Deformity Is Not The Only Characteristic Of Inflammatory Arthritis
Many people, but not all people, are aware that joint deformity is among the signs and symptoms of RA. Hand deformity is a common, visible sign of the disease. Foot deformity is also associated with RA, but it may less visible covered by socks and shoes. If you walk with a limp, or have other gait abnormalities, that may be apparent to others, but they wouldn’t necessarily think of RA versus an injury.
What Joints Does Ra Affect
RA usually starts in your hands. The most common affected areas on your body are:
- Elbows
- The knuckle where each finger meets your hand
- The first joint in your fingers
But RA can appear anywhere on your body, including:
- Toes
- Shoulders
- Finger joint closest to the thumbnail
Your symptoms usually are symmetrical, meaning that they show up in the same joints on both sides of your body.
It doesnât happen often, but RA can also affect joints in your voice box called the cricoarytenoid joints. It can make your voice hoarse. Rarely, you may lose your voice.
What Is Rheumatoid Arthritis Symptoms Causes Diagnosis Treatment And Prevention
Rheumatoid arthritis is a chronic inflammatory disease of the joints. Within the body, joints are the points where bones come together and allow for movement. Most of these joints those called synovial joints also provide shock absorption.
RA is an autoimmune condition, in which your immune system mistakes the linings of your joints as “foreign” and attacks and damages them, resulting in inflammation and pain.
Recommended Reading: What Are The Beginning Signs Of Rheumatoid Arthritis
