Can Psoriatic Arthritis Affect Children Too
As many as 12,000 children in the UK are affected by arthritis. It is known as juvenile chronic arthritis , of which there are three main types, stills disease, polyarticular juvenile chronic arthritis and polyarticular onset juvenile chronic arthritis. Psoriatic arthritis is a minor subset of JCA and is uncommon.
Other Medications For Pain
When the pain of PsA is severe or when it does not go away with traditional PsA treatments, you may want to talk to your health care provider about medication that helps reduce your sensitivity to pain.
Prescription pain medications such as Gabapentin and Pregabalin are used to treat neurological pain. Certain anti-depressants called noradrenergic and specific serotonergics can reduce your sensitivity to pain as well. Capsaicin, a compound found in chili peppers, has a numbing effect on pain receptors. Applying a local anesthetic like prilocaine can help minimize the initial burning sensation of capsaicin.
Blend Quick Meals That Are Easy To Eat
If you have a blender, smoothies are an easy catch-all for ingredients that might be tricky to incorporate into everyday meals. For example, its easy to sprinkle some ginger, turmeric, or chia seeds and flaxseeds into a liquid breakfast or a snack. Add leafy greens for a boost of vitamins and minerals.
For those with psoriasis of the lips, gums, or mouth tissue, drinking from a straw may be less painful than chewing. Although you shouldnt rely on a liquid diet to manage your symptoms, incorporating smoothies into your eating plan could help make life easier during a flare-up.
Blenders that double as food processors are a great tool for transitioning toward a Mediterranean diet. The Mediterranean diet is popular in the medical community for its proven benefits for many inflammatory conditions, including psoriasis. You can use a food processor to make an olive tapenade or blend your own hummus with extra virgin olive oil to boost your intake of monounsaturated fatty acids. For monounsaturated fat with a Mexican twist, guacamole is also easy to prepare in the food processor. Add lemon to keep it from browning.
Read Also: What’s The Difference Between Arthritis And Osteoarthritis
Risks And Side Effects
While coffee in moderation has some health benefits, it can cause unwanted side effects and risks when consumed in excess. Caffeine intake over 400 milligrams per day could lead to:
- Elevated heart rate
- Increased risk for some diseases
- Caffeine withdrawal
In addition, adding creamer, sugar, or other sweeteners increases health risks. For example, added calories and sugar could cause excess weight and increase your risk of developing diabetes.
Trigger: You Have High Stress Levels
Stress can trigger psoriatic arthritis flares, says Dr. Bose those skin and joint exacerbations can, in turn, trigger more stress. Keeping calm is easier said than done, but there are some stress management methods that PsA patients and psychologists find helpful, including resting, exercising, and asking for help.
Of course, for some people, hearing that stress is a psoriatic arthritis trigger may lead to feelings of more stress, creating a vicious cycle. But for others, knowing about this link may provide the permission you need to prioritize self-care however you practice it as part of your disease management toolkit.
You May Like: Does Arthritis Make You Swell
Treatments For The Arthritis
Non-steroidal anti-inflammatory drugs
NSAIDs, or non-steroidal anti-inflammatory drugs, can reduce pain, but they might not be enough to treat symptoms of psoriatic arthritis for everyone.
Some people find that NSAIDs work well at first but become less effective after afew weeks. If this happens, itmight help to try a different NSAID.
There are about 20 different NSAIDs available, including ibuprofen, etoricoxib, etodolac and naproxen.
Like all drugs, NSAIDs can have side effects. Your doctor will reduce the risk ofthese, by prescribing the lowest effective dose for the shortest possible period of time.
NSAIDs can sometimes cause digestive problems, such as stomach upsets, indigestion or damage to the lining of the stomach. You may also be prescribed a drug called a proton pump inhibitor , such as omeprazole or lansoprazole, to help protect the stomach.
For some people, NSAIDs can increase the risk of heart attacks or strokes. Although this increased risk is small, your doctor will be cautious about prescribing NSAIDs ifthere are other factors that may increase your overall risk, for example, smoking, circulation problems, high blood pressure, high cholesterol, or diabetes.
Some people have found that taking NSAIDs made their psoriasis worse. Tell your doctor if this happens to you.
Steroid treatment
Steroid injections into a joint can reduce pain and swelling, but the effects do wear off after a few months.
Disease-modifying anti-rheumatic drugs
Oral Or Injected Drugs
There are a variety of drugs that target skin cell production or your immune system. These include:
Corticosteroids
These medications mimic cortisol, a naturally occurring anti-inflammatory hormone produced by your body. These are normally taken by mouth and can help reduce inflammation. Injected forms can provide temporary inflammation relief.
