When To Get Medical Advice
See a GP if you have persistent pain, swelling or stiffness in your joints even if you have not been diagnosed with psoriasis.
If you’ve been diagnosed with psoriasis, you should have check-ups at least once a year to monitor your condition. Make sure you let the doctor know if you’re experiencing any problems with your joints.
How Custom Beauty Works
Create Your Treatment
Our algorithm creates a unique routine with a few customized products. The algorithm uses 50+ years of skincare research.
Divide and Rule
Every product is designed for one problem. Apply the product when the problem appears. Much like you treat flu or headache.
Changing Your Diet Wont Cure Psoriatic Arthritis
There is no known cure for psoriatic arthritis, and making dietary changes like going paleo or gluten free isnt a remedy. The good news, however, is that a healthy diet with plenty of anti-inflammatory fruits and vegetables thats low in fats and sugars can help keep psoriatic arthritis symptoms under control. Also try to steer clear of dairy and caffeine, which may aggravate psoriatic arthritis symptoms, says Dr. Markenson.
Read Also: What Is The Difference Between Plaque Psoriasis And Psoriatic Arthritis
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else.
Psoriatic arthritis can be classed as a disability if it:
- makes daily tasks difficult
- lasts for more than 12 months.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
The Relationship Between Psoriatic Arthritis And Psoriasis
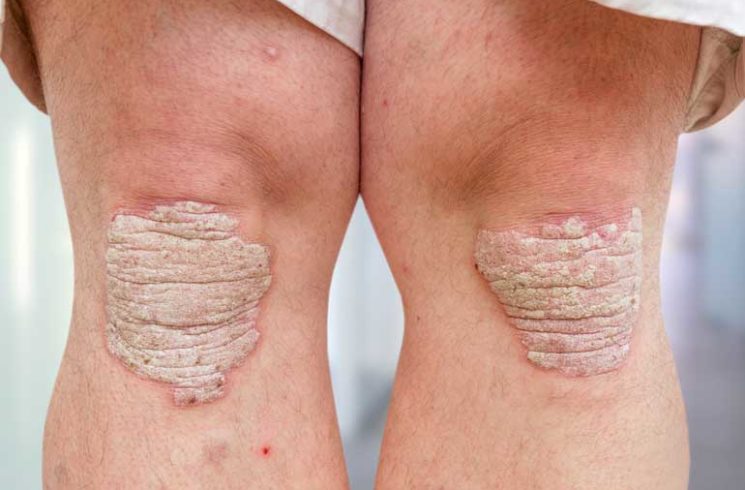
Psoriasis is a risk factor for PsA. Approximately 30 percent of people with chronic psoriasis develop PsA. Around 15 percent of people with PsA have no history of psoriasis before the onset of arthritis. The two are distinct chronic conditions, though they share a genetic connection. Psoriasis is an inflammatory and autoimmune skin disease. PsA is an inflammatory form of rheumatic disease or inflammatory arthritis.
The majority of PsA diagnoses are made in people who already have psoriasis. PsA usually starts 10 to 20 years after the onset of psoriasis. However, a person can develop PsA at any age, whether or not they have developed psoriasis. A MyPsoriasisTeam member shared, I’ve suffered with psoriatic arthritis for as long as I’ve had psoriasis: 30 years .
But the two conditions do not always occur together. Everyone seems to have psoriasis along with psoriatic arthritis, another MyPsoriasisTeam member said. I just have psoriatic arthritis.
Read Also: How Do You Find Out If You Have Rheumatoid Arthritis
How Is Psoriatic Arthritis Treated
Treatment will depend on your symptoms, age, and general health. It will also depend on the severity of your condition.