What Ra Does To Your Heart And Lungs
RA can affect more than just your joints. Complications can involve your organs, blood vessels, and bones.
RA can damage your lungs or inflame the lining around them. This causes chest pain that worsens with breathing, called pleurisy. Lung problems are the most common symptoms of RA outside the joints. This may not cause symptoms, or you might notice shortness of breath. Your doctor can treat it with drugs that ease the inflammation in your lungs.
Severe inflammation from RA in your lungs can make the tissue stiff, thickened, and scarred. This is pulmonary fibrosis, a hard-to-treat condition that makes it tough to breathe.
Likewise, RA can inflame the lining around your heart or your heart muscle . You probably wouldnât notice symptoms from that. Thereâs a chance you could feel shortness of breath or sharp, stabbing chest pain. If you do, call your doctor. It can also raise your odds of heart failure, atrial fibrillation, and stroke.
When RA gets into the cartilage that connects your ribs to your sternum, it can feel like youâre having a heart attack. This is known as chest wall pain.
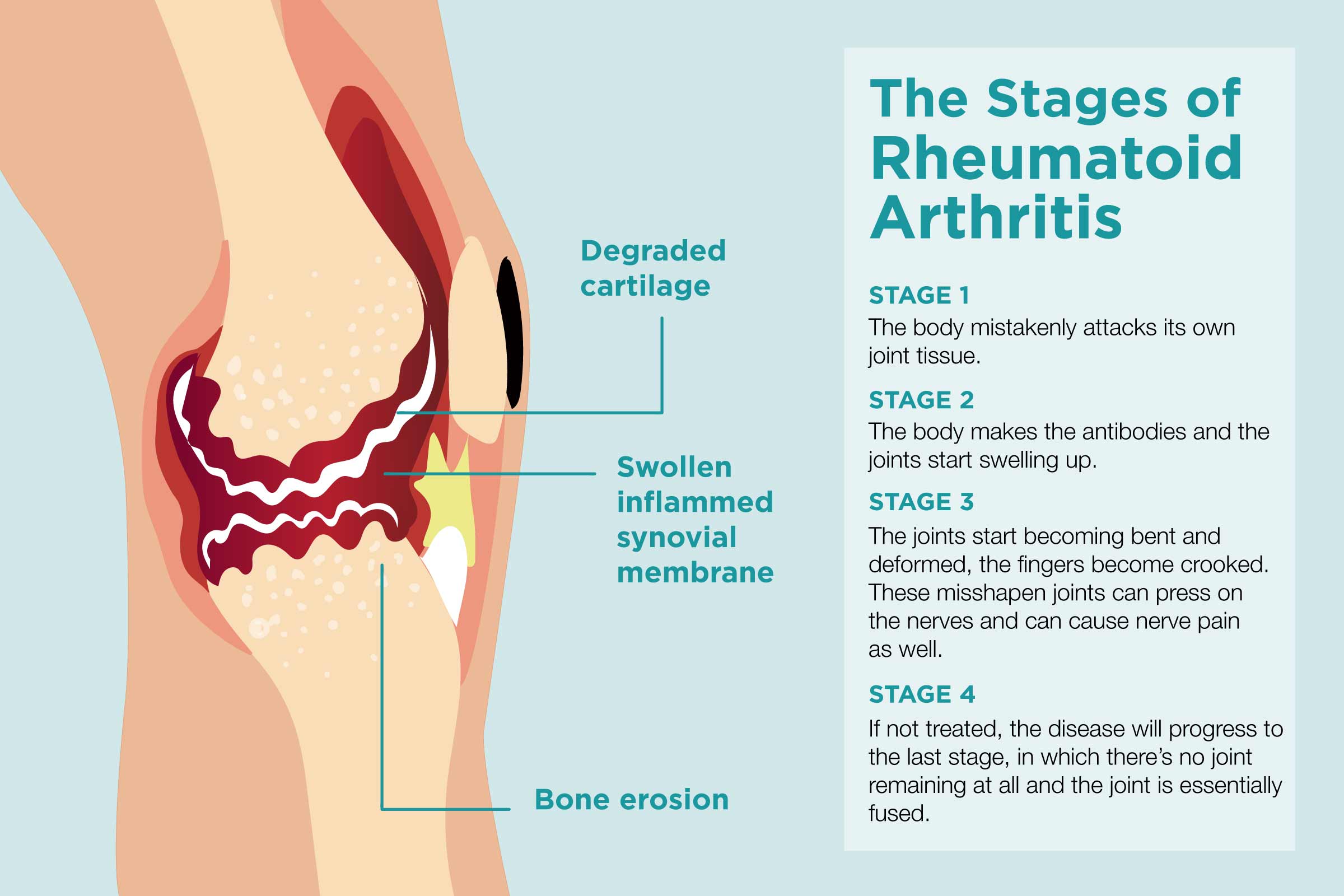
Ra Progression: What Are The Signs Of Rheumatoid Arthritis Progression
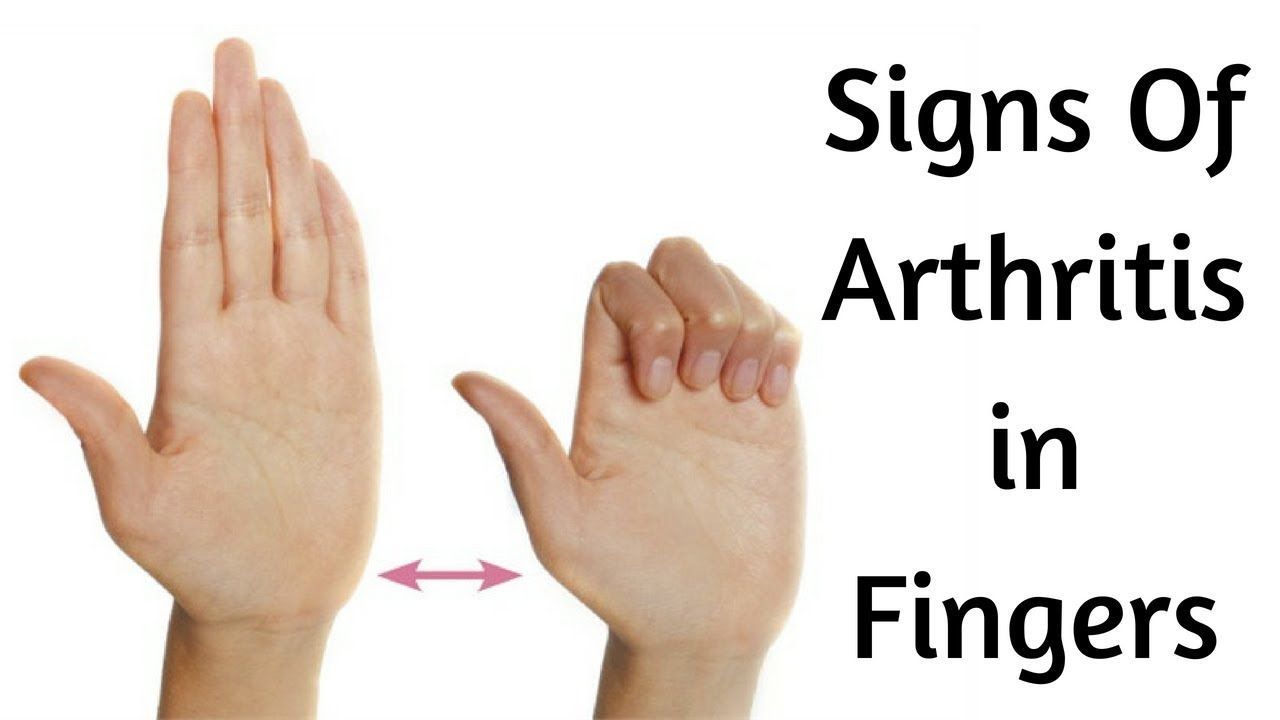
If you suspect you have rheumatoid arthritis or have been recently diagnosed with RA, you will likely have lots of questions and be feeling uncertain about what this disease means for your future. What is the normal RA progression? Will my symptoms get worse? How can I manage the disease? Do I have to have a surgery?