Long-term use can result in facial swelling and weight gain. It may also increase your risk for osteoporosis.
Disease-modifying antirheumatic drugs
These medications suppress the chemicals in your body that cause inflammation. This can help reduce prevent joint damage. DMARDs are typically taken by mouth but can also be injected.
Biologics
These medications can prevent inflammation on a cellular level. Biologics are typically injected. The main types of biologics are anti-tumor necrosis factor-alpha drugs, abatacept, and ustekinumab. Each blocks different proteins within the body.
Your risk for infection may increase while taking biologics since they work by suppressing your immune system.
Read Also: Are Peanuts Good For Arthritis
How Can I Find The Appropriate Care I Need
Initially your GP is the first point of contact, who then should refer you on to a dermatologist/rheumatologist, if this is not already the case. If you are not happy with the advice you receive, remember you are always entitled to seek a second opinion. Remember, If you are seeing a dermatologists for your psoriasis and a rheumatologists for your arthritis make sure each is aware of this, so they can liaise and provide you with appropriate care for both conditons.
Misdiagnosis Is A Chronic Problem
Psoriatic arthritis shares some symptoms with other conditions, such as rheumatoid arthritis, osteoarthritis, fibromyalgia, lupus, and gout. This can make getting an accurate diagnosis difficult.
In a study published in June 2018 in the British Medical Journal, investigators found that 96 percent of people who were diagnosed with psoriatic arthritis received at least one prior misdiagnosis.
Recommended Reading: What Foods Not To Eat With Rheumatoid Arthritis
Spinal Arthritis May Contribute To Other Issues In The Spine
Spinal arthritis may cause bone spurs overgrowths on the edges of the bones. In the spine, bone spurs particularly affect facet joints, making them grow larger. This condition is called facet joint hypertrophy. Although bone spurs on their own are not harmful, they may narrow the passages for the spinal cord and the nerves exiting the spine. This may lead to two painful conditions:
-
Spinal stenosis compression of the spinal cord inside the spinal canal
-
Radiculopathy pinching of the peripheral nerves as they exit the spine
Ankylosing spondylitis may also cause additional problems such as:
-
Stress fractures in places where new bone has formed
-
Collapsed vertebrae
-
A spinal deformity called kyphosis
Living With Psoriatic Arthritis
There is no cure for psoriatic arthritis. But you can reduce your symptoms by stickingto your treatment plan. Manage pain with medicine, acupuncture, and meditation. Getenough exercise. Good exercises include yoga, swimming, walking, and bicycling. Workwith a physical or occupational therapist. He or she can suggest devices to help you withyour daily tasks.
Read Also: Is Tens Unit Good For Arthritis
What Is Psoriatic Arthritis
Psoriatic arthritis primarily affects people with psoriasis, an inflammatory condition in which skin cells first build up quickly and then turn to scales. The scales are usually whitish-silver before they turn into thick, red patches. Most people with PsA are diagnosed with psoriasis first, but it’s possible to have joint symptoms before skin lesions occur.
Psoriatic arthritis often appears in people when they are between the ages of 30 and 50 and about 10 years after they develop psoriasis. However, some people develop PsA without ever developing or noticing psoriasis.
When severe, PsA can affect the fingers, toes, and spine. Both psoriasis and PsA are known for flare-upsperiods of high activityand periods of remission, where symptoms are mild or mostly absent.
Take Pain Medications For Psoriatic Arthritis
Over-the-counter pain medications such as ibuprofen and naproxen are often used to manage pain in psoriatic arthritis. If those don’t provide enough relief, John M. Davis, III, MD, a rheumatologist at the Mayo Clinic in Rochester, Minnesota, also recommends trying non-narcotic prescription medications, which change the way the brain’s pain center processes certain proteins that trigger pain. Although these drugs aren’t narcotics, side effects can include stomach upset and bad dreams.
Other medications to treat psoriatic arthritis include traditional disease-modifying anti-rheumatic drugs and biologic therapies, which can help ease pain and slow joint damage. Always follow your treatment plan as prescribed and talk to your doctor before taking a pain medication.
Also Check: What Medications Treat Rheumatoid Arthritis
Who Is At Risk For Psoriatic Arthritis
Psoriasis affects 2-3 percent of the population or approximately 7 million people in the U.S. and up to 30% of these people can develop psoriatic arthritis. Psoriatic arthritis occurs most commonly in adults between the ages of 35 and 55 however, it can develop at any age. Psoriatic arthritis affects men and women equally.