Boththe skin condition and the joint inflammation are treated. Early diagnosis andtreatment helps prevent joint damage. Some medicines used to treat psoriatic arthritisinclude:
- Nonsteroidal anti-inflammatory medicines to ease symptoms
- Corticosteroids for inflammation
- Immunosuppressive medicines such as methotrexate to reduce inflammation if NSAIDs donât work
- Biologic medicines to ease inflammation
- Vitamins and minerals such as calcium and vitamin D to slow bone deformation
Other treatment may include:
Oral Or Injected Drugs
There are a variety of drugs that target skin cell production or your immune system. These include:
Corticosteroids
These medications mimic cortisol, a naturally occurring anti-inflammatory hormone produced by your body. These are normally taken by mouth and can help reduce inflammation. Injected forms can provide temporary inflammation relief.
Long-term use can result in facial swelling and weight gain. It may also increase your risk for osteoporosis.
Disease-modifying antirheumatic drugs
These medications suppress the chemicals in your body that cause inflammation. This can help reduce prevent joint damage. DMARDs are typically taken by mouth but can also be injected.
Biologics
These medications can prevent inflammation on a cellular level. Biologics are typically injected. The main types of biologics are anti-tumor necrosis factor-alpha drugs, abatacept, and ustekinumab. Each blocks different proteins within the body.
Your risk for infection may increase while taking biologics since they work by suppressing your immune system.
Don’t Miss: What To Take For Arthritis Pain In Foot
What Happens To Patients With Psoriatic Arthritis
Genes implicated in the pathogenesis of PsA include Cw6,IL-23 R alleles and Act1, a molecule in the IL-17R signaling pathway and other MHC Class I alleles , Class I major histocompatibility complex chain-related gene A . Environmental events have also been associated with the onset of psoriatic arthritis, including rubella vaccination, injury sufficient to require a medical consultation, recurrent oral ulcers, moving house and fracture requiring hospitalization.
From a clinical perspective, PsA patients can present with features of RA or spondyloarthritis . The synovial pathology is more akin to findings in spondyloarthritis than RA with infiltrating neutrophils, CD163+ macrophages, and the lack of an antibody response to the shared epitope as observed in RA.The importance of local biomechanical properties in disease pathogenesis, particularly as it relates to the enthesis, has been emphasized. The model of the synovio-entheseal complex delineates an innate immune response triggered by biomechanical and inflammatory events at the enthesis, which subsequently involve adjacent synovium and cartilage.
Mortality rates for PsA were higher than age-matched controls but recent evidence indicates that mortality may not be higher than observed in the general population. PsA patients do have higher rates of mortality from cardiovascular disease than controls.
Pharmacologic considerations
What Are The Symptoms Of Psoriasis
The symptoms will vary based on what type of PsO you have. But most commonly, PsO looks like this:
-
Scaly patches that are red or purple with a silvery surface
-
Plaques on the scalp
-
Lesions that are painful, itchy, and bleed
-
Pitting, brittleness, and discoloration of the nails. The nail can also detach from the nail bed.
Recommended Reading: Does Arthritis Qualify For Social Security Disability
Key Points About Psoriatic Arthritis
- Psoriatic arthritis is a form of arthritis with a skin rash.
- Psoriasis is a chronic skin and nail disease. It causes red, scaly rashes and thick, pitted fingernails. The rash may come before or after the arthritis symptoms.
- Psoriatic arthritis causes inflamed, swollen, and painful joints. It happens most often in the fingers and toes. It can lead to deformed joints.
- Treatment may include medicines, heat and cold, splints, exercise, physical therapy, and surgery.
You’re A Psoriatic Arthritis Expert
Most people who have psoriatic arthritis usually do research on symptoms and new therapies after theyve lived with the condition for a time. They also take it on themselves to talk about their findings with people close to them.
Its important to educate the people around you, says Rabe. I consider myself an expert because Im always researching and learning about my disease, which makes me comfortable answering questions to help my loved ones better understand what Im going through.