These are all frequent questions asked by RA sufferers. The reality though is that each patient will experience a unique progression of this disease. RA progression depends on multiple unpredictable variables. Because it is still unclear exactly what triggers RA, it can be nearly impossible to predict an exact outcome.
Below is some general information about what to expect as well as the different stages of RA including the advanced condition known as progressive rheumatoid arthritis.
Also Check: What Foods Are Good For Rheumatoid Arthritis
What Are The Symptoms Of Ra In The Hands
The most common symptoms involve pain, swelling and stiffness in the hands and fingers. You may also experience:
- Numbness and tingling similar to carpal tunnel syndrome.
- Joints that are warm and tender to the touch.
- Misshapen joints in your wrist or fingers.
- Fatigue
You will usually experience symptoms in both hands. The pain and stiffness from RA lasts for more than an hour after waking up.
When Can You Get A Covid
It will be up to your states guidelines, but the ACR is pushing for RA patients to be prioritized for vaccination before the general population of similar age and sex. The White House recently declared that all adults in the United States will be eligible for vaccination no later than May 1 so either way, you may not need to wait long.
Government officials are working to make sure every adult will actually be able to get the vaccine by May 1 by increasing the number of locations where people can get vaccinated , expanding the professionals who can administer shots , and providing tools to make it easier to find vaccines , per The White House.
As soon as you have the opportunity to get the vaccine, experts are urging rheumatoid arthritis patients and everyone else to do so. As for which vaccine to get? The official recommendation is to get whatever vaccine youre offered, says Dr. Kaplan.
Once you get your vaccine, you still need to be careful to follow standard mitigation efforts. For more information, heres what immunocompromised people should know about the CDC recommendations for fully vaccinated people.
Recommended Reading: How Do You Know If You Have Arthritis
Loss Of Joint Function
Because rheumatoid arthritis leads to pain, swelling, and tenderness of the involved joints, there is the loss of joint function. The swelling and sensitivity impede the full motion and stability of the joint and it becomes incapable of carrying the movement with confidence, balance, and completeness. This loss of joint function leads to limping, lack of coordination, loss of grip and dexterity, and disability.
Most Rheumatologists And Public Health Experts Want People Living With Rheumatic Diseases Like Rheumatoid Arthritis To Get The Vaccine At The Soonest Opportunity
Learn more about our FREE COVID-19 Patient Support Program for chronic illness patients and their loved ones.
If you live with rheumatoid arthritis, an inflammatory and autoimmune form of arthritis, you may understandably have many questions and concerns about getting the COVID-19 vaccine.
Heres the bottom line: Especially if you have rheumatoid arthritis, most rheumatologists and public health experts recommend you get the COVID-19 vaccine. In fact, guidance from the American College of Rheumatology states that autoimmune and inflammatory rheumatic disease patients should receive the vaccine when theyre eligible.
While getting the vaccine would ideally occur in the setting of well-controlled disease, you should get the COVID-19 vaccine as soon as possible regardless of disease activity and severity, with the exception of extreme cases say, in the intensive care unit.
Heres everything you need to know about getting the COVID-19 vaccine if you have rheumatoid arthritis.
Recommended Reading: Is Gluten Bad For Arthritis
Types Of Inflammatory Arthritis
Some of the common types of inflammatory arthritis are:
- Rheumatoid arthritis :RA is an autoimmune condition. In RA, your immune system mistakenly attacks the lining of your joints.
- Psoriatic arthritis :PsA is a type of arthritis that impacts individuals with the skin condition psoriasis. Its an autoimmune condition in which the immune system attacks healthy joint and skin tissue.
- Axial spondyloarthritis: Axial spondyloarthritis is a type of inflammatory arthritis that mainly impacts the spine and sacroiliac joints. The SI joints are the joints that connect your hipbone to your spine.
- Lupus arthritis: Like RA and PsA, lupus is an autoimmune condition. Many people with lupus have musculoskeletal involvement, which can lead to joint pain and swelling.
- Juvenile idiopathic arthritis :JIA is a type of inflammatory arthritis that affects children and adolescents. Its an autoimmune condition in which the immune system mistakenly attacks healthy joint tissues.