It is possible to develop psoriatic arthritis with only a family history of psoriasis and while less common, psoriatic arthritis can occur before psoriasis appears. Children of parents with psoriasis are three times more likely to have psoriasis and are at greater risk for developing psoriatic arthritis. The most typical age of juvenile onset is 9-11 years of age.
The Effects Of Psoriatic Arthritis On The Body
PsA is an autoimmune disorder that causes the immune system to attack healthy parts of the body, mostly the skin and the joints.
This causes pain, stiffness, and swelling in the joints, either singly or throughout the body. Early treatment is essential to avoid long-term joint and tissue deterioration.
Psoriatic arthritis usually develops within 10 years of developing psoriasis. Skin psoriasis causes flare-ups of red, patchy skin that can occur anywhere on the body.
According to the National Psoriasis Foundation, about 30 percent of people with psoriasis eventually develop PsA.
In some cases, PsA is diagnosed before you have skin psoriasis because the arthritic symptoms might be more noticeable.
Its also possible to develop PsA without having psoriasis, especially if you have a family history of psoriasis. Both skin psoriasis and inflammatory types of arthritis are considered autoimmune disorders.
PsA is a chronic, or long-term, condition. Anyone can get it, but its most common between ages 30 and 50 years. Since theres no cure, treatment is aimed at managing symptoms and preventing permanent joint damage.
Research theorizes that genetics play a part in the development of psoriatic arthritis. Scientists are trying to find out which genes are involved. Identifying the genes may allow the development of gene therapy treatment.
Also Check: Is My Hip Pain Arthritis
Limit Dairy Products If Necessary
Some people with psoriatic arthritis may experience worsened symptoms after consuming dairy products, said Dr. Jhin. “There’s always been talk about milk being a source of inflammation. I would tell people with any type of inflammatory disease to limit dairy. With any inflammation, dairy can be a source of aggravated inflammation.”
But Dr. Jhin noted that dairy is good for you in other ways . So, it’s fine to keep eating dairy if you can tolerate it without experiencing worsened symptoms.
Four Main Types Of Psoriatic Arthritis
There are 78 major joints in the body and psoriatic arthritis can affect any one of these. Usually, however, certain joints are more likely to be affected . Different patterns are found. Sometimes just one or two joints are a problem but often several joints, both large and small and on both sides of the body, are involved. About a third of people with psoriatic arthritis also have spondylitis which can result in a painful, stiff back or neck. Psoriasis can affect the nails with pitting, discolouration and thickening and this may be associated with inflammation in the joints at the end of the finger or toe. Another way in which psoriatic arthritis can be recognized is the finding of a sausage-like swelling of a finger or toe, called dactylitis. This is caused by inflammation occurring simultaneously in joints and tendons, painful heels and other bony prominence can also occur and this is caused by inflammation where gristle attaches to bone.
Read Also: Is Cheese Good For Arthritis
Foods To Avoid With Psoriatic Arthritis
Psoriatic arthritis is one the most common types of arthritis and nearly 30% of people with psoriasis will develop psoriatic arthritis in their lifetime. It affects both men and women, usually between ages 30 to 50. Fortunately, there are healthy ways to reduce the stiffness and joint pain that come along with psoriatic arthritis. Making changes to your diet is a smart first step and can help you eliminate foods that trigger flare-ups and cause inflammation.
Researchers have found that cutting back on sugar, dairy, gluten, and certain fats can reduce symptoms of psoriatic arthritis. Eating a healthy diet filled with lean meats, fruits and vegetables can have a positive impact and help you lose weight to ease pressure on your joints. No matter what diet you choose, its important to watch portion size and eat a wide range of nutrients.
If you want to incorporate a psoriasis arthritis diet into your daily routine, start by talking to your doctor. Eliminate trigger foods to see how they affect your symptoms. Then you and your doctor can determine what type of diet will be best for your body moving forward.