Recommended Reading: What Is The Most Effective Pain Reliever For Arthritis
The Two Inflammatory Conditions Often Go Hand
by Health WriterGetty Images/sankalpmaya
Psoriasis and psoriatic arthritis have similar sounding names, but what could a skin condition have to do with an arthritic one? It turns out, a lot. Both diseases are autoimmune-related, meaning an overactive immune system triggers an inflammatory response that leads to symptoms. In the case of PsO, the inflammation shows up on your skin as thick, scaly plaques with PsA, inflammation primarily attacks your joints along with your skin. At least, that’s usually what happens. But is it possible that you can have PsA without PsO? We asked top doctors for the bottom line.
Treatments For The Arthritis
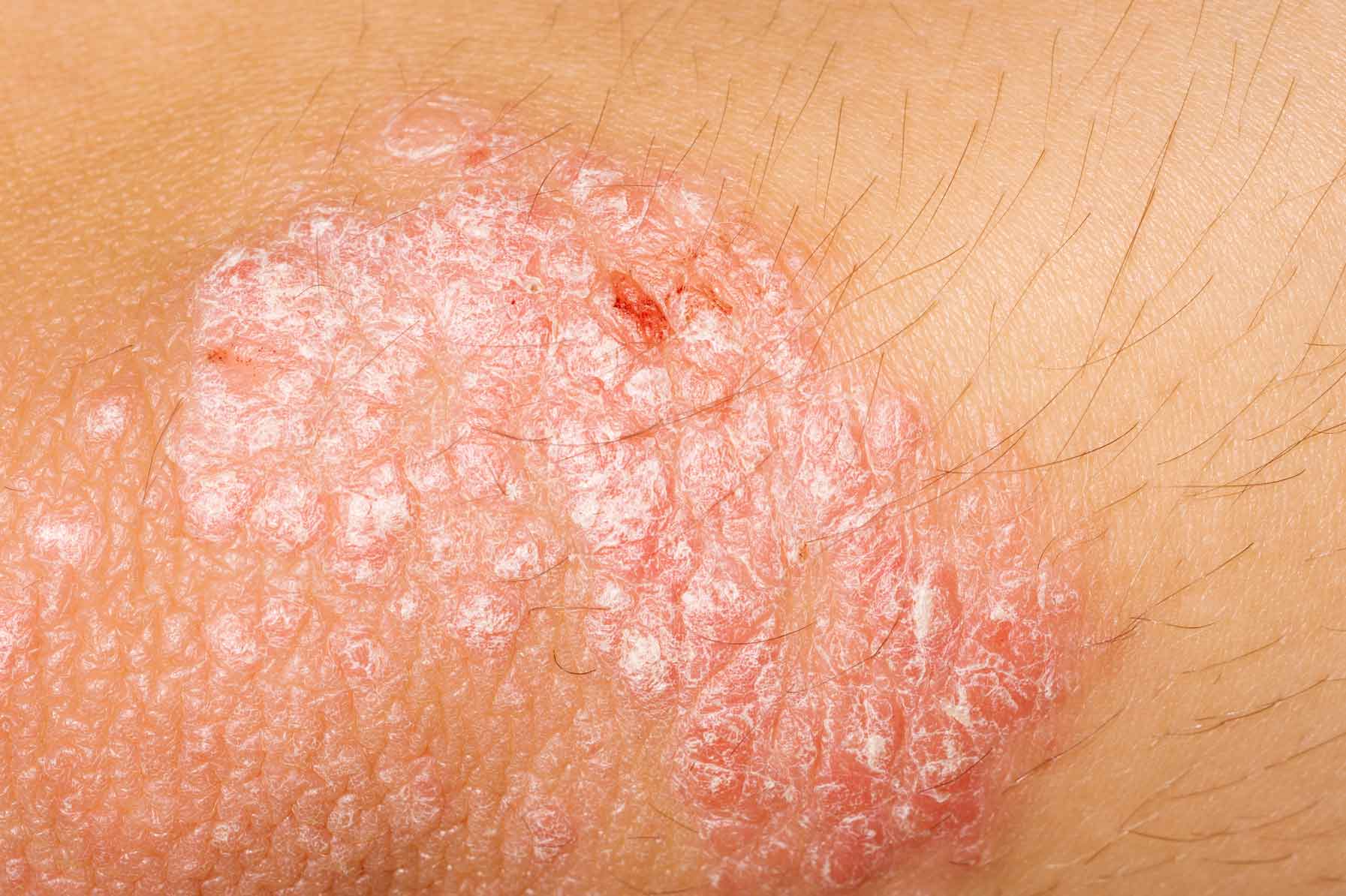
Non-steroidal anti-inflammatory drugs
NSAIDs, or non-steroidal anti-inflammatory drugs, can reduce pain, but they might not be enough to treat symptoms of psoriatic arthritis for everyone.
