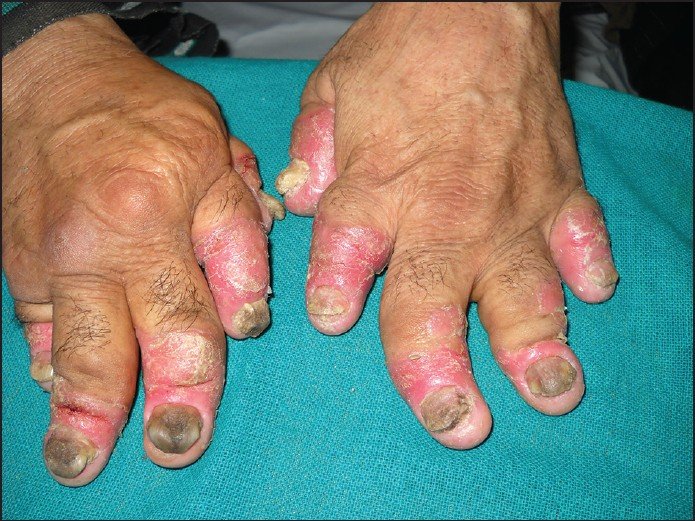
What Is Arthritis Mutilans
The most severe form of PsA is called arthritis mutilans. Approximately 5% of people with PsA have arthritis mutilans. Arthritis mutilans is characterized by digital shortening of the fingers or toes due to severe bone destruction. In arthritis mutilans, the bones in the fingers or toes degrade and begin telescoping into each other, sometimes referred to as a pencil-in-cup deformity, as it resembles a pencil in a cup on x-ray images. It may also be called opera glass finger. Arthritis mutilans is often associated with PsA that affects many joints throughout the body , as well as symmetrical distribution , inflammation between the spine and the pelvis , and long disease duration. Arthritis mutilans causes severe deformity and loss of function for the person with PsA.6
Also Check: What Can I Take Over The Counter For Arthritis Pain
What Are The Symptoms
Psoriatic arthritis can affect any joint in the body and symptoms can vary from person to person. It can develop slowly with mild symptoms, or come on quickly and be severe. The most common symptoms are:
- pain, swelling and stiffness in one or more joints
- pain and stiffness in the buttocks, lower back or neck
- pain in tendons, such as at the back of the heel or sole of the foot
- changes in nails, such as thickening, colour change or separation from the skin
- pain and redness in the eyes.
Most Rheumatologists And Public Health Experts Want People Living With Rheumatic Diseases Like Psoriatic Arthritis To Get The Vaccine As Soon As They Can
Learn more about our FREE COVID-19 Patient Support Program for chronic illness patients and their loved ones.
If you live with psoriatic arthritis, an inflammatory and autoimmune form of arthritis that affects about 30 percent of people with psoriasis, you may understandably have many questions and concerns about getting the COVID-19 vaccine.
Heres the bottom line: Especially if you have an autoimmune condition like psoriatic arthritis, most rheumatologists and public health experts recommend you get vaccinated against COVID-19. In its COVID-19 Task Force Guidance, the National Psoriasis Foundation says that in most cases, patients with psoriatic disease who dont have contraindications should take the first authorized COVID-19 vaccine that becomes available to them.
Similarly, the American College of Rheumatology states that autoimmune and inflammatory rheumatic disease patients , which includes people with psoriatic arthritis, should receive the vaccine when theyre eligible.
The ACR also states that disease activity and severity should not delay you from getting the vaccine except in extreme cases . That said, vaccination would ideally take place in the setting of well-controlled disease.
Heres everything you need to know about getting the COVID-19 vaccine if you have psoriatic arthritis.
Also Check: How To Deal With Arthritis