- Gout:Gout is an inflammatory condition that can cause joints to swell and become sensitive and painful. Its triggered by the presence of uric acid crystals in the joints.
Generally speaking, all types of inflammatory arthritis involve the following symptoms in the joints:
- tenderness or pain
- stiffness
- redness
However, each type of inflammatory arthritis can also have unique symptoms or impact a specific area of the body. Lets explore this now.
Favorite Orgs For Essential Rheumatoid Arthritis Information
The American College of Rheumatology is an organization for physicians, health professionals, and scientists that advances rheumatology through education, research, advocacy, and practice support relating to the care of people with arthritis and rheumatic and musculoskeletal diseases. It publishes two medical journals and promotes research into rheumatological conditions.
The Arthritis Foundation is a nonprofit organization dedicated to the prevention, control, and cure of arthritis. The foundation provides information and resources, access to optimal care, advancements in science, and community networking.
CreakyJoints is a leading support, education, advocacy, and research organization for people living with arthritis and rheumatic disease. It is dedicated to raising awareness of all forms of arthritis, which includes educating people about the available varieties of treatment and management strategies.
You May Like: Does Arthritis Pain Cause Fatigue
What Is Juvenile Idiopathic Arthritis
Arthritis doesn’t affect young people as much as it does adults, but lots of teens still get it. Arthritis is an of the synovial membrane, which lines the joints . When it becomes inflamed, fluid is produced. The joints can become stiff, swollen, painful, and warm to the touch. Over time, inflammation in a joint can damage the cartilage and bone.
“Idiopathic” is a medical word that doctors use to describe a disease that has no known cause. Juvenile idiopathic arthritis is the most common kind of arthritis among kids and teens. Kids usually find out they have this disease between the ages of 6 months and 16 years.
Symptoms That Affect Your Skin
Some people with RA get rheumatoid nodules. These are bumps under the skin. Most of the time, they arenât painful, and they move easily when you touch them. About one in four people with RA get these skin bumps.
They usually happen on your elbows, but they might show up on other bony areas like:
Read Also: How To Treat Arthritis In Lumbar Spine
Physical Therapy And Assistive Devices
Physical therapy can help improve muscle strength, flexibility, and range of motion. Stronger muscles can better support a joint, possibly easing pain during movement.
Assistive devices, like canes, raised toilet seats, or equipment to help you drive a car and open jar lids, are available to help you maintain independence and daily function.
How Is Rheumatoid Arthritis Diagnosed
While no single test can definitively diagnose RA, doctors consider several factors when evaluating a person for rheumatoid arthritis.
The diagnostic process typically begins when a doctor gets your medical history and conducts a physical exam. They will ask you about your symptoms to look for signs of RA, in particular things like prolonged joint swelling and morning stiffness that lasts at least half an hour after you wake up.
Next, your doctor will order blood tests to detect rheumatoid factor and anti-citrullinated protein antibodies , which can be specific markers for RA and could indicate RA. You can still have symmetrical inflammatory arthritis with or without systemic markers of inflammation.
In the future, doctors may be able to diagnose RA using infrared light.
Read Also: Can You Exercise With Arthritis
Ra In Hands: What Hand Joints Are Affected By Rheumatoid Arthritis
Its no fun waking up like this: your hands ache. Your fingers are stiff and sometimes twisted. They may even feel hot and tender to the touch. There is no good hand that isnt plagued by these symptoms. Its another flare-up of rheumatoid arthritis , a malady that can affect any joint in the body, but frequently settles in the hands.
How Is Ra Treated
RA can be effectively treated and managed with medication and self-management strategies. Treatment for RA usually includes the use of medications that slow disease and prevent joint deformity, called disease-modifying antirheumatic drugs biological response modifiers are medications that are an effective second-line treatment. In addition to medications, people can manage their RA with self-management strategies proven to reduce pain and disability, allowing them to pursue the activities important to them. People with RA can relieve pain and improve joint function by learning to use five simple and effective arthritis management strategies.
Read Also: What Blood Tests Are Used To Diagnose Psoriatic Arthritis
Causes And Risk Factors Of Rheumatoid Arthritis
RA develops when white blood cells, which normally protect the body from foreign invaders such as bacteria and viruses, enter the synovium . Inflammation ensues the synovium thickens, causing swelling, redness, warmth, and pain in the synovial joint.
Researchers don’t know exactly what causes the immune system to invade the synovium, but it’s believed that genes and environmental factors play a role in the development of RA.
Rheumatology
But not everyone with these identified gene variants develops RA, and people without them can still develop it. So, it’s likely that environmental factors often trigger the disease, particularly in people with a genetic makeup that makes them more susceptible to it. These factors include:
- Viruses and bacteria
- Female hormones
- Obesity, which also increases progression of disability for people with RA.Obese patients are less likely to achieve RA remission regardless of the treatment they receive.