Some people find that NSAIDs work well at first but become less effective after afew weeks. If this happens, itmight help to try a different NSAID.
There are about 20 different NSAIDs available, including ibuprofen, etoricoxib, etodolac and naproxen.
Like all drugs, NSAIDs can have side effects. Your doctor will reduce the risk ofthese, by prescribing the lowest effective dose for the shortest possible period of time.
NSAIDs can sometimes cause digestive problems, such as stomach upsets, indigestion or damage to the lining of the stomach. You may also be prescribed a drug called a proton pump inhibitor , such as omeprazole or lansoprazole, to help protect the stomach.
For some people, NSAIDs can increase the risk of heart attacks or strokes. Although this increased risk is small, your doctor will be cautious about prescribing NSAIDs ifthere are other factors that may increase your overall risk, for example, smoking, circulation problems, high blood pressure, high cholesterol, or diabetes.
Some people have found that taking NSAIDs made their psoriasis worse. Tell your doctor if this happens to you.
Steroid treatment
Steroid injections into a joint can reduce pain and swelling, but the effects do wear off after a few months.
Disease-modifying anti-rheumatic drugs
Read Also: What Food Causes Rheumatoid Arthritis
Who Can Diagnose And Treat Psoriatic Arthritis
If you have painful, swollen joints and other symptoms, start with your primary care doctor, says Dr. Parody. They may refer you to a rheumatologist, who specializes in diagnosing and treating arthritis and other diseases that affect the joints, muscles and bones.
Some psoriatic arthritis treatments will also help calm skin symptoms. But if you have bothersome psoriasis symptoms, it can be helpful to see a dermatologist, too .
What Are Psoriasis And Psoriatic Arthritis
Psoriasis is a skin disease that causes your body to make new skin cells much faster than normal. These cells build up on your skinâs surface. They form thick, scaly, flaky patches called plaques.
Psoriasis plaques can form anywhere on your body. The most common spots are your elbows, knees, lower back, and scalp. Plaques can be large or small, itchy, or even painful.
Psoriasis can also affect your nails. They can become thick, pitted, and crumbly.
Psoriatic arthritis is a type of arthritis that causes pain, swelling, and damage in the joints.
In both conditions, symptoms can flare up and then go away for a while.
Up to 30% of people with psoriasis will get psoriatic arthritis. Most people with psoriatic arthritis have psoriasis for about 10 years before they have joint symptoms. But some people have psoriatic arthritis alone without ever developing the skin symptoms of psoriasis.
Having a severe form of one disease doesnât mean youâre more likely to get the other disease. You can have severe psoriasis on your skin but never develop psoriatic arthritis. People with severe joint pain from psoriatic arthritis may have only mild skin rashes or none at all.
Read Also: How To Beat Rheumatoid Arthritis Naturally
Blood Tests For Psa And Ra
Blood tests can also help tell the difference between PsA and RA.
About 80 percent of people with RA are said to have seropositive RA, which means they test positive for rheumatoid factor or for cyclic citrullinated peptide antibodies.
Most people with PsA do not have RF or CCP antibodies and are considered seronegative. However, it is also possible to have seronegative RA.
You May Like: How To Deal With Arthritis
Talk With Others Who Understand
MyPsoriasisTeam is the social network for people with psoriatic disease and their loved ones. More than 94,000 members come together to ask questions, give advice, and share their experiences of life with psoriasis or PsA.
