Psoriatic Arthritis Nail Care Tips
Treating psoriasis and psoriatic arthritis can help reduce the uncomfortable symptoms of nail psoriasis. The following tips can also help keep your nails healthy and pain-free.
- Avoid using nail polish or polish removers with harsh chemicals, as they may make your nails more brittle. Products labeled 8-free or 10-free are made without harsh ingredients.
- Dont pick at your nails or cuticles.
- Keep your nails trimmed short. Long nails are more likely to catch on things and crack or peel back, says Dr. Husni.
- Protect your hands. Wear gloves when doing dishes or yardwork to keep them dry and protected from damage.
Managing the symptoms of psoriatic arthritis can be a handful. With some TLC, you can keep those hands healthy. Toes, too.
Other Conditions That Can Cause Hand Pain Include:
Carpal tunnel syndrome
Rheumatoid arthritis can raise your risk of this condition, but many other factors can contribute as well, including anatomy of your wrist, nerve-damaging diseases and possibly repetitive hand motions. Its tricky because you could have carpal tunnel syndrome that is related to RA or not at all related to RA.
Also Check: What Medication Is Used For Arthritis
Treatment Options For Nail Psoriasis
To treat psoriatic arthritis nail changes, your doctor may prescribe topical creams or ointments to rub on your nails. Systemic medications to treat psoriasis or psoriatic arthritis can also help a lot. These medications might include:
- Nonsteroidal anti-inflammatory medications to reduce inflammation.
- Disease-modifying antirheumatic drugs to block inflammation.
- Biologics, a special class of DMARDs, which target specific parts of your immune system that drive inflammation in psoriatic arthritis.
Also Check: Are Muscle Relaxers Good For Arthritis
When Do Nail Symptoms Occur
PsA may not present the same way for every person, but it typically always develops in stages.
In its preclinical stage, psoriatic inflammation may only cause fatigue, heel pain, and joint pain. At this time, doctors may not yet be able to identify the condition as PsA.
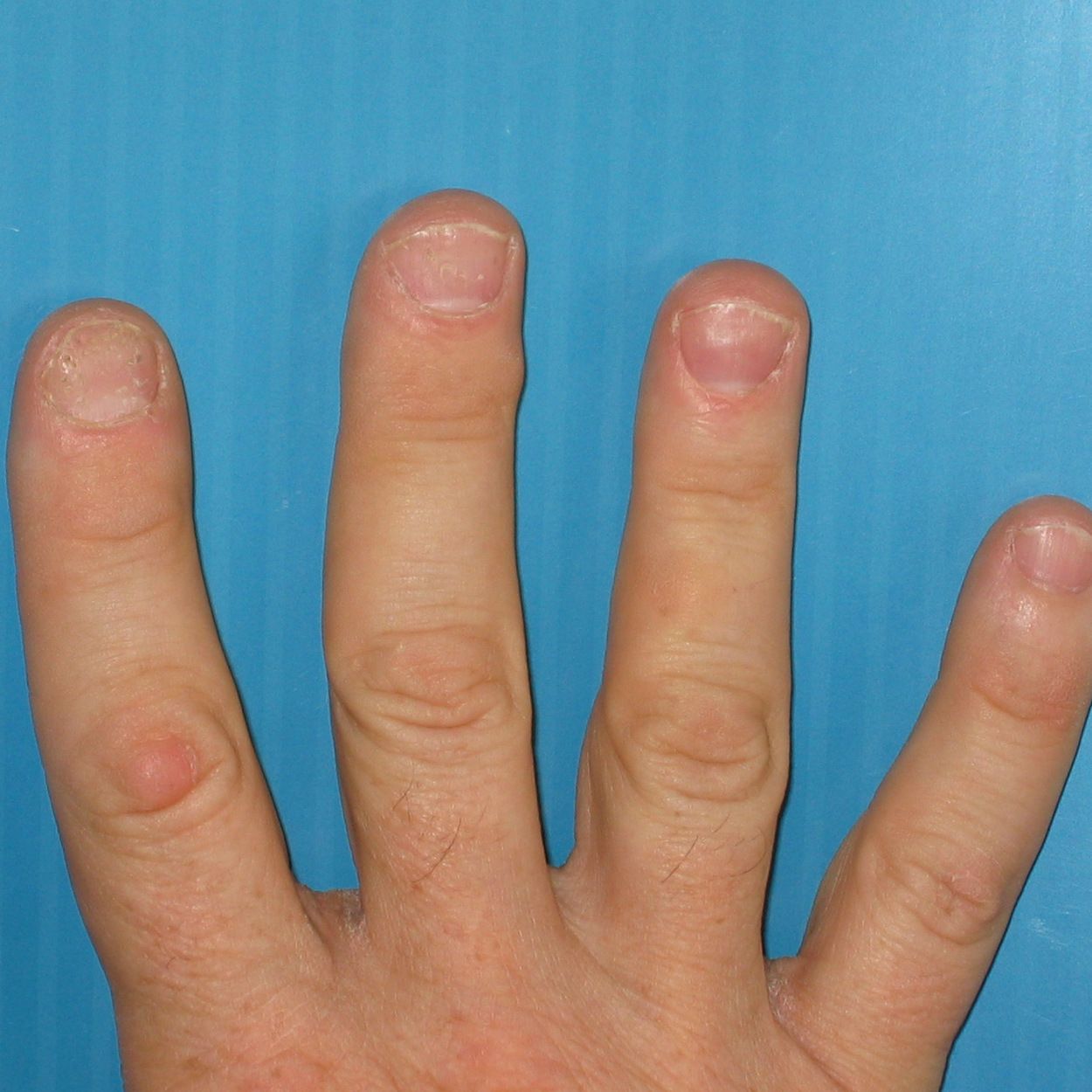
Once the condition progresses a little, nail changes can begin to occur. These include pitting, discoloration, softness, holes, and dactylitis, or the swelling of the toe or finger. This may still be an early phase of the condition.
As the condition progresses even further, these and other symptoms may get worse and progress to severe damage to the bones.
Ankylosing Spondylitis Vs Rheumatoid Arthritis
In Greek, ankylos means stiffening of a joint, means vertebra, and itis means inflammation. Ankylosing spondylitis is a form of inflammatory arthritis that primarily affects the spine, but it can affect other joints too.
How is it similar to RA? People with ankylosing spondylitis often report morning pain and stiffness. They may also feel feverish and fatigued. Affected joints can feel swollen and tender.
How is it different? Ankylosing spondylitis usually produces symptoms in the low back, hips, and/or shoulders first. In contrast, rheumatoid arthritis usually first affects smaller joints, such as those in the hands and feet . Some people with ankylosing spondylitis experience eye symptoms, including redness, light sensitivity, and blurred vision.
Both diseases can affect anyone however, RA is most frequently diagnosed in women ages 30 to 60 and ankylosing spondylitis is more frequently diagnosed in males under the age of 40.1
Don’t Miss: What Are The Signs And Symptoms Of Rheumatoid Arthritis
What Vitamin Are You Lacking When You Have Ridges In Your Nails
With the abundance of food in the United States, you may think of nutrient deficiencies as a problem of undeveloped countries, but low intakes due to poor diet or absorption issues are not uncommon. A deficiency in vitamin A, or the minerals calcium and zinc may cause ridges to appear on your nails.
What autoimmune disease causes ridges in fingernails?
A chronic skin condition that affects one in a hundred people, Lichen Planus causes longitudinal ridging in about 10% of people affected with the disorder. It is an autoimmune disease in which the inflammatory cells attack an unknown protein in the body.
What does psoriatic arthritis look like on hands? Stiff, puffy, sausage-like fingers or toes are common, along with joint pain and tenderness. The psoriasis flares and arthritis pain can happen at the same time and in the same place, but not always. You may also notice: Dry, red skin patches with silvery-white scales.
What causes longitudinal ridges in fingernails? They are sometimes called longitudinal striations or bands. Slight vertical ridges in fingernails often develop in older adults, possibly due to a slowing of cell turnover. This is when new skin cells produced below the surface of your skin rise up to take the place of dead cells that are discarded from the surface.
What Is Rheumatoid Arthritis
Rheumatoid arthritis, or RA, is an autoimmune and inflammatory disease, which means that your immune system attacks healthy cells in your body by mistake, causing inflammation in the affected parts of the body.
RA mainly attacks the joints, usually many joints at once. RA commonly affects joints in the hands, wrists, and knees. In a joint with RA, the lining of the joint becomes inflamed, causing damage to joint tissue. This tissue damage can cause long-lasting or chronic pain, unsteadiness , and deformity .
RA can also affect other tissues throughout the body and cause problems in organs such as the lungs, heart, and eyes.
Recommended Reading: Rheumatoid Arthritis Pain At Night
Don’t Miss: Is Lemon Water Good For Rheumatoid Arthritis
You Have Swollen Reddened Skin Around Your Nails
Sometimes people with psoriatic arthritis develop a skin infection around their nails called paronychia, explains Dr. Garshick. This can happen when your nail separates from the bed, when your nails are cracked, or when you have broken skin that allows bacteria, dirt, or other organisms in the cut, according to the Cleveland Clinic. With paronychia, the skin around one or more of your fingernails may suddenly be swollen, reddened, and painful. Paronychia typically requires medical attention treatment depends on the severity of your infection but could include antibiotics, according to the Cleveland Clinic.
How Rheumatoid Arthritis Affects Your Hands
Many joints are covered with a lining called the synovium, which lubricates the joint so it moves more easily. When you have rheumatoid arthritis, the synovium becomes inflamed, thickens, and produces an excess of joint fluid. This is known as synovitis. That extra fluid along with the inflammatory chemicals released by the immune system causes swelling, damages cartilage, and softens the bone within the joint. The swollen tissue may stretch the surrounding ligaments, resulting in deformity and instability, according to the American Society for Surgery of the Hand. The inflammation may also weaken and damage tendons. Ligaments are connective tissues that join two bones tendons are connective issues that join muscle to bone.
When RA strikes the hand, it is most common in the wrist and finger knuckles more specifically the MCP joint, or the large knuckle where the fingers and thumb meet the hand, and the PIP joint, or middle knuckle, explains Jemima Albayda, MD, Assistant Professor of Medicine in the Division of Rheumatology at Johns Hopkins Medicine in Baltimore.
The first knuckle at the top of the finger closest to the nails the DIP, or distal interphalangeal joint is generally spared in RA. In the wrist, RA often affects the joint between the two bones of the forearm, the radius and ulna.
Recommended Reading: Does Rheumatoid Arthritis Affect The Back
Signs And Symptoms Of Rheumatoid Arthritis Of The Hand
Stiffness, swelling, and pain are symptoms common to all forms of arthritis in the hand. In rheumatoid arthritis, some joints may be more swollen than others. There is often a sausage-shaped swelling of the finger. Other symptoms of rheumatoid arthritis of the hand include:
- A soft lump over the back of the hand that moves with the tendons that straighten the fingers
- A creaking sound during movement
- A shift in the position of the fingers as they drift away from the direction of the thumb
- Swelling and inflammation of the tendons that bend the fingers, resulting in clicking or triggering of the finger as it bends, and sometimes causing numbness and tingling in the fingers
- Rupture of tendons with loss of ability to straighten or bend certain fingers or the thumb
- Unstable joints in the wrist, fingers, and thumb
- Deformity in which the middle joint of the finger becomes bent and the end joint hyperextended
- Hyperextension at the middle joint of the finger associated with a bent fingertip
You May Like: What Can Help Arthritis In The Lower Back
Ra Flares Can Have Triggers
It is possible for a specific activity or event to initiate a flare-up. The activity or event sets off inflammation in the body that is difficult to stop. A flare may be triggered by:
- An illness, such as the flu
- An injury or surgery
Triggers vary from person to person. In addition, not all RA flares have clear triggers.
Also Check: Is Physical Therapy Good For Arthritis
Psoriatic Arthritis Vs Rheumatoid Arthritis
According to the National Psoriasis Foundation, 85% of people with psoriatic arthritis also have psoriasis, a condition that can cause red, patchy areas of skin and pitted fingernails.2 But a person does not have to have psoriasis to have psoriatic arthritis, and psoriasis is not always obvious , so a diagnosing doctor will look for other distinguishing symptoms.
See Psoriatic Arthritis Symptoms
How is it similar to RA? Psoriatic arthritis frequently affects the fingers and toes, as well as the knees, wrists and ankles. Affected joints may be swollen, stiff, and painful, especially in the morning. People may feel fatigued.
How is it different? Psoriatic arthritis usually affects the distal joints of the fingers and toesdistal joints are the joints furthest away from the body, such as the third knuckle of a finger. In contrast, RA commonly affects the first and/or second knuckles of the hands.
Rheumatoid Arthritis Nail Changes: Causes And Treatment
| | |
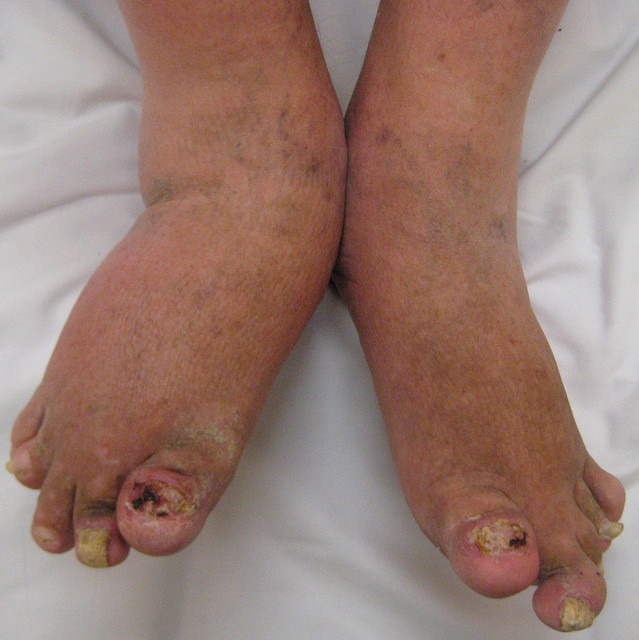
Not only does rheumatoid arthritis cause painful swelling and inflammation in the joints, it can also cause changes to the nails. These changes have long been understood to be caused by RA, with studies as far back as 1960 noting the symptom. Even if nail issues arent as painful as other RA symptoms, they can still cause discomfort and, when noticeable, make someone feel self-conscious.
This article discusses the causes of nail problems or changes in RA, possible treatment options, and advice from myRAteam members on how to handle these issues.
Don’t Miss: Is Laser Therapy Good For Arthritis
Hands In Systemic Diseases
The hand is known to frequently present signs or symptoms of generalized or systemic diseases. Because the hand contains structures from the skin, muscular, skeletal, circulatory, and nervous systems, it often provides clues to diseases which are yet to be diagnosed in other parts of the body. Presentation of complaints, lesions, symptoms or signs in the hand may alert the hand surgeon to these systemic diseases. Although the hand surgeon may not treat all of these diseases, he is in a position to help make the diagnosis and refer the patient to a different specialist.
Musculoskeletal diseases may result in enlargement of the joints. Arthritis diseases commonly are associated with these abnormalities.
Enlargement of the middle joint of a finger. This is called a Bouchards Node.
Figure 1: This is a common finding in osteoarthritis. There is often pain and stiffness. Deformity is also seen.
Enlargement of the small joint of a finger or thumb is called a Heberdens node.
Figure 2: This is a classic sign in osteoarthritis. There may or not be pain, but stiffness or instability may be present. Deformity to the side or down is common when more severe.
Enlargement of a finger/thumb joint may also occur from deposition of crystals from diseases like Gout.
Enlargement of a whole digit, associated with inflammation, may be due to an inflammatory disease. One form is called dactylitis.
Figure 8: Half & Half nails have been associated with chronic kidney failure.
Is My Joint Pain Rheumatoid Arthritis Or Spondyloarthropathy
Ankylosing spondylitis, psoriatic arthritis, and reactive arthritis are part of a group of arthritic conditions called seronegative spondyloarthropathies. Seronegative means that people with these conditions typically do not have antibodies called rheumatoid factors in their blood. In contrast, established rheumatoid arthritis patients often test positive for rheumatoid factor.
See Rheumatoid Arthritis Symptoms
You May Like: What Medication Is Given For Arthritis
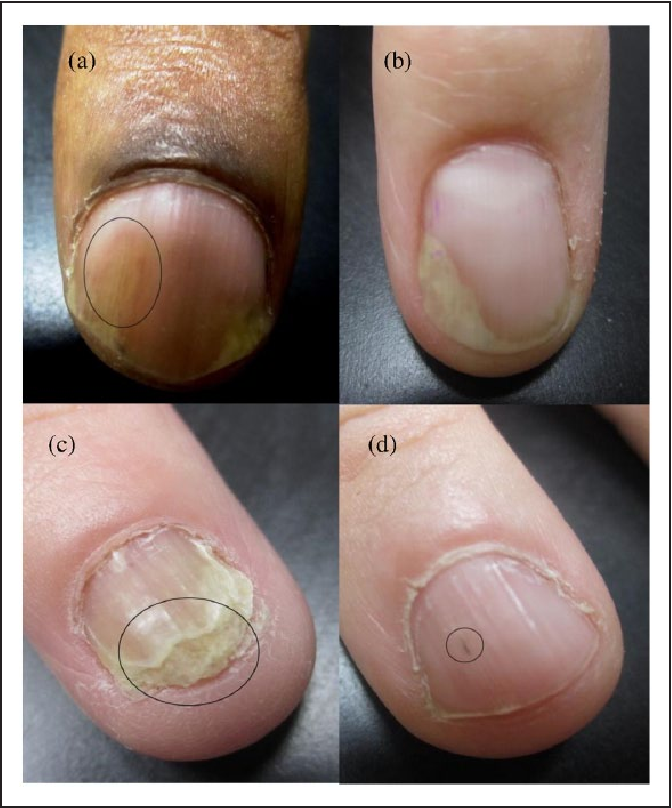
Your Fingernail Separates From Your Nail Bed
This condition, called onycholysis, happens when your fingernail becomes loose and separates from your nail bed, explains Dr. Garshick. Generally, the nail separates starting at the tip and travels down to where your nail meets the skin. In severe cases, people can lose their entire nail. The space created by this separation can lead to an infection, which well get to next. Furthermore, you might notice the separated part of your nail looks opaque and has a white, yellow, or green tinge, according to the Mayo Clinic. Onycholysis treatment includes topical retinoids, steroid injections, or a combination of oral medication and ultraviolet radiation therapy, according to the AAD.
What Areas Of The Body Does Rheumatoid Arthritis Affect Mosaic Weighted Blanket
We are in need of solutions that soothe joints or muscles. What Areas Of The Body Does Rheumatoid Arthritis Affect. Living with Rheumatoid Arthritis may be hard sometimes you need help stretching with deep tissue tools and finding relief when sleeping with the Mosaic weighted blanket.
Im seeing a ton of rave reviews regarding these Mosaic blankets. I had to dig deeper and I found out that Mosaics are designed to be 8-12% of your body weight. Were referring to the same sort of hacks that provide calm to arthritis, anxiety, and also those that experience clinical PTSD. The idea is to give the feeling of being held or hugged to you. The fuzzy and warm feelings you get from this sort of sensory input is replicated through an weighted blanket. The majority of the times you experience pain or numbness in the joints or muscle its because you are unable to relax or stretch that joint or muscle.
This blanket, provides the experience of being hugged tight, which is as soothing regardless of your age.