Read Also: How Do I Know If I Have Hip Arthritis
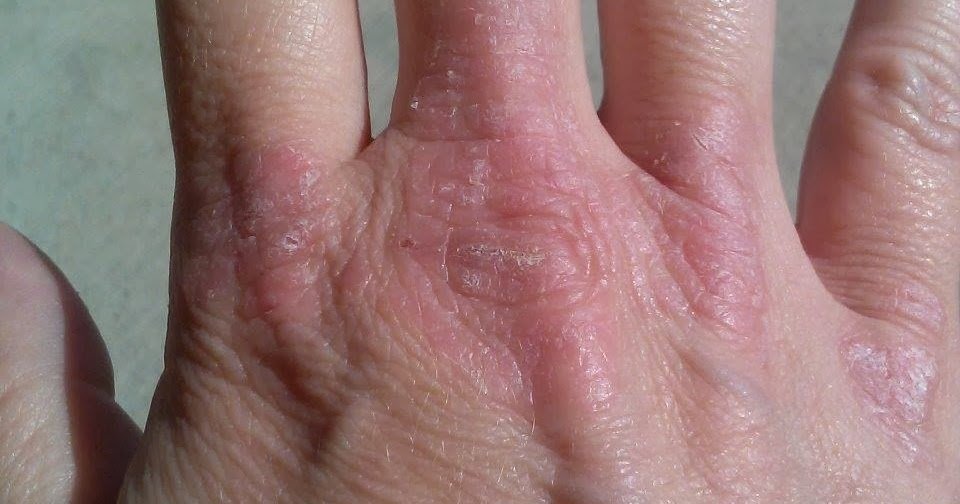
Nail Changes: A Sign Of Psoriasis
Up to 80 percent of people living with psoriatic arthritis experience some type of nail issue, according to a study published in 2017 in the journal Reumatologia. Evidence suggests that nail psoriasis is a strong predictor of joint disease and may show up years before arthritis symptoms.
The study notes that pitting is the most common sign of nail psoriasis. Pitting looks like superficial depressions in the nail.
Another type of nail change that can occur is known as onycholysis, or a separating of the nail from the nail bed.
Many people find the appearance of nail symptoms psychologically distressing, says Dr. Gupta. Extensive cases may confer significant morbidity and functional impairments. Therefore, managing nail psoriasis is an integral part of psoriatic arthritis therapy.
Treatment options for nail psoriasis include topical ointments as well as systemic therapies.
Don’t Miss: What Kind Of Doctor To See For Arthritis
Spinal Arthritis: What You Need To Know
-
Osteoarthritis is the most common type of arthritis to affect the spine.
-
Arthritis can occur anywhere along the spine, but is more frequent in the lower back and neck.
-
Pain and stiffness are the most common symptoms of spinal arthritis.
-
Causes of spinal arthritis are still largely unknown except for osteoarthritis, which is typically a result of wear and tear.
-
Spinal arthritis treatment may include pain medications, steroid injections, physical therapy and surgery in severe cases.
Lifestyle Remedies For Psoriatic Arthritis
Making lifestyle changes can prevent and control flares as well as alleviate the muscle weakness and joint stiffness associated with psoriatic arthritis. Lifestyle remedies include the following:
- Use assistive devices during flare-ups. Immobilize certain body parts with the use of splints, braces, orthotics, crutches, or walkers so they can rest.
- Exercise can keep joints flexible, strengthen your muscles, and boost your overall health. Walking, biking, swimming, and yoga are just a few exercises that wont stress your joints.
- Protect your joints by modifying how you perform daily tasks. For example, use a jar opener to remove a lid.
- Apply hot and cold packs. The heat and cold can help lessen the pain sensation.
- Keep your weight at a healthy level. Your joints will have less strain on them as a result.
Don’t Miss: Does Arthritis Pain Move Around The Body
Typical Symptoms For Hips & Psoriatic Arthritis
Symptoms of PsA in the hips include:
- Pain in the hip joint, which may include pain in the groin, outer thigh, or buttocks
- Pain or stiffness, especially first thing in the morning or after a period of rest
- Difficulty walking, or walking with a limp
- Stiffness or reduced range of motion2,3
- Sexual intercourse may be painful, especially for women with PsA that affects the hips.7
Understanding Remission And Minimal Disease Activity
Psoriatic arthritis disease progression is not inevitable. When your PsA is treated with medications that reduce immune system overactivity, you can reduce your disease activity to a point that its no longer causing significant symptoms or increasing the risk of long-term health issues.
In general, going into remission means that you are no longer showing signs of active disease. Decades ago, remission wasnt conceivable for most people with psoriatic arthritis, but thanks to a proliferation in medication treatment options, getting to remission is a possibility for PsA patients today.
However, going into remission does not mean that you will stay there indefinitely. It is common for PsA symptoms to wax and wane. Even if youve been in remission for a long time and your pain starts coming back and you start flaring more, you may need to change your medication for better control, says Dr. Haberman.
You may also hear the phrase minimal disease activity in conjunction with psoriatic arthritis and remission.
Doctors dont have a clear definition of what it means to be in remission in PsA, but they have defined something called minimal disease activity as a treatment target. This is what your doctor may use to determine whether your PsA disease activity is low enough that you have few symptoms and a low risk of long-term damage.
People are considered to be in minimal disease activity when their scores on five out of these seven criteria are low enough.
Read Also: What Can I Take For Arthritis In My Neck