Do you have psoriasis or PsA or both? Which came first? Leave a comment below or start a discussion on MyPsoriasisTeam.
Recommended Reading: What Is Better For Arthritis Aleve Or Advil
Can You Have Psoriatic Arthritis Without A Rash
Although rash is a common indicator of PsA, you can develop PsA without having a rash. About 15 percent of people develop PsA without previously having psoriasis, estimates the National Psoriasis Foundation. Sometimes, people develop PsA and psoriasis at the same time.
In these situations, its important to be aware of what the other symptoms of PsA are.
Although rash is commonly associated with PsA, it isnt the only symptom.
Other symptoms include:
- morning stiffness and low back pain
- swelling, pain, or tenderness in joints
- tendon or ligament pain
The Psoriasis Arthritis Symptoms To Watch For
If you are concerned about developing psoriatic arthritis, there are some symptoms to watch out for. First of all, if you have psoriasis already, that is the number one risk factor for getting psoriatic arthritis. Watch for lesions on the nails as a good indicator the ailment will most likely develop.
Family history and age are also determining factors. If you have a parent or sibling with the disease, you are more likely to acquire it as well. The condition usually is diagnosed most frequently in patients between the 30 and 50 years old.
Recommended Reading: What Is The Best Biologic For Rheumatoid Arthritis
How To Utilize Team Care
- Specialty consultations include dermatology, orthopedics, podiatry, endocrinology, and cardiology.
- Dermatology nurses with expertise in wound care.
- Pharmacists are required for preparation of infusables.
- Dieticians are key members of the team because of the high prevalence of obesity and metabolic syndrome.
- Physical and occupational therapists and pedorthists are integral members of the team.
Who Will Be Responsible For My Healthcare
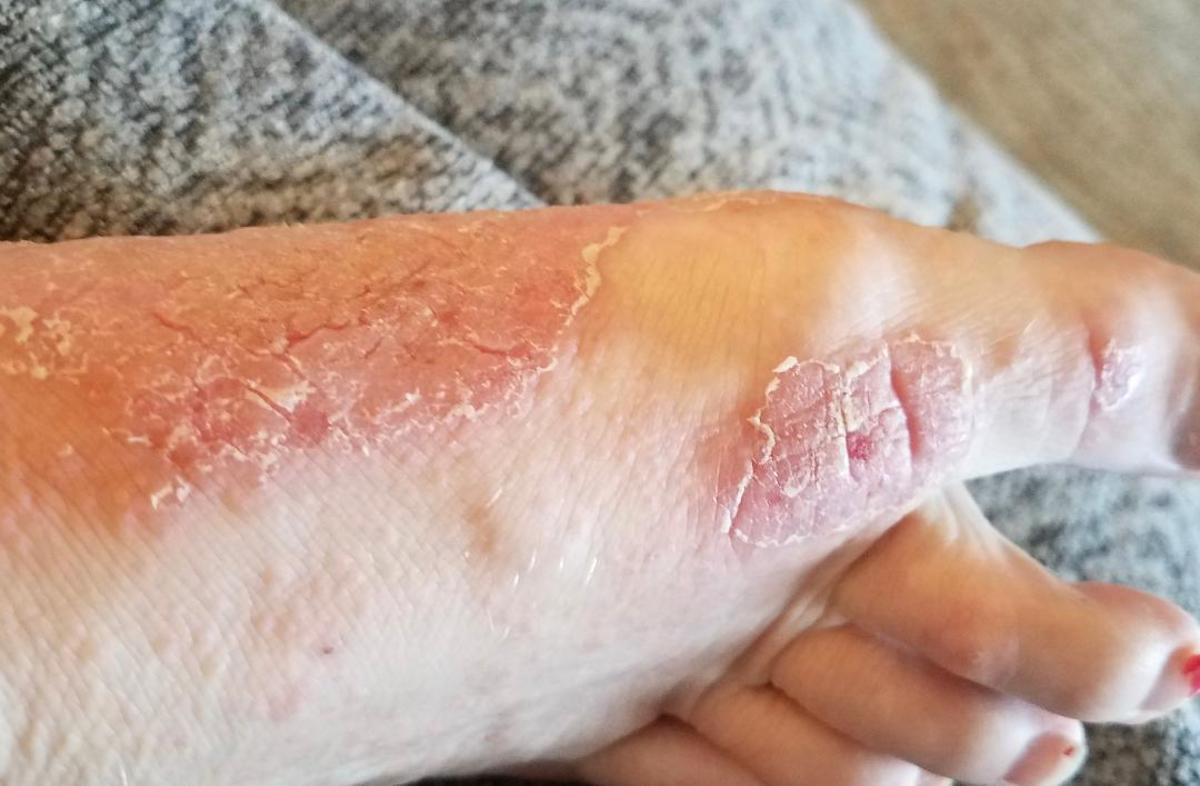
Youre likely to see a team of healthcare professionals.