- Severely stressful events
- Foods
Children up to age 16 who experience prolonged swollen or painful joints anywhere in the body are typically diagnosed with juvenile idiopathic arthritis .
Treatments For Ra Swelling
If the swelling is severe, a doctor may recommend removing excess fluid from the affected joint. This procedure is called joint aspiration and is generally carried out under local anesthetic.
A doctor may also inject a substance called hydrocortisone into the joint. This is an anti-inflammatory medication that can reduce some of the symptoms that lead to swelling.
As well as these more immediate fixes, a doctor may prescribe medications to help a person control their RA.
Some people will take a combination of medications designed to prevent RA flare-ups and slow the diseases progression.
Examples of these medications include:
Also Check: How Do You Get Arthritis In Hands
Which Joints In The Hands Are Affected By Ra
The joints that connect your fingers to your hands are among the ones most often affected. You are also likely to experience symptoms in the the joints between your wrist and forearms and the middle knuckles in your fingers. The outermost joints are the least likely to be affected by RA. Usually, people will not start feeling pain there until the joints further down the hand have been affected.
Symptoms Of Progressive Rheumatoid Arthritis

Here are some general warning signs and symptoms that you may have developed progressive rheumatoid arthritis:
The active state of the disease is becoming more frequent Flare-ups are occurring regularly and lasting for longer periods of time Your pain and swelling are becoming more intense, spreading throughout other areas of your body Your diagnosis occurred early on, and so the disease has had a long time to develop You are beginning to develop rheumatoid nodules that you didnt have before Your blood tests show high levels of Rheumatoid Factor or anti-CCP
If you suspect that your rheumatoid arthritis has become progressive, consult your rheumatologist to determine the changes in your condition and discuss potential adjustments to your treatment plan.
You May Like: Are There Tests For Arthritis
Reduced Range Of Motion
Sometimes, the swelling associated with rheumatoid arthritis can be so severe that it causes joints to lock up, unable to be moved. This happens because the tendons surrounding a joint have become so inflamed that joint movement is rendered nearly impossible. A locked joint in the knee can be mistaken for a meniscus tear, so proper diagnosis by a rheumatologist is important when dealing with locked joints and reduced range of motion.
Seronegative Ra Could Become Seropositive Down The Road
Your rheumatoid arthritis markers may change over time from negative to positive, since many people with seronegative rheumatoid arthritis begin to develop RF or ACPA antibodies. It happens, but its not that common, says Dr. Domingues. Dr. Cush says people with seronegative rheumatoid arthritis may start to develop RF or ACPA within the first two years of diagnosis.
RELATED: Rheumatoid Arthritis Myths Debunked
Recommended Reading: How Do You Treat Arthritis In The Hip
Why Im Interested In Rheumatoid Arthritis Swelling
About four years ago, my toe joints swelled to twice their normal size. Naïve to RA politics, I did not photograph them. Neither did my podiatrist.
After a few weeks, the swelling subsided. As I detail in my RA Onset Story, RA symptoms methodically spread to every joint in a neat symmetrical fashion. I was systematically disabled. Since then, I live with tremendous pain, stiffness, and disability. However, I never again saw that remarkable swelling I did at the beginning only minor puffiness.
Over a year ago, I began to research RA swelling because my rheumatology doctor was puzzled and frustrated. Is that funny? Why didnt the doctor do what I did? Oh well, on with our story.
How Is Seronegative Rheumatoid Arthritis Diagnosed
Once the blood tests rule out the presence of RF and anti-CPPs in the patient, it becomes more difficult to achieve a rheumatoid arthritis diagnosis. However, it does happen. Just as having the presence of antibodies doesnt necessarily solidify a seropositive rheumatoid arthritis diagnosis, the absence of antibodies doesnt necessarily rule out a rheumatoid arthritis diagnosis.
If a patient exhibits strong symptoms of rheumatoid arthritis , x-rays can be performed to further examine the symptoms. If the x-ray results indicate bone and cartilage erosion and damage, then a rheumatoid arthritis diagnosis can be made.
Testing for levels of inflammation in a patients joints also helps to support a rheumatoid arthritis diagnosis in seronegative patients. Here are some important criteria doctors follow when diagnosing seronegative rheumatoid arthritis:
- Negative antibody blood test results
- Symmetrical symptoms
- Polyarthritic symptoms, meaning multiple joints are affected
- Condition is inflammatory
Also Check: How To Ease Arthritis Pain In Ankle