Anyone who has experienced this type of distress and sought relief knows how frustrating it can be.
So at about $150 for the blanket that could last years and help alleviate pain and allow me to sleep it is a no brainer.
But beware, not all are created and just a few are made for breathability. Like any great idea, tons of brands pop up to provide inferior products .
Recommended Reading: What Does Early Arthritis Feel Like
Rheumatoid Arthritis Vs Osteoarthritis
Many people confuse rheumatoid arthritis with osteoarthritis due to their similar symptoms, but the two diseases are caused by different factors.
What is Osteoarthritis?
Whereas rheumatoid arthritis is an autoimmune disease that causes joint malfunction due to inflammation, osteoarthritis is a mechanical disease brought on by the destruction of joints through wear and tear.
Osteoarthritis is the most common form of arthritis, with approximately 27 million Americans over the age of 25 having been diagnosed with it. Osteoarthritis is also most commonly seen in people middle-aged to elderly and is the top cause of disability in those age groups, though it can also appear in younger people who have sustained joint injuries.
With osteoarthritis, the cartilage, joint lining, ligaments, and bone are all affected by deterioration and inflammation. When the cartilage begins to break down due to stress or changes in the body, the surrounding bones slowly get bigger and begin to fail.
Osteoarthritis is a slowly progressing disease and occurs in the joints of the hand, spine, hips, knees, and toes. Furthermore, risk factors of this disease most often stem from lifestyle or biological causes, such as:
Osteoarthritis sometimes occurs alongside rheumatoid arthritis or other disease, such as gout.
Symptoms Of Psoriatic Arthritis
The severity of the condition can vary considerably from person to person. Some people may have severe problems affecting many joints, whereas others may only notice mild symptoms in 1 or 2 joints.
There may be times when your symptoms improve and periods when they get worse .
Relapses can be very difficult to predict, but can often be managed with medicine when they do occur.
Read Also: What To Do If You Think You Have Arthritis
Can Arthritis In Fingers Affect Nails
Nail symptoms are common in people with psoriasis and even more common in those with psoriatic arthritis. As many as 80% of people with psoriatic arthritis notice changes in their nails. In fact, nail symptoms can be an early warning sign of this type of arthritis.
Does lupus cause nail problems? Lupus Symptom: Nail Changes
Lupus can cause the nails to crack or fall off. They may be discolored with blue or reddish spots at the base. These spots are actually in the nail bed, the result of inflamed small blood vessels. Swelling may also make the skin around the base of the nail look red and puffy.
Can osteoarthritis affect your fingernails?
Osteoarthritic changes of the distal interphalangeal joints may cause nail lesions by exerting direct pressure on the nail matrix or by interfering with local blood flow. Moreover, inflammation of the Heberdens nodes is often present and seems to participate in the development of nail alteration.
How do you treat psoriatic arthritis of the nails? Some treatments work to target your nails directly, such as:
Rheumatoid Arthritis And Your Circulatory System: Ra Can Trigger Anemia And Fatigue
A large percentage of people living with RA experience anemia, a shortage of red blood cells or the iron-rich hemoglobin in the red blood cells. Red blood cells carry oxygen from your lungs to all the cells in the body and organs, so when your organs arent getting enough O2, you can experience weakness, fatigue, headaches, shortness of breath, dizziness, and more.
There are different types of anemia, and the most common type in RA patients is called anemia of inflammation and chronic disease , explains rheumatologist Robert W. Lightfoot, MD, a professor of medicine in the division of rheumatology at the University of Kentucky College of Medicine in Lexington.
No one knows exactly why anemia is more common with RA, but it may be that RAs inflammatory molecules interfere with the bodys ability to use iron, which in turn leads to anemia. Iron supplementation can help, but the best treatment is keeping the inflammation of RA under control with DMARD medication.
Another cause of fatigue: Inflammation can trigger the release of cytokines, molecules that are associated with fatigue. In addition, the depression and pain that can come along with RA can readily sap energy.
Recommended Reading: How To Care For Someone With Rheumatoid Arthritis