Your doctor, usually a rheumatologist, will be responsible for your overall care. And a specialist nurse may help monitor your condition and treatments. A skin specialist called a dermatologist may be responsible for the treatment of your psoriasis.
You may also see:
- A physiotherapist, who can advise on exercises to help maintain your mobility.
- An occupational therapist, who can help you protect your joints, for example, by using splints for the wrist or knee braces. You may be advised to change the way you do some tasks to reduce the strain on your joints.
- A podiatrist, who can assess your footcare needs and offer advice onspecial insoles and good supportive footwear.
Read Also: How To Tell If You Have Arthritis In Your Wrist
Your Energy Level Is Like A Bank Account
Psoriatic arthritis can cause extreme fatigue. For every task you complete, or plan to complete, you drain your daily energy bank. Putting on mascara or talking to a neighbor on the street costs you energy. And sometimes, even if its the first thing you do after waking up, a shower may be all it takes to put you right back in bed.
Its important to rest when you need to and not push yourself too hard, especially on days when your symptoms are particularly severe, says Joseph Markenson, MD, a rheumatologist at Hospital for Special Surgery in New York City. Its also important for the loved ones of those who have psoriatic arthritis to understand how draining the condition can be for example, people who have psoriatic arthritis may have to cancel plans frequently or head home early and be sympathetic and patient.
What Causes Psoriatic Arthritis
The genes you inherit from your parents and grandparents can make you more likely to develop psoriatic arthritis. If you have genes that put you at risk of this condition, the following may then trigger it:
- an infection
- being overweight
There is also an element of chance, and it might not be possible to say for certain what caused your condition.
Psoriasis and psoriatic arthritis are not contagious, so people cant catch it from one another.
Don’t Miss: How Can You Treat Rheumatoid Arthritis
Why Some People With Psoriasis Develop Psa
Although psoriasis and PsA may appear unrelated, both conditions reflect underlying immune system problems.
In psoriasis, your overactive immune system causes your bodys skin cells to develop too rapidly. This can be triggered by many environmental factors, such as stress or smoking.
One thing these triggers have in common is that they stimulate your bodys inflammation response. This same inflammation response can happen in your joints. Inflamed joints are what cause PsA.
In PsA, white blood cells target your bodys tissues instead of protecting your body against foreign substances. Though PsA is connected to psoriasis, it has very distinctive symptoms of its own. For this reason, some researchers have referred to PsA as a disease within a disease.
The Centers for Disease Control and Prevention calculates that 10 to 20 percent of people with psoriasis will go on to develop PsA. This is slightly lower than the figures provided by the National Psoriasis Foundation, which put the risk at about 1 in 3, or 30 percent.
Psoriasis is typically diagnosed by the onset of plaques. These are scaly patches of raised, silver-white or reddish skin. PsA affects your joints, typically those in your fingers, toes, and lower back.
PsA can come in many forms. It can trigger other side effects such as fatigue and decreased range of motion. Because psoriasis is more visibly apparent, its often easier to diagnosis than